
Strategies to Manage Tourette Syndrome in Children
Strategies to manage Tourette Syndrome in children are crucial for helping kids thrive. This isn’t just about managing tics; it’s about understanding the whole child – their emotional well-being, academic success, and social interactions. We’ll explore a range of approaches, from behavioral therapies and educational adjustments to medical interventions and lifestyle changes, all aimed at empowering children and their families.
Navigating Tourette Syndrome can feel overwhelming, but with the right knowledge and support, families can find effective strategies to help their children manage their symptoms and lead fulfilling lives. This post delves into the multifaceted aspects of managing Tourette’s in children, providing practical advice and resources to guide you on this journey.
Understanding Tourette Syndrome in Children
Tourette Syndrome (TS) is a neurological disorder characterized by involuntary, repetitive movements and vocalizations called tics. While it can significantly impact a child’s life, understanding the condition is the first step towards effective management and support. This section will explore the key aspects of TS in children, providing a clearer picture of this often misunderstood condition.
Types of Tics Associated with Tourette Syndrome
Tics are the hallmark of Tourette Syndrome. They are classified into two main categories: motor tics and phonic (vocal) tics. Motor tics range from simple movements like eye blinking or shoulder shrugging to more complex actions such as touching objects repeatedly or making unusual gestures. Phonic tics can include simple sounds like throat clearing or sniffing, or more complex vocalizations such as grunting, shouting words or phrases, or even repeating heard sounds (echolalia).
It’s important to note that the severity and types of tics can vary significantly between individuals and even fluctuate over time within the same individual. A child might experience a range of tics throughout the day, with some tics appearing more frequently than others.
Typical Age of Onset and Developmental Trajectory
Tourette Syndrome typically begins in childhood, most often between the ages of 4 and 6 years old. The onset is usually gradual, with tics initially appearing as simple motor movements. Over time, the tics may become more complex and/or vocal tics may develop. The severity of tics often peaks during adolescence and then tends to lessen in severity as the individual enters adulthood, though some tics may persist.
The developmental trajectory is not uniform; some individuals experience a significant reduction in tic severity, while others continue to experience noticeable tics throughout their lives. For example, a child might initially exhibit only eye blinking, which might later progress to include throat clearing and then eventually evolve to include more complex motor movements and vocalizations before gradually lessening in frequency and intensity.
Common Comorbidities Associated with Tourette Syndrome in Children
