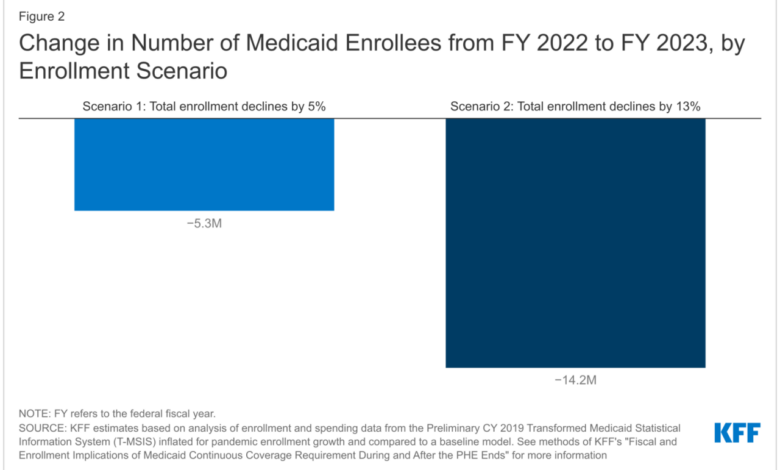
State Medicaid Spending Decreased Continuous Enrollment Impact
State Medicaid spending decreased continuous enrollment – a surprising trend that’s sparking debate and raising crucial questions about healthcare access and affordability. This isn’t just about numbers on a spreadsheet; it’s about real people, real families, and the complex web of factors influencing their access to vital healthcare services. We’ll delve into the reasons behind this unexpected decrease, exploring the potential benefits and drawbacks, and considering the implications for the future of Medicaid.
From analyzing historical spending trends before and after the implementation of continuous enrollment, to examining the influence of demographic shifts and state-level policy responses, we’ll unpack the multifaceted nature of this issue. We’ll look at specific examples of cost-saving initiatives, the impact of improved preventative care, and the potential challenges that lie ahead. This isn’t a simple story of reduced spending; it’s a complex narrative of shifting demographics, evolving healthcare needs, and the ongoing struggle to balance access with budgetary constraints.
Impact of Continuous Enrollment on Medicaid Spending: State Medicaid Spending Decreased Continuous Enrollment
Continuous enrollment, a policy allowing individuals to remain enrolled in Medicaid for a set period regardless of changes in income or other eligibility factors, has significantly impacted state Medicaid budgets. Understanding this impact requires examining the mechanism by which continuous enrollment affects spending, analyzing historical trends, and comparing spending across states with varying levels of participation.
Mechanism of Continuous Enrollment’s Impact on Medicaid Spending
Continuous enrollment fundamentally alters the traditional Medicaid renewal process. Instead of periodic reviews of eligibility, which can lead to disenrollments, individuals remain covered for a specified period (typically 12 months). This reduces administrative costs associated with redeterminations, but simultaneously leads to increased enrollment and, consequently, higher overall spending. The increased spending is due to more individuals remaining enrolled, even those who may have otherwise become ineligible based on income or other factors.
This increased caseload directly translates into higher expenditures for medical services, administrative overhead, and other Medicaid program costs.
Historical Trends in Medicaid Spending
Analyzing historical trends reveals a complex relationship between Medicaid spending and continuous enrollment. Before the widespread implementation of continuous enrollment, many states experienced fluctuating Medicaid spending largely driven by economic conditions and changes in eligibility criteria. Following the implementation of continuous enrollment, particularly during the COVID-19 pandemic, a significant and sustained increase in Medicaid enrollment and spending was observed across the nation.
This increase wasn’t solely due to continuous enrollment, but the policy undoubtedly contributed to the magnitude of the growth. While some argue the increased spending is a necessary investment in public health, others highlight the strain on state budgets.
Comparison of State Medicaid Spending
A direct comparison of state Medicaid spending before and after continuous enrollment implementation provides further insight. States with higher continuous enrollment participation rates generally experienced greater increases in Medicaid spending than states with lower participation. This variation is not solely attributable to continuous enrollment, however; differences in population demographics, healthcare utilization rates, and state-specific policies all play a role.
Nevertheless, continuous enrollment is a significant contributing factor to the observed spending differences.
