
Texas Emergency Abortion, Ectopic Pregnancy, EMTALA Complaints
Texas emergency abortion ectopic pregnancy emtala complaints – Texas emergency abortion, ectopic pregnancy, and EMTALA complaints highlight a complex intersection of state law, federal regulations, and patient rights. The restrictive Texas abortion laws clash directly with the federal Emergency Medical Treatment and Labor Act (EMTALA), which mandates stabilizing treatment for all patients regardless of their ability to pay. This creates a critical situation for women experiencing ectopic pregnancies or other life-threatening conditions requiring immediate abortion care.
The resulting legal and ethical dilemmas faced by both patients and healthcare providers are significant and far-reaching, leading to numerous complaints and ongoing legal battles.
This post delves into the intricacies of this contentious issue, examining the legal landscape in Texas, the application of EMTALA in emergency abortion cases, the challenges faced by patients, the ethical considerations for healthcare providers, and the analysis of complaints filed regarding EMTALA violations. We’ll explore real-world scenarios, examine legal precedents, and offer a comprehensive overview of this critical healthcare access debate.
Texas Law and Emergency Abortion Access: Texas Emergency Abortion Ectopic Pregnancy Emtala Complaints

Source: winnipegfreepress.com
Navigating the legal landscape surrounding abortion in Texas is complex, particularly when considering emergency situations. The state’s restrictive abortion laws, while generally prohibiting most abortions after six weeks of pregnancy, contain exceptions designed to protect the life and health of the pregnant person. Understanding these exceptions and their practical implications is crucial.
Emergency Abortion Exceptions in Texas Law
Texas law allows for abortions when necessary to save the life or preserve the health of the pregnant person. This exception is broadly interpreted to encompass situations where continuing the pregnancy poses a serious risk of death or substantial impairment of a major bodily function. This includes cases of ectopic pregnancies, where the fertilized egg implants outside the uterus, a life-threatening condition requiring immediate medical intervention.
The law does not explicitly define “substantial impairment,” leaving room for medical judgment in determining the necessity of an abortion. However, the lack of clear definitions and the potential for legal challenges create uncertainty for both medical providers and patients.
Comparison with Other States’ Emergency Medical Care Laws
Texas’s approach to emergency abortion access contrasts sharply with many other states. While some states have similar “life and health” exceptions, the enforcement and interpretation of these exceptions can vary widely. Some states have enacted laws explicitly protecting the right to emergency abortion care, ensuring that healthcare providers are not penalized for providing medically necessary abortions. In contrast, Texas’s restrictive environment creates a chilling effect, potentially leading to delays in treatment or providers refusing care out of fear of legal repercussions.
This difference highlights the significant disparities in access to essential healthcare across the United States.
The ongoing debate surrounding Texas emergency abortion access, especially for ectopic pregnancies and EMTALA complaints, is incredibly stressful. I’ve been feeling the pressure in my wrists lately, and honestly, I’ve been looking into alternative treatments like those outlined in this helpful article on ways to treat carpal tunnel syndrome without surgery , hoping to find some relief.
The emotional toll of fighting for reproductive rights is exhausting, and I need to prioritize my own well-being amidst this fight.
Legal Requirements and Penalties for Emergency Abortion Care in Texas
The following table Artikels the key legal aspects related to providing and seeking emergency abortion care in Texas. It’s important to note that this information is for general understanding and should not be considered legal advice. Consult with a legal professional for specific guidance.
| Action | Legal Requirement | Potential Penalty (for providers) | Potential Penalty (for patients) |
|---|---|---|---|
| Providing Emergency Abortion | Must be medically necessary to save the life or preserve the health of the pregnant person; must comply with all other applicable state laws (e.g., reporting requirements). | Criminal penalties (felony charges, fines, imprisonment), civil lawsuits, loss of medical license. Penalties can vary significantly depending on the specific circumstances. | Generally, no penalties for the patient seeking necessary medical care. |
| Seeking Emergency Abortion | The patient must present with a life-threatening condition requiring immediate medical intervention. | None | None |
| Reporting Requirements | Physicians are required to report certain medical information, potentially including abortions, to state authorities. | Failure to report can result in fines and other penalties. | N/A |
EMTALA and its Application in Texas Abortion Cases
The Emergency Medical Treatment and Labor Act (EMTALA) is a federal law mandating that hospitals participating in Medicare provide stabilizing treatment to any individual who comes to the emergency room regardless of their ability to pay or insurance status. This seemingly straightforward principle becomes significantly complex when applied to the context of abortion care in states like Texas, where restrictive abortion laws exist.
