
What is Congenital Insensitivity to Pain Signs, Causes, Treatment
What is congenital insensitivity to pain signs causes and treatment – What is congenital insensitivity to pain, signs, causes, and treatment? It’s a question that unveils a fascinating, yet often heartbreaking, reality. Imagine a life without the warning signal of pain – a world where seemingly harmless actions could lead to severe injury. This condition, known as congenital insensitivity to pain (CIP), impacts individuals in profound ways, affecting not just their physical well-being but their entire lives.
We’ll delve into the mysteries of CIP, exploring its genetic roots, the challenges it presents, and the ongoing efforts to improve the lives of those affected.
Congenital insensitivity to pain is a rare disorder characterized by the inability to feel pain from birth. This lack of pain perception stems from genetic mutations that disrupt the body’s pain signaling pathways. The consequences can be devastating, leading to frequent injuries, unnoticed infections, and severe complications. Understanding the complexities of CIP, from its genetic basis to its management, is crucial for providing effective support and improving the quality of life for individuals living with this condition.
We’ll cover the diagnostic process, various treatment options, and the importance of multidisciplinary care in effectively managing CIP.
Introduction to Congenital Insensitivity to Pain (CIP): What Is Congenital Insensitivity To Pain Signs Causes And Treatment
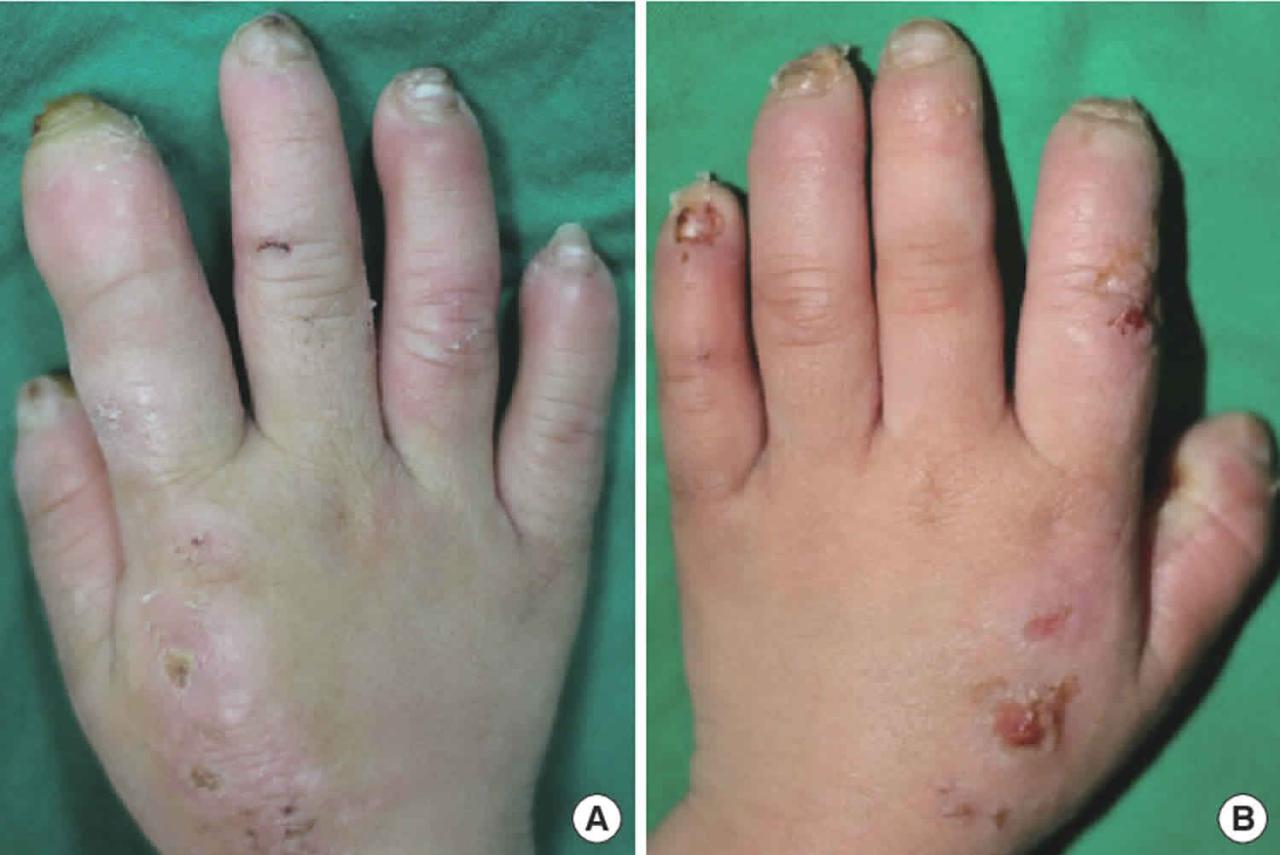
Source: healthjade.net
Congenital insensitivity to pain (CIP), also known as congenital analgesia, is a rare group of inherited disorders characterized by the inability to feel pain. This isn’t simply a reduced sensitivity; individuals with CIP experience a complete or near-complete absence of pain perception, along with other sensory deficits that can vary widely depending on the specific genetic mutation. The exact prevalence is difficult to pinpoint due to the rarity of the condition and challenges in diagnosis, but estimates suggest it affects only a few individuals per million worldwide.The impact of CIP on an individual’s life is profound and often devastating.
Without the crucial warning system of pain, individuals are at extremely high risk of severe injuries, such as burns, fractures, and infections, which often go unnoticed until they are life-threatening. This constant vulnerability leads to significant physical damage and increased morbidity. Beyond the physical risks, the lack of pain perception also impacts emotional and social development. The inability to experience the protective aspect of pain can affect self-awareness, emotional regulation, and social interactions, leading to developmental delays and behavioral challenges.