Tourette Syndrome frequently co-occurs with other conditions, often referred to as comorbidities. These can include Attention-Deficit/Hyperactivity Disorder (ADHD), obsessive-compulsive disorder (OCD), oppositional defiant disorder (ODD), anxiety disorders, and learning disabilities. The presence of these comorbidities can significantly impact a child’s academic performance, social interactions, and overall well-being. For instance, a child with TS and ADHD might struggle with impulsivity and inattention in the classroom, while a child with TS and OCD might experience significant distress from repetitive rituals and intrusive thoughts.
Understanding and managing these co-occurring conditions is crucial for comprehensive care.
Comparison of Tourette Syndrome with Other Similar Conditions
Differentiating Tourette Syndrome from other conditions with similar symptoms is important for accurate diagnosis and treatment. The following table compares TS with some other conditions that might present with overlapping symptoms:
| Condition | Tic Severity | Other Symptoms | Onset |
|---|---|---|---|
| Tourette Syndrome | Multiple motor and at least one vocal tic, present for at least one year | ADHD, OCD, anxiety, learning disabilities | Typically before age 18 |
| Chronic Motor Tic Disorder | Multiple motor tics, but no vocal tics, present for at least one year | May co-occur with other conditions, but less frequently than in TS | Typically before age 18 |
| Chronic Vocal Tic Disorder | Multiple vocal tics, but no motor tics, present for at least one year | May co-occur with other conditions, but less frequently than in TS | Typically before age 18 |
| Transient Tic Disorder | Single or multiple motor and/or vocal tics, lasting less than one year | Generally resolves without treatment | Typically before age 18 |
Behavioral Management Strategies: Strategies To Manage Tourette Syndrome In Children
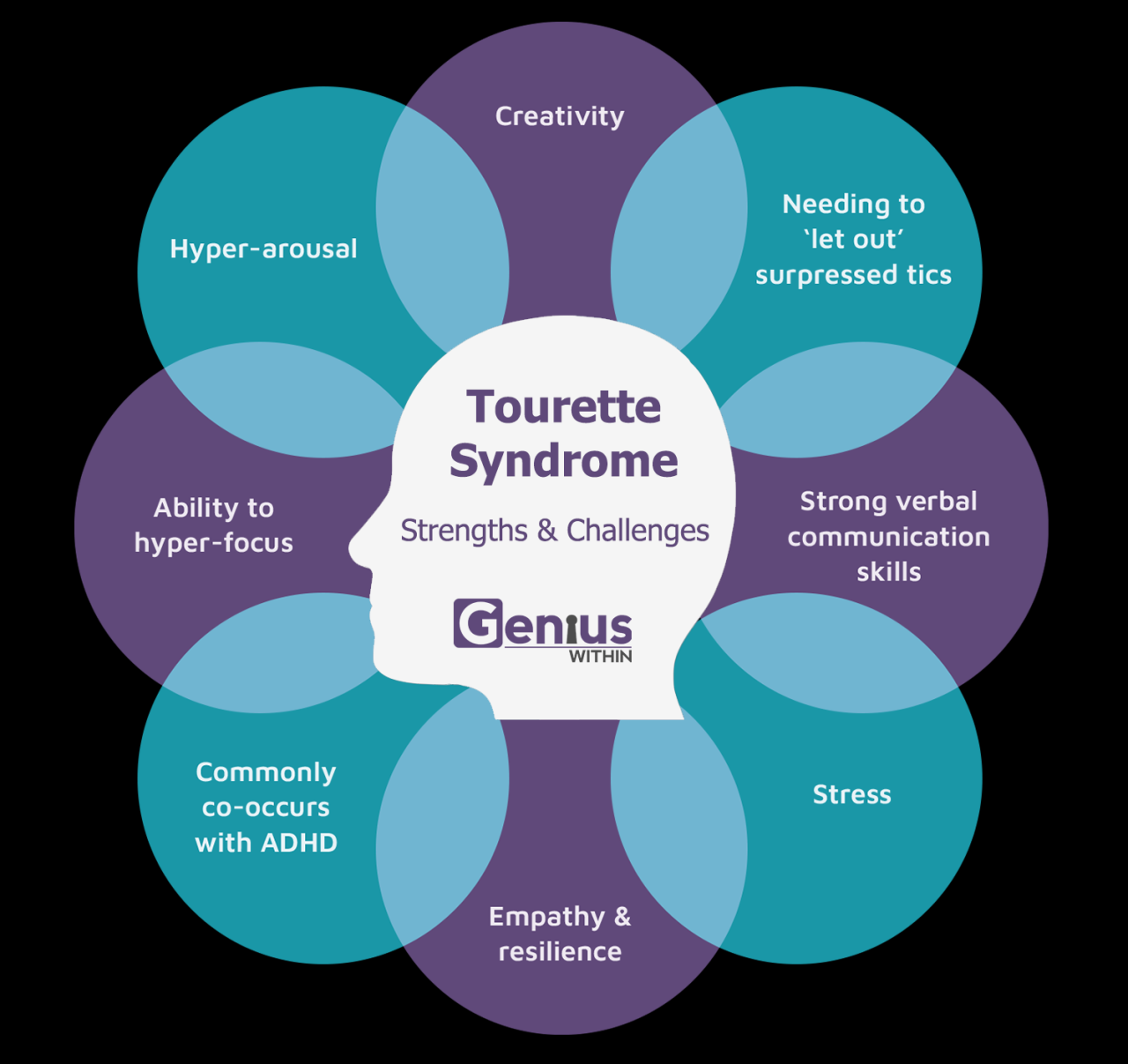
Source: geniuswithin.org
Behavioral therapies offer powerful tools for managing Tourette Syndrome in children. These strategies focus on modifying behaviors associated with tics, improving coping mechanisms, and enhancing the child’s overall quality of life. By understanding and implementing these techniques, parents and caregivers can significantly reduce tic severity and improve their child’s well-being.
Positive Reinforcement Techniques for Tic Management
Positive reinforcement is a cornerstone of effective tic management. Instead of focusing on punishing tics, this approach rewards desired behaviors, making them more likely to occur. For example, if a child successfully resists a tic for a specific period, they might receive praise, a small reward, or extra screen time. Consistency is key; rewards should be delivered immediately after the desired behavior.
This reinforces the connection between the behavior and the positive consequence. The rewards should be tailored to the child’s individual preferences and age appropriateness, ensuring motivation remains high. For instance, a younger child might respond well to stickers, while an older child might prefer extra playtime or a small allowance.
