Veterans Affairs EHR Contract Extended Oracle
Veterans affairs ehr contract extended oracle – Veterans Affairs EHR Contract Extended: Oracle – the news is out, and it’s a big one for veterans’ healthcare! This massive contract extension with Oracle means continued use of their Electronic Health Record (EHR) system, impacting millions. But what does this really mean for the quality of care our veterans receive? Let’s dive into the details, exploring both the potential benefits and the lingering questions this extension raises.
This post will unpack the intricacies of the extended contract, examining its financial implications, the technological aspects of Oracle’s EHR, and crucially, the impact on veterans’ access to timely and effective healthcare. We’ll also discuss government oversight, data security concerns, and what the future might hold for the VA’s EHR system. Get ready for a deep dive into a topic that directly affects the well-being of our nation’s heroes.
Contract Details and Implications
The extension of the Veterans Affairs (VA) electronic health record (EHR) contract with Oracle represents a significant commitment to modernizing the healthcare system for veterans. This extension, while addressing immediate needs, also raises important questions about long-term costs and the overall effectiveness of the Cerner Millennium system (now owned by Oracle) in meeting the unique demands of VA healthcare.
This analysis will delve into the specifics of the extended contract, examining its terms, projected costs, and potential impacts.
Extended Contract Overview
The extended VA-Oracle contract builds upon the original agreement to implement the Cerner Millennium EHR system across all VA medical facilities. While precise details regarding the extension’s terms are not publicly available in their entirety due to confidentiality clauses, reports suggest a focus on resolving existing implementation challenges, improving system functionality, and ensuring interoperability with other healthcare systems. This extension prioritizes completing the nationwide rollout and addressing ongoing technical and logistical hurdles encountered during the initial phases of implementation.
The extension also likely includes provisions for ongoing maintenance, updates, and technical support.
Key Terms and Conditions
While the full contract remains confidential, key aspects likely included in the extended agreement revolve around deliverables and timelines. The extension almost certainly includes revised deadlines for full system implementation at all VA facilities, potentially incorporating a phased approach to minimize disruption. Furthermore, performance metrics and penalties for non-compliance are likely included, holding Oracle accountable for delivering a functional and reliable system.
Finally, the contract likely specifies mechanisms for resolving disputes and addressing future system upgrades and maintenance. These provisions are crucial to ensure the VA receives the promised system capabilities and ongoing support.
Projected Costs and Budgetary Implications
The financial implications of the extended contract are substantial. While exact figures remain undisclosed, estimates suggest the extension will add significantly to the overall cost of the EHR modernization project. This increased cost is attributable to several factors, including addressing previously encountered implementation issues, incorporating necessary system improvements, and covering extended support and maintenance periods. For example, the initial cost overruns associated with the project’s initial rollout provided a clear indication of the potential for further budgetary pressures.
These unforeseen expenses often stem from complexities in integrating legacy systems, adapting the EHR to the unique needs of VA facilities, and providing adequate training for VA staff. Transparency regarding the budget allocation for the extension is crucial for public accountability and ensuring responsible use of taxpayer funds.
Comparison of Original and Extended Contract Terms
| Aspect | Original Contract | Extended Contract | Difference/Implication |
|---|---|---|---|
| Implementation Timeline | [Insert original timeline if available, otherwise use placeholder like “Initial Timeline X”] | [Insert revised timeline if available, otherwise use placeholder like “Revised Timeline Y”] | [Explain the difference and its implications, e.g., “Extension of X months/years, indicating delays and potential cost increases.”] |
| Total Cost | [Insert original estimated cost if available, otherwise use placeholder like “Estimated Cost A”] | [Insert revised estimated cost if available, otherwise use placeholder like “Revised Estimated Cost B”] | [Explain the difference and its implications, e.g., “Increase of B-A dollars, highlighting budgetary impact.”] |
| Key Performance Indicators (KPIs) | [List KPIs from original contract if available, otherwise use placeholders.] | [List revised KPIs if available, otherwise use placeholders.] | [Compare and contrast KPIs, highlighting changes and their rationale.] |
| Dispute Resolution Mechanisms | [Describe original mechanisms if available, otherwise use placeholders.] | [Describe revised mechanisms if available, otherwise use placeholders.] | [Highlight any changes and their potential impact on resolving future issues.] |
Impact on Veterans Healthcare
The extension of the Oracle contract for the Veterans Affairs EHR system carries significant implications for the healthcare received by millions of veterans. This decision, while potentially controversial, presents both opportunities for improvement and challenges that need careful consideration. The success of this extension hinges on effectively addressing these dual aspects to ensure veterans continue to receive the high-quality care they deserve.The extended contract offers the potential for improved access to veteran healthcare.
