Cytomegalovirus in Pregnancy Risks, Diagnosis, Management
What happens if you have cytomegalovirus during pregnancy risks diagnosis management – What happens if you have cytomegalovirus during pregnancy? Risks, diagnosis, and management are crucial aspects of navigating this often-unseen challenge. This common viral infection can have significant implications for both mother and baby, and understanding the potential effects, testing methods, and available care is vital for informed decision-making. Let’s delve into the complexities of cytomegalovirus (CMV) during pregnancy and explore the best strategies for mitigating potential risks.
From transmission routes and prevalence rates to the potential long-term consequences for the child, this post aims to provide a comprehensive overview of CMV in pregnancy. We’ll cover diagnostic tools, treatment options (or lack thereof in many cases!), and preventative measures you can take to protect yourself and your baby. Because knowledge is power, especially when it comes to safeguarding your pregnancy journey.
Cytomegalovirus (CMV) Infection During Pregnancy: What Happens If You Have Cytomegalovirus During Pregnancy Risks Diagnosis Management
Cytomegalovirus (CMV) is a common virus that can cause serious complications if contracted during pregnancy. Understanding how CMV is transmitted, its prevalence, and the stages of infection is crucial for expectant mothers and healthcare providers. This information aims to provide a clear overview of CMV infection during pregnancy, highlighting key aspects for informed decision-making.
Transmission of CMV to the Fetus
CMV can be transmitted to a fetus through several routes during pregnancy. The most common is vertical transmission, meaning the virus passes from the mother to the fetus across the placenta. This can occur at any point during pregnancy, but the risk of severe infection is generally higher in the first trimester. Another less common route is transmission during labor and delivery, where the infant may become infected as it passes through the birth canal.
Finally, although rare, postnatal transmission can occur through breast milk, although this is usually less severe than congenital infection. The likelihood of fetal infection varies depending on several factors, including the timing and severity of the mother’s infection.
Prevalence of Congenital CMV Infection
Globally, congenital CMV infection is a significant public health concern. Estimates suggest that 0.2% to 2.2% of infants are born with congenital CMV infection each year, varying considerably across different regions and populations. For example, regions with lower socioeconomic status or limited access to healthcare often report higher rates. In developed countries, the prevalence may be slightly lower, but it still represents a considerable number of affected infants annually.
The true prevalence is likely underestimated, as many congenital CMV infections are asymptomatic and go undiagnosed.
Stages of CMV Infection in Pregnant Women
CMV infection in pregnant women typically progresses through several stages. Initially, many women experience a primary infection, characterized by mild flu-like symptoms, which are often overlooked or misattributed to other illnesses. This asymptomatic primary infection is common and can easily be missed. Subsequently, some women may experience a reactivation of a previous CMV infection, where the virus, dormant in the body, becomes active again.
So, you’re worried about cytomegalovirus (CMV) during pregnancy? The risks are real, including potential birth defects, and early diagnosis is key for management strategies. Maintaining a healthy diet is crucial during pregnancy, and understanding nutritional needs is vital – that’s why I found this article on are women and men receptive of different types of food and game changing superfoods for women so insightful.
Knowing what foods support a healthy pregnancy can help mitigate some of the risks associated with CMV, alongside medical advice, of course. Remember, early detection and a healthy lifestyle are your best allies in navigating a CMV-positive pregnancy.
Reactivation is usually less severe than a primary infection. The severity of the maternal infection does not always correlate directly with the severity of the fetal infection; however, a primary infection during pregnancy carries a greater risk of transmission to the fetus than reactivation. Understanding these stages helps in risk assessment and potential management strategies.