Habit Reversal Training (HRT) for Reducing Tic Frequency and Severity
Habit Reversal Training is a comprehensive behavioral therapy that combines several techniques to reduce tic frequency and severity. It typically involves four key steps: awareness training (identifying tic precursors), competing response training (developing a different behavior to replace the tic), relaxation training (managing stress and anxiety that can exacerbate tics), and social support (involving family and friends in the process).
For example, a child with a shoulder shrug tic might be taught to consciously relax their shoulders and perform a competing response like gently massaging them. The goal is not to eliminate tics entirely, but to reduce their frequency and impact on daily life. HRT requires consistent practice and often involves collaboration between therapists, parents, and the child.
Relaxation and Stress Management Techniques for Children with Tourette Syndrome
Stress and anxiety can significantly worsen tic symptoms. Therefore, teaching children relaxation techniques is crucial. Deep breathing exercises, progressive muscle relaxation (systematically tensing and releasing muscle groups), and mindfulness meditation are all effective methods. Visualisation techniques, where the child creates calming mental images, can also be beneficial. These techniques can be integrated into daily routines, such as before bedtime or before situations that typically trigger tics.
A calming environment, regular exercise, and sufficient sleep also play vital roles in stress reduction. For example, a child might practice deep breathing for five minutes before school each morning.
A Structured Behavioral Intervention Plan
A structured behavioral intervention plan (BIP) provides a framework for managing tics effectively. This plan should be individualized to the child’s specific needs and tics.
Helping kids manage Tourette Syndrome often involves a multi-pronged approach, including behavioral therapies and sometimes medication. It’s fascinating to consider how early detection of neurological conditions can improve outcomes, which made me think about research into detecting other conditions early, like the intriguing question of whether can eye test detect dementia risk in older adults. Understanding the potential for early intervention in diverse neurological conditions, like this eye test for dementia, highlights the importance of ongoing research across the spectrum of neurological disorders and how this might inform future approaches to Tourette’s management.
| Goal | Strategy | Evaluation Method |
|---|---|---|
| Reduce the frequency of eye blinking tics by 50% within 8 weeks. | Implement Habit Reversal Training focusing on competing response (e.g., gently squeezing a stress ball) and positive reinforcement (e.g., sticker chart for successful tic suppression). | Weekly tic counts recorded by parents and therapist; review of progress at weekly therapy sessions. |
| Improve coping skills in stressful situations to minimize tic exacerbation. | Teach relaxation techniques (deep breathing, progressive muscle relaxation) and mindfulness exercises. Role-playing stressful situations. | Observation of child’s response to stressful situations; self-report of stress levels and tic frequency using a daily log. |
| Increase the child’s self-awareness of tic precursors. | Utilize video recordings of tics to identify precursor behaviors. Engage in journaling to record situations that trigger tics. | Review of video recordings and journal entries; parent and therapist feedback on the child’s self-awareness. |
Educational Interventions and Support
Navigating the educational landscape for a child with Tourette Syndrome requires a multifaceted approach that prioritizes understanding, inclusion, and individualized support. Successful academic progress hinges on creating a learning environment that acknowledges the unique challenges presented by the condition while fostering the child’s strengths and potential. This involves collaboration between parents, teachers, and healthcare professionals to develop a comprehensive plan tailored to the child’s specific needs.Creating an inclusive and supportive classroom environment is crucial for children with Tourette Syndrome.
The classroom should be a place where tics are accepted as part of the child’s neurology, not as a behavioral issue requiring punishment. Educators play a vital role in educating their peers about Tourette Syndrome, promoting understanding and empathy, and minimizing potential teasing or stigmatization. A calm and organized classroom environment, with clear routines and expectations, can significantly reduce tic severity for many children.
Flexible seating arrangements, allowing the child to move around if needed, can also be beneficial.
Classroom Accommodations and Modifications
Effective accommodations and modifications can significantly improve a child’s academic performance. These adjustments should be tailored to the specific challenges the child faces, such as difficulty with attention, impulsivity, or motor control. For example, a child struggling with writing might benefit from using a laptop or assistive technology. Allowing extra time for tests and assignments can alleviate pressure and improve accuracy.
Breaking down large tasks into smaller, more manageable steps can improve focus and reduce feelings of overwhelm. Visual aids, such as checklists and graphic organizers, can assist with organization and memory. Providing a quiet space for breaks or sensory regulation can help the child manage tics and maintain focus. In some cases, preferential seating away from distractions might be beneficial.
