
Side Effects of Excess Electrolytes A Health Concern
Side effects of excess electrolytes: It sounds scary, right? But understanding what happens when your body has too much of a good thing – like sodium, potassium, or calcium – is crucial for your health. We often hear about the importance of electrolytes for athletic performance, but what about the potential downsides of having too many? This post dives into the often-overlooked side effects of electrolyte imbalances, helping you understand the signs, causes, and ways to prevent these potentially serious issues.
Electrolytes are essential minerals that carry an electric charge, playing vital roles in numerous bodily functions, from muscle contractions to nerve impulses. While necessary for life, an excess of these minerals can disrupt the delicate balance within your body, leading to a range of symptoms, some mild and others quite serious. We’ll explore specific conditions like hypernatremia (too much sodium), hyperkalemia (too much potassium), and others, examining the symptoms, causes, and treatment options for each.
Let’s get into the nitty-gritty!
Introduction to Electrolyte Imbalance
Electrolytes are essential minerals that carry an electric charge when dissolved in body fluids like blood and other bodily fluids. They play a vital role in numerous bodily functions, including maintaining fluid balance, muscle contractions, nerve impulses, and regulating the pH of your blood. Without the correct balance of electrolytes, your body simply cannot function properly. An imbalance, whether it’s a deficiency or excess, can lead to a range of symptoms, from mild discomfort to life-threatening conditions.Electrolyte balance is a delicate dance, constantly adjusted by your body to maintain optimal health.
Seriously, too many electrolytes can mess you up – nausea, muscle weakness, the whole shebang. It’s a reminder that even seemingly healthy things need balance, much like the risks involved in procedures like egg freezing, as highlighted in this article about Karishma Mehta’s experience: karishma mehta gets her eggs frozen know risks associated with egg freezing.
Understanding those risks, just like knowing the downsides of electrolyte overload, is crucial for making informed choices about your health.
Understanding the role of electrolytes, their dietary sources, and the regulatory mechanisms involved is crucial for appreciating the impact of imbalances.
The Role of Electrolytes in the Body
Electrolytes such as sodium (Na+), potassium (K+), calcium (Ca2+), magnesium (Mg2+), chloride (Cl-), bicarbonate (HCO3-), and phosphate (PO43-) each have specific functions. Sodium is crucial for maintaining fluid balance and nerve impulse transmission. Potassium is essential for muscle contractions and heart function. Calcium is vital for bone health, muscle function, and blood clotting. Magnesium plays a role in numerous enzyme reactions and muscle relaxation.
Chloride helps maintain fluid balance and stomach acid production. Bicarbonate is a key player in maintaining blood pH. Phosphate is involved in bone formation and energy metabolism. Disruptions to the levels of any of these electrolytes can have significant consequences.
So, I’ve been reading up on the nasty side effects of excess electrolytes lately – nausea, muscle weakness, the whole shebang. It got me thinking about overall health markers, and I stumbled upon this fascinating article: can eye test detect dementia risk in older adults. It highlights how subtle changes in our bodies can signal bigger issues, reminding me that maintaining electrolyte balance is just one piece of the complex puzzle of staying healthy as we age.
Dietary Sources of Electrolytes
A balanced diet naturally provides the electrolytes your body needs. Sodium is readily available in processed foods, table salt, and many naturally salty foods. Potassium is abundant in fruits and vegetables, particularly bananas, potatoes, and spinach. Calcium is found in dairy products, leafy green vegetables, and fortified foods. Magnesium is present in nuts, seeds, whole grains, and legumes.
Chloride is found in table salt and many processed foods. The body also produces bicarbonate, and phosphate is found in many foods, especially dairy and meat. However, it’s important to note that excessive intake of some electrolytes, especially sodium, can be detrimental to health.
Excess electrolytes can be seriously dangerous, leading to issues like heart problems and even death. Managing electrolyte balance is crucial, especially for those with kidney disease, which is why the news that the FDA approved clinical trials for pig kidney transplants in humans, as reported by this article , is so exciting. Successfully transplanting these organs could significantly improve the lives of many who struggle with electrolyte imbalances caused by kidney failure.
Understanding the risks of both electrolyte imbalances and the transplant procedure itself remains vital.
