UnitedHealth Prior Authorization Gastroenterology Plan
UnitedHealth prior authorization gastroenterology plan – navigating this can feel like deciphering a medical hieroglyphic, right? Getting the care you need shouldn’t be a bureaucratic obstacle course. This post aims to shed some light on the process, demystifying the ins and outs of UnitedHealthcare’s gastroenterology coverage and prior authorization procedures. We’ll cover everything from understanding your plan’s specifics to appealing a denied request, empowering you to advocate for your health.
We’ll explore the different UnitedHealthcare gastroenterology plans, comparing their coverage, costs, and network access. We’ll walk you through the prior authorization process step-by-step, highlighting what documentation you’ll need and what to expect in terms of timelines. We’ll also discuss the crucial differences between using in-network versus out-of-network gastroenterologists and the potential financial implications. Finally, we’ll arm you with the knowledge to navigate appeals if your prior authorization is denied.
UnitedHealthcare Gastroenterology Plans

Source: ecareindia.com
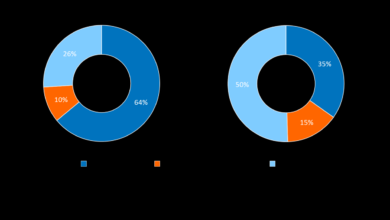
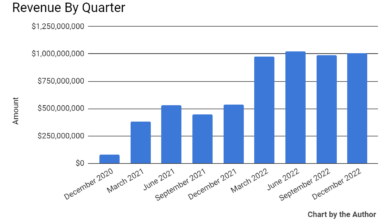
Navigating the world of health insurance can be daunting, especially when dealing with specialized care like gastroenterology. UnitedHealthcare offers a range of plans, each with its own set of benefits and limitations. Understanding these differences is crucial for choosing the plan that best fits your individual needs and budget. This overview will help you compare key features to make an informed decision.
UnitedHealthcare Gastroenterology Plan Options
UnitedHealthcare provides various plans, broadly categorized into HMOs (Health Maintenance Organizations), PPOs (Preferred Provider Organizations), and POS (Point of Service) plans. Each type offers different levels of flexibility and cost-sharing. HMOs generally have lower premiums but restrict you to a specific network of doctors. PPOs offer more flexibility with higher premiums and out-of-pocket costs. POS plans blend features of both HMOs and PPOs.
Specific gastroenterology coverage within these plan types varies further based on the specific plan chosen. For example, some plans may offer better coverage for colonoscopies than others, or have different cost-sharing structures for specialist visits.
Benefits and Limitations of UnitedHealthcare Gastroenterology Plans
The benefits and limitations of each UnitedHealthcare gastroenterology plan are primarily determined by the plan’s type (HMO, PPO, POS), its specific tier (e.g., Bronze, Silver, Gold, Platinum), and any additional riders or supplemental insurance purchased. Generally, higher premium plans offer lower out-of-pocket costs and broader network access. Lower premium plans often involve higher deductibles, co-pays, and coinsurance, potentially resulting in significant out-of-pocket expenses for extensive gastroenterology care.
Limitations can include restrictions on the choice of specialists, pre-authorization requirements for certain procedures, and limitations on the number of visits covered annually.
Comparison of UnitedHealthcare Gastroenterology Plans
Choosing the right plan requires careful consideration of cost, network access, and out-of-pocket expenses. The following table compares four hypothetical UnitedHealthcare gastroenterology plans to illustrate these differences. Remember that actual plan details vary by location and year, so always check the plan details directly with UnitedHealthcare for the most up-to-date information.
Navigating UnitedHealthcare’s prior authorization process for gastroenterology can be a headache, especially with the current complexities. The delays are often exacerbated by the medical coding backlog, which is why I was so interested to read about the ai powered solution to the medical coding worker shortage. Faster coding could significantly streamline the entire prior authorization process for plans like UnitedHealthcare’s, ultimately benefiting both patients and providers.