The key is to work collaboratively with the child, parents, and healthcare professionals to identify strategies that are effective and practical.
Collaboration Between Parents, Educators, and Healthcare Professionals
Effective management of Tourette Syndrome in the school setting requires a strong partnership between parents, educators, and healthcare professionals. Open communication is vital. Parents can provide valuable insights into their child’s triggers, coping mechanisms, and individual needs. Educators can observe the child’s behavior in the classroom and provide feedback on the effectiveness of interventions. Healthcare professionals can offer medical expertise and guidance on medication management and other therapeutic approaches.
Regular meetings and collaborative planning sessions are essential to ensure that the child’s educational plan is consistently updated and adjusted as needed. This team approach allows for a holistic and supportive approach to the child’s education and well-being. A shared understanding of the condition and a commitment to working together are crucial for success.
Resources and Support Systems for Children with Tourette Syndrome and Their Families
Access to appropriate resources and support systems is essential for families navigating the challenges of Tourette Syndrome.
- The Tourette Association of America (TAA): Offers information, support groups, and resources for families and individuals affected by Tourette Syndrome.
- The National Institute of Neurological Disorders and Stroke (NINDS): Provides research-based information on Tourette Syndrome and related disorders.
- Local support groups and organizations: Many communities have local support groups that offer peer-to-peer support and resources for families.
- School psychologists and special education teachers: These professionals can provide valuable support and guidance in developing individualized education plans (IEPs) and implementing accommodations in the classroom.
- Pediatricians and neurologists specializing in Tourette Syndrome: These healthcare professionals can provide medical care and guidance on medication and other treatments.
Medical Management Approaches

Source: healthyplace.com
Tourette Syndrome (TS) often requires a multifaceted approach to management, and medication plays a significant role for many children. While not a cure, medication can effectively reduce the severity and frequency of tics, improving a child’s quality of life and allowing them to better participate in school and social activities. The decision to use medication, and which medication to use, is made in consultation with a physician specializing in neurology or child psychiatry, taking into account the child’s specific symptoms, age, and overall health.Medication’s role in managing TS focuses primarily on reducing tic severity.
This can involve lessening the frequency, intensity, or both, of motor and phonic tics. The goal isn’t always complete tic suppression, but rather to achieve a level of control that minimizes disruption to the child’s daily life and allows for better functioning. It’s important to remember that medication effectiveness varies significantly between individuals, and finding the right medication and dosage can be a process requiring time and adjustment.
Types of Medications Used to Treat Tourette Syndrome
Several classes of medications are commonly used to treat TS. These medications work through different mechanisms in the brain, impacting neurotransmitter systems believed to be involved in tic development. The choice of medication depends on various factors including the severity of symptoms, the presence of co-occurring conditions (such as ADHD or OCD), and the child’s individual response to treatment.
It’s crucial to work closely with a healthcare professional to find the most effective and safe approach.
Alpha-2 Adrenergic Agonists
Alpha-2 adrenergic agonists, such as clonidine and guanfacine, are often used as first-line treatments for TS, particularly in younger children. These medications can help reduce both motor and phonic tics by affecting neurotransmitters in the brain. While generally well-tolerated, potential side effects can include drowsiness, low blood pressure, and fatigue. Careful monitoring is necessary, especially in children.
Antipsychotics
Atypical antipsychotics, such as risperidone and aripiprazole, are sometimes used to manage more severe tics or those that haven’t responded to other treatments. These medications can be effective in reducing tic severity but carry a higher risk of side effects compared to alpha-2 agonists. These potential side effects can include weight gain, metabolic changes, and movement disorders. Regular monitoring for these side effects is essential.
Comparing Medication Approaches
Alpha-2 adrenergic agonists generally have a milder side effect profile than atypical antipsychotics, making them a preferable first-line treatment option for many children. However, they may be less effective in managing severe tics. Atypical antipsychotics are reserved for cases where other medications have proven insufficient, due to their potential for more significant side effects. The decision of which medication to use, or whether to use medication at all, is a collaborative one between the child, their parents, and their healthcare provider.
Individual responses vary greatly, and a trial-and-error approach is often necessary to find the optimal treatment plan.