Risks Associated with CMV Infection During Pregnancy
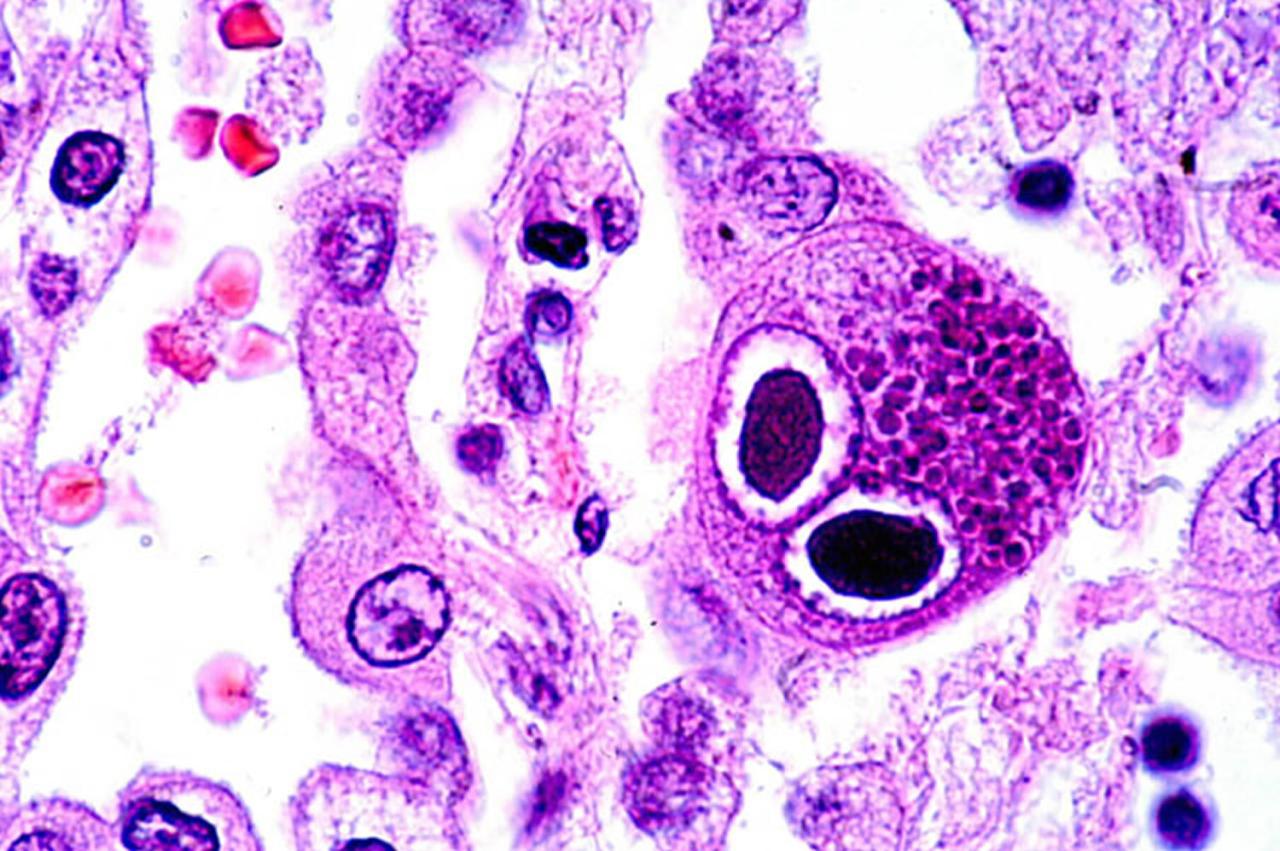
Source: healthjade.net
Cytomegalovirus (CMV) infection during pregnancy poses significant risks to both the mother and, more importantly, the developing fetus. While many pregnant women experience asymptomatic CMV infection, a considerable percentage of infants born to infected mothers will experience congenital CMV, leading to a range of health problems. The severity of these problems varies greatly depending on several factors, including the timing and severity of the maternal infection.
Understanding these risks is crucial for appropriate prenatal care and management.
Short-Term Effects of Congenital CMV Infection on Newborns
Congenital CMV infection can manifest in newborns in various ways, ranging from mild to severe. Some infants may show no symptoms at birth, while others exhibit a wide spectrum of problems. Short-term effects often become apparent in the first few weeks or months of life and can include jaundice (yellowing of the skin and eyes), low birth weight, hepatosplenomegaly (enlarged liver and spleen), petechiae (small red or purple spots on the skin), and microcephaly (abnormally small head size).