Mechanisms of Electrolyte Regulation
The body employs several sophisticated mechanisms to maintain electrolyte balance. The kidneys play a central role, filtering blood and regulating the excretion of electrolytes in urine. Hormones like aldosterone and antidiuretic hormone (ADH) influence the reabsorption of sodium and water in the kidneys. The gastrointestinal tract also plays a role in electrolyte absorption and excretion. For instance, if your body detects low levels of sodium, the kidneys will retain more sodium, and your thirst mechanism will be triggered to encourage you to drink more water.
Similarly, other hormones and regulatory processes constantly monitor and adjust electrolyte levels to maintain homeostasis. This intricate system ensures that the levels of electrolytes remain within a narrow, healthy range.
Excess Sodium (Hypernatremia)
Source: healthjade.net
Hypernatremia, or high blood sodium levels, is a serious electrolyte imbalance that can have significant consequences for your health. While our bodies need sodium to function properly, an excess can disrupt various bodily processes, leading to a range of symptoms, from mild discomfort to life-threatening complications. Understanding the causes, symptoms, and long-term effects of hypernatremia is crucial for effective prevention and management.
Symptoms of Hypernatremia
The symptoms of hypernatremia vary depending on the severity and rate of sodium increase. In mild cases, you might experience subtle changes, while severe hypernatremia can lead to dramatic and dangerous symptoms. Early recognition is key to prompt treatment and preventing serious complications.
Conditions Leading to Hypernatremia
Several conditions can contribute to the development of hypernatremia. These often involve situations where the body loses more water than sodium, or where there’s excessive sodium intake without a corresponding increase in water.
- Dehydration: Prolonged diarrhea, excessive sweating (especially during intense exercise or heat exposure), and inadequate fluid intake are common causes. The loss of water concentrates the sodium in the blood.
- Diabetes Insipidus: This condition involves a deficiency in the antidiuretic hormone (ADH), which regulates water reabsorption in the kidneys. This leads to excessive water loss in urine, concentrating sodium in the blood.
- Kidney Disease: Impaired kidney function can affect the body’s ability to regulate sodium levels, potentially leading to hypernatremia.
- Congestive Heart Failure: In some cases, severe heart failure can impair the kidneys’ ability to excrete sodium, leading to an increase in blood sodium levels.
- Excessive Sodium Intake: Consuming a diet extremely high in sodium, particularly with limited water intake, can also contribute to hypernatremia. This is less common than other causes but can be a factor, especially in individuals with impaired kidney function.
Long-Term Effects of Chronic Hypernatremia
Chronic hypernatremia, if left untreated, can lead to significant long-term health problems. The persistent elevation of sodium levels can damage various organs and systems.
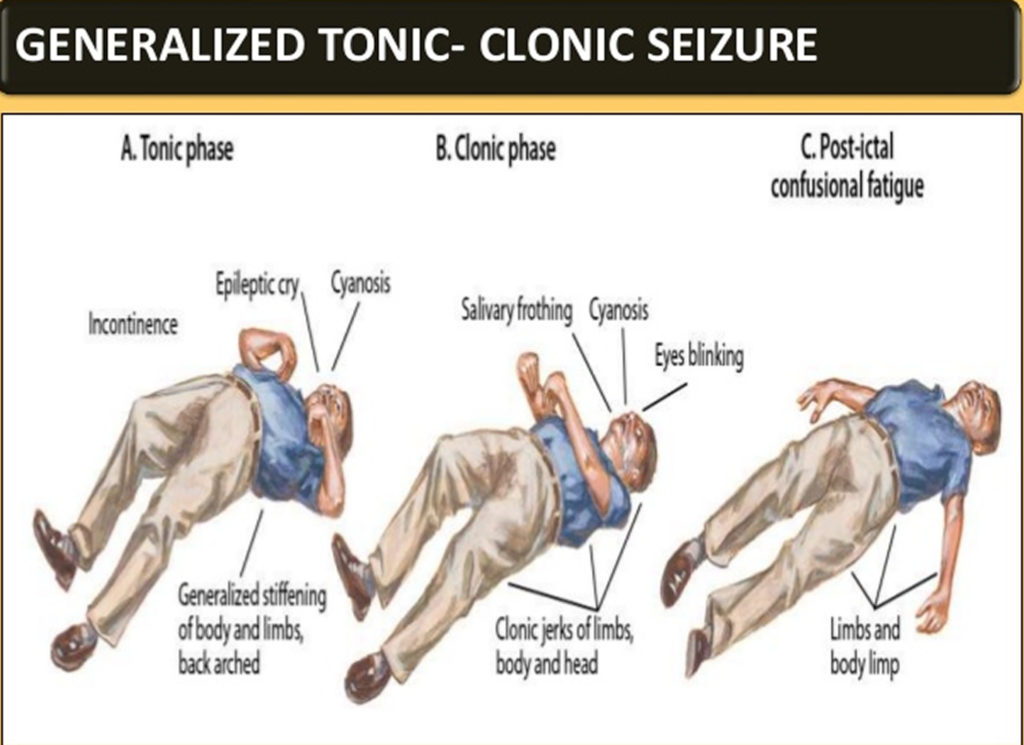
- Brain Damage: High sodium levels can cause brain cells to shrink, leading to neurological problems such as seizures, confusion, and coma. In severe cases, permanent brain damage can occur.