Commonly Prescribed Medications: Benefits and Side Effects
| Medication | Class | Potential Benefits | Potential Side Effects |
|---|---|---|---|
| Clonidine | Alpha-2 adrenergic agonist | Reduces tic frequency and severity, improves sleep | Drowsiness, low blood pressure, fatigue, dizziness |
| Guanfacine | Alpha-2 adrenergic agonist | Reduces tic frequency and severity, may improve attention | Drowsiness, low blood pressure, fatigue, irritability |
| Risperidone | Atypical antipsychotic | Significant reduction in tic severity in some cases | Weight gain, metabolic changes, increased risk of type 2 diabetes, movement disorders (tardive dyskinesia) |
| Aripiprazole | Atypical antipsychotic | Reduces tic severity, may improve other symptoms like irritability | Weight gain, anxiety, insomnia, akathisia (restlessness) |
Lifestyle Factors and Considerations
Managing Tourette Syndrome (TS) in children isn’t solely about medication and therapy; lifestyle plays a significant role in managing tic severity and improving overall well-being. A holistic approach, incorporating healthy habits, can significantly impact a child’s quality of life and ability to cope with their condition. This section explores the crucial connection between lifestyle choices and TS management.
Sleep Hygiene and Tic Severity
Sufficient sleep is paramount for children, especially those with TS. Sleep deprivation can exacerbate tics, leading to increased frequency and intensity. A consistent sleep schedule, a relaxing bedtime routine, and a comfortable sleep environment are crucial. Creating a calming atmosphere, avoiding screen time before bed, and ensuring the child gets enough hours of sleep (typically 9-11 hours for school-aged children) can make a noticeable difference in tic control.
Lack of sleep can also impact mood regulation, making anxiety and irritability more pronounced, which in turn can worsen tics. Parents should monitor their child’s sleep patterns and address any sleep disturbances promptly.
Nutrition and Tic Control, Strategies to manage tourette syndrome in children
While there’s no specific diet proven to cure TS, a healthy, balanced diet can contribute to overall well-being and potentially influence tic severity. A diet rich in fruits, vegetables, whole grains, and lean protein provides the necessary nutrients for brain function and overall health. Limiting processed foods, sugary drinks, and artificial additives, which can sometimes contribute to hyperactivity and irritability, is advisable.
Regular meals and snacks can help maintain stable blood sugar levels, preventing energy crashes that might trigger or worsen tics. Individual responses to different foods vary, so parents should observe their child’s diet and identify any potential triggers or sensitivities. Working with a registered dietitian or nutritionist can provide personalized dietary guidance.
The Importance of Regular Physical Activity
Regular physical activity offers numerous benefits for children with TS, extending beyond just physical health. Exercise acts as a natural stress reliever, helping to reduce anxiety and improve mood. The release of endorphins during physical activity can have a calming effect, potentially lessening tic severity. Moreover, exercise promotes better sleep, contributing to improved tic control. Activities like swimming, cycling, team sports, or even simple playtime can be highly beneficial.
Finding activities the child enjoys is key to ensuring consistent participation. The goal isn’t intense athletic training but rather regular, moderate-intensity physical activity.
Stress Management Techniques for Children with TS
Stress and anxiety can significantly worsen tics. Teaching children coping mechanisms for stress is crucial. Techniques such as deep breathing exercises, mindfulness practices (like meditation or yoga), and progressive muscle relaxation can be effective. Cognitive behavioral therapy (CBT) can also be highly beneficial in teaching children to identify and manage stressful situations. Creating a supportive and understanding environment at home and school is equally important in reducing stress levels.
Encouraging open communication and providing emotional support can significantly alleviate anxiety. Family therapy can help the entire family learn effective coping strategies.
Healthy Lifestyle Choices for Overall Well-being
A holistic approach to managing TS involves integrating several healthy lifestyle choices. Here are some examples:
- Prioritize sleep: Aim for a consistent sleep schedule and create a relaxing bedtime routine.
- Eat a balanced diet: Focus on whole, unprocessed foods, limiting sugary drinks and processed snacks.
- Engage in regular physical activity: Find enjoyable activities that promote movement and fitness.
- Practice stress management techniques: Incorporate deep breathing, mindfulness, or relaxation exercises.
- Maintain social connections: Foster strong relationships with family, friends, and peers.
- Seek professional support: Work with a multidisciplinary team including doctors, therapists, and educators.
Long-Term Outlook and Support
Living with Tourette Syndrome (TS) is a journey, and understanding its long-term trajectory is crucial for families and individuals alike. While TS’s severity can fluctuate throughout life, many children experience a significant reduction in tic severity during adolescence and adulthood. This doesn’t mean the tics disappear entirely; rather, they often become less frequent, less intense, or more manageable.
