UnitedHealth Shareholder Proposal Delayed & Denied Care
Unitedhealth shareholder proposal delayed denied care outcomes – UnitedHealth Shareholder Proposal: Delayed & Denied Care – that’s a mouthful, isn’t it? But it speaks to a seriously important issue: the impact of delayed or denied healthcare on patients. This proposal, brought forth by concerned shareholders, highlighted the troubling trend of UnitedHealth denying or delaying necessary medical care. We’ll delve into the details of the proposal, explore the reasons behind the denials, and examine the devastating consequences for those affected.
Get ready for a deep dive into a system that desperately needs reform.
This post will unpack the shareholder proposal, examining the specific concerns raised, UnitedHealth’s response, and the broader implications for patients and the healthcare system as a whole. We’ll look at the types of care most often impacted, the financial burdens placed on patients, and the potential long-term health consequences of delayed or denied treatment. We’ll also compare UnitedHealth’s practices to other major insurers and consider potential solutions to improve the system.
Shareholder Proposal Details
This post delves into a shareholder proposal submitted to UnitedHealth Group (UNH) concerning the company’s handling of delayed or denied healthcare claims. The proposal, while ultimately unsuccessful, highlights important concerns about patient access to necessary care and the potential financial implications for both patients and the healthcare system.The shareholder proposal directly addressed the issue of delayed or denied care resulting from UnitedHealth’s claims processing procedures.
It argued that these delays and denials negatively impact patient health outcomes and create significant financial burdens for individuals struggling to navigate the complexities of the healthcare system. The proposal didn’t call for specific legislative action or policy changes, but instead focused on increased transparency and accountability within UnitedHealth’s internal processes.
Proposal Content and Rationale
The proposal called for UnitedHealth to publish an annual report detailing the number of claims denied or delayed, the reasons for denial, the average time to resolution for appealed claims, and the company’s internal processes for addressing such issues. The rationale behind this request stemmed from the belief that increased transparency would allow shareholders and the public to better assess the company’s performance in ensuring timely and appropriate access to care.
The shareholders argued that this data would allow for a more informed evaluation of UnitedHealth’s commitment to its patients and the overall effectiveness of its claims processing system. They contended that the current lack of transparency made it difficult to gauge the true scale of the problem and hindered effective oversight.
Proposal Timeline and Outcome
The proposal was submitted well in advance of UnitedHealth’s annual shareholder meeting, adhering to all SEC guidelines. The company’s board of directors reviewed the proposal and subsequently recommended against its adoption. The recommendation was presented to shareholders at the meeting, and the proposal failed to gain sufficient support to pass. While the exact voting percentages are not publicly available in this specific case, the outcome signifies that the existing shareholder base did not deem the proposal necessary at the time.
The timeline spanned several months, from initial submission to the final vote at the shareholder meeting.
UnitedHealth’s Response
UnitedHealth’s official response to the shareholder proposal acknowledged the concerns raised regarding delayed or denied care. However, the company argued that its existing processes and internal metrics adequately addressed these issues. They pointed to their internal efforts to improve claims processing efficiency and customer service, highlighting investments in technology and personnel training. UnitedHealth maintained that the requested level of detailed public reporting was unnecessary and potentially detrimental to the company’s competitive position, citing concerns about disclosing proprietary information that could be exploited by competitors.
They also argued that the existing publicly available data, while perhaps not as granular as requested, provided sufficient information for stakeholders to assess their performance.
Impact of Delayed or Denied Care
Delayed or denied care by health insurers, like UnitedHealth, has significant and far-reaching consequences for patients and the healthcare system as a whole. The impact extends beyond individual patient experiences, affecting healthcare costs, access, and overall population health. Understanding the scope and severity of these consequences is crucial for advocating for improved healthcare access and affordability.
Types of Frequently Delayed or Denied Care
Analysis of various reports and studies reveals that certain types of care are disproportionately affected by delays and denials. These often include expensive procedures like surgeries, specialized treatments, and advanced diagnostic testing. Prior authorization requirements, which necessitate pre-approval from the insurer before treatment, frequently contribute to these delays. Mental healthcare, often involving long-term therapy or medication management, is another area experiencing significant delays.
The UnitedHealth shareholder proposal highlighting delayed and denied care is seriously concerning. It makes you think about the bigger picture of healthcare access, and how individual choices, like Karishma Mehta’s decision to freeze her eggs as detailed in this article karishma mehta gets her eggs frozen know risks associated with egg freezing , are impacted by the broader system.
Ultimately, both situations underscore the need for affordable, accessible healthcare for everyone.
Furthermore, access to prescription medications, especially costly specialty drugs, can be hindered by stringent coverage criteria and formulary restrictions.