Everyday activities, from walking to eating, become fraught with danger.
Congenital insensitivity to pain (CIP) is a rare condition where individuals can’t feel pain, leading to serious injuries. Understanding its genetic causes and finding effective treatments is crucial. Interestingly, nutritional needs might play a role in overall health and well-being, which makes me wonder if the specific dietary requirements discussed in this article, are women and men receptive of different types of food and game changing superfoods for women , could potentially impact the management of CIP symptoms, though more research is needed to explore this connection.
Further research into CIP focuses on improving quality of life for those affected.
The Impact of CIP on Daily Life
The absence of pain severely limits an individual’s ability to navigate everyday life safely. Simple actions that most people take for granted, like checking the temperature of food or avoiding sharp objects, become significant challenges. For instance, a child with CIP might unknowingly burn their hand on a hot stove or repeatedly injure their mouth while chewing. They may also sustain frequent injuries from falls or collisions without realizing the extent of the damage.
This constant risk of injury can lead to significant physical limitations and reliance on caregivers for even basic tasks. The psychological consequences can be equally significant, leading to anxiety, depression, and difficulties forming relationships.
Historical Overview of CIP Research
Understanding and researching CIP has evolved significantly over time. Early documented cases often lacked the genetic understanding available today, leading to misdiagnosis and a lack of effective management strategies. The initial focus was primarily on clinical observations of affected individuals, noting the striking absence of pain perception and the resulting injuries. As genetic research advanced, scientists identified specific gene mutations responsible for various forms of CIP.
Understanding congenital insensitivity to pain involves exploring its varied signs, genetic causes, and limited treatment options. It’s fascinating how seemingly unrelated conditions can offer insights into human health; for instance, research is exploring whether an eye test, as discussed in this article on can eye test detect dementia risk in older adults , could potentially aid early diagnosis of neurological issues.
Returning to congenital insensitivity to pain, further research into its complex mechanisms is crucial for developing effective management strategies.