- Kidney Damage: Chronic hypernatremia can put extra stress on the kidneys, potentially leading to chronic kidney disease.
- Cardiovascular Problems: Elevated sodium levels can contribute to high blood pressure and increase the risk of cardiovascular diseases, such as heart attack and stroke.
- Cognitive Impairment: Long-term exposure to high sodium levels can lead to cognitive decline and memory problems.
Comparison of Hypernatremia Severity
The following table summarizes the symptoms, treatment approaches, and potential complications associated with different levels of hypernatremia severity. Remember, this is for informational purposes only and should not be used for self-diagnosis or treatment. Always consult a healthcare professional for any health concerns.
| Severity | Symptoms | Treatment Approach | Potential Complications |
|---|---|---|---|
| Mild | Mild thirst, lethargy, irritability | Increased fluid intake, dietary sodium restriction | Generally few complications with prompt treatment |
| Moderate | Increased thirst, confusion, muscle weakness, nausea, vomiting | Intravenous fluid administration, careful monitoring of sodium levels | Seizures, dehydration |
| Severe | Severe confusion, seizures, coma, respiratory arrest | Intravenous fluid administration, careful monitoring, possibly dialysis | Permanent brain damage, death |
Excess Potassium (Hyperkalemia)
Source: vecteezy.com
Hyperkalemia, or high potassium levels in the blood, is a serious electrolyte imbalance that can have significant consequences for the heart and other organs. Unlike sodium imbalances, which are often linked to dehydration or excessive intake, hyperkalemia arises from a complex interplay of factors affecting potassium regulation in the body. Understanding the causes, symptoms, and treatment of hyperkalemia is crucial for effective medical management.
Causes of Hyperkalemia
Hyperkalemia can stem from both dietary factors and underlying medical conditions. Dietary causes are less common than medical causes, but excessive potassium intake from supplements or certain foods (like bananas, potatoes, and oranges) can contribute, especially in individuals with impaired kidney function. More frequently, however, hyperkalemia is a consequence of medical issues affecting potassium excretion or distribution within the body.
Dietary Causes of Hyperkalemia
Excessive consumption of potassium-rich foods and supplements can lead to hyperkalemia, particularly in individuals with compromised kidney function. This is because the kidneys play a crucial role in regulating potassium levels by excreting excess potassium in the urine. When kidney function is impaired, the body’s ability to remove excess potassium is reduced, leading to a build-up in the bloodstream.
For example, a patient with chronic kidney disease who consumes a diet high in potassium might experience a rapid increase in their serum potassium levels.
Medical Causes of Hyperkalemia
A wide range of medical conditions can disrupt potassium homeostasis and cause hyperkalemia. These include acute or chronic kidney disease (the most common cause), conditions affecting adrenal gland function (such as Addison’s disease), medications (e.g., certain diuretics, ACE inhibitors, and NSAIDs), and certain types of tissue damage (e.g., rhabdomyolysis, burns, or severe trauma). In these situations, the body either fails to excrete sufficient potassium or potassium is released from damaged cells into the bloodstream in excess.
For instance, patients undergoing chemotherapy might experience hyperkalemia due to tumor lysis syndrome, where the breakdown of cancer cells releases large amounts of potassium into the circulation.
