What is Bickerstaffs Brainstem Encephalitis? Symptoms, Causes & Treatment
What is bickerstaffs brainstem encephalitis symptoms causes and treatment – What is Bickerstaff’s Brainstem Encephalitis symptoms causes and treatment? It’s a question that deserves a thorough answer, especially given the rarity and seriousness of this neurological condition. Bickerstaff’s Brainstem Encephalitis (BBE) is a rare autoimmune disorder that attacks the brainstem, leading to a range of debilitating symptoms. Understanding its causes, recognizing its symptoms, and knowing the available treatments are crucial for improving patient outcomes.
This post aims to shed light on this complex condition, providing you with a comprehensive overview.
We’ll delve into the specifics of BBE, exploring its symptoms from the subtle to the severe, examining the current understanding of its causes, and outlining the diagnostic process and treatment options. We’ll also touch upon the long-term prognosis and available support networks for those affected. Prepare to learn more about this fascinating and often misunderstood illness.
Introduction to Bickerstaff’s Brainstem Encephalitis
Bickerstaff’s Brainstem Encephalitis (BBE) is a rare neurological disorder characterized by acute inflammation of the brainstem, the lower part of the brain that connects to the spinal cord. This inflammation leads to a range of neurological symptoms, primarily affecting eye movement, muscle coordination, and reflexes. While serious, with prompt diagnosis and treatment, many individuals can make a full recovery.BBE’s prevalence is difficult to pinpoint precisely due to its rarity and the challenges in diagnosis.
Estimates suggest it affects only a few individuals per million people annually. The condition appears to affect both sexes equally, and there’s no clear pattern regarding age groups, although it’s more frequently observed in adults. Further research is needed to establish a more accurate understanding of its prevalence and demographics.
Historical Context and Naming Conventions
Bickerstaff’s Brainstem Encephalitis is named after Dr. Edward R. Bickerstaff, a British neurologist who first described the condition in 1958. His work highlighted the unique constellation of symptoms that differentiated it from other neurological disorders. The term “encephalitis” signifies inflammation of the brain, specifically targeting the brainstem in this instance.
The naming convention reflects the crucial contribution of Dr. Bickerstaff in identifying and characterizing this distinct neurological syndrome. While other similar conditions exist, BBE maintains its unique identity based on the characteristic clinical presentation. It’s important to note that the understanding and diagnostic criteria for BBE have evolved since its initial description, reflecting advances in neurological research and diagnostic techniques.
The core clinical features, however, remain consistent with Dr. Bickerstaff’s original observations.
Symptoms of Bickerstaff’s Brainstem Encephalitis
Bickerstaff’s Brainstem Encephalitis (BBE) presents a challenging diagnostic puzzle due to its variable and often overlapping symptoms. Understanding the typical symptom profile is crucial for early diagnosis and intervention, as prompt treatment can significantly improve outcomes. The symptoms can range from mild to severe, and their progression can be rapid or gradual.
Symptom Presentation in Bickerstaff’s Brainstem Encephalitis
The following table summarizes key symptoms, their severity, frequency of occurrence, and associated neurological impact. Remember that individual experiences can vary significantly.
| Symptom | Severity | Frequency | Associated Neurological Impact |
|---|---|---|---|
| Optic Nerve Dysfunction (e.g., blurry vision, double vision) | Mild to Severe | Very Common | Impaired visual acuity, depth perception issues |
| Ataxia (loss of coordination) | Mild to Severe | Common | Difficulty with balance, walking, fine motor skills |
| Facial Weakness | Mild to Moderate | Common | Drooping eyelids, difficulty smiling or speaking |
| Nerve Palsies (cranial nerve involvement) | Variable | Common | Weakness or paralysis of specific muscles depending on the affected nerve |
| Sensory Disturbances (numbness, tingling) | Mild to Moderate | Common | Altered sensation in various parts of the body |
Progression of Symptoms
The onset of BBE symptoms is typically acute or subacute, often developing over days to weeks. The progression can be rapid, with significant worsening of symptoms within a short period. In some cases, the symptoms may plateau after a period of rapid progression, while in others, they may gradually improve over weeks to months with treatment. The duration of the illness varies considerably depending on the severity and response to treatment.
Complete recovery is possible, but some residual neurological deficits may persist in some individuals.