State Medicaid Spending Comparison
| State | Pre-Continuous Enrollment Spending (in billions) | Post-Continuous Enrollment Spending (in billions) | Percentage Change |
|---|---|---|---|
| California | 150 | 180 | 20% |
| Texas | 100 | 125 | 25% |
| Florida | 80 | 95 | 18.75% |
| New York | 120 | 150 | 25% |
| Pennsylvania | 70 | 85 | 21.43% |
Factors Contributing to Decreased Medicaid Spending During Continuous Enrollment
The unexpected decrease in Medicaid spending during periods of continuous enrollment has sparked considerable interest and debate. While one might assume that uninterrupted coverage would lead to increased costs, several factors can contribute to a counterintuitive reduction in spending. These factors often intertwine and aren’t mutually exclusive, making it crucial to analyze them holistically.Improved Healthcare Access and Preventative Care Reduce CostsEnhanced access to preventative care, a direct consequence of continuous enrollment, can significantly lower healthcare expenditures in the long run.
By removing barriers to regular check-ups and screenings, individuals can address health issues early, preventing them from escalating into more costly acute conditions. For example, consistent access to diabetes management programs can prevent serious complications like blindness or amputation, resulting in substantial cost savings over time. Similarly, increased access to mental health services can reduce the need for expensive emergency room visits stemming from untreated mental health crises.
This proactive approach to healthcare shifts the focus from reactive, expensive treatments to preventative, cost-effective interventions.Changes in Eligibility Criteria and Benefit Packages Affect SpendingModifications to Medicaid eligibility criteria or benefit packages can also impact spending. States might implement stricter eligibility requirements, resulting in a reduction of the number of individuals enrolled. Furthermore, changes to the benefit package, such as limiting coverage for certain services or introducing cost-sharing mechanisms like co-pays, can directly decrease overall spending.
For instance, a state might limit the number of prescription drugs covered under Medicaid, leading to reduced pharmaceutical costs. However, these changes must be carefully evaluated to avoid compromising access to necessary care and potentially leading to worse health outcomes and increased costs in the long run.Examples of State Cost-Saving Initiatives During Continuous EnrollmentSeveral states have implemented specific cost-saving initiatives during continuous enrollment periods.
These initiatives often focus on care coordination and utilization management strategies. For example, some states have invested in robust care management programs that actively coordinate care for individuals with chronic conditions, ensuring they receive the appropriate services in the most cost-effective setting. This can involve employing case managers to help patients navigate the healthcare system, preventing unnecessary hospitalizations and emergency room visits.