Continued investment in the system, assuming proper implementation, can lead to a more streamlined and integrated healthcare experience. This includes better interoperability between different VA facilities and potentially with private healthcare providers, facilitating smoother transitions of care and reducing duplicated efforts. However, the continued reliance on a single vendor also presents inherent risks.
Potential Benefits of the Extended Contract
A key benefit lies in the potential for enhanced system stability and reduced disruption. Frequent system changes and upgrades can be highly disruptive to healthcare operations, impacting both providers and patients. An extended contract provides a longer-term horizon for planned improvements, minimizing these disruptions and allowing for more predictable system maintenance. This stability is crucial for the seamless delivery of care and the effective management of patient data.
Furthermore, a longer-term contract allows for more strategic planning and investment in training and support for VA staff, leading to increased proficiency and improved efficiency in utilizing the system.
Challenges and Risks Associated with Continued Reliance on Oracle
Continued reliance on a single vendor, in this case Oracle, presents several potential risks. The lack of competition can potentially lead to higher costs and less innovation compared to a more competitive market. There’s also the risk of vendor lock-in, making it difficult and costly to switch to a different system in the future if Oracle fails to meet the VA’s needs or if a superior alternative emerges.
Furthermore, any major system failure or security breach could have catastrophic consequences for veteran healthcare access and data security. The VA needs robust contingency plans and rigorous security protocols to mitigate these risks.
Expected System Improvements and Upgrades
The contract extension should include provisions for significant system improvements and upgrades. These could include enhanced functionalities for telehealth, improved patient portals with more self-service options, and better integration with other healthcare systems. Specifically, the VA should prioritize upgrades to address previously reported issues such as slow response times, difficulties with data entry, and inadequate reporting capabilities. The success of these improvements will depend heavily on effective project management, rigorous testing, and adequate training for VA staff.
Oracle will need to demonstrate a commitment to addressing past shortcomings and delivering a significantly improved system.
Potential Improvements to Patient Care
The anticipated improvements resulting from the contract extension could significantly benefit veterans’ healthcare.
- Improved access to telehealth services, allowing veterans in remote areas or with mobility issues to receive timely care.
- Enhanced patient portals providing veterans with greater control over their healthcare information and appointment scheduling.
- Reduced wait times for appointments and services due to streamlined workflows and improved system efficiency.
- More accurate and timely access to medical records, facilitating better coordination of care between different providers.
- Improved data analysis capabilities to support better decision-making in healthcare resource allocation and quality improvement initiatives.
Technological Aspects of the EHR System: Veterans Affairs Ehr Contract Extended Oracle
The Veterans Affairs’ (VA) adoption of Oracle’s Cerner Millennium EHR system represents a significant technological undertaking, impacting the delivery of healthcare to millions of veterans. Understanding the system’s core functionalities, its comparison to other leading EHRs, and its interoperability is crucial for assessing its overall effectiveness and potential for future improvements.
Core Functionalities of Oracle’s Cerner Millennium EHR at the VA
Oracle’s Cerner Millennium provides a comprehensive suite of tools for managing patient health information. Key functionalities include electronic health records (EHRs) with integrated clinical documentation, order entry (including medication, lab, and radiology orders), results management, scheduling, billing, and patient portal access. The system supports various clinical specialties, facilitating a holistic view of a veteran’s health across different care settings.