Hopefully, this tech will improve the efficiency of the entire system, including UnitedHealth’s gastroenterology plan.
| Plan Name | Monthly Premium | Annual Deductible | Copay (Specialist Visit) | Network Size |
|---|---|---|---|---|
| Example Plan A (HMO Bronze) | $300 | $6,000 | $50 | Small – Local Network |
| Example Plan B (HMO Silver) | $450 | $4,000 | $40 | Medium – Regional Network |
| Example Plan C (PPO Gold) | $700 | $2,000 | $30 | Large – National Network |
| Example Plan D (PPO Platinum) | $1000 | $1,000 | $20 | Extensive – National Network |
Prior Authorization Process for Gastroenterology Services: Unitedhealth Prior Authorization Gastroenterology Plan
Navigating the prior authorization process for gastroenterology services with UnitedHealthcare can feel like wading through a swamp, but understanding the steps involved can significantly streamline the process. This guide Artikels the process, required documentation, typical timelines, and strategies to avoid common pitfalls.
The prior authorization process is a crucial step to ensure your gastroenterology procedures are covered by your UnitedHealthcare plan. Failure to obtain prior authorization may result in significant out-of-pocket expenses. The process itself involves submitting a detailed request to UnitedHealthcare, which they then review to determine medical necessity.
Navigating the UnitedHealth prior authorization process for gastroenterology can be a real headache, especially when you’re trying to focus on your health. Proper nutrition is key to recovery, and I’ve been researching how diet impacts gut health; it’s fascinating to learn more about this from articles like this one on are women and men receptive of different types of food and game changing superfoods for women , which highlights the importance of tailored nutrition.
Understanding these dietary nuances helps me advocate for myself during the authorization process with UnitedHealth.
Required Documentation for Prior Authorization Requests
The necessary documentation varies depending on the specific procedure, but generally includes the completed prior authorization form, a detailed referral from your primary care physician, and comprehensive medical records. These records should clearly demonstrate the medical necessity of the procedure. For common procedures like colonoscopies and endoscopies, this typically includes a detailed history of the patient’s symptoms, relevant diagnostic test results (such as stool tests or imaging studies), and the physician’s rationale for recommending the procedure.
Missing or incomplete documentation is a frequent cause of delays.
Step-by-Step Prior Authorization Process
- Physician Submission: Your gastroenterologist initiates the process by submitting a prior authorization request to UnitedHealthcare, using their preferred method (online portal, fax, or mail). This request includes the completed form and all supporting documentation.
- UnitedHealthcare Review: UnitedHealthcare reviews the submitted documentation to assess the medical necessity of the requested procedure. This review may involve consultation with their medical professionals.
- Decision Notification: UnitedHealthcare will notify your gastroenterologist (and potentially you) of their decision. This notification will specify whether the prior authorization has been approved, denied, or requires additional information.
- Appeal Process (if applicable): If the prior authorization is denied, your gastroenterologist can submit an appeal, providing additional information or rationale to support the medical necessity of the procedure.
Typical Timeframe for Prior Authorization Approvals and Denials
The typical timeframe for a prior authorization decision is generally between 2-7 business days. However, delays can occur due to incomplete documentation, complex cases requiring additional review, or high claim volumes. In some instances, the process may take significantly longer, especially if an appeal is necessary. For example, a particularly complex case involving a rare condition might take up to several weeks for a decision.
Challenges and Strategies to Mitigate Delays
Common challenges include incomplete or missing documentation, unclear medical necessity justification, and delays in communication between the physician’s office and UnitedHealthcare. To mitigate these delays, it’s crucial to ensure all required documentation is complete and accurate before submission. Clear and concise communication between the physician and UnitedHealthcare is essential. Proactive follow-up on the status of the request can also help prevent unexpected delays.
For example, confirming the receipt of the request and inquiring about the review status after a reasonable timeframe can keep the process moving forward. Having a dedicated staff member responsible for managing prior authorizations can significantly improve efficiency and reduce delays.
In-Network vs. Out-of-Network Gastroenterologists
Choosing between an in-network and out-of-network gastroenterologist significantly impacts your healthcare costs when you have a UnitedHealthcare plan. Understanding these differences is crucial for budgeting and making informed decisions about your care. This section will explore the financial implications of each choice.
The primary difference lies in the negotiated rates between UnitedHealthcare and the healthcare providers. In-network providers have pre-negotiated rates with your insurance company, meaning your plan covers a larger portion of the services. Out-of-network providers haven’t established these agreements, leading to higher out-of-pocket expenses for you.