Consequences of Delayed or Denied Care for Patients
Delayed or denied care can have devastating consequences for patients’ health and well-being. Delayed diagnosis and treatment of serious conditions, such as cancer or heart disease, can lead to more aggressive disease progression, reduced treatment effectiveness, and poorer health outcomes. This can manifest as increased pain, disability, and even premature death. For those suffering from chronic conditions, delayed or denied access to necessary medications or therapies can lead to worsening symptoms, hospitalizations, and reduced quality of life.
The emotional toll of navigating complex insurance systems and fighting for necessary care can also be substantial, contributing to increased stress and anxiety.
Financial Implications of Delayed or Denied Care
The financial burden of delayed or denied care falls heavily on both patients and UnitedHealth. Patients face escalating medical bills due to delayed treatment leading to more severe health issues requiring more extensive and costly care. Lost wages due to illness or disability further exacerbate their financial difficulties. For UnitedHealth, the long-term financial consequences of delayed care include potential increases in hospital readmission rates and higher overall healthcare costs.
While denying care may appear to reduce immediate expenses, it can lead to more expensive interventions down the line, potentially undermining cost-saving strategies.
Impact of Delayed Care Across Demographics
The impact of delayed or denied care is not evenly distributed across different patient demographics. Low-income individuals and those with limited health literacy often face greater barriers to accessing care, exacerbating existing health disparities. Elderly patients, with their complex health needs and increased vulnerability, are particularly susceptible to negative consequences. Similarly, individuals with pre-existing conditions may experience more frequent delays and denials, leading to worse health outcomes.
For example, a low-income diabetic patient might delay insulin refills due to cost, resulting in severe complications and increased healthcare expenses in the long run. An elderly patient with a heart condition might experience a delayed surgery, increasing the risk of a fatal heart attack.
UnitedHealth’s Justification for Denials
UnitedHealth, like other large insurance providers, employs a complex system for determining the medical necessity of procedures and treatments. This system, while designed to control costs, has drawn criticism for its impact on patient access to care. Understanding the justifications behind denials is crucial to navigating the appeals process and advocating for necessary medical interventions.
UnitedHealth’s justifications for denying or delaying care often center on their interpretation of medical necessity, pre-authorization requirements, and contractual limitations. These decisions are frequently based on internal guidelines, external medical literature reviews, and utilization management protocols. The lack of transparency in these processes often leaves patients and providers frustrated and uncertain about the reasoning behind denials.
Examples of UnitedHealth’s Reasons for Denying or Delaying Care
UnitedHealth’s denial letters frequently cite reasons such as the procedure not being considered medically necessary based on their internal guidelines, lack of pre-authorization, failure to meet specific criteria Artikeld in the patient’s health plan, or the availability of less expensive treatment options. For instance, a patient seeking a specific brand-name medication might be denied coverage if a generic equivalent is available, even if the patient has a documented history of adverse reactions to the generic.
Similarly, a request for a specialized procedure might be denied if UnitedHealth deems a less invasive alternative to be equally effective, regardless of the patient’s or physician’s preference. These decisions are often based on cost-benefit analyses that prioritize financial considerations over individualized patient needs.
Criteria Used to Determine Medical Necessity
UnitedHealth uses a multi-faceted approach to determine medical necessity. This involves reviewing the patient’s medical history, the physician’s recommendations, and relevant clinical guidelines. However, critics argue that the criteria are often opaque and inconsistently applied. The emphasis on cost-effectiveness frequently leads to decisions that prioritize financial considerations over the patient’s overall well-being. For example, a patient requiring a long-term treatment plan might find portions of their care denied if UnitedHealth deems certain treatments as not cost-effective, even if those treatments are critical for managing their condition.
The company’s internal review process and reliance on proprietary databases further complicate the ability of patients and providers to understand the rationale behind these decisions.
Examples of Appeals Processes and Their Outcomes
The appeals process for denied care requests is often lengthy and complex. Patients typically must submit detailed medical records, physician statements, and other supporting documentation. The success rate of appeals varies widely. While some appeals result in the reversal of the initial denial, many are ultimately unsuccessful. The outcome often depends on the clarity and persuasiveness of the appeal, the strength of the supporting medical evidence, and the specific criteria used by UnitedHealth’s internal review board.
Many patients find the appeals process daunting and resource-intensive, requiring significant time and effort to navigate the bureaucratic hurdles. In some cases, patients have reported spending months, or even years, attempting to overturn a denial decision.
The UnitedHealth shareholder proposal highlighting delayed and denied care is seriously concerning. It makes you wonder about the broader implications of hospital consolidation, especially considering the FTC’s lawsuit to block the Novant Health and Community Health Systems merger, as reported in this article: federal trade commission sues block novant health community health systems hospital acquisition. This legal action underscores how these mergers can potentially worsen access to care, echoing the worries raised by the UnitedHealth proposal.