Specific features include advanced analytics capabilities for population health management and tools to support care coordination between VA facilities and community providers. Furthermore, the system aims to provide a seamless patient experience through its patient portal, allowing veterans to access their medical records, schedule appointments, and communicate with their providers.
Comparison with Other Leading EHR Systems
Several leading EHR systems exist, each with its strengths and weaknesses. Comparing Cerner Millennium to systems like Epic and Allscripts reveals both similarities and differences. All three systems offer core EHR functionalities, but their user interfaces, workflow designs, and specific features vary. Epic, for instance, is known for its robust clinical decision support tools and extensive integration capabilities.
Allscripts offers a more modular approach, allowing healthcare organizations to customize their implementations. Cerner Millennium, as implemented by the VA, aims for a comprehensive, integrated system across all VA facilities, though this integration presents its own challenges. A key difference lies in the scale of implementation; the VA’s deployment is one of the largest and most complex EHR implementations globally.
Interoperability with Other Healthcare Information Systems, Veterans affairs ehr contract extended oracle
Interoperability—the ability of different systems to exchange and use data—is a critical aspect of modern healthcare. The VA’s implementation of Cerner Millennium aims to improve interoperability within the VA system and with external healthcare providers. This involves using standardized data exchange formats like HL7 and FHIR to facilitate seamless communication with other EHR systems and health information exchanges (HIEs).
However, achieving complete interoperability remains a significant challenge. The complexity of the VA’s healthcare system and the diversity of external systems require ongoing efforts to ensure effective data sharing and reduce the risk of data silos. Successful interoperability depends on robust APIs, standardized data models, and effective data governance policies.
Strengths and Weaknesses of Oracle’s Cerner Millennium EHR at the VA
| Strength | Weakness | Strength | Weakness |
|---|---|---|---|
| Comprehensive functionality covering various clinical specialties | Complexity of the system leading to steep learning curves for users | Potential for improved care coordination through data integration | Challenges in achieving seamless interoperability with external systems |
| Standardized system across all VA facilities, enabling consistent care | Initial implementation challenges and ongoing technical issues | Advanced analytics capabilities for population health management | Potential for data security vulnerabilities given the large scale of data |
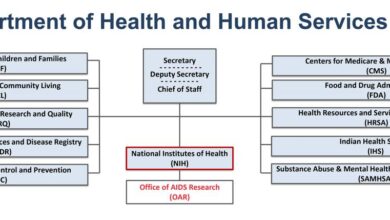
Government Oversight and Accountability

Source: slideplayer.com
The Veterans Affairs EHR contract extension with Oracle is huge news, impacting healthcare delivery for millions. This reminds me of another significant medical advancement: the FDA’s recent approval of clinical trials for pig kidney transplants in humans, as reported here: fda approves clinical trials for pig kidney transplants in humans. Such breakthroughs highlight the need for robust, reliable systems like the updated VA EHR to manage this influx of complex medical data efficiently.
The improved system will be vital for coordinating care and research across the board.
The extension of the Oracle Cerner contract for the Veterans Affairs EHR system necessitates robust government oversight to ensure taxpayer dollars are well-spent and veterans receive the high-quality healthcare they deserve. Multiple agencies and mechanisms are in place to monitor this massive undertaking, balancing the need for efficient implementation with rigorous accountability.Government oversight bodies play a crucial role in scrutinizing the contract’s implementation, preventing cost overruns, and ensuring the system meets its intended goals.
This oversight isn’t simply about catching mistakes; it’s about proactively shaping the project’s trajectory to maximize its effectiveness and minimize potential risks. Transparency is key, allowing for public understanding and engagement in a process that directly impacts millions of veterans.
Agencies Involved in Oversight
The Department of Veterans Affairs (VA) itself has internal oversight mechanisms, but external bodies also play significant roles. The Government Accountability Office (GAO), for example, conducts audits and investigations to assess program performance and identify areas for improvement. Congress, through its committees, holds hearings and conducts reviews, demanding accountability from the VA and its contractors. Furthermore, the Office of Inspector General (OIG) within the VA investigates allegations of fraud, waste, and abuse, ensuring ethical conduct throughout the project’s lifecycle.