Infants with symptomatic congenital CMV may also experience hearing loss, which might not be immediately detectable. These early signs often prompt further investigation and diagnosis. The presence of these symptoms warrants immediate medical attention and close monitoring for potential long-term complications.
Long-Term Health Consequences of Congenital CMV
The long-term effects of congenital CMV infection can be significant and far-reaching. Even infants who appear healthy at birth may develop complications later in life. These long-term consequences often affect sensory organs and the neurological system. Hearing loss is a particularly common and serious long-term complication, potentially leading to speech and language delays. Vision impairment, including retinitis (inflammation of the retina), can also occur.
Neurological problems such as intellectual disability, cerebral palsy, and seizures are other potential long-term effects. The severity of these long-term complications is highly variable and depends on several factors, including the timing and severity of the maternal infection, as well as individual factors. Early intervention and supportive care are crucial in mitigating these long-term consequences.
Severity of Potential Complications Based on Timing of Infection
The timing of CMV infection during pregnancy significantly impacts the likelihood and severity of congenital CMV in the newborn. Infection early in pregnancy (first trimester) is associated with a higher risk of severe complications compared to later infections.
| Timing of Infection | Frequency of Severe Outcomes | Common Symptoms | Long-Term Effects |
|---|---|---|---|
| First Trimester | High | Microcephaly, severe intellectual disability, hearing loss, vision impairment, seizures | Significant intellectual disability, severe hearing loss, vision impairment, cerebral palsy |
| Second Trimester | Moderate | Hearing loss, hepatosplenomegaly, jaundice | Hearing loss, mild to moderate intellectual disability, developmental delays |
| Third Trimester | Low | Hearing loss, jaundice | Mild hearing loss, few other significant long-term effects |
Risk Factors for CMV Infection and Transmission to the Fetus
Several factors increase the likelihood of a pregnant woman contracting CMV and transmitting it to her fetus. These include close contact with young children (who are often asymptomatic carriers), exposure to saliva or urine of infected individuals, and occupational exposure (for example, healthcare workers). Women who have multiple children or work in childcare settings are at increased risk.
Additionally, maternal immune status plays a role; individuals with compromised immune systems are more susceptible to severe infection. Understanding these risk factors allows for preventative measures and early detection strategies.
Diagnosis of CMV Infection in Pregnant Women
Diagnosing cytomegalovirus (CMV) infection during pregnancy is crucial for managing potential risks to the developing fetus. Several methods are available, each with its strengths and limitations, and the approach often depends on the clinical context and the timing of testing. Accurate diagnosis relies on differentiating between primary (first-time) infection and reactivation of a previous infection.
Methods for Screening and Diagnosing CMV Infection
Screening for CMV infection in pregnant women typically involves testing for the presence of CMV antibodies in the mother’s blood. These tests can detect both IgM and IgG antibodies. IgM antibodies generally indicate a recent infection, while IgG antibodies suggest past exposure or infection. However, the interpretation of these tests can be complex and requires careful consideration of the clinical picture.
Interpreting CMV Antibody Tests
The presence of CMV IgM antibodies alone is often interpreted as suggestive of a recent infection, although it’s not definitive proof of active infection during pregnancy. A positive IgM test along with a rising titer of IgG antibodies (meaning the IgG antibody levels are increasing over time) strongly supports an active primary infection. Conversely, the presence of IgG antibodies alone usually indicates past infection and immunity, meaning the mother is unlikely to experience a primary infection during the current pregnancy.
However, a negative IgM test with a positive IgG test does not entirely rule out a primary infection.
Limitations and Potential for False Results
It’s crucial to understand that CMV antibody tests are not perfect. False-positive IgM results can occur, especially in women with autoimmune diseases or other infections that cross-react with the CMV IgM test. Conversely, false-negative results are possible, particularly in early stages of infection when antibody levels are still low. Furthermore, some individuals with past CMV infection might have low levels of IgG antibodies, potentially leading to a false-negative result.