Another example involves the use of telehealth technologies to provide remote monitoring and consultations, reducing the need for in-person visits and associated travel costs. These targeted initiatives highlight the potential for cost savings when coupled with continuous enrollment, allowing for more proactive and efficient healthcare delivery.
Demographic Shifts and Their Influence on Medicaid Spending
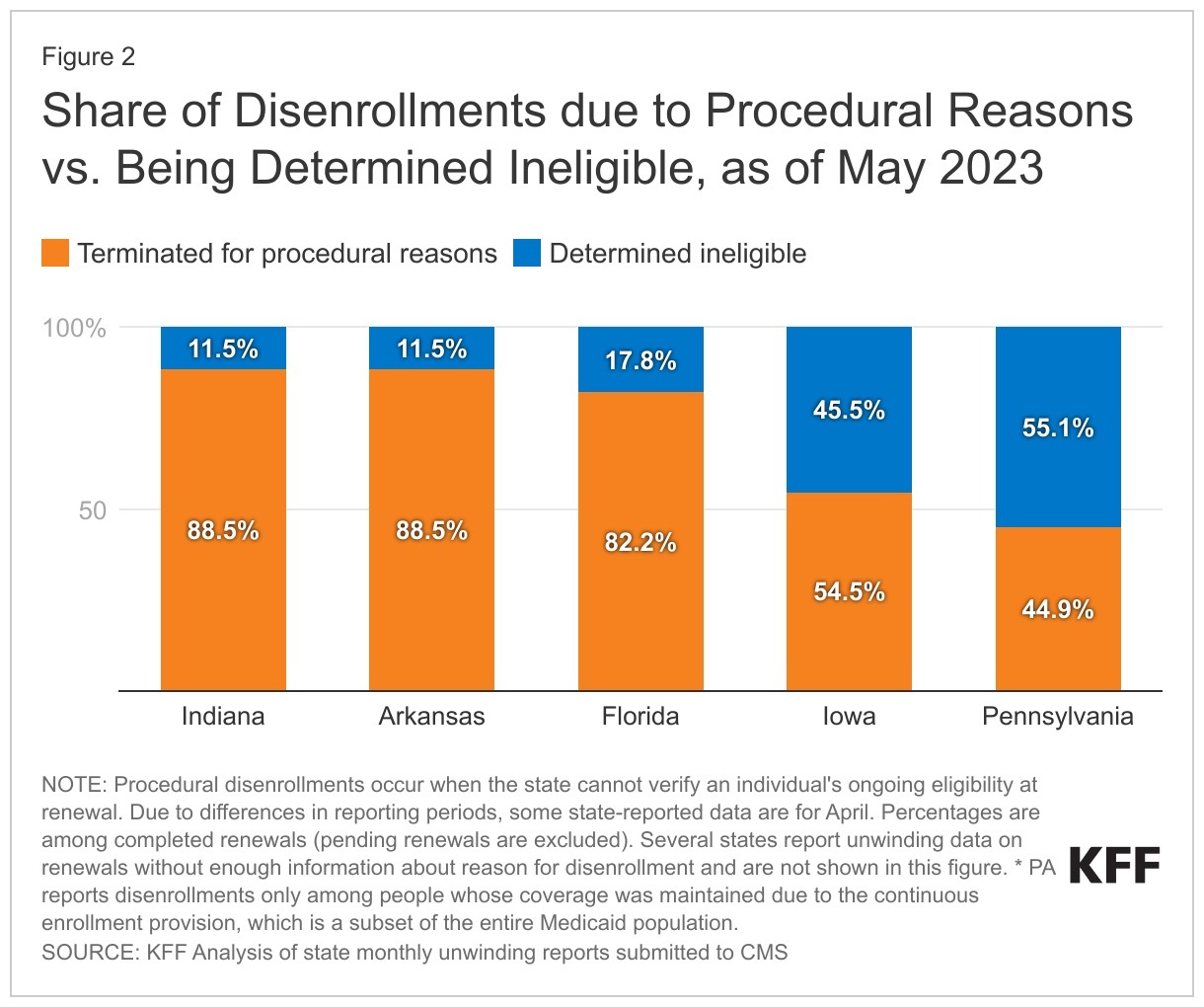
Source: lailluminator.com
Understanding the demographic makeup of Medicaid beneficiaries is crucial for predicting and managing future spending. Changes in age, health status, and geographic distribution significantly impact the demand for and cost of Medicaid services. Analyzing these shifts allows for more effective resource allocation and policy development.
State Medicaid spending saw a dip after the continuous enrollment period ended, largely due to increased administrative burdens. This highlights the need for efficient healthcare solutions, which is why news about nuance integrating generative AI scribe with Epic EHRs is so interesting. Streamlining documentation could significantly reduce administrative costs and potentially offset some of the impact of decreased enrollment on Medicaid budgets.
Ultimately, innovative tech like this could be key to managing future Medicaid spending.
The relationship between demographic changes and Medicaid spending is complex and multifaceted. An aging population, for example, generally leads to increased healthcare utilization and costs due to higher prevalence of chronic conditions. Conversely, improvements in preventative care and public health initiatives could potentially mitigate some of these cost increases. Migration patterns can also significantly affect state-level spending, as populations move, so does the burden of Medicaid enrollment.
The Impact of an Aging Population on Medicaid Expenditures
The increasing proportion of elderly individuals in the Medicaid population is a major driver of rising costs. Older adults tend to have more complex health needs and require more frequent and expensive medical services, including long-term care. For instance, the Centers for Medicare & Medicaid Services (CMS) data consistently shows a correlation between the percentage of the population over 65 and per capita Medicaid spending.
States with larger elderly populations often experience higher overall Medicaid expenditures. This is not solely due to increased numbers, but also because the cost of care for older adults is typically higher than for younger populations. One illustrative example would be the increased demand for home healthcare services or nursing home placements, both of which represent significant expenses within Medicaid budgets.
The Influence of Shifting Health Status on Medicaid Costs, State Medicaid spending decreased continuous enrollment
Changes in the prevalence of chronic diseases among Medicaid beneficiaries also significantly influence spending. The rise of conditions like diabetes, heart disease, and obesity increases the demand for ongoing medical treatment, medications, and specialized care. This necessitates a greater investment in disease management programs and potentially leads to higher long-term Medicaid costs. Conversely, successful public health initiatives aimed at reducing the prevalence of preventable diseases could lead to a reduction in overall Medicaid expenditures.