Understanding the interplay between EMTALA and state-level abortion restrictions is crucial for ensuring appropriate medical care in emergency situations.EMTALA’s Application to Ectopic Pregnancies and Emergency Abortion CareEMTALA’s application to ectopic pregnancies is particularly relevant. An ectopic pregnancy, where a fertilized egg implants outside the uterus, is a life-threatening medical emergency requiring immediate intervention. Often, this intervention involves medication or surgery to remove the pregnancy, a procedure that many consider an abortion.
The ongoing debate around Texas emergency abortion access, particularly for ectopic pregnancies and EMTALA complaints, highlights the complexities of healthcare in a crisis. This is further complicated by financial instability in some hospital systems; for example, the recent news that Steward Health Care secured financing to avoid bankruptcy raises concerns about potential impacts on patient care, especially given the already strained resources dedicated to emergency reproductive healthcare in Texas.
The financial health of hospitals directly impacts their ability to provide timely and appropriate care, influencing the outcome of EMTALA complaints related to abortion access.
In Texas, where abortion access is severely limited, the potential conflict between state law and federal EMTALA mandates becomes stark. The necessity to provide stabilizing treatment under EMTALA can directly contradict state laws restricting abortion access, creating a legal and ethical dilemma for healthcare providers.Potential Conflicts Between Texas Abortion Laws and EMTALAThe conflict arises from the fact that Texas’s abortion laws significantly restrict access to abortion care, even in medical emergencies.
While EMTALA requires stabilizing treatment, including potentially abortion-related procedures, to prevent death or serious harm, Texas law may create obstacles to providing this care. For instance, Texas law might require certain waiting periods, parental consent (for minors), or other restrictions that would delay or prevent necessary medical intervention, directly violating EMTALA’s mandate for immediate stabilization. This creates a situation where healthcare providers must navigate potentially conflicting legal obligations, risking legal repercussions regardless of their actions.Examples of Potential ConflictsConsider a hypothetical scenario: A woman presents to a Texas emergency room with a ruptured ectopic pregnancy, a condition that requires immediate surgical intervention to save her life.
However, the hospital, fearing legal repercussions under Texas abortion law, delays or refuses to perform the necessary procedure. This delay could lead to severe complications, even death, directly violating EMTALA’s requirement to provide stabilizing treatment. Another example could involve a woman experiencing a miscarriage with severe complications requiring intervention to prevent life-threatening hemorrhage. If Texas law restricts the type of intervention necessary to stabilize the patient, the hospital could be in violation of EMTALA.
The legal gray area created by these conflicting laws puts both patients and healthcare providers in precarious positions.
Patient Experiences and Challenges
Navigating the Texas healthcare system to access emergency abortion care, particularly in cases of ectopic pregnancy, presents significant challenges for patients. The restrictive legal environment, coupled with logistical hurdles, creates a complex and often traumatic experience for those seeking essential medical treatment. These obstacles can lead to significant delays in care, resulting in potentially life-threatening consequences.The impact of delays in receiving necessary care for ectopic pregnancies is profoundly serious.
Ectopic pregnancies, where a fertilized egg implants outside the uterus, are life-threatening if left untreated. A delay in diagnosis and treatment can lead to a rupture of the fallopian tube, causing internal bleeding, severe pain, and even death. The longer the delay, the greater the risk of these severe complications. Early intervention is crucial for preserving the patient’s health and fertility.
Obstacles to Accessing Emergency Abortion Services in Texas
The restrictive legal landscape in Texas significantly impacts a patient’s ability to access timely and appropriate care. Many obstacles arise at various stages of the process, creating a cascade of difficulties that can delay or even prevent necessary treatment.
- Navigating Legal Restrictions: The Texas legislature has enacted numerous laws restricting abortion access, including mandatory waiting periods, parental consent requirements for minors, and limitations on the types of facilities that can provide abortion services. These regulations create unnecessary barriers for patients already facing a medical emergency.
- Finding a Willing Provider: Due to the restrictive laws and potential legal repercussions, many healthcare providers in Texas are hesitant or unwilling to provide abortion care, even in emergency situations. This scarcity of providers forces patients to travel long distances, often incurring significant costs and delays.
- Financial Barriers: The cost of medical care, including transportation, accommodation, and medical procedures, can be prohibitive for many Texans. The lack of insurance coverage or inadequate financial resources can prevent patients from accessing necessary care, even when it’s medically necessary.