These limitations highlight the importance of considering the clinical presentation and other factors when interpreting the results. For example, a woman with symptoms consistent with CMV infection but with a negative antibody test might benefit from further investigations, including PCR testing.
Polymerase Chain Reaction (PCR) Testing
PCR testing directly detects the CMV DNA in various samples, including blood, urine, and amniotic fluid. This method offers a more direct detection of active viral replication compared to antibody testing. A positive PCR test from a maternal blood sample suggests active CMV infection, while a positive PCR test from amniotic fluid indicates fetal infection. However, PCR testing is more expensive and complex than antibody testing, and it’s not always readily available.
Also, a negative PCR result doesn’t definitively rule out infection, particularly in the early stages.
Interpreting PCR Results and their Limitations
A positive PCR result from maternal blood provides strong evidence of active infection. However, it doesn’t automatically imply fetal infection. The risk of fetal transmission is higher with primary infection compared to reactivation. Conversely, a negative PCR result doesn’t rule out infection entirely, especially in the early stages of infection. Also, the sensitivity of PCR can vary depending on the laboratory and the method used.
For example, a test with low sensitivity might miss a low viral load. Therefore, it is critical to interpret the PCR results alongside clinical findings and other laboratory data.
Management of CMV Infection During Pregnancy

Source: rockvilleobgyn.com
Managing cytomegalovirus (CMV) infection during pregnancy presents a unique challenge because there’s no universally effective treatment to prevent congenital CMV infection. The approach is largely determined by the gestational age at infection and the severity of the mother’s illness. The focus is primarily on monitoring the mother and fetus and providing supportive care.
Current treatment options are limited and often focused on managing symptoms rather than directly eradicating the virus. The decision to intervene therapeutically is carefully considered and depends heavily on the individual circumstances of the pregnancy. Expectant management, meaning close monitoring without specific antiviral therapy, is the most common approach.
Treatment Options for CMV Infection During Pregnancy
While there’s no cure for CMV, treatment focuses on alleviating symptoms and supporting the pregnant woman’s overall health. In some cases, antiviral medications might be considered, particularly if the mother experiences severe symptoms or if there’s evidence of significant fetal involvement. The most commonly used antiviral medication is ganciclovir, but its use during pregnancy is carefully weighed against potential risks to the developing fetus.
Other antivirals, such as valganciclovir, may also be considered in certain situations. These medications are usually reserved for severe cases and their use should be determined in consultation with specialists experienced in managing CMV infection in pregnancy. The decision to use antiviral medication will be based on a thorough assessment of the risks and benefits for both the mother and the fetus.
So, you’re worried about cytomegalovirus (CMV) during pregnancy? The risks can range from mild to severe, depending on when infection occurs. Diagnosis involves blood tests, and management focuses on supportive care. It’s a stark reminder of how important good health is, especially when you see news like the recent hospitalization of Monali Thakur, as reported in this article monali thakur hospitalised after struggling to breathe how to prevent respiratory diseases , highlighting the need to protect ourselves from respiratory illnesses.
Returning to CMV, early detection is key to minimizing potential complications for both mother and baby.
Rationale for Expectant Management
Expectant management, involving close monitoring of the mother and fetus, is the standard approach for most CMV infections during pregnancy. This is primarily because the majority of CMV infections during pregnancy are asymptomatic or cause only mild symptoms in the mother. In these cases, the risk of significant fetal complications is relatively low. Furthermore, the potential side effects of antiviral medications, especially during pregnancy, need to be carefully considered.
The benefits of antiviral treatment in most cases are not clearly established and may not outweigh the potential harm to the developing fetus. The goal of expectant management is to identify and manage any potential complications promptly, while minimizing unnecessary interventions. Regular monitoring includes ultrasounds to assess fetal growth and development, and blood tests to monitor the mother’s health.
Decision-Making Flowchart for Managing CMV Infection
The decision to pursue active treatment versus expectant management is complex and requires careful consideration of multiple factors. The following flowchart illustrates a simplified decision-making process:
Flowchart: Imagine a flowchart with two main branches stemming from “CMV Infection Diagnosed in Pregnancy”.