Cost Differences for Common Procedures
The financial disparities between in-network and out-of-network care can be substantial. For instance, a colonoscopy performed by an in-network gastroenterologist might cost you a small copay, while the same procedure with an out-of-network provider could result in thousands of dollars in out-of-pocket expenses after your insurance applies its allowed amount. Similarly, an endoscopy, a less invasive procedure, will also show a notable difference in cost-sharing.
The specific amounts will vary depending on your individual plan and the provider’s charges.
Implications of Using Out-of-Network Providers
Utilizing out-of-network gastroenterologists significantly affects your plan benefits and out-of-pocket costs. Your insurance company will likely reimburse a smaller percentage of the total bill, leaving you responsible for a much larger portion. This can lead to unexpectedly high medical bills and could exceed your annual out-of-pocket maximum more quickly. You may also encounter difficulties with claims processing, as the out-of-network provider’s billing practices may not align with your insurance company’s procedures.
Pre-authorization may also be more complex and less likely to be approved.
Financial Comparison Table
The following table illustrates potential cost differences for several common gastroenterology services. These are illustrative examples and actual costs can vary based on geographic location, the specific procedure performed, and the individual provider’s fees. Always check your Explanation of Benefits (EOB) for the precise charges and reimbursements.
| Service | In-Network Estimated Cost (with insurance) | Out-of-Network Estimated Cost (with insurance) | Out-of-Pocket Difference |
|---|---|---|---|
| Colonoscopy | $100 copay | $2,000 – $3,000 | $1,900 – $2,900 |
| Endoscopy | $50 copay | $1,000 – $1,500 | $950 – $1,450 |
| Upper GI Endoscopy | $75 copay | $1,200 – $1,800 | $1,125 – $1,725 |
| Consultation | $25 copay | $300 – $500 | $275 – $475 |
Specific Procedure Coverage and Limitations
Navigating the world of health insurance can be confusing, especially when it comes to understanding exactly what your plan covers. This section aims to clarify the specific coverage and limitations for common gastroenterology procedures under various UnitedHealthcare plans. Remember, this information is for general guidance only, and your specific plan details will determine your actual coverage. Always refer to your individual policy documents for the most accurate and up-to-date information.
It’s crucial to understand that UnitedHealthcare offers a range of plans, each with its own specific benefits and cost-sharing structures. These differences directly impact the coverage for procedures like colonoscopies, endoscopies, and ERCPs. Factors such as your plan type (PPO, HMO, etc.), your deductible, and your copay will all play a role in your out-of-pocket expenses.
Colonoscopy Coverage
Colonoscopies, a vital screening tool for colorectal cancer, are generally well-covered under most UnitedHealthcare plans, especially when performed as a preventative measure. However, coverage details can vary.
- Preventive Colonoscopy: Many plans cover preventative colonoscopies at recommended intervals (typically every 10 years for individuals with average risk) with minimal or no out-of-pocket costs after meeting your deductible and any applicable copay. This is often considered a preventative service and therefore subject to less stringent requirements.
- Diagnostic Colonoscopy: If a colonoscopy is performed for diagnostic purposes (e.g., investigating symptoms like rectal bleeding), the coverage might differ. You may have higher co-pays or coinsurance responsibilities. Pre-authorization may also be required.
- Limitations: Frequency limitations may exist. For example, your plan might only cover a preventative colonoscopy every 10 years, unless medically necessary.
Endoscopy Coverage
Endoscopies, encompassing procedures like upper endoscopy (esophagogastroduodenoscopy or EGD) and small bowel endoscopy, also have varying coverage depending on the reason for the procedure.
- Diagnostic Endoscopy: Coverage for diagnostic endoscopies performed to investigate symptoms (e.g., abdominal pain, unexplained weight loss) is generally good, but cost-sharing might apply depending on the plan. Pre-authorization may be needed.
- Therapeutic Endoscopy: If the endoscopy involves a therapeutic intervention (e.g., removing a polyp), coverage is typically provided, but cost-sharing might be higher than for a purely diagnostic procedure.
- Limitations: Similar to colonoscopies, frequency limitations might apply. Also, specific diagnostic criteria might be required for coverage.