- Lack of Information and Support: Patients may struggle to find accurate and reliable information about their options and available resources. The stigma surrounding abortion further complicates the process, making it difficult for patients to seek help and support.
- Time Constraints: The time-sensitive nature of ectopic pregnancies necessitates immediate medical attention. Delays caused by navigating legal and logistical barriers can have life-threatening consequences.
Hypothetical Case Study: Navigating the Texas Healthcare System
Imagine Maria, a 30-year-old woman experiencing severe abdominal pain. She suspects an ectopic pregnancy, but finding a doctor willing to confirm her diagnosis and provide treatment proves incredibly difficult. She initially visits her local clinic, but the physician refuses to perform the necessary tests or refer her to a specialist, citing concerns about legal ramifications. Maria spends days searching online for providers who will treat her, facing numerous dead ends and experiencing escalating pain.
Eventually, she travels hundreds of miles to a larger city, incurring substantial travel and accommodation expenses. The delay in receiving appropriate care leads to a ruptured fallopian tube, resulting in emergency surgery and a lengthy recovery period. This scenario highlights the devastating consequences of restrictive abortion laws and the numerous obstacles faced by patients in Texas seeking essential medical care.
Healthcare Provider Perspectives and Responsibilities
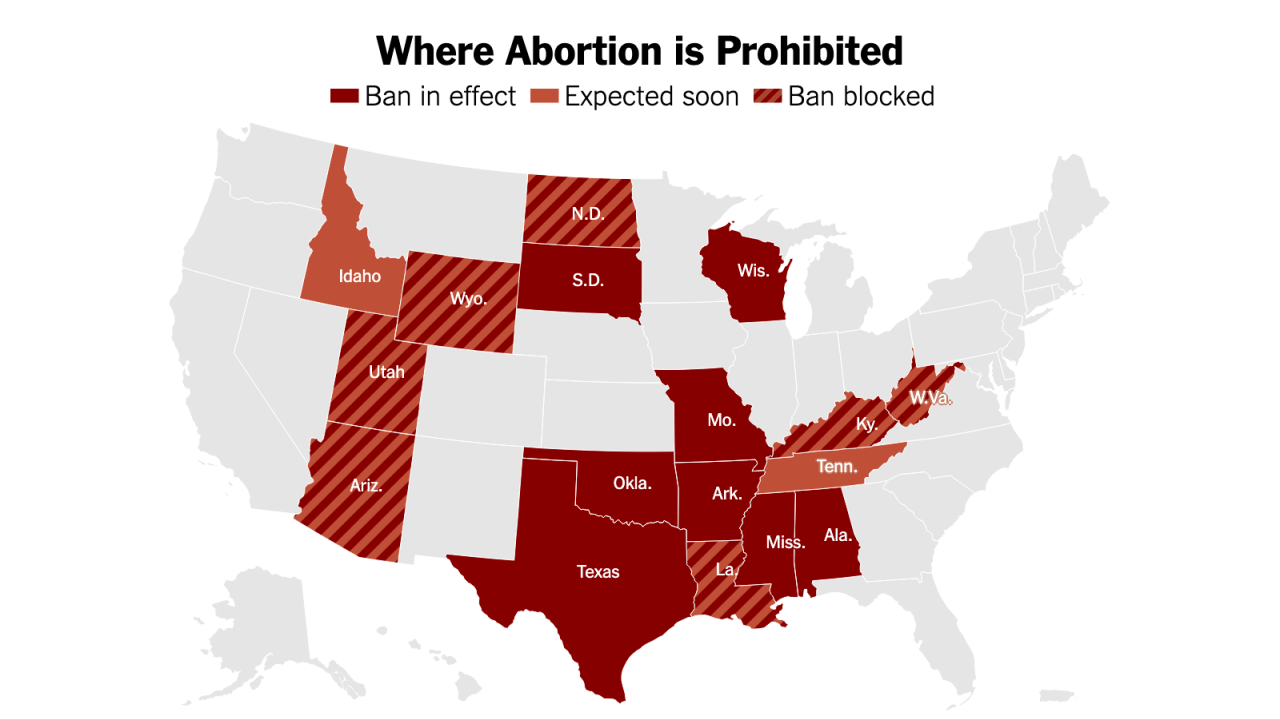
Source: nyt.com
The current legal landscape surrounding abortion in Texas presents significant ethical and legal dilemmas for healthcare providers. Navigating the complexities of state laws, particularly in emergency situations, necessitates a careful understanding of both the letter and the spirit of the law, while simultaneously upholding the ethical obligation to provide appropriate medical care. The potential consequences for non-compliance are severe, impacting not only the provider’s professional license but also potentially leading to criminal charges.The ethical dilemmas faced by Texas healthcare providers center on the conflict between their professional responsibility to provide the best possible care for their patients and the restrictions imposed by state abortion laws.