This breakthrough allowed for a more precise understanding of the underlying mechanisms involved in pain sensation and the development of potential diagnostic tools and therapies. The ongoing research continues to focus on identifying new gene mutations, developing effective pain management strategies (although true pain sensation cannot be restored), and improving the overall quality of life for individuals affected by CIP.
Signs and Symptoms of CIP
Congenital insensitivity to pain (CIP) manifests in a variety of ways, depending on the specific genetic mutation and its impact on nerve function. The hallmark of CIP is, of course, the inability to feel pain, but this lack of sensation extends beyond just pain, impacting other crucial sensory perceptions. The severity and presentation of symptoms can vary significantly between individuals, even within the same family.
Characteristic Symptoms of CIP
The absence of pain perception is the most striking feature of CIP. However, other sensory deficits are also common, including reduced or absent sensitivity to temperature (both hot and cold), touch, and pressure. This lack of feedback from the body can lead to a range of serious consequences. The following table summarizes common symptoms, categorized by severity and age of onset.
Note that this is not an exhaustive list, and the presentation can be highly variable.
| Symptom | Severity | Age of Onset | Frequency |
|---|---|---|---|
| Inability to feel pain | Severe | Childhood | Constant |
| Reduced temperature sensation | Moderate to Severe | Childhood | Constant |
| Self-mutilating behaviors (e.g., biting, burning) | Variable | Childhood | Variable |
| Frequent injuries (burns, fractures, cuts) | Variable | Childhood | Variable |
| Joint damage from repetitive injuries | Moderate to Severe | Adolescence/Adulthood | Variable |
| Infections (often unnoticed until advanced) | Severe | Childhood/Adulthood | Variable |
| Delayed or absent development of protective reflexes | Moderate | Childhood | Constant |
| Abnormal gait or posture due to unnoticed injuries | Moderate | Childhood/Adolescence | Variable |
| Intellectual disability (in some cases) | Variable | Childhood | Constant |
Impact on Bodily Functions
The lack of pain perception significantly impacts various bodily functions. Without the warning signal of pain, individuals with CIP are prone to serious injuries that often go unnoticed until they become severe. This can lead to complications such as chronic joint problems, bone fractures, and severe infections. Furthermore, the lack of temperature sensation can result in burns or frostbite, often without the individual realizing the damage until it’s substantial.
The absence of protective reflexes, such as pulling away from a hot stove, further increases the risk of injury.
Secondary Injuries and Complications
The most significant consequence of CIP is the high risk of secondary injuries and complications. The inability to sense pain means that even minor injuries can go untreated, leading to serious infections, chronic pain (ironically, from the untreated injuries), and permanent disability. For example, a simple cut may become infected and lead to sepsis, or a fracture may heal improperly, resulting in long-term mobility issues.
Repeated injuries to joints can cause significant arthritis and deformation. The cumulative effect of these untreated injuries can have a profound impact on an individual’s quality of life. Early diagnosis and proactive interventions are crucial in minimizing these risks.
Causes and Genetic Basis of CIP
Congenital insensitivity to pain (CIP), also known as congenital analgesia, is a rare condition characterized by the inability to feel pain. This isn’t simply a reduced sensitivity; it’s a complete absence of the sensation, leading to significant health risks due to unnoticed injuries and infections. Understanding the genetic underpinnings of CIP is crucial for diagnosis, management, and potential future therapeutic interventions.
The condition’s diverse presentation stems from mutations in several different genes, highlighting the complex interplay of proteins involved in pain signaling pathways.
Genetic Mutations Associated with CIP
Different forms of CIP are linked to mutations in various genes, each playing a crucial role in pain perception. These mutations disrupt the normal function of proteins involved in transmitting pain signals from the periphery to the brain. The specific gene affected determines the severity and specific features of the condition. For instance, mutations in the SCN9A gene are frequently associated with a complete absence of pain sensation, while mutations in other genes might lead to a milder form of the disorder.
The variations in clinical presentation reflect the complexity of the pain pathway and the multiple steps involved in pain signal transduction.