Branch 1: Asymptomatic Mother or Mild Symptoms, Normal Fetal Ultrasound
This branch leads to “Expectant Management: Close Monitoring (Ultrasound, Blood Tests)” which then leads to “Regular Follow-up Appointments”.
Branch 2: Symptomatic Mother (Severe Symptoms) OR Abnormal Fetal Ultrasound Findings
This branch leads to “Consultation with Maternal-Fetal Medicine Specialist”. This then leads to a decision point: “Consider Antiviral Therapy (Ganciclovir/Valganciclovir) based on severity of maternal and fetal involvement. Weigh risks and benefits carefully.” This then leads to either “Antiviral Therapy initiated and close monitoring” or “Expectant Management with close monitoring”.
This flowchart provides a general Artikel. The actual management will be tailored to the individual patient’s specific circumstances, including gestational age at infection, the severity of maternal symptoms, and any evidence of fetal involvement. The decision-making process should always involve a multidisciplinary team, including obstetricians, infectious disease specialists, and neonatologists.
Prevention of CMV Transmission During Pregnancy
Preventing cytomegalovirus (CMV) infection during pregnancy is crucial because infection can lead to serious complications for the developing baby. While there’s no vaccine currently available, proactive measures can significantly reduce the risk of contracting and transmitting CMV. This involves understanding the routes of transmission and implementing practical strategies to minimize exposure.The primary routes of CMV transmission are through contact with bodily fluids, particularly saliva, urine, and respiratory secretions, of infected individuals.
Infants and young children are especially likely to shed the virus, making close contact with them a significant risk factor for pregnant women. Understanding this transmission pathway is the first step in effective prevention.
Hygiene Practices to Reduce CMV Risk
Maintaining rigorous hygiene practices is fundamental in preventing CMV transmission. Thorough handwashing is the cornerstone of this strategy. It’s essential to wash hands frequently and meticulously, especially after contact with children, diapers, or surfaces that may be contaminated with saliva or urine. Handwashing should involve using soap and water for at least 20 seconds, paying particular attention to the areas between fingers and under fingernails.
The use of alcohol-based hand sanitizers can be supplementary but should not replace thorough handwashing with soap and water. Additionally, avoiding touching your face, especially your eyes, nose, and mouth, can help prevent the virus from entering your body.
Strategies for Reducing Contact with Young Children
Given the high rate of CMV shedding among young children, limiting close contact is a vital preventative measure. While avoiding all contact is unrealistic, pregnant women can take steps to minimize exposure. This might involve asking others to care for young children, particularly those in daycare or preschool settings where the risk of CMV exposure is higher. If direct contact is unavoidable, ensure thorough handwashing before and after any interaction.
It’s also advisable to avoid sharing utensils, cups, or other personal items with young children. Remember that CMV can also be transmitted through breast milk, though the risk of severe infection in the infant is generally low.
Awareness of CMV Symptoms and Seeking Medical Advice
Recognizing potential CMV symptoms is crucial for early intervention. While many CMV infections are asymptomatic, some individuals experience flu-like symptoms such as fever, fatigue, muscle aches, and swollen glands. If a pregnant woman experiences these symptoms, particularly in the context of potential CMV exposure, seeking immediate medical attention is vital. Early diagnosis allows for appropriate monitoring and management of the pregnancy, minimizing potential risks to the developing fetus.
Prompt medical consultation allows for testing and assessment, ensuring the health of both the mother and the child.
Preventative Measures Summary
- Wash your hands thoroughly and frequently with soap and water for at least 20 seconds, especially after contact with children, diapers, or potentially contaminated surfaces.
- Use alcohol-based hand sanitizer as a supplement to handwashing, but not as a replacement.
- Avoid touching your eyes, nose, and mouth.
- Limit close contact with young children, especially those in daycare or preschool settings. If contact is unavoidable, ensure thorough handwashing before and after interaction.