Symptoms of Hyperkalemia
The symptoms of hyperkalemia can vary widely depending on the severity and rate of potassium elevation. Mild hyperkalemia may be asymptomatic. However, as potassium levels rise, symptoms can include muscle weakness, fatigue, paresthesias (tingling or numbness), and gastrointestinal disturbances such as nausea and vomiting. In severe cases, hyperkalemia can lead to life-threatening cardiac arrhythmias, potentially causing cardiac arrest.
The hallmark of severe hyperkalemia is often changes in the electrocardiogram (ECG), showing characteristic peaked T waves, widened QRS complexes, and ultimately, cardiac standstill.
Treatment of Hyperkalemia
Treatment for hyperkalemia depends on the severity of the condition and the patient’s clinical presentation. Mild hyperkalemia may only require dietary modifications, such as restricting potassium intake. However, moderate to severe hyperkalemia requires more urgent interventions to rapidly lower potassium levels and prevent potentially fatal cardiac arrhythmias. Treatment strategies include administering intravenous calcium gluconate to stabilize cardiac membranes, administering insulin and glucose to shift potassium into cells, using cation exchange resins to bind and eliminate potassium through the gastrointestinal tract, and, in severe cases, dialysis to remove potassium from the blood.
Diagnostic Pathway for Hyperkalemia
A flowchart illustrating the diagnostic pathway for hyperkalemia would begin with a patient presenting with symptoms suggestive of electrolyte imbalance or a known risk factor (e.g., kidney disease, medication use). A blood test measuring serum potassium levels would be the initial diagnostic step. If hyperkalemia is confirmed, further investigations would be necessary to identify the underlying cause. This could involve assessing kidney function, checking adrenal hormone levels, and reviewing the patient’s medication history.
Depending on the findings, appropriate treatment would be initiated. For instance, a patient with mild hyperkalemia due to dietary factors might only need dietary adjustments, while a patient with severe hyperkalemia due to acute kidney injury would require urgent medical intervention, including dialysis.
Excess Calcium (Hypercalcemia): Side Effects Of Excess Electrolytes
Hypercalcemia, characterized by abnormally high levels of calcium in the blood, can significantly disrupt the body’s delicate balance. This condition doesn’t always present with obvious symptoms, making early detection crucial. The effects of elevated calcium ripple through various organ systems, impacting their function and overall well-being.
Physiological Effects of Elevated Calcium Levels
Calcium plays a vital role in numerous physiological processes, including muscle contraction, nerve impulse transmission, and blood clotting. When calcium levels rise excessively, these processes become dysregulated. Elevated calcium interferes with the normal functioning of cells, leading to a cascade of effects that can manifest in various ways, ranging from subtle changes to severe complications. For example, excessive calcium can inhibit the release of certain hormones, affecting metabolism and other bodily functions.
The impact varies depending on the severity and duration of the hypercalcemia.
Hypercalcemia’s Impact on Organ Systems
Hypercalcemia’s effects are widespread, impacting several organ systems. The kidneys, for instance, may struggle to excrete the excess calcium, potentially leading to kidney stones and impaired kidney function. The gastrointestinal system can experience reduced motility, resulting in constipation, nausea, and vomiting. The cardiovascular system may be affected by changes in heart rhythm and blood pressure. Furthermore, the nervous system can be impacted, leading to symptoms such as fatigue, confusion, and even cognitive impairment in severe cases.
In the musculoskeletal system, hypercalcemia can weaken bones, increasing the risk of fractures.
Medical Conditions Associated with Hypercalcemia
Several medical conditions can contribute to hypercalcemia. Hyperparathyroidism, a condition where the parathyroid glands produce excessive parathyroid hormone (PTH), is a common cause. Malignancies, particularly those involving bone metastases, can also release calcium into the bloodstream. Certain medications, such as thiazide diuretics, can also contribute to hypercalcemia. Furthermore, prolonged immobilization can lead to increased bone resorption and elevated calcium levels.
Granulomatous diseases, such as sarcoidosis, can also cause hypercalcemia due to increased vitamin D production.
Dietary Recommendations for Individuals at Risk of Hypercalcemia
It’s crucial for individuals at risk of hypercalcemia to carefully manage their dietary calcium intake. A balanced diet is key, and consulting a registered dietitian or healthcare professional is recommended for personalized guidance.
- Limit dairy products: Reduce consumption of milk, cheese, and yogurt, which are high in calcium.
- Choose low-calcium alternatives: Opt for calcium-reduced or calcium-free alternatives for dairy products.