The Veterans Affairs EHR contract extension with Oracle is huge news, impacting millions. It makes you wonder about the future of healthcare IT, especially considering the recent shakeups in the private sector. For example, check out this article on despite Walmart Health’s closure, the company healthcare destination, Scott Bowman , which highlights the challenges even large corporations face.
Ultimately, the VA’s decision underscores the importance of robust, reliable systems for veteran care.
These agencies utilize various methods, including financial audits, performance reviews, and system testing, to evaluate the contract’s progress and adherence to stipulations. For instance, the GAO might review cost reports to identify any significant deviations from the budget, while the OIG might investigate allegations of improper procurement practices.
Mechanisms for Ensuring Accountability and Transparency
Accountability and transparency are achieved through several mechanisms. Regular progress reports submitted by the VA to Congress are publicly available, providing insight into the project’s timeline and budget. Independent evaluations, often conducted by external experts, provide unbiased assessments of the system’s functionality and effectiveness. Publicly accessible databases may track key performance indicators (KPIs), such as system uptime and user satisfaction.
Furthermore, the VA may be required to establish a formal process for addressing complaints and concerns raised by veterans and healthcare providers. For example, a dedicated feedback portal could allow users to report bugs or suggest improvements. This feedback would then be incorporated into future system updates, demonstrating a commitment to continuous improvement and responsiveness to user needs.
The use of open data initiatives could further enhance transparency by making relevant data readily available for public analysis and scrutiny.
Avenues for Public Feedback and Scrutiny
The public has various avenues to provide feedback and scrutinize the contract. Individuals can contact their elected officials to express concerns or request information. They can also submit comments to the VA directly through established channels. Moreover, advocacy groups representing veterans’ interests often monitor the project closely and provide public commentary on its progress and challenges. The media plays a vital role in reporting on the contract’s implementation, highlighting both successes and shortcomings.
Finally, academic researchers and independent analysts may conduct studies and publish findings, contributing to a broader understanding of the project’s impact. For instance, a research paper might analyze the system’s effect on wait times for veteran appointments.
Potential Oversight Measures
To ensure effective implementation and accountability, several oversight measures should be implemented:
- Regular and independent audits of financial expenditures and performance metrics.
- Establishment of clear and measurable performance goals, with regular progress reporting to Congress and the public.
- Implementation of a robust system for tracking and addressing user feedback and complaints.
- Independent evaluation of the system’s functionality, security, and interoperability.
- Continuous monitoring of the system’s performance to identify and address potential issues promptly.
- Transparent communication with stakeholders, including veterans, healthcare providers, and the public.
- Enforcement of strict penalties for non-compliance with contract terms and conditions.
- Regular review of the contract’s terms and conditions to ensure they remain relevant and effective.
Future of Veterans Affairs EHR System
The recent extension of the Oracle Cerner contract provides a crucial window to assess and plan for the long-term future of the VA’s EHR system. While the current system addresses immediate needs, a proactive approach is vital to ensure the VA remains at the forefront of healthcare technology and continues to provide the best possible care for our veterans.
This necessitates a strategic vision that encompasses upgrades, technological integration, and robust oversight.The VA’s EHR system faces several challenges and opportunities in the coming years. Successfully navigating this landscape requires a multi-faceted approach focusing on modernization, interoperability, and the seamless integration of emerging technologies. This will not only improve the efficiency and effectiveness of veteran care but also enhance the overall patient experience.
Long-Term Strategies Beyond the Current Contract
The extension provides valuable time for the VA to refine its long-term strategy. This should involve a comprehensive review of the system’s strengths and weaknesses, incorporating feedback from clinicians, veterans, and other stakeholders. Key aspects of this long-term strategy should include a detailed plan for data migration and system optimization, ensuring a smooth transition to any future upgrades or replacements.
Furthermore, a robust training and support program for staff will be crucial to maximize the system’s potential and minimize disruption during transitions. The strategy must also incorporate clear metrics for measuring the system’s success in improving patient care and operational efficiency. For example, tracking reductions in wait times, improved medication adherence, and enhanced care coordination can provide tangible evidence of the system’s positive impact.