In cases of ectopic pregnancies or other life-threatening conditions requiring abortion procedures, providers must weigh the potential risks of delaying or denying treatment against the legal repercussions of performing an abortion that may not meet the narrow exceptions Artikeld in Texas law. This creates an agonizing situation, forcing healthcare professionals to make decisions with potentially life-altering consequences for both themselves and their patients.
Legal Consequences for Violating Texas Abortion Laws, Texas emergency abortion ectopic pregnancy emtala complaints
Healthcare providers in Texas who violate the state’s abortion laws, even in emergency situations, face significant legal consequences. These can range from the suspension or revocation of their medical license to criminal charges, including felony indictments and substantial fines or imprisonment. The legal ramifications are particularly severe in cases where the prosecution can demonstrate a deliberate disregard for the law or a pattern of non-compliance.
The threat of legal action creates a climate of fear and uncertainty, potentially discouraging providers from offering necessary care, even when it is medically indicated. This chilling effect can significantly impact access to essential healthcare services for women in Texas.
Perspectives of Different Healthcare Professionals
The perspectives of various healthcare professionals regarding their responsibilities under EMTALA and Texas law concerning emergency abortion care differ based on their roles and training. Physicians, for instance, often bear the primary responsibility for making medical decisions and may face greater legal risk. Nurses, while not directly making the final decisions, play a critical role in providing care and support to both the patient and the physician, potentially facing legal repercussions for complicity.
EMTs, on the other hand, primarily focus on stabilizing the patient and transporting them to appropriate facilities, but they too are bound by EMTALA and must ensure patients receive necessary emergency care. The differing legal vulnerabilities and professional responsibilities create a complex web of considerations for each healthcare professional involved in such cases.
Support Systems and Resources for Healthcare Providers
Given the immense pressure and potential legal risks involved, support systems and resources are crucial for healthcare providers in Texas navigating these challenging situations. Professional organizations such as the Texas Medical Association and the American College of Obstetricians and Gynecologists offer guidance, legal counsel, and peer support. Additionally, some hospitals and healthcare systems may provide internal resources, such as legal teams or ethics committees, to assist providers in making informed decisions and navigating legal complexities.
Access to these support systems, however, may vary significantly depending on the individual provider’s circumstances and their employing institution’s policies. The availability and accessibility of such support remain critical factors in ensuring that providers can continue to offer safe and ethical care to their patients.
Analysis of Complaints Filed Regarding EMTALA Violations
EMTALA, the Emergency Medical Treatment and Active Labor Act, is designed to prevent patient dumping—the practice of refusing to treat or transferring patients based on their inability to pay or other discriminatory factors. In the context of Texas’s restrictive abortion laws, EMTALA complaints have become increasingly significant, alleging that hospitals are violating the law by delaying or denying emergency care related to pregnancy complications, including ectopic pregnancies and miscarriages.
Analyzing these complaints reveals crucial patterns and challenges in ensuring access to timely and appropriate medical care.
Key Themes and Issues in EMTALA Complaints
Complaints filed against Texas healthcare facilities regarding EMTALA violations in the context of abortion care frequently center on allegations of delays in treatment for emergency medical conditions related to pregnancy. These delays often involve unnecessary waiting periods, requests for additional testing or consultations that delay necessary care, and the transfer of patients to facilities not equipped to handle their medical needs.
A common theme is the assertion that healthcare providers prioritize adherence to Texas’s abortion restrictions over the immediate medical needs of the patient, potentially leading to severe health consequences or even death. Another recurring issue involves the lack of clear and consistent protocols for handling emergency situations involving pregnancy complications, leaving patients vulnerable to inconsistent care and potential violations of EMTALA.
The fear of legal repercussions under Texas’s abortion laws also appears to influence healthcare providers’ decision-making, leading to hesitancy in providing timely and necessary care.
The ongoing debate around Texas’s restrictive abortion laws, particularly concerning emergency situations like ectopic pregnancies and EMTALA complaints, highlights a critical access issue. This lack of access is further exacerbated by news like the steward ohio hospitals closures pennsylvania facility at risk , showing how dwindling healthcare resources impact vulnerable populations. The potential for further restrictions and closures only intensifies the urgency of ensuring adequate emergency care, especially for those needing time-sensitive reproductive healthcare.