- Reduce calcium-rich vegetables: Limit intake of leafy green vegetables like kale and spinach, which are naturally high in calcium.
- Control calcium supplements: Avoid excessive calcium supplementation unless specifically prescribed by a doctor.
- Increase fluid intake: Adequate hydration helps the kidneys excrete excess calcium.
Excess Magnesium (Hypermagnesemia)
Hypermagnesemia, or an excess of magnesium in the blood, might seem less discussed than its sodium or potassium counterparts, but it’s a serious electrolyte imbalance with potentially life-threatening consequences. While often linked to kidney disease, it can also arise from excessive magnesium intake through medications or supplements. Understanding its symptoms, interactions, and diagnosis is crucial for timely intervention.
Symptoms of Hypermagnesemia
The symptoms of hypermagnesemia vary widely depending on the severity of the magnesium elevation. Mild hypermagnesemia may present with few noticeable symptoms, possibly only subtle changes detected through blood tests. As magnesium levels increase, however, more pronounced symptoms emerge. These can include nausea, vomiting, and weakness. More severe hypermagnesemia can lead to profound muscle weakness, loss of deep tendon reflexes, slowed heart rate (bradycardia), hypotension (low blood pressure), respiratory depression, and even coma.
The progression from mild to severe symptoms is usually gradual, but rapid increases in magnesium levels can lead to a sudden onset of severe symptoms.
Drug Interactions with Hypermagnesemia
Many medications can interact with magnesium, either increasing the risk of hypermagnesemia or exacerbating its effects. For example, magnesium-containing antacids or laxatives, when taken in excessive amounts or by individuals with impaired kidney function, can significantly raise blood magnesium levels. Certain antibiotics, such as aminoglycosides, can also increase the risk of hypermagnesemia. Moreover, the effects of other medications can be altered by high magnesium levels.
For instance, neuromuscular blocking agents used during surgery might have a prolonged and intensified effect in patients with hypermagnesemia, increasing the risk of respiratory paralysis. Careful medication management is essential for individuals at risk of or diagnosed with hypermagnesemia.
Diagnostic Tests for Hypermagnesemia
A simple blood test measuring serum magnesium levels is the primary method for diagnosing hypermagnesemia. This test provides a quantitative measure of the magnesium concentration in the blood, allowing for accurate assessment of the severity of the imbalance. Other tests might be ordered to investigate the underlying cause of the hypermagnesemia, such as kidney function tests (creatinine and glomerular filtration rate) and tests to assess for other electrolyte imbalances.
The diagnosis often requires careful interpretation of the magnesium level in conjunction with the patient’s clinical presentation and medical history.
Hypermagnesemia Across Age Groups
The effects of hypermagnesemia can vary across different age groups. Infants, particularly those born prematurely, are especially vulnerable to the toxic effects of elevated magnesium levels, due to their immature renal function. Symptoms in infants might include hypotonia (decreased muscle tone), respiratory depression, and cardiac arrhythmias. Adults typically experience the range of symptoms previously described, from mild nausea to severe respiratory and cardiac complications.
Elderly individuals, often with pre-existing kidney disease, are also at increased risk of developing hypermagnesemia and may be more susceptible to the neurological and cardiovascular effects, potentially experiencing more severe consequences even with moderate increases in magnesium levels. Age-specific considerations are vital when managing hypermagnesemia.
Excess Phosphorus (Hyperphosphatemia)
Source: dreamstime.com
Hyperphosphatemia, or high levels of phosphorus in the blood, is often overlooked but can be a serious condition, especially when coupled with other electrolyte imbalances. It’s crucial to understand its causes, consequences, and management strategies to ensure optimal patient care. This condition is frequently intertwined with other electrolyte disturbances, creating a complex clinical picture that requires careful attention.
Relationship Between Hyperphosphatemia and Other Electrolyte Imbalances
Hyperphosphatemia often occurs alongside other electrolyte abnormalities, most notably hypocalcemia (low calcium). This is because phosphorus and calcium share an inverse relationship; when phosphorus levels rise, the body often tries to compensate by reducing calcium levels. This interplay can lead to a cascade of symptoms, affecting various bodily functions. For instance, high phosphorus levels can interfere with calcium absorption in the gut and increase calcium excretion by the kidneys, further exacerbating hypocalcemia.