Genes Implicated in CIP and Their Roles
Several genes have been identified as being implicated in CIP. The most commonly associated gene is SCN9A, which encodes the Nav1.7 sodium channel. This channel is essential for the transmission of pain signals along nerve fibers. Mutations in SCN9A can lead to a loss of function of the Nav1.7 channel, preventing the propagation of pain signals. Other genes, such as TRKA, NTRK1, and NGF, are also involved in the development and function of pain-sensing neurons and their interactions, with mutations in these genes resulting in varying degrees of CIP.
Further research continues to identify additional genes that contribute to this complex condition.
Inheritance Patterns of CIP
CIP can be inherited in several ways, depending on the affected gene. Many cases of CIP follow an autosomal recessive inheritance pattern, meaning that two copies of a mutated gene (one from each parent) are required for the condition to manifest. In other instances, an autosomal dominant pattern is observed, where only one copy of the mutated gene is sufficient to cause the disorder.
Finally, some forms of CIP exhibit X-linked inheritance, affecting males more severely than females. The inheritance pattern is crucial for genetic counseling and family planning, allowing for accurate risk assessment for future generations.
Molecular Mechanisms Underlying the Lack of Pain Sensation
The molecular mechanisms underlying CIP are complex and multifaceted, but they generally involve disruption of the normal function of proteins involved in pain signal transduction. For example, mutations in SCN9A, as mentioned earlier, result in a non-functional or poorly functioning Nav1.7 sodium channel. This prevents the generation and propagation of action potentials along nociceptive (pain-sensing) neurons, effectively blocking the transmission of pain signals to the brain.
Other genes involved in CIP may affect different stages of pain signaling, including the production, release, or binding of neurotransmitters crucial for pain perception. The precise mechanisms vary depending on the specific gene and the nature of the mutation.
Diagnosis of CIP
Diagnosing congenital insensitivity to pain (CIP) requires a careful and thorough approach, combining clinical evaluation with specific diagnostic tests. The process aims to confirm the diagnosis, differentiate CIP from other conditions mimicking its symptoms, and identify the underlying genetic cause, if possible. Early diagnosis is crucial for implementing appropriate management strategies to minimize potential complications.
The clinical evaluation process begins with a detailed medical history, focusing on the patient’s pain perception from birth. The physician will inquire about the presence or absence of responses to painful stimuli, such as needlesticks, burns, or injuries. A comprehensive physical examination is then performed to assess for any associated anomalies, such as self-mutilating behaviors, unnoticed injuries, or signs of nerve damage.
The doctor will look for signs of recurrent infections, fractures, and joint damage, all common consequences of CIP.
Clinical Evaluation and Diagnostic Tests
The clinical evaluation plays a vital role in the diagnostic process. It involves a thorough assessment of the patient’s history of pain perception, physical examination, and neurological examination to assess the patient’s sensory function. This may include testing for responses to various types of stimuli, such as pinprick, temperature changes, and pressure. The absence of a normal pain response is a key indicator of CIP.
Further investigation may involve nerve conduction studies (NCS) and electromyography (EMG) to evaluate nerve function. These tests help to assess the integrity of the peripheral nerves and identify any underlying nerve damage that might mimic the symptoms of CIP. Genetic testing is also crucial, focusing on genes known to be associated with CIP, such as SCN9A, TRKA, and NTRK1.
These tests help identify specific genetic mutations responsible for the condition. Imaging studies, such as X-rays or MRIs, might be used to identify any injuries or damage resulting from the lack of pain sensation.
Differential Diagnosis
Several conditions can present symptoms similar to CIP, making accurate diagnosis challenging. These include conditions affecting nerve function, such as hereditary sensory and autonomic neuropathies (HSANs), which are a group of inherited disorders affecting sensory and autonomic nerves. These conditions may cause reduced or absent pain sensation, but they usually present with additional symptoms such as muscle weakness, sweating abnormalities, and gastrointestinal issues.