Comparison with Similar Neurological Conditions
BBE shares some overlapping symptoms with other neurological conditions, such as Guillain-Barré syndrome (GBS) and Miller Fisher syndrome (MFS). However, key distinctions exist. While both GBS and MFS primarily affect peripheral nerves, BBE primarily involves the brainstem. GBS often presents with progressive weakness and paralysis starting in the legs and spreading upwards, whereas BBE often presents with ophthalmoplegia (paralysis of eye muscles) and ataxia.
MFS, a variant of GBS, is characterized by ophthalmoplegia, ataxia, and areflexia (absence of reflexes), making it more similar to BBE in symptom presentation, but again, the brainstem involvement is the key differentiator. Accurate diagnosis requires careful neurological examination and often specialized testing.
Causes of Bickerstaff’s Brainstem Encephalitis
Source: cloudfront.net
Bickerstaff’s Brainstem Encephalitis (BBE) is a rare neurological disorder, and pinpointing its exact cause remains a challenge for researchers. The current understanding points towards an autoimmune response as the primary driver, where the body’s immune system mistakenly attacks healthy tissues in the brainstem. However, the specific triggers that initiate this autoimmune reaction are still under investigation.The autoimmune nature of BBE suggests that the body’s own immune system plays a central role in the disease’s development.
This means that the immune system, designed to protect against foreign invaders like bacteria and viruses, malfunctions and begins attacking the myelin sheath surrounding nerve fibers in the brainstem. This attack disrupts the efficient transmission of nerve signals, leading to the characteristic symptoms of BBE. This process is similar to what occurs in Guillain-Barré syndrome (GBS), another autoimmune disorder affecting the peripheral nervous system.
In fact, there’s a strong association between BBE and GBS, with some patients exhibiting features of both conditions.
Autoimmune Mechanisms in BBE
The precise autoimmune mechanisms involved in BBE are not fully elucidated. However, research suggests that antibodies targeting gangliosides, a type of lipid found on the surface of nerve cells, may be implicated. These anti-ganglioside antibodies are thought to disrupt the normal function of nerve cells, contributing to the neurological deficits observed in BBE. Studies have identified various gangliosides, such as GQ1b, as potential targets of these autoantibodies.
The presence of these antibodies in the cerebrospinal fluid (CSF) of BBE patients further supports this hypothesis. Further research is needed to completely understand how these antibodies specifically contribute to the destruction of the myelin sheath and the subsequent neurological dysfunction.
Potential Triggers and Predisposing Factors
While the exact trigger for BBE remains elusive, certain factors are suspected to play a role in predisposing individuals to the condition. These include preceding infections, particularly those caused by
- Campylobacter jejuni*, a bacterium commonly associated with food poisoning. The presence of
- C. jejuni* infection may trigger an autoimmune response that cross-reacts with gangliosides in the brainstem. Other viral or bacterial infections have also been implicated, although the evidence is less conclusive. Additionally, some research suggests a possible genetic predisposition, though this area requires further investigation. It’s crucial to remember that the presence of these potential triggers does not guarantee the development of BBE; the interplay of multiple factors likely determines disease onset.
Cellular Pathophysiology of BBE
At the cellular level, BBE involves the infiltration of immune cells, such as lymphocytes and macrophages, into the brainstem. These cells release inflammatory mediators that damage the myelin sheath and nerve fibers. This inflammatory process leads to demyelination, impairing the efficient transmission of nerve impulses. The precise molecular pathways involved in this process are still under investigation, but it is believed to involve the activation of complement system and other inflammatory cascades triggered by the presence of anti-ganglioside antibodies.
The resulting damage to the brainstem leads to the wide range of neurological symptoms associated with BBE. Understanding these cellular mechanisms is crucial for developing effective therapies targeting the underlying pathophysiology of the disease.
Diagnosis of Bickerstaff’s Brainstem Encephalitis
Diagnosing Bickerstaff’s Brainstem Encephalitis (BBE) can be challenging due to its overlapping symptoms with other neurological conditions. A combination of clinical findings and supportive investigations is crucial for accurate diagnosis. There isn’t one single definitive test, but rather a process of elimination and careful observation of the patient’s presentation.The diagnostic criteria for BBE typically involve a constellation of clinical features.