- Avoid sharing utensils, cups, or other personal items with young children.
- Seek immediate medical attention if you experience flu-like symptoms, especially if you have had potential exposure to CMV.
Impact on Fetal Development
Source: amazonaws.com
Cytomegalovirus (CMV) infection during pregnancy can have a significant impact on fetal development, with the severity depending on several factors, including the timing of infection and the mother’s immune response. The virus’s ability to cross the placenta and infect fetal tissues leads to a range of potential consequences, from asymptomatic infection to severe birth defects. Understanding these mechanisms and their effects at different gestational stages is crucial for effective prenatal care and management.CMV infection disrupts fetal development through several mechanisms.
The virus directly infects fetal cells, causing cellular damage and disrupting normal cell growth and differentiation. This damage is particularly impactful on rapidly dividing cells, commonly found in developing organs. The inflammatory response triggered by the infection further exacerbates the damage, releasing cytokines and other inflammatory mediators that can harm fetal tissues. Additionally, the virus can interfere with the production of essential proteins and signaling molecules necessary for proper organ development.
The specific effects depend on which organs and tissues are infected and the stage of development at the time of infection.
Effects on Specific Organ Systems
CMV’s impact on fetal development is multifaceted, affecting various organ systems. The most commonly affected organs include the brain, eyes, ears, and liver. Infection of the brain can lead to microcephaly (small head size), intellectual disability, seizures, and cerebral palsy. Eye infections can result in chorioretinitis (inflammation of the retina and choroid), which can cause vision impairment or blindness.
Hearing loss is another common complication, often resulting from damage to the inner ear. Liver involvement can manifest as hepatomegaly (enlarged liver) and jaundice. Other organs, such as the lungs, spleen, and kidneys, may also be affected, although less frequently. The severity of organ involvement varies widely depending on several factors, including gestational age at the time of infection and maternal immune response.
Impact of Infection Timing
The timing of CMV infection during pregnancy significantly influences the severity of its effects on fetal development. Infections occurring early in pregnancy (first trimester) tend to result in more severe outcomes due to the rapid organogenesis occurring during this period. Infection during this critical stage can lead to more extensive damage and a higher incidence of major birth defects.
Later infections (second and third trimesters) may still cause problems, but these are often less severe, potentially resulting in milder developmental delays or hearing loss rather than major structural abnormalities. However, even late-term infections can still lead to significant health consequences for the newborn. For instance, a late infection could cause a less severe hearing loss compared to an early infection that might cause severe intellectual disability.
This highlights the importance of early diagnosis and management strategies.
Potential Birth Defects Associated with Congenital CMV Infection
Congenital CMV infection can lead to a wide range of birth defects. The list below highlights some of the potential complications:
The severity and combination of these defects vary greatly depending on factors such as the timing of infection, viral load, and maternal and fetal immune responses. Some infants may have only mild symptoms, while others may experience severe disabilities requiring lifelong medical care.
- Microcephaly (small head size)
- Intellectual disability
- Hearing loss
- Vision impairment (including chorioretinitis)
- Seizures
- Cerebral palsy
- Hepatomegaly (enlarged liver)
- Jaundice
- Petechiae (small red or purple spots on the skin)
- Thrombocytopenia (low platelet count)
- Intrauterine growth restriction (IUGR)
- Premature birth
Postnatal Management and Follow-up
The birth of a baby diagnosed with congenital cytomegalovirus (CMV) infection understandably brings a wave of concerns for parents. Postnatal management focuses on early detection of complications, providing supportive care, and minimizing long-term effects. Close monitoring and specialized interventions are crucial for optimizing the infant’s development and overall health.Postnatal care for infants with congenital CMV infection involves a multidisciplinary approach, encompassing pediatricians, ophthalmologists, audiologists, and developmental specialists.
The intensity of follow-up depends on the severity of the initial infection and the presence of any noticeable symptoms at birth. Regular check-ups are essential to track the infant’s progress and address any emerging health issues promptly.