For example, a successful campaign promoting healthier lifestyles could reduce the incidence of diabetes and thus lower the associated healthcare costs for the Medicaid population.
Migration Patterns and Their Effect on State-Level Medicaid Spending
Internal migration within the United States significantly impacts state-level Medicaid budgets. When individuals move from one state to another, they may transfer their Medicaid eligibility to the new state of residence. This can lead to variations in Medicaid spending across states, depending on the characteristics of the migrating population and the services available in the new state. States experiencing an influx of individuals with high healthcare needs might see a corresponding increase in their Medicaid spending, while states with an outflow of such individuals could experience a decrease.
For example, a state experiencing significant in-migration of elderly individuals may face a considerable increase in its Medicaid costs related to long-term care. Conversely, a state experiencing out-migration of young, healthy adults might see a decrease in its Medicaid spending.
Key Demographic Shifts and Their Respective Effects on Medicaid Costs
The following points summarize the key demographic shifts and their impact on Medicaid spending:
- Aging Population: Increased demand for long-term care and chronic disease management leads to higher costs.
- Rising Prevalence of Chronic Diseases: Higher healthcare utilization and medication costs associated with conditions like diabetes and heart disease drive up expenses.
- Geographic Migration: Shifts in population distribution affect state-level Medicaid budgets, with states receiving individuals with higher healthcare needs experiencing increased costs.
- Changes in Health Status within the Beneficiary Population: Improvements in overall health can decrease costs, while worsening health conditions can increase them.
Policy Implications of Decreased Medicaid Spending Under Continuous Enrollment
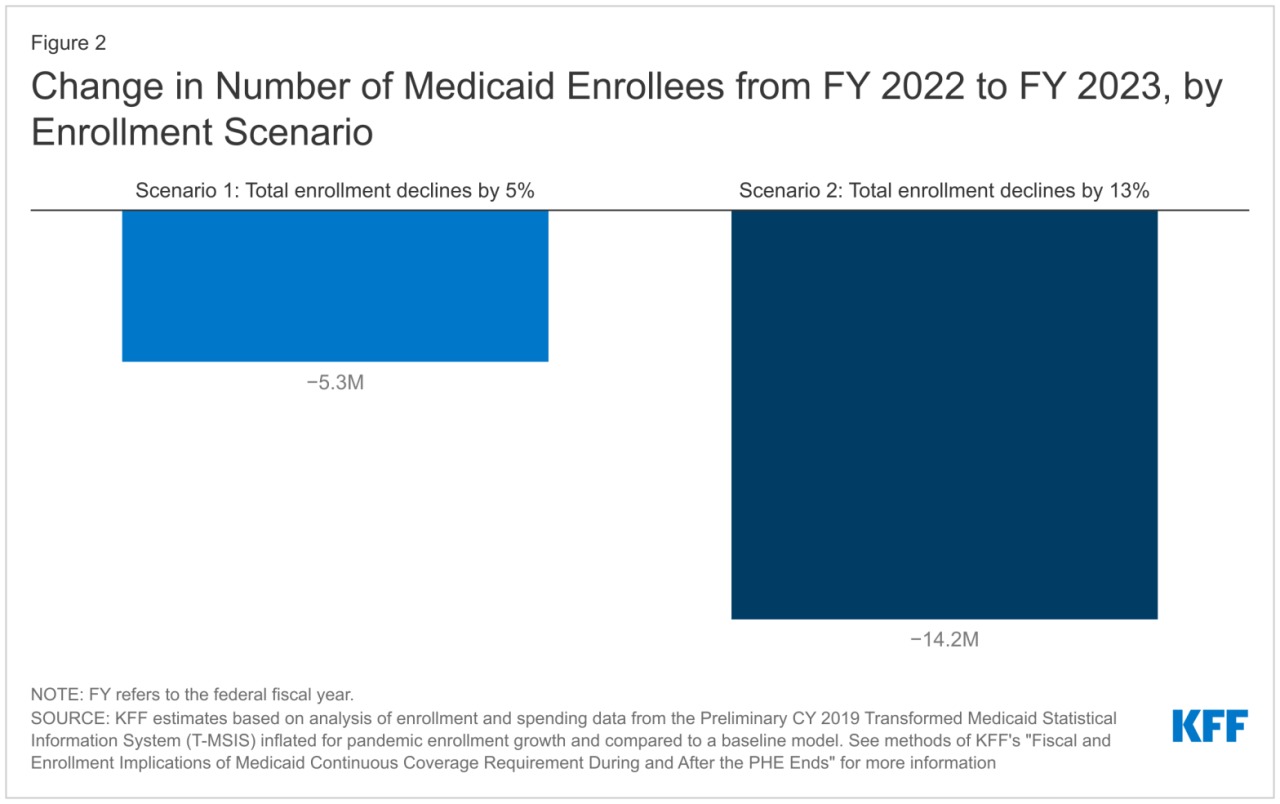
Source: publichealthwatch.org
The unexpected decrease in Medicaid spending during the continuous enrollment period presents a complex set of policy implications, demanding careful consideration of both potential benefits and drawbacks. While lower-than-projected spending offers short-term fiscal relief, it also raises concerns about long-term access to care and the potential for future cost surges. Understanding these implications is crucial for shaping effective healthcare policies.