Potential Future Upgrades or Replacements
The current system, while a significant improvement over previous iterations, may eventually require a full or partial replacement. This could involve migrating to a newer version of the Cerner platform, incorporating enhanced features and functionalities, or even exploring alternative EHR systems that better meet the VA’s evolving needs. A phased approach to upgrades, focusing on incremental improvements and thorough testing, would mitigate risks and ensure minimal disruption to patient care.
So, the Veterans Affairs EHR contract extension with Oracle is huge news, impacting millions. It got me thinking about long-term planning, and I was reminded of Karishma Mehta’s recent decision to freeze her eggs – you can read about her experience and the associated risks here: karishma mehta gets her eggs frozen know risks associated with egg freezing.
It’s a stark reminder that life choices, like major government contracts, have long-term implications. The VA EHR system, similarly, will shape healthcare for veterans for years to come.
For instance, the VA could prioritize upgrades to specific modules, such as scheduling or medication management, before tackling more comprehensive system-wide changes. This phased approach, mirrored in many large-scale IT projects, allows for iterative feedback and adjustment, minimizing the potential for major setbacks.
Integration of New Technologies
The future VA EHR system should be designed to seamlessly integrate cutting-edge technologies. Artificial intelligence (AI) holds significant promise for improving diagnostic accuracy, predicting patient risks, and personalizing treatment plans. AI-powered tools could analyze vast amounts of patient data to identify patterns and trends, enabling proactive interventions and improved care coordination. Similarly, telehealth capabilities are essential for extending the reach of VA healthcare services to veterans in remote areas or with mobility limitations.
The integration of virtual consultations, remote monitoring, and other telehealth tools would enhance access to care and improve patient outcomes. For example, remote monitoring of vital signs could alert clinicians to potential problems before they escalate, preventing hospitalizations and improving overall health management. The successful implementation of AI and telehealth requires careful consideration of data privacy, security, and ethical implications.
Roadmap for Future System Development and Upgrades
A potential roadmap could involve a three-phase approach:Phase 1 (Years 1-3): Focus on system optimization and incremental upgrades to the existing Cerner platform. This includes addressing identified shortcomings, improving user interface and workflow, and enhancing interoperability with other healthcare systems. Implementation of basic telehealth functionalities would also be a priority during this phase.Phase 2 (Years 4-7): Implementation of advanced AI-powered tools for predictive analytics, risk stratification, and personalized medicine.
Expansion of telehealth capabilities to include virtual consultations, remote patient monitoring, and integration with wearable technology.Phase 3 (Years 8-10): A comprehensive review of the system’s performance and a determination of whether a full or partial replacement is necessary. This phase would involve exploring alternative EHR systems, conducting thorough testing and evaluation, and developing a detailed migration plan.
The ultimate goal is to create a fully integrated, AI-powered, and telehealth-enabled EHR system that meets the evolving needs of veterans for decades to come.
Data Security and Privacy Considerations

Source: 13newsnow.com
The extension of the Oracle Cerner contract for the Veterans Affairs EHR system necessitates a thorough examination of the data security and privacy measures in place to protect the sensitive health information of millions of veterans. This is paramount given the scale of the system and the inherent vulnerabilities associated with electronic health records. Robust security protocols are essential not only to comply with regulations but also to maintain the trust and confidence of veterans who rely on the VA for their healthcare.The VA’s approach to data security involves a multi-layered strategy encompassing various technological and procedural safeguards.
This includes encryption of data both in transit and at rest, access controls based on the principle of least privilege, regular security audits and vulnerability assessments, and a comprehensive incident response plan. However, even the most sophisticated systems are susceptible to breaches, and understanding potential vulnerabilities is crucial for proactive risk mitigation.
Data Security Measures Implemented
The VA employs a range of security measures to protect veteran health information. These include robust firewalls to prevent unauthorized access, intrusion detection systems to monitor network traffic for malicious activity, and data loss prevention (DLP) tools to prevent sensitive data from leaving the network without authorization. Multi-factor authentication is implemented to ensure that only authorized personnel can access the system.