Other conditions that can mimic CIP include certain types of central nervous system disorders affecting pain processing, or severe mental illnesses where individuals might not report pain even if it is experienced. Careful consideration of the patient’s complete clinical picture and the use of appropriate diagnostic tests are essential to differentiate CIP from these other conditions.
Diagnostic Flowchart
The following flowchart Artikels the steps involved in the diagnosis of CIP:
Start → Detailed Medical History (Pain Perception from Birth) → Comprehensive Physical Examination (Anomalies, Injuries) → Neurological Examination (Sensory Function Testing) → Absence of Normal Pain Response? → Yes: Further Investigations (NCS, EMG, Genetic Testing, Imaging) → Genetic Mutation Identified? → Yes: Diagnosis of CIP (Specify Gene) → No: Differential Diagnosis (HSANs, other neurological conditions) → No: Investigate alternative diagnoses → End
Treatment and Management of CIP
Congenital insensitivity to pain (CIP) presents unique challenges, demanding a multifaceted approach to management. Effective treatment focuses not only on managing pain (which, paradoxically, is absent) but also on preventing injuries and mitigating the severe complications that frequently arise from the lack of pain perception. This necessitates a collaborative effort involving various medical professionals and a strong emphasis on patient education and proactive lifestyle adjustments.
Congenital insensitivity to pain (CIP) is a rare condition where individuals can’t feel pain, leading to serious injuries. Understanding its genetic causes and developing effective treatments is crucial. This reminds me of the amazing advancements in organ transplantation; the recent news that the fda approves clinical trials for pig kidney transplants in humans highlights how medical breakthroughs can improve lives dramatically.
Research into CIP, though vastly different, shares the same drive to alleviate suffering and improve quality of life.
Current Treatment Options for Managing CIP
There is no cure for CIP, as the underlying genetic defect remains. Treatment focuses entirely on managing the consequences of the condition. This primarily involves meticulous injury prevention and prompt treatment of any injuries that do occur. Pain medication is, of course, unnecessary, but managing other symptoms such as inflammation or infection is crucial. This may involve antibiotics, anti-inflammatory drugs, or other medications depending on the specific injury or complication.
Regular medical check-ups are essential for early detection and intervention.
Injury Prevention Strategies for Individuals with CIP
Given the profound risk of severe injury and infection, proactive injury prevention is paramount. This requires a multi-pronged strategy involving close monitoring, protective equipment, and environmental modifications. For instance, padding sharp corners of furniture, using protective gear during physical activities, and avoiding potentially hazardous situations are essential. Parents and caregivers of children with CIP must be exceptionally vigilant and educated on potential dangers.
Regular skin checks are also vital to detect early signs of injury or infection that might otherwise go unnoticed.
The Role of Multidisciplinary Care in Managing CIP
Effective management of CIP necessitates a team approach. A multidisciplinary team typically includes:
- Physicians: Provide regular medical check-ups, manage any infections or complications, and oversee overall care.
- Physical Therapists: Help improve motor skills, coordination, and strength, reducing the risk of falls and injuries. They can also help with range of motion and flexibility.
- Occupational Therapists: Focus on adaptive strategies for daily living, such as modified utensils or assistive devices to enhance safety and independence.
- Psychologists or Counselors: Provide emotional support for both the individual with CIP and their family, addressing the psychological challenges associated with the condition. This support is crucial in helping individuals cope with the anxieties and frustrations of living with CIP.
Preventative Measures and Lifestyle Adjustments for Individuals with CIP
Individuals with CIP and their caregivers must proactively implement numerous preventative measures and lifestyle adjustments. This includes:
- Regular check-ups: Frequent medical examinations are crucial for early detection of injuries or infections.
- Protective gear: Wearing protective clothing, padding, and helmets during activities.
- Environmental modifications: Removing hazards from the home and work environment.
- Careful monitoring: Constant vigilance for signs of injury or infection, even minor ones.
- Temperature awareness: Preventing burns from hot surfaces and frostbite from cold.
- Adaptive strategies: Using modified tools and assistive devices to perform daily tasks safely.