However, a small percentage of individuals continue to experience significant tic symptoms into adulthood, highlighting the importance of ongoing support and management.The developmental trajectory of TS is highly individual. Some children may experience a peak in tic severity around the onset of puberty, followed by a gradual decline. Others may see more consistent symptom levels throughout their development.
Factors like stress, sleep deprivation, and underlying medical conditions can significantly influence the severity and frequency of tics. It’s essential to remember that TS is not a progressive neurological disease; it’s a neurodevelopmental condition, meaning the underlying condition itself doesn’t worsen over time, although the symptoms may vary in intensity and presentation.
Developmental Trajectory of Tourette Syndrome
The typical developmental trajectory often involves an initial onset of motor tics (simple repetitive movements), followed by the emergence of phonic tics (vocalizations). The severity and frequency of tics typically peak during childhood, often around ages 10-12. Many individuals experience a significant reduction in tic severity during adolescence, with some experiencing a near-complete remission of symptoms by adulthood.
However, a substantial number of individuals continue to experience some level of tics, though often less disruptive than in childhood. For example, a child who experiences frequent, disruptive shouting tics might, in adulthood, experience occasional throat clearing or eye blinking. The specific pattern of symptom changes varies widely between individuals.
Ongoing Monitoring and Support
Regular monitoring by a healthcare professional is crucial throughout a person’s life with TS. This includes regular check-ups with a neurologist or psychiatrist specializing in TS to assess tic severity, evaluate the effectiveness of current treatments, and adjust the treatment plan as needed. Ongoing monitoring helps identify any emerging comorbidities (other conditions often associated with TS, such as ADHD or OCD) that may require additional support.
Furthermore, regular communication between the healthcare provider, the child, their parents/guardians, and educators ensures a coordinated and comprehensive approach to management. For instance, regular check-ins could help identify triggers for increased tic severity, allowing for proactive adjustments to the child’s routine or treatment.
Fostering Self-Esteem and Independence
Building self-esteem and promoting independence are vital aspects of supporting children with TS. Creating a supportive and understanding environment at home and school is paramount. Educating family members, friends, and teachers about TS helps reduce stigma and fosters acceptance. Encouraging participation in activities and hobbies that the child enjoys, regardless of their tics, promotes a sense of accomplishment and self-worth.
Positive reinforcement and focusing on the child’s strengths, rather than their challenges, build confidence. For example, celebrating a child’s artistic talent or athletic ability, even if their performance is affected by tics, reinforces their self-worth.
Creating a Personalized Support Plan
Developing a personalized support plan is essential for each child with TS. This plan should be collaborative, involving the child, their parents/guardians, healthcare providers, educators, and other relevant professionals. The plan should address the child’s specific needs and challenges, encompassing medical management, behavioral interventions, educational accommodations, and social support. The plan should be regularly reviewed and updated to reflect the child’s changing needs and the effectiveness of interventions.
For instance, a child struggling with social anxiety due to their tics might benefit from social skills training and peer support groups, while a child experiencing academic challenges might need individualized education plans and assistive technology. The plan should also include strategies for managing stress and promoting overall well-being.
Concluding Remarks
Successfully managing Tourette Syndrome in children requires a holistic approach, combining medical interventions, behavioral strategies, and supportive environments. Remember, every child is unique, and what works for one might not work for another. Open communication with healthcare professionals, educators, and therapists is key to developing a personalized plan that addresses the child’s specific needs and fosters their overall well-being.
This journey is a marathon, not a sprint, and with consistent effort and support, children with Tourette Syndrome can flourish.
Essential Questionnaire
What is the difference between simple and complex tics?
Simple tics are brief, sudden movements or sounds (e.g., eye blinking, throat clearing). Complex tics involve a sequence of movements or sounds (e.g., touching objects repeatedly, making a series of vocalizations).
Does Tourette Syndrome always involve coprolalia (swearing)?
No, coprolalia is a relatively rare symptom of Tourette Syndrome. Many individuals with Tourette’s do not experience this.
My child is struggling socially. How can we help?
Social skills training, peer support groups, and open communication with school staff can help children with Tourette’s navigate social situations. Educating peers about the condition can also reduce stigma and improve social acceptance.
Are there support groups for families of children with Tourette Syndrome?
Yes, many organizations offer support groups and online communities for families affected by Tourette Syndrome. These groups provide a valuable opportunity to connect with others facing similar challenges and share experiences and coping strategies.