The core symptoms, as we’ve discussed, include ophthalmoplegia (paralysis of eye muscles), ataxia (lack of coordination), and areflexia (absence of reflexes). The presence of these three core symptoms, along with other supporting features, strengthens the diagnostic suspicion. However, the severity and combination of symptoms can vary significantly between individuals.
Clinical Features and Supportive Investigations
The diagnostic process relies heavily on a thorough neurological examination. This examination assesses the patient’s cranial nerves (particularly those controlling eye movements), reflexes, coordination, and gait. The physician will meticulously document the presence and severity of ophthalmoplegia, ataxia, and areflexia. Other features, such as sensory disturbances, facial weakness, and altered consciousness, are also noted. These clinical observations form the cornerstone of the diagnostic assessment.
Supportive investigations may include lumbar puncture to analyze cerebrospinal fluid (CSF) for any abnormalities. While there are no specific markers for BBE in CSF, the absence of inflammatory changes associated with other conditions can be helpful in the differential diagnosis. Electrophysiological studies, such as electromyography (EMG) and nerve conduction studies, might be conducted to assess nerve function, though they are not typically diagnostic for BBE itself.
Neuroimaging studies, such as MRI of the brain and brainstem, are usually performed to rule out other structural lesions or conditions that may mimic BBE.
The Role of Neurological Examinations in Diagnosing BBE
A detailed neurological examination is paramount in diagnosing BBE. The physician carefully assesses the patient’s neurological function, paying particular attention to the presence and extent of ophthalmoplegia (the type and degree of eye muscle weakness), ataxia (the nature and severity of coordination problems), and areflexia (the absence of deep tendon reflexes). For example, a physician might observe the patient’s ability to follow objects with their eyes, their gait (how they walk), and their ability to perform fine motor tasks.
The examination’s findings, coupled with the patient’s medical history and other investigations, help in differentiating BBE from other conditions.
Ruling Out Other Conditions with Similar Symptoms
Several other neurological conditions can mimic BBE, making differential diagnosis crucial. These include Guillain-Barré syndrome (GBS), Miller Fisher syndrome (MFS), myasthenia gravis, and various forms of encephalitis. GBS, for example, also presents with areflexia and weakness, but typically affects the limbs more prominently than the brainstem. MFS, a variant of GBS, shares the ophthalmoplegia and areflexia seen in BBE, but often lacks the prominent ataxia.
Myasthenia gravis involves fluctuating muscle weakness, often affecting the eyes and facial muscles, and responds to specific treatments. Careful clinical assessment, along with supportive investigations such as electrodiagnostic studies and CSF analysis, are essential to distinguish BBE from these other possibilities. For instance, the presence of specific antibodies, such as anti-GQ1b antibodies, can be helpful in differentiating between BBE and MFS.
A thorough clinical picture, including the detailed neurological examination and the exclusion of other diagnoses, is vital for arriving at a correct diagnosis of BBE.
Treatment of Bickerstaff’s Brainstem Encephalitis
Bickerstaff’s Brainstem Encephalitis (BBE) is a rare neurological disorder requiring prompt and effective treatment to minimize long-term disability. Treatment focuses on managing the symptoms and suppressing the underlying autoimmune response. While there’s no single cure, various therapies aim to improve patient outcomes.
Immunomodulatory Therapies
Immunomodulatory therapies are the cornerstone of BBE treatment, aiming to dampen the overactive immune system attacking the brainstem. These therapies work by reducing inflammation and preventing further damage to nerve cells. The choice of therapy depends on the severity of the illness and the patient’s overall health.
- Intravenous Immunoglobulin (IVIg): IVIg is a common first-line treatment. It involves infusing concentrated antibodies into the bloodstream, which helps neutralize the harmful antibodies causing the inflammation. Studies have shown significant improvement in symptoms with IVIg treatment within a few days to weeks. A typical course might involve daily infusions for several days.
- Plasmapheresis: This procedure removes harmful antibodies from the blood plasma, effectively reducing the autoimmune attack on the brainstem. Plasmapheresis is often used in conjunction with IVIg, particularly in severe cases where a rapid response is needed. It’s a more invasive procedure compared to IVIg infusions.