The EMTALA Complaint Process and Potential Outcomes
Filing an EMTALA complaint involves several steps. First, a formal complaint must be filed with the relevant federal agency, typically the U.S. Department of Health and Human Services (HHS). This complaint must include detailed information about the incident, including dates, times, names of healthcare providers, and a description of the alleged violation. The HHS Office of Civil Rights (OCR) then investigates the complaint, gathering evidence and interviewing witnesses.
The investigation can be lengthy, potentially lasting several months or even years. Potential outcomes range from a finding of no violation to a finding of a violation, which may result in financial penalties, corrective action plans, and other remedial measures for the healthcare facility. In some cases, the OCR may refer the matter to the Department of Justice for further legal action.
The process can be complex and challenging for individuals navigating it, often requiring legal assistance.
Significant Legal Precedents and Court Cases
While there aren’t numerous landmark Supreme Court cases directly addressing EMTALA and abortion access in Texas, several lower court cases and legal opinions have addressed related issues. These cases frequently involve the interpretation of “stabilization” under EMTALA in the context of pregnancy complications and the extent to which abortion restrictions can impact a hospital’s obligation to provide emergency care. These cases underscore the ongoing legal battles surrounding the intersection of EMTALA and abortion access, highlighting the complexities of balancing federal law with state regulations.
The lack of clear legal precedent in this specific area contributes to the ongoing uncertainty faced by both patients and healthcare providers in Texas.
Summary of EMTALA Complaints: Types, Outcomes, and Key Findings
| Type of Complaint | Outcome | Key Findings | Relevant Case (Illustrative Example) |
|---|---|---|---|
| Delay in treatment for ectopic pregnancy | Violation found; financial penalty imposed | Hospital delayed treatment due to concerns about state abortion laws, resulting in patient harm. | (Hypothetical case: Doe v. County Hospital – details would be based on a real case with details changed to protect privacy) |
| Refusal to provide necessary medication for miscarriage management | Violation found; corrective action plan mandated | Hospital staff hesitated to administer medication due to ambiguity in state law, delaying necessary care. | (Hypothetical case: Roe v. City Medical Center – details would be based on a real case with details changed to protect privacy) |
| Transfer of patient to a facility lacking appropriate resources | No violation found (due to insufficient evidence) | Investigation found that while there were delays, they did not constitute a violation of EMTALA’s stabilization requirement. | (Hypothetical case: Jane v. Suburban Hospital – details would be based on a real case with details changed to protect privacy) |
Summary

Source: abcnews.com
Navigating the complex web of Texas abortion laws and EMTALA in emergency situations is fraught with challenges for both patients and healthcare providers. The conflicting legal frameworks create significant obstacles to timely and necessary medical care, potentially leading to severe health consequences for women. Understanding the nuances of these laws, the potential conflicts, and the process for filing EMTALA complaints is crucial for ensuring accountability and protecting the rights of individuals seeking emergency medical care.
The ongoing legal battles and the persistent need for clarity underscore the urgent need for reform and a more consistent approach to ensuring access to essential healthcare services.
Clarifying Questions
What constitutes an emergency under EMTALA related to abortion?
EMTALA defines an emergency as a condition that manifests itself by acute symptoms of sufficient severity (including the excruciating pain of an ectopic pregnancy) such that the absence of immediate medical attention could reasonably be expected to result in placing the health of the individual (or, with respect to a pregnant woman, the health of the woman or her unborn child) in serious jeopardy, serious impairment to bodily functions, or serious dysfunction of any bodily organ or part.
Can a hospital be penalized for violating EMTALA in an abortion case?
Yes. Hospitals can face significant financial penalties and potential legal action for violating EMTALA, even if the violation involves a patient seeking abortion care in an emergency situation. The penalties can be substantial, and the legal ramifications can be severe.
What resources are available for patients facing challenges accessing emergency abortion care in Texas?
Several organizations provide legal and logistical support to patients seeking emergency abortion care in Texas. These organizations can offer guidance on navigating the legal complexities, finding appropriate healthcare providers, and accessing financial assistance.
What are the typical outcomes of EMTALA complaints related to abortion in Texas?
Outcomes vary, but complaints may lead to investigations, settlements, changes in hospital policies, or even legal action. The success of a complaint depends on the specific circumstances and the strength of the evidence presented.