Additionally, hyperphosphatemia can sometimes be seen with hypomagnesemia (low magnesium) and hyperkalemia (high potassium), although the relationships are less direct than with calcium. The interplay between these electrolytes necessitates a holistic approach to diagnosis and treatment.
Risk Factors Associated with Hyperphosphatemia, Side effects of excess electrolytes
Several factors increase the risk of developing hyperphosphatemia. Chronic kidney disease (CKD) is a primary culprit, as the kidneys play a vital role in phosphorus excretion. When kidney function declines, phosphorus accumulates in the blood. Patients with CKD often require dialysis, which, while life-saving, can sometimes lead to fluctuations in phosphorus levels. Other risk factors include hypoparathyroidism (underactive parathyroid glands), which reduces the body’s ability to regulate phosphorus, and certain types of tumors that release excessive amounts of phosphorus into the bloodstream.
Additionally, excessive intake of phosphorus-rich foods, particularly in individuals with compromised kidney function, can contribute to hyperphosphatemia. Finally, rhabdomyolysis (muscle breakdown) can release large amounts of phosphorus into the circulation, leading to a rapid elevation in serum phosphorus levels.
Management Strategies for Hyperphosphatemia
Managing hyperphosphatemia involves a multifaceted approach focused on controlling dietary phosphorus intake and promoting its excretion. Dietary restrictions, limiting phosphorus-rich foods like dairy products, processed meats, and colas, are often recommended. Phosphate binders, medications that bind to phosphorus in the gastrointestinal tract, preventing its absorption, are a cornerstone of treatment, particularly for individuals with CKD. These binders are typically taken with meals.
In cases of severe hyperphosphatemia, dialysis may be necessary to remove excess phosphorus from the blood. Addressing underlying conditions, such as hypoparathyroidism or CKD, is also crucial for long-term management. Regular monitoring of serum phosphorus levels is essential to assess treatment effectiveness and adjust strategies as needed.
Causes and Treatment Options for Hyperphosphatemia
| Causes of Hyperphosphatemia | Treatment Options |
|---|---|
| Chronic kidney disease (CKD) | Phosphate binders, dietary restriction, dialysis |
| Hypoparathyroidism | Calcium and vitamin D supplementation, phosphate binders |
| Tumor lysis syndrome | Hydration, dialysis, allopurinol (to prevent uric acid build-up) |
| Excessive intake of phosphorus | Dietary modification |
| Rhabdomyolysis | Fluid resuscitation, supportive care, dialysis (if necessary) |
General Effects of Excess Electrolytes
Excess electrolytes, regardless of the specific ion involved, can wreak havoc on the body’s delicate internal balance. While the specific symptoms vary depending on which electrolyte is in excess, there are several common threads that link these seemingly disparate conditions. Understanding these general effects is crucial for recognizing and managing electrolyte imbalances effectively.Excess electrolytes disrupt cellular function in several ways.
High concentrations of ions outside cells can alter the osmotic pressure, drawing water out of cells and causing them to shrink. This dehydration at the cellular level impairs their ability to function normally, leading to a cascade of problems throughout the body. Conversely, some excess electrolytes can interfere with the proper functioning of cellular enzymes and ion channels, disrupting vital processes like nerve impulse transmission and muscle contraction.
Cardiovascular System Effects of Excess Electrolytes
The cardiovascular system is particularly vulnerable to electrolyte imbalances. Excess electrolytes can significantly alter heart rhythm and contractility. For example, hyperkalemia (high potassium) can lead to a life-threatening condition called cardiac arrest due to the disruption of the electrical signals that control the heart’s rhythm. Similarly, hypercalcemia (high calcium) can cause irregular heartbeats and increase the risk of cardiac arrhythmias.
These effects are due to the alteration of the heart muscle cells’ electrical properties and their ability to contract effectively. The changes in heart rate and rhythm can manifest as palpitations, weakness, and even sudden cardiac death in severe cases.
Common Symptoms Across Electrolyte Excesses
A range of nonspecific symptoms commonly appear across various electrolyte excesses. These often include nausea, vomiting, and fatigue. These symptoms reflect the widespread disruption caused by electrolyte imbalances, affecting multiple organ systems. Muscle weakness or cramps are also frequently reported, reflecting the disruption of muscle function at the cellular level. In severe cases, neurological symptoms such as confusion, seizures, and even coma can occur.
The severity of these symptoms varies depending on the degree of imbalance and the specific electrolyte involved.