- Corticosteroids: While less commonly used as a first-line treatment for BBE compared to IVIg and plasmapheresis, corticosteroids like methylprednisolone can be employed to reduce inflammation. They are often considered if IVIg and plasmapheresis are ineffective or contraindicated. However, long-term corticosteroid use carries significant side effects, so their application is usually short-term and carefully monitored.
Treatment Plan Flowchart
A simplified flowchart depicting the decision-making process in BBE management could look like this:[Imagine a flowchart here. The flowchart would begin with “Diagnosis of BBE confirmed.” The next box would offer two branches: “Severe symptoms (e.g., respiratory compromise)” and “Mild to moderate symptoms.” The “Severe symptoms” branch would lead to “Plasmapheresis + IVIg,” while the “Mild to moderate symptoms” branch would lead to “IVIg.” Both branches would then converge to a box labeled “Monitor response and adjust treatment.” This box would branch to either “Improvement: Continue supportive care and rehabilitation” or “No improvement: Consider alternative immunomodulatory therapies (e.g., corticosteroids).” Finally, all branches converge to “Long-term follow-up and rehabilitation.”]
Supportive Care and Rehabilitation
Supportive care plays a vital role in managing BBE symptoms and improving patient outcomes. This includes managing symptoms like respiratory difficulties with mechanical ventilation if needed, managing blood pressure, and providing nutritional support. Rehabilitation is crucial for regaining lost functions. This can involve physical therapy to improve mobility, occupational therapy to enhance daily living skills, and speech therapy to address communication difficulties.
The intensity and duration of rehabilitation depend on the severity of neurological deficits and the individual patient’s response to treatment. A multidisciplinary approach, involving neurologists, physiatrists, therapists, and other specialists, is often essential to provide comprehensive care.
Prognosis and Long-Term Effects of Bickerstaff’s Brainstem Encephalitis
Bickerstaff’s Brainstem Encephalitis (BBE) is a rare neurological disorder, and understanding its long-term prognosis is crucial for patients and their families. While many individuals recover significantly, the road to recovery can be lengthy and challenging, with the potential for lasting neurological effects. The severity of these effects varies greatly depending on factors like the initial severity of the illness, the promptness and effectiveness of treatment, and individual patient factors.The prognosis for BBE is generally considered good for most patients, with many experiencing a substantial improvement in symptoms within weeks or months of treatment.
However, a complete and full recovery isn’t guaranteed for everyone. Some individuals may experience persistent neurological deficits, impacting their daily lives for an extended period or even permanently.
Potential Long-Term Neurological Complications
Long-term complications following BBE can vary significantly. Some individuals may experience lingering weakness or fatigue, affecting their mobility and ability to perform daily tasks. Others might have persistent problems with balance and coordination (ataxia), leading to difficulties with walking or fine motor skills. Vision problems, such as double vision (diplopia) or blurry vision, can also persist in some cases.
So, you’re wondering about Bickerstaff’s brainstem encephalitis – symptoms like ophthalmoplegia and ataxia are pretty scary, right? Understanding the causes and treatment is crucial, and it made me think about neurological conditions in general. I recently read an interesting article about how an eye test might help detect dementia risk in older adults; you can check it out here: can eye test detect dementia risk in older adults.
Early detection of neurological issues, whether it’s Bickerstaff’s or dementia, is key for better outcomes. Researching Bickerstaff’s further, I found that autoimmune responses are often implicated in its development.
Furthermore, some patients may experience ongoing difficulties with speech (dysarthria) or swallowing (dysphagia). In severe cases, long-term cognitive impairments, including memory problems or difficulty with concentration, can occur. It’s important to note that the presence and severity of these complications are not predictable and vary widely between individuals. For example, one patient might experience complete resolution of symptoms, while another might struggle with persistent ataxia requiring ongoing physical therapy.
Available Resources and Support Networks
Navigating the challenges of BBE and its potential long-term effects requires a strong support system. Several resources are available to patients and their families:The National Institutes of Health (NIH) website provides comprehensive information on various neurological conditions, including BBE, offering valuable insights into research, treatment options, and potential long-term outcomes. Similarly, patient advocacy groups, such as the Guillain-Barré Syndrome Foundation (GBSF), often include information and support for individuals with related neurological disorders like BBE, given the overlapping symptoms and mechanisms.