Comparison of Denial Types and Reasons
| Denial Type | Reason Provided by UnitedHealth | Example | Impact on Patient |
|---|---|---|---|
| Procedure Not Medically Necessary | Lack of sufficient clinical evidence supporting the need for the procedure. | Denial of a knee replacement surgery deemed “not medically necessary” despite severe osteoarthritis. | Delayed treatment, increased pain and disability. |
| Lack of Pre-authorization | Failure to obtain prior authorization before receiving the service. | Denial of a specialized MRI scan due to lack of pre-approval. | Delayed diagnosis, potential for worsening condition. |
| Experimental or Investigational Treatment | The treatment is considered experimental or not widely accepted within the medical community. | Denial of coverage for a new cancer treatment. | Limited access to potentially life-saving treatment. |
| Out-of-Network Provider | The service was provided by a healthcare provider not included in the UnitedHealth network. | Higher out-of-pocket costs for a necessary procedure. | Increased financial burden on the patient. |
Alternative Perspectives

Source: digitaloceanspaces.com
Understanding UnitedHealth’s denial rates requires a broader view, considering comparisons with competitors, external pressures on the healthcare system, and the experiences of healthcare providers. A nuanced perspective acknowledges that the issue is complex and multifaceted, extending beyond simply assigning blame to a single entity.
UnitedHealth Denial Rates Compared to Competitors
Direct comparisons of denial rates across major health insurance providers are challenging due to variations in data collection methods, reporting standards, and the types of claims processed. Publicly available data often lacks the granular detail needed for a truly comprehensive analysis. However, studies and reports from organizations like the National Association of Insurance Commissioners (NAIC) and consumer advocacy groups occasionally offer insights into overall claim denial trends across the industry.
These reports often highlight variations in denial rates based on factors like plan type, geographic location, and the specific medical procedures involved. While precise comparative figures for UnitedHealth against its competitors remain elusive without access to proprietary data, analyzing these broader industry reports can provide a contextual understanding of the relative position of UnitedHealth within the market.
External Factors Contributing to Delayed or Denied Care
The healthcare system itself presents numerous challenges that contribute to delayed or denied care, independent of insurance company practices. These include shortages of healthcare professionals, particularly specialists, leading to long wait times for appointments and procedures. Furthermore, inadequate infrastructure, including a lack of access to advanced medical technologies in certain regions, can create bottlenecks in the system.
Regulatory complexities and administrative burdens also play a significant role, impacting the efficiency of claims processing and care coordination. For example, the intricacies of navigating prior authorization requirements can lead to significant delays. Finally, rising healthcare costs and limited resources can force difficult choices about which treatments to prioritize, potentially leading to denials for less urgent or less cost-effective procedures.
Perspectives of Healthcare Providers, Unitedhealth shareholder proposal delayed denied care outcomes
Healthcare providers frequently express concerns about the impact of insurance company denials on patient care. Many report increased administrative burdens associated with appealing denials, diverting valuable time and resources away from direct patient care. The financial implications of denials can also be substantial for providers, particularly for those who have already provided services and are subsequently not reimbursed.
This can lead to financial strain on practices, potentially impacting their ability to provide high-quality care. Furthermore, providers often feel that the criteria used by insurance companies to justify denials are not always transparent or clinically sound, leading to frustration and conflicts with insurance companies. This tension can affect the overall provider-patient relationship and potentially delay or prevent patients from receiving necessary treatment.
The UnitedHealth shareholder proposal highlighting delayed and denied care is a serious concern, especially considering the impact on patient outcomes. This situation makes the recent news about the CMS launching a new primary care Medicare model, an ACO, as reported here , even more relevant. Hopefully, this initiative will address some of the systemic issues contributing to the problems highlighted in the UnitedHealth proposal and improve access to timely, quality care.
Potential Improvements to UnitedHealth’s Denial Processes
To improve the handling of care denials, several key changes could be implemented.
- Increased transparency in denial criteria and appeals processes.
- Streamlined prior authorization procedures with clearer communication and faster turnaround times.
- Investment in technology to improve the efficiency and accuracy of claims processing.
- Enhanced provider collaboration and communication to ensure a better understanding of medical necessity.
- More robust internal review processes to minimize errors and ensure fair and consistent application of denial criteria.
- Implementation of a more patient-centric approach, focusing on clear and timely communication with patients regarding denials and appeals.