Long-Term Health Consequences of Chronic Electrolyte Imbalances
Chronic electrolyte imbalances, if left unaddressed, can lead to serious long-term health problems. Prolonged hyperkalemia, for example, can contribute to kidney damage and potentially lead to kidney failure. Chronic hypercalcemia can increase the risk of kidney stones and osteoporosis. These long-term consequences highlight the importance of early diagnosis and effective management of electrolyte disorders. For instance, a patient with chronic hypernatremia (high sodium) might experience persistent hypertension, increasing their risk of stroke and heart disease.
The cumulative effects of these imbalances can significantly impact quality of life and longevity.
Prevention and Management Strategies
Maintaining a healthy electrolyte balance is crucial for overall well-being. Electrolyte imbalances, whether from excess or deficiency, can lead to serious health complications. Fortunately, through mindful lifestyle choices and regular medical attention, we can significantly reduce the risk of these imbalances. This section will Artikel practical strategies for preventing and managing electrolyte issues.
Importance of Hydration
Adequate hydration is the cornerstone of electrolyte balance. Water acts as the solvent, distributing electrolytes throughout the body and facilitating their proper function. Dehydration concentrates electrolytes, increasing the risk of excess. Conversely, excessive water intake can dilute electrolytes, leading to deficiencies. The recommended daily fluid intake varies depending on factors like climate, activity level, and overall health, but aiming for consistent hydration throughout the day is key.
Signs of dehydration include thirst, dark urine, dizziness, and fatigue. Staying ahead of thirst is important; don’t wait until you’re parched to drink.
Dietary Adjustments for Electrolyte Intake
Our diet plays a significant role in electrolyte balance. Processed foods are often high in sodium, contributing to hypernatremia. Similarly, excessive consumption of potassium-rich foods, while generally beneficial, can be problematic for individuals with kidney issues. A balanced diet emphasizing whole, unprocessed foods, fruits, and vegetables provides a more natural and regulated source of electrolytes. Moderation is key; avoid overconsumption of salty snacks, processed meats, and foods high in potassium if you have pre-existing conditions.
Consulting a registered dietitian can provide personalized dietary guidance based on individual needs and health status.
Role of Regular Medical Checkups
Regular medical checkups are essential for early detection and management of electrolyte imbalances. Blood tests can accurately measure electrolyte levels, allowing healthcare providers to identify potential problems before they become severe. Individuals with underlying medical conditions, such as kidney disease, heart failure, or diabetes, are at higher risk and should undergo more frequent monitoring. Early intervention through lifestyle adjustments, medication, or other treatments can prevent serious complications.
Don’t hesitate to discuss any concerns about electrolyte balance with your doctor, especially if you experience symptoms like muscle weakness, cramps, or irregular heartbeat.
Last Recap
Maintaining a healthy electrolyte balance is key to overall well-being. While electrolyte imbalances can stem from various underlying medical conditions, simple lifestyle changes like mindful hydration and a balanced diet can significantly reduce your risk. Remember, paying attention to your body’s signals and seeking medical advice when necessary are crucial steps in preventing and managing electrolyte issues. This isn’t just about athletic performance; it’s about your overall health and well-being.
So stay informed, stay hydrated, and stay healthy!
Questions Often Asked
Can I get excess electrolytes from supplements?
Yes, excessive use of electrolyte supplements, particularly those with high sodium or potassium content, can easily lead to imbalances. Always follow recommended dosages and consult a healthcare professional before using them, especially if you have pre-existing health conditions.
What are the early warning signs of an electrolyte imbalance?
Early signs can be subtle and vary depending on the electrolyte involved but might include unusual fatigue, muscle weakness or cramps, nausea, vomiting, confusion, or changes in heart rhythm. If you experience any of these, it’s best to seek medical attention.
How is an electrolyte imbalance diagnosed?
A blood test is typically used to measure electrolyte levels in the blood. Your doctor might also order other tests depending on your symptoms and medical history to determine the underlying cause of the imbalance.
Are there any foods I should avoid if I’m at risk of electrolyte imbalances?
This depends on the specific electrolyte imbalance. For example, those at risk of hypernatremia should limit high-sodium foods like processed meats and salty snacks. Those with kidney problems might need to limit potassium-rich foods like bananas and spinach. A doctor or registered dietitian can provide personalized dietary advice.