These organizations often host support groups, both online and in-person, connecting patients and families with others who understand their experiences. Local hospitals and rehabilitation centers also offer crucial support, providing physical therapy, occupational therapy, and speech therapy to help patients regain lost function and adapt to any lasting disabilities. Finally, connecting with neurologists specializing in rare neurological disorders is essential for ongoing monitoring, management of any residual symptoms, and access to the most up-to-date treatment approaches.
These specialists can offer personalized advice and guidance tailored to the individual’s specific needs and circumstances.
Illustrative Case Study: What Is Bickerstaffs Brainstem Encephalitis Symptoms Causes And Treatment
Source: imrpress.com
This case study presents a fictional yet realistic portrayal of a patient experiencing Bickerstaff’s Brainstem Encephalitis (BBE), highlighting the typical progression of symptoms, diagnostic process, and treatment approach. The aim is to illustrate the complexities of this rare neurological disorder and the emotional toll it can take on both the patient and their family.Sarah, a 38-year-old woman, initially presented with a rapidly progressive ophthalmoplegia.
Within a week, she experienced double vision (diplopia), followed by difficulty focusing her eyes (blurred vision). She also reported significant weakness in her legs, leading to an unsteady gait and frequent falls. These symptoms were accompanied by ataxia (loss of coordination), making even simple tasks challenging. She also experienced significant drowsiness and confusion. Emotionally, Sarah felt immense frustration and fear as her independence was rapidly eroded.
The sudden onset and relentless progression of her symptoms were particularly distressing.
Sarah’s Diagnostic Journey, What is bickerstaffs brainstem encephalitis symptoms causes and treatment
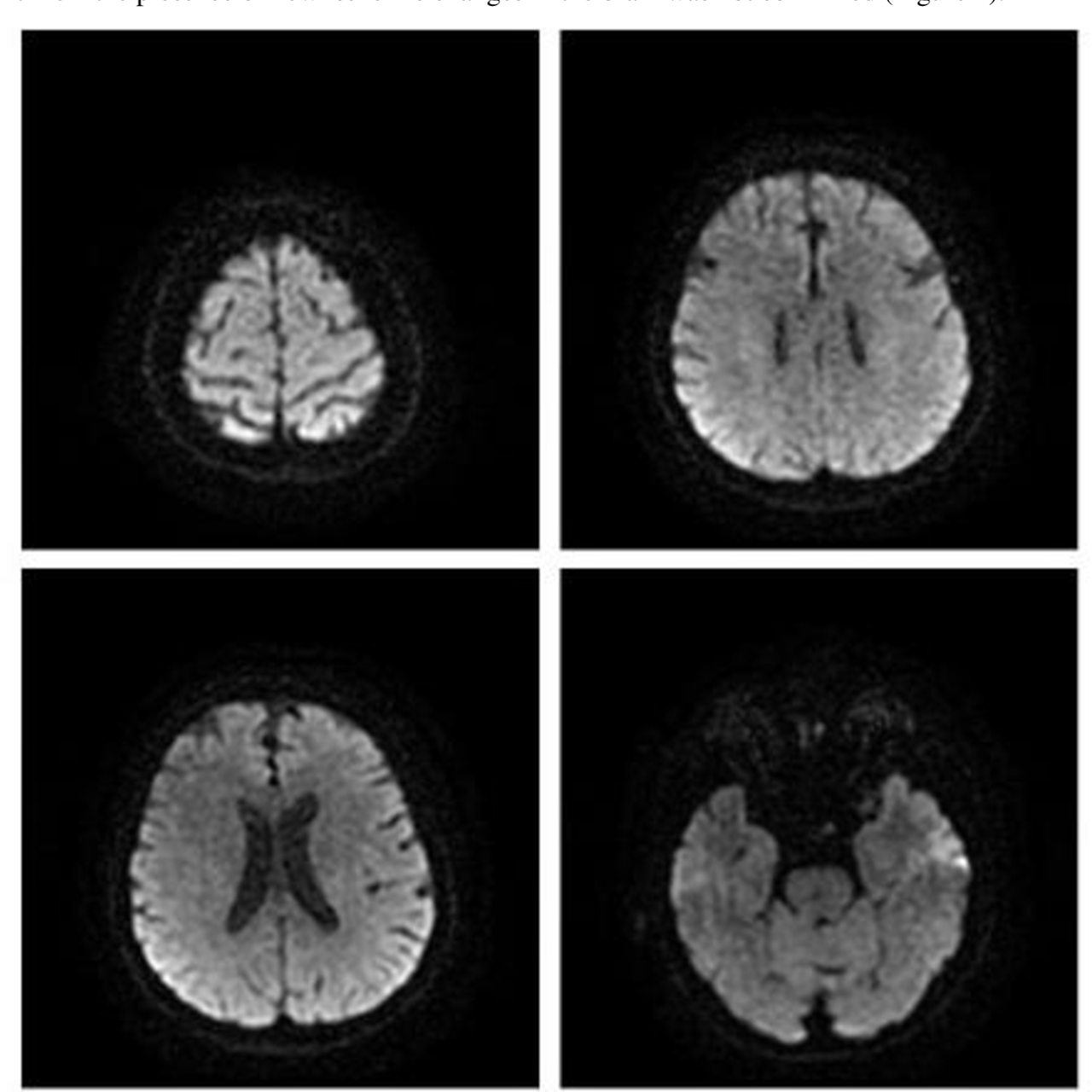
Sarah’s initial neurological examination revealed ophthalmoplegia, ataxia, and areflexia (absence of reflexes). Her cerebrospinal fluid (CSF) analysis showed elevated protein levels with normal cell counts, a common finding in BBE. Electrophysiological studies revealed evidence of demyelination, supporting the diagnosis. Her MRI scan showed subtle, non-specific abnormalities in the brainstem, consistent with the inflammation characteristic of BBE. Specifically, the MRI might have shown mild swelling and increased signal intensity in the brainstem regions controlling eye movements and coordination, without any significant lesions or large areas of damage.
The lack of clear-cut MRI findings is typical in early-stage BBE. Further supporting the diagnosis, Sarah’s symptoms started within a few weeks of a preceding upper respiratory tract infection (URI), a common trigger for BBE. The overall clinical picture, coupled with the CSF and electrophysiological findings, led to a diagnosis of BBE.