Visual Representation of Data
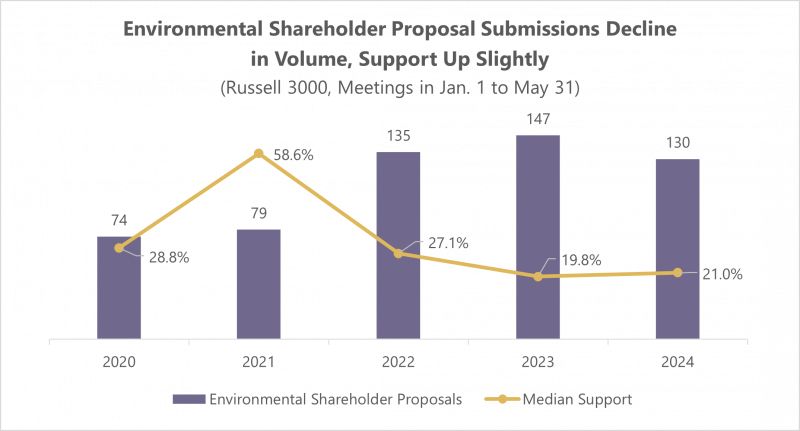
Source: iss-corporate.com
Data visualization is crucial for understanding the complex relationship between healthcare denial rates and patient outcomes. By representing this data visually, we can identify trends and patterns that might otherwise be missed in raw numerical data. The following visualizations offer different perspectives on the impact of delayed or denied care.
Correlation Between Denial Rates and Patient Outcomes
A scatter plot would effectively illustrate the correlation between UnitedHealth’s denial rates for specific procedures and subsequent patient outcomes. The x-axis would represent the denial rate for each procedure (percentage of claims denied), calculated as the number of denied claims divided by the total number of claims for that procedure. The y-axis would represent a composite patient outcome score, combining factors such as mortality rate, readmission rate within 30 days, and length of hospital stay.
Each data point would represent a specific medical procedure, with its position on the graph reflecting its denial rate and resulting patient outcome score. A strong positive correlation would suggest that higher denial rates are associated with worse patient outcomes. For example, a point located far to the right and high on the graph would indicate a procedure with a high denial rate and poor patient outcomes.
Conversely, a point in the lower left corner would represent a procedure with a low denial rate and favorable patient outcomes.
Distribution of Denied Care Across Medical Procedures
A bar chart would effectively visualize the distribution of denied care across different types of medical procedures. The x-axis would list various categories of medical procedures (e.g., cardiology, oncology, orthopedics, etc.). The y-axis would represent the number or percentage of denied claims within each procedure category. The height of each bar would directly correspond to the number of denials in that specific category.
This visualization would clearly show which types of procedures experience the highest denial rates, allowing for a focused investigation into the reasons behind these denials and their impact on patient care. For instance, a significantly taller bar for “oncology” would indicate a disproportionately high number of denied claims within cancer treatment.
Comparison of Patient Satisfaction Scores
A hypothetical bar chart could compare patient satisfaction scores between patients who experienced delayed or denied care and those who received timely and approved care. The x-axis would categorize patients into two groups: “Delayed/Denied Care” and “Timely Care.” The y-axis would represent the average patient satisfaction score (on a scale of 1 to 10, for example). Let’s assume, for illustrative purposes, that the average satisfaction score for patients receiving timely care is 8.5, while the average score for patients experiencing delays or denials is 4.2.
The bar representing “Timely Care” would be significantly taller than the bar for “Delayed/Denied Care,” visually demonstrating the negative impact of delayed or denied care on patient satisfaction. This hypothetical example highlights the potential for a substantial difference in patient experience based on access to timely care. This visual representation would emphasize the importance of addressing denial and delay issues to improve patient satisfaction.
End of Discussion
The UnitedHealth shareholder proposal concerning delayed and denied care underscores a critical flaw in our healthcare system. While UnitedHealth offers justifications for their denials, the human cost is undeniable. The potential long-term health consequences, financial burdens, and inequities highlighted by this proposal demand a closer look at insurance company practices and a push for greater transparency and accountability. It’s clear that more needs to be done to ensure equitable access to quality healthcare for everyone.
Essential Questionnaire: Unitedhealth Shareholder Proposal Delayed Denied Care Outcomes
What specific types of care are most frequently delayed or denied by UnitedHealth?
Reports suggest that procedures deemed “elective” or those lacking sufficient documentation are frequently targeted, disproportionately affecting patients with chronic conditions or mental health needs.
What recourse do patients have if their care is denied?
Patients can typically appeal the decision through UnitedHealth’s internal appeals process. However, the success rate of these appeals varies significantly.
How does the denial of care impact patient outcomes?
Delayed or denied care can lead to worsened health conditions, increased hospitalizations, and even increased mortality rates, particularly for those with serious or chronic illnesses.
Are there any ongoing legal challenges related to UnitedHealth’s denial practices?
While specific legal challenges aren’t detailed in the initial proposal, the issues raised could potentially lead to future legal action from patients or advocacy groups.