- Education and training: Ongoing education for the individual and their caregivers on injury prevention and self-care.
- Stress management techniques: Employing strategies to manage stress and anxiety, which can be heightened by the condition.
Illustrative Case Studies
Understanding the diverse manifestations and management strategies for Congenital Insensitivity to Pain (CIP) is best achieved through examining individual cases. While each person’s experience is unique, these examples illustrate the broad spectrum of challenges and the importance of tailored care.
Case Study 1: A Young Child with CIP and Self-Injurious Behavior
Eight-year-old Lily was diagnosed with CIP at age two after repeatedly sustaining unnoticed injuries. Her parents initially attributed her frequent bruises and cuts to clumsiness. However, Lily’s lack of response to pain, coupled with her frequent self-biting and head-banging, raised concerns. Lily’s CIP is associated with a mutation in the SCN9A gene. Her management involves a multidisciplinary approach including regular physical therapy to improve her motor skills and reduce the risk of injury. Occupational therapy focuses on developing adaptive strategies to manage her self-injurious behaviors, and close parental supervision is crucial. Psychological support is provided to both Lily and her family to address the emotional challenges associated with her condition. Lily’s parents have learned to proactively protect her environment, removing potential hazards and employing protective gear. Despite these interventions, Lily’s life is significantly impacted by her condition, requiring constant vigilance and careful monitoring to prevent injuries.
Case Study 2: An Adolescent with CIP and Limited Awareness of Injury, What is congenital insensitivity to pain signs causes and treatment
Fifteen-year-old David was diagnosed with CIP later in life, initially presenting with recurrent, unnoticed fractures. His CIP is linked to a mutation in the TRKA gene. David’s lack of pain sensation resulted in a series of serious injuries, including multiple bone fractures and severe burns. He has limited awareness of the extent of his injuries, requiring constant monitoring by his caregivers. His treatment focuses on injury prevention through protective measures and careful environmental modifications. He receives regular medical check-ups to detect and treat injuries promptly. David’s physical therapy focuses on rehabilitation from past injuries and improving his mobility. He also participates in adaptive physical education programs to promote fitness and physical activity while minimizing risk. David’s case highlights the importance of early diagnosis and proactive management to prevent life-threatening complications. The impact on his social life is significant, limiting his participation in many typical adolescent activities.
Long-Term Prognosis and Quality of Life
The long-term prognosis and quality of life for individuals with CIP vary significantly depending on the severity and type of the condition, as well as the availability of appropriate support and medical care. Individuals with milder forms of CIP may experience fewer severe injuries and may lead relatively independent lives with appropriate preventative measures. However, those with more severe forms may face a greater risk of life-threatening injuries, chronic pain from secondary complications, and significant limitations in their daily activities.
Early diagnosis and intervention are crucial in improving the long-term outlook. Multidisciplinary management teams, including medical professionals, therapists, and social workers, play a vital role in providing comprehensive care and support.
Impact on Family Members and Caregivers
Living with a family member who has CIP presents unique challenges for family members and caregivers. The constant worry about potential injuries, the need for intense supervision, and the emotional toll of managing the condition can lead to significant stress and burnout. Families often face financial burdens associated with medical care, therapy, and specialized equipment. Social support networks and access to resources specifically designed to support families of individuals with CIP are crucial in improving the overall well-being of both the affected individual and their caregivers.
Regular access to respite care and counseling services can help alleviate stress and improve the quality of life for the entire family.
Future Research Directions
Congenital insensitivity to pain (CIP) research is a dynamic field with significant unmet needs. While progress has been made in understanding the genetic basis and developing some management strategies, much remains unknown. Further research is crucial to improve the lives of individuals affected by this debilitating condition. This section will highlight key areas requiring further investigation and potential avenues for therapeutic advancements.The complexity of CIP, with its diverse genetic causes and varying clinical presentations, necessitates a multi-pronged research approach.
A deeper understanding of the underlying molecular mechanisms is paramount to developing