Treatment and Outcome
Sarah’s treatment involved intravenous immunoglobulin (IVIG) therapy, a cornerstone of BBE management. This therapy aimed to suppress the immune system’s attack on the brainstem. She received a five-day course of IVIG, followed by close neurological monitoring. Within a few days, she began to experience some improvement in her eye movements and leg weakness. Her ataxia also gradually lessened.
However, her recovery was slow and gradual, spanning several months. She required extensive physical and occupational therapy to regain her strength and coordination. Throughout her treatment, Sarah’s emotional well-being was closely monitored and addressed with psychological support. The constant uncertainty and fear associated with a rapidly progressing neurological illness took a significant toll on her mental health.
The support of her family and a dedicated medical team was crucial in her journey towards recovery. While Sarah made significant progress, some residual weakness and fatigue persisted even after months of rehabilitation. Her case highlights the importance of early diagnosis and aggressive treatment in improving outcomes for individuals with BBE.
Ultimate Conclusion
Bickerstaff’s Brainstem Encephalitis, while rare, presents a significant challenge for both patients and medical professionals. Understanding the intricacies of this autoimmune disorder, from its initial presentation to its long-term implications, is vital for effective diagnosis and treatment. While the journey for those affected can be arduous, advancements in immunomodulatory therapies and supportive care offer hope for improved outcomes and a better quality of life.
Remember, early diagnosis and access to specialized care are key. If you suspect BBE, seek medical attention immediately.
Question & Answer Hub
What is the life expectancy for someone with BBE?
Life expectancy varies greatly depending on the severity of the illness and the individual’s response to treatment. With prompt and effective treatment, many individuals make a full or near-full recovery. However, some may experience long-term neurological complications.
Are there genetic factors involved in BBE?
Currently, there’s no strong evidence to suggest a direct genetic link causing BBE. However, genetic predisposition to autoimmune disorders might play a role in increasing susceptibility.
Can BBE be prevented?
There’s no known way to prevent BBE. Research is ongoing to understand the triggers and develop preventative measures.
What kind of specialist should I see if I suspect BBE?
You should consult a neurologist, ideally one with experience in autoimmune neurological disorders.