Hearing Evaluation and Intervention, What happens if you have cytomegalovirus during pregnancy risks diagnosis management
Hearing loss is a significant concern in infants with congenital CMV infection. A comprehensive hearing assessment, typically involving auditory brainstem response (ABR) testing, is conducted soon after birth. Early detection of hearing impairment is vital, as timely intervention through hearing aids or cochlear implants can significantly improve language development and communication skills. For instance, a baby diagnosed with moderate hearing loss at one month of age might benefit from early intervention programs and hearing aids, allowing for normal language acquisition by the time they reach preschool.
So, you’re worried about cytomegalovirus (CMV) during pregnancy – the risks, diagnosis, and management can be daunting. Understanding the potential impact on your baby is crucial, and sometimes, thinking about other serious health risks can put things in perspective. For example, pre-existing conditions like high blood pressure, a major risk factor for stroke, can complicate pregnancy significantly, just as learning about risk factors that make stroke more dangerous helps you understand the seriousness of the condition.
Returning to CMV, early diagnosis and monitoring are key to managing the potential consequences for both you and your baby.
Neurodevelopmental Assessment and Support
Congenital CMV can affect brain development, potentially leading to developmental delays or disabilities. Regular neurodevelopmental assessments, including developmental milestones monitoring and neurological examinations, are crucial to identify any delays in motor skills, cognitive abilities, or language development. Early intervention services, such as physical therapy, occupational therapy, and speech therapy, can be beneficial in addressing developmental challenges and maximizing the infant’s potential.
For example, a child showing delayed motor skills at six months might benefit from physical therapy to improve their gross motor abilities, allowing them to reach developmental milestones more closely aligned with their peers.
Ophthalmological Examination and Management
Retinitis, an inflammation of the retina, is a potential complication of congenital CMV infection. Regular ophthalmological examinations are necessary to detect and manage retinitis, as early intervention can prevent vision loss. Treatment might involve antiviral medications to control the infection and prevent further retinal damage. A child with early detection of CMV retinitis might undergo antiviral treatment, preventing significant vision impairment later in life.
Long-Term Monitoring and Support
Long-term follow-up is essential for infants with congenital CMV infection. Regular check-ups continue throughout childhood and adolescence to monitor for potential long-term complications, such as hearing loss, vision problems, and developmental delays. Ongoing support from healthcare professionals and access to appropriate therapies are crucial for optimizing the child’s development and quality of life. For instance, a child with mild cognitive delays identified at age three might benefit from ongoing educational support and therapies throughout their schooling.
Support Resources for Families
Families affected by congenital CMV infection can benefit from access to support groups, online communities, and patient advocacy organizations. These resources provide valuable information, emotional support, and a sense of community for families navigating the challenges of raising a child with congenital CMV. Connecting with other families facing similar situations can provide comfort, practical advice, and a shared understanding of the challenges and triumphs involved.
Many organizations offer educational materials, counseling services, and advocacy for improved access to healthcare and support services.
Last Recap
Navigating a CMV diagnosis during pregnancy can be stressful, but armed with knowledge, you can approach this situation with confidence. Remember, early detection and understanding the potential risks are key to making informed decisions about your care. While there’s no cure for CMV, proactive measures and close monitoring can significantly improve outcomes. Don’t hesitate to reach out to your healthcare provider with any questions or concerns; their expertise is invaluable in ensuring a healthy pregnancy and a healthy baby.
General Inquiries
Can I pass CMV to my baby if I’ve had it before?
If you’ve had a CMV infection in the past, you’re likely immune and won’t re-infect your baby. However, it’s always best to discuss your history with your doctor.
What are the symptoms of CMV in pregnant women?
Many pregnant women with CMV experience no symptoms. Some may experience flu-like symptoms, which can be easily mistaken for other illnesses. This is why testing is crucial.
Is there a vaccine for CMV?
Unfortunately, there isn’t currently a vaccine for CMV. Prevention focuses on hygiene and reducing exposure.
What kind of follow-up care is needed for babies born with CMV?
Follow-up care varies depending on the severity of the infection. It often includes regular hearing tests, vision screenings, and neurological evaluations.