ERCP Coverage
Endoscopic retrograde cholangiopancreatography (ERCP) is a more complex procedure used to diagnose and treat conditions affecting the bile ducts and pancreas. Coverage for ERCP is typically subject to stricter requirements.
- Medical Necessity: Coverage for ERCP is usually contingent upon demonstrating medical necessity. This requires your physician to clearly document the medical reason for the procedure.
- Pre-authorization: Pre-authorization is almost always required for ERCPs due to their complexity and cost. Failure to obtain pre-authorization can lead to significantly higher out-of-pocket costs.
- Limitations: Specific diagnostic criteria and documentation are usually needed to justify the medical necessity of an ERCP. Frequency limitations might also apply.
Appealing Prior Authorization Denials
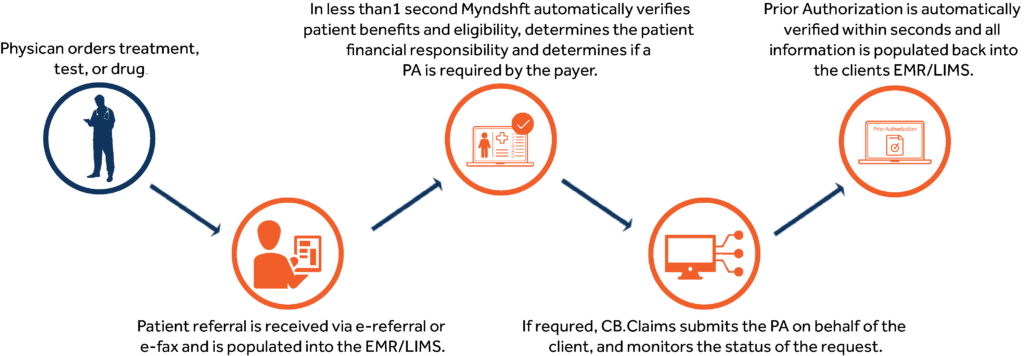
Source: myndshft.com
Navigating UnitedHealth’s prior authorization process for gastroenterology can feel like a maze, especially with the recent changes in healthcare regulations. The Supreme Court’s decision to overturn the Chevron Doctrine, as reported in this article scotus overturns chevron doctrine healthcare , could significantly impact how insurance companies like UnitedHealth operate, potentially affecting the future of prior authorization procedures.
This means we might see even more hurdles in getting timely approvals for necessary gastroenterology care.
Navigating the prior authorization process for gastroenterology services can sometimes feel like a maze. Even with careful preparation, denials can occur. Understanding the appeals process is crucial to ensuring timely access to necessary care. This section Artikels the steps involved in appealing a denied prior authorization request from UnitedHealthcare.
The appeal process for a denied prior authorization generally involves submitting a formal request for reconsideration to UnitedHealthcare. This request needs to clearly state your disagreement with the initial denial, provide compelling evidence supporting the medical necessity of the requested service, and follow UnitedHealthcare’s specific procedures. Failure to follow these procedures may result in your appeal being rejected.
The process is designed to ensure fairness and transparency, offering a mechanism to challenge decisions when appropriate medical justification exists.
Reasons for Appealing a Prior Authorization Denial
Valid reasons for appealing a prior authorization denial often center on demonstrating that the initial decision failed to adequately consider the specific medical circumstances of the patient. This requires a thorough understanding of the denial reason and the supporting medical documentation. For example, a denial might stem from a perceived lack of medical necessity, an incorrect interpretation of the patient’s medical history, or an oversight of relevant clinical guidelines.
Examples of valid reasons include, but are not limited to, the following:
- The denial failed to adequately consider the patient’s unique medical history and current condition.
- The denial did not account for relevant clinical guidelines or peer-reviewed medical literature supporting the requested procedure.
- The denial was based on inaccurate or incomplete information about the patient’s condition or the requested service.
- The denial was inconsistent with previous approvals for similar services or procedures.
- The denial did not appropriately consider the potential risks and benefits of alternative treatment options.
Required Documentation for an Appeal
Supporting your appeal with comprehensive and well-organized documentation is vital. The strength of your appeal directly correlates with the quality and completeness of the evidence provided. UnitedHealthcare will likely require specific documentation to support your claim.