Regular security awareness training is provided to staff to educate them about phishing scams, malware, and other social engineering tactics. Furthermore, the system undergoes regular penetration testing to identify and address potential vulnerabilities before they can be exploited. Data encryption, both at rest and in transit, is a critical component, using strong encryption algorithms to protect the confidentiality of the data.
Regular updates and patching of the system software and infrastructure are also crucial to mitigate known vulnerabilities.
Potential Vulnerabilities and Risks
Despite the implemented security measures, several vulnerabilities and risks remain. The sheer volume of data stored within the system represents a significant target for cyberattacks. Phishing attacks targeting VA employees remain a persistent threat, potentially granting malicious actors access to the system. Insider threats, either malicious or accidental, pose another significant risk. Software vulnerabilities in the EHR system itself, or in related applications, could be exploited to gain unauthorized access.
The increasing reliance on cloud-based services also introduces new vulnerabilities, requiring robust security controls and compliance with cloud security standards. Finally, the complexity of the system, with its numerous interconnected components, can make it difficult to identify and address all potential vulnerabilities. A successful breach could lead to the exposure of sensitive personal information, including medical records, social security numbers, and financial data.
HIPAA Compliance Measures
The VA’s EHR system is subject to the Health Insurance Portability and Accountability Act (HIPAA), which mandates stringent security and privacy regulations for protected health information (PHI). The system is designed to comply with HIPAA’s security rule, which Artikels administrative, physical, and technical safeguards for protecting electronic PHI. This includes implementing access controls to restrict access to PHI based on roles and responsibilities, maintaining audit trails to track access to PHI, and implementing procedures for handling and reporting security incidents.
The VA also adheres to HIPAA’s privacy rule, which Artikels requirements for the use and disclosure of PHI. This includes obtaining patient consent for the use and disclosure of PHI, except in certain limited circumstances. Regular audits and compliance reviews are conducted to ensure ongoing adherence to HIPAA regulations.
Hypothetical Data Breach Scenario and Consequences
Imagine a scenario where a phishing email successfully compromises the credentials of a VA employee with administrative privileges. The attacker gains access to the EHR system and exfiltrates a large amount of sensitive veteran health information. This data could be sold on the dark web, used for identity theft, or used to target veterans with further malicious activities.
The consequences could be devastating, including reputational damage to the VA, financial losses due to legal action and remediation efforts, and a significant erosion of public trust. Veterans could experience identity theft, financial fraud, and emotional distress. The impact on national security could also be significant if sensitive information relating to veterans’ military service were compromised. This hypothetical scenario highlights the critical importance of robust security measures and a comprehensive incident response plan.
Last Word
The extension of the Veterans Affairs EHR contract with Oracle is a complex issue with far-reaching consequences. While it promises continued access to a familiar system, critical questions remain about long-term costs, system upgrades, and data security. Ultimately, the success of this extension hinges on transparent government oversight, continuous system improvements, and a commitment to prioritizing the needs of the veterans who rely on this system for their healthcare.
It’s a story that deserves continued monitoring and public engagement to ensure our veterans receive the best possible care.
FAQ Resource
What are the key improvements promised in the extended contract?
The contract details specific upgrades to the system’s interoperability, user interface, and cybersecurity measures. Exact details are often confidential, but public statements should highlight key improvements.
How does the cost of this extension compare to previous years?
The exact figures are usually part of the confidential contract, but budgetary information is often available through public records requests or government transparency initiatives. Comparing costs year-over-year provides valuable context.
What happens if Oracle fails to meet the terms of the contract?
The contract should Artikel specific penalties and performance standards. Government oversight bodies have mechanisms to enforce these stipulations and potentially seek alternative solutions if Oracle doesn’t deliver.
Are there alternative EHR systems being considered for the future?
The VA is likely exploring long-term solutions and might consider other EHR systems. Publicly available strategic plans or reports may shed light on future system considerations.