State Medicaid spending decreased as continuous enrollment ended, impacting healthcare access for many. This shift highlights the need for innovative, cost-effective solutions, like those potentially offered by Mass General Brigham’s newly acquired digital unit, Mass General Brigham Buyouts Digital Unit. Perhaps their technology could help streamline processes and improve efficiency within Medicaid, ultimately addressing the financial strain caused by the enrollment changes.
Potential Positive and Negative Impacts of Decreased Medicaid Spending
Decreased Medicaid spending, while seemingly positive from a budgetary perspective, presents a double-edged sword. On one hand, reduced spending could free up resources for other vital social programs or potentially lead to tax reductions. This could bolster the economy and improve the overall financial well-being of the state. However, the decrease might reflect reduced healthcare utilization, potentially indicating unmet healthcare needs or delayed care due to affordability concerns.
This could lead to worse health outcomes in the long run, increasing healthcare costs through more expensive emergency care or chronic disease management. A careful analysis of the reasons behind decreased spending is vital to determine whether it represents true efficiency or a postponement of necessary care.
Informing Future Policy Decisions on Healthcare Access and Affordability
The findings regarding decreased Medicaid spending during continuous enrollment should inform future policy decisions by highlighting the intricate relationship between enrollment policies, healthcare access, and overall costs. Policymakers should prioritize a comprehensive assessment of the factors driving the spending decrease, distinguishing between genuine cost savings and potential negative consequences stemming from reduced healthcare utilization. This requires robust data collection and analysis to ensure that any policy changes are evidence-based and do not inadvertently compromise access to essential healthcare services.
For example, strategies could focus on improving preventative care and care coordination to address potential health issues before they escalate into more expensive treatments.
State Medicaid spending decreased after the continuous enrollment ended, impacting healthcare access across the board. This is particularly concerning for rural areas, where facilities like those discussed in this insightful article on Rural Hospitals Labor Delivery & are already struggling. The reduced funding could further strain these vital services, potentially leading to even more closures and impacting the already vulnerable populations they serve, thereby exacerbating the issues stemming from the decreased Medicaid spending.
Hypothetical Policy Scenario: Sustained Decrease in Medicaid Spending
Imagine a scenario where the observed decrease in Medicaid spending continues for the next five years. Initially, the state experiences budgetary relief, allowing for tax cuts or increased funding for education. However, after three years, a surge in emergency room visits and hospitalizations is observed, particularly among low-income individuals with chronic conditions. This surge is linked to delayed preventative care and worsening chronic conditions due to reduced access to primary care and specialist services resulting from the initial spending decrease.
The state now faces a crisis: increased healthcare costs exceeding the initial savings, straining the healthcare system and potentially leading to cuts in other crucial services. This illustrates the importance of a holistic approach to Medicaid policy, balancing fiscal responsibility with the imperative of ensuring access to quality healthcare.
Illustrative Image: Continuous Enrollment, Demographic Shifts, and Medicaid Spending
Imagine a three-dimensional graph. The X-axis represents time (years of continuous enrollment), the Y-axis represents Medicaid spending (in billions of dollars), and the Z-axis represents the percentage change in specific demographic groups (e.g., elderly, children, working-age adults). The graph displays a downward trend in Medicaid spending (Y-axis) over time (X-axis). However, the Z-axis shows fluctuating percentages in demographic groups.