Typically, this documentation includes:
- A completed appeal form provided by UnitedHealthcare.
- A detailed explanation of why you disagree with the initial denial, clearly referencing the specific reasons for the denial.
- Copies of all relevant medical records, including the patient’s medical history, diagnostic test results, and physician’s notes, specifically addressing the medical necessity of the requested service.
- Relevant clinical guidelines or peer-reviewed medical literature supporting the requested procedure.
- Letters of support from the patient’s physician and potentially other specialists.
Appeal Resolution Timeframe
The timeframe for resolving an appeal can vary depending on several factors, including the complexity of the case and the completeness of the submitted documentation. While UnitedHealthcare aims for a timely resolution, it’s important to understand that the process may take several weeks or even months.
For example, a straightforward appeal with clear documentation might be resolved within a few weeks, while a more complex appeal requiring additional review or external consultation could take several months. Proactive communication with UnitedHealthcare throughout the appeals process can help track progress and ensure a timely resolution. It is advisable to follow up on the status of your appeal after a reasonable period.
Member Resources and Support
Navigating the healthcare system can be challenging, especially when dealing with complex procedures like those often requiring prior authorization in gastroenterology. UnitedHealthcare understands this and provides a robust network of resources and support to help its members throughout the process. This section details the various avenues available to you for assistance.Understanding your options for obtaining help with prior authorizations and other plan-related questions is crucial for a smooth experience.
UnitedHealthcare offers multiple channels to ensure members receive timely and accurate information. This includes phone support, online tools, and helpful printed materials.
Contacting UnitedHealthcare
Members can reach UnitedHealthcare through several methods, ensuring accessibility for everyone. The primary method is via phone, using the member services number found on your insurance card. Representatives are available to answer questions regarding prior authorizations, benefits, coverage details, and any other plan-related inquiries. For those who prefer written communication, mailing addresses are also available, allowing for submitting questions or appeals via mail.
Additionally, many members find the online portal a convenient and efficient way to communicate with their provider.
Online Tools and Portals
UnitedHealthcare provides a comprehensive online member portal accessible via their website. This portal allows members to view their benefits summary, check the status of prior authorization requests, download claim forms, and access helpful educational materials related to gastroenterology services. The portal is designed for easy navigation and intuitive use, enabling members to manage their healthcare needs efficiently. For example, the portal displays a clear timeline of a prior authorization request, indicating its current status (e.g., pending, approved, denied) and providing any necessary updates.
This transparency empowers members to proactively address any potential issues.
Available Member Resources and Support Options, Unitedhealth prior authorization gastroenterology plan
The following list summarizes the various resources and support options available to UnitedHealthcare members:
- Phone Support: Access to knowledgeable representatives via a dedicated member services phone number.
- Online Member Portal: A secure website for managing benefits, checking prior authorization statuses, and accessing educational materials.
- Mail Correspondence: The option to communicate with UnitedHealthcare through written mail.
- Printed Materials: Brochures and guides providing information about benefits, coverage, and the prior authorization process.
- Provider Directory: An online directory to locate in-network gastroenterologists.
Closing Summary
Successfully navigating the UnitedHealth prior authorization gastroenterology plan requires understanding your specific plan details and the process involved. Remember, you’re not alone in this! Armed with the right information and a proactive approach, you can significantly improve your chances of a smooth and timely authorization process. Don’t hesitate to contact UnitedHealthcare directly if you need further assistance or clarification – knowing your rights and options is key to getting the care you deserve.
Question & Answer Hub
What happens if my prior authorization is denied?
Don’t panic! You have the right to appeal the decision. The process typically involves submitting additional documentation and explaining why you believe the denial was unwarranted. Check your plan documents for specific appeal procedures.
How long does the prior authorization process usually take?
The timeframe varies, but it often takes several business days to a couple of weeks. Submitting a complete and accurate request can help expedite the process.
Can I get pre-authorization for multiple procedures at once?
It depends on your plan and the procedures. It’s best to contact UnitedHealthcare to clarify if this is possible.
Where can I find my plan’s specific coverage details?
Your plan’s details, including coverage for specific procedures, should be Artikeld in your member handbook or available online through your UnitedHealthcare account.