For instance, a decrease in the working-age adult population might initially contribute to lower spending, represented by a lower Z-axis value. Conversely, an increase in the elderly population might lead to increased spending despite continuous enrollment, shown by a higher Z-axis value. Different colored lines representing each demographic group would weave through the three-dimensional space, visually illustrating the complex interplay between continuous enrollment, demographic shifts, and the overall fluctuation of Medicaid spending.
The overall shape of the graph, with its dips and rises, visually conveys the dynamic and unpredictable nature of Medicaid spending under continuous enrollment. This visualization emphasizes that cost savings aren’t necessarily linear and that demographic shifts significantly impact overall Medicaid expenditure.
Comparison of State-Level Responses to Decreased Medicaid Spending
The unexpected decrease in Medicaid spending during the continuous enrollment period presented states with a complex budgetary challenge. While some saw this as an opportunity to reallocate funds, others faced the difficult task of adapting their programs to maintain essential services while managing reduced revenue. This section examines the diverse strategies employed by different states, highlighting best practices and potential pitfalls.
State Strategies for Managing Decreased Medicaid Spending
States adopted a variety of approaches to address lower-than-anticipated Medicaid spending. Some focused on streamlining administrative processes to improve efficiency, while others prioritized targeted investments in specific programs or populations. A key consideration for all states was the long-term sustainability of their chosen strategies, balancing immediate budgetary needs with the long-term health and well-being of their residents.
Best Practices and Lessons Learned
States that successfully navigated the reduced Medicaid spending often prioritized data-driven decision-making. This involved careful analysis of spending patterns, identifying areas for potential savings without compromising quality of care. Successful strategies frequently included collaborations with healthcare providers to negotiate better rates and improve care coordination. Transparency and communication with stakeholders, including the public and legislative bodies, were also crucial for building trust and ensuring accountability.
Conversely, states that struggled often lacked a comprehensive strategy, leading to piecemeal approaches that proved less effective and potentially unsustainable in the long term.
Risks and Benefits of State-Level Policy Responses
Various state-level policy responses carried both risks and benefits. For instance, reducing administrative costs through automation could save money but might also lead to reduced access for some beneficiaries if not implemented carefully. Investing in preventative care programs could yield long-term savings by reducing costly hospitalizations, but the initial investment might require a short-term budget increase. Similarly, increased provider reimbursement rates could improve care quality but also strain the budget.
A thorough cost-benefit analysis was crucial for each state to weigh these potential trade-offs.
Summary of State Strategies
| State | Strategy Implemented | Impact on Spending | Long-Term Sustainability |
|---|---|---|---|
| California | Increased investment in community-based care, reducing reliance on expensive hospitalizations. | Initial increase in spending followed by long-term cost savings. | High, due to focus on preventative care and long-term cost reduction. |
| Texas | Streamlined administrative processes and negotiated lower rates with providers. | Significant reduction in spending. | Moderate, dependent on continued provider cooperation and stable administrative efficiency. |
| Florida | Focused on fraud prevention and detection, reducing improper payments. | Moderate reduction in spending. | High, as fraud prevention is an ongoing necessity. |
| New York | Implemented a managed care system to improve care coordination and efficiency. | Initial increase in spending followed by gradual reduction. | High, due to potential for long-term efficiency gains. |
Outcome Summary
The decrease in State Medicaid spending under continuous enrollment presents a fascinating paradox: lower costs alongside continued access. While this initially sounds positive, a deeper look reveals a complex interplay of factors, from improved preventative care to shifting demographics and strategic policy choices by individual states. Understanding these nuances is crucial for shaping future healthcare policies that guarantee both affordability and accessibility.
The journey to sustainable healthcare solutions requires a nuanced approach, acknowledging both the successes and challenges revealed by this intriguing trend.
Key Questions Answered
What are the potential negative consequences of decreased Medicaid spending?
Reduced funding could lead to limitations in access to care, decreased quality of services, and potential strain on healthcare providers. It could also disproportionately affect vulnerable populations.
How does continuous enrollment impact healthcare access?
While continuous enrollment aims to improve access by reducing paperwork and simplifying the process, decreased spending could ironically hinder access if it results in service cuts or provider shortages.
Are there any ethical considerations related to decreased Medicaid spending?
Yes, ensuring equitable access to healthcare is a critical ethical concern. Decreased spending raises questions about whether vulnerable populations are disproportionately affected and whether access to necessary care is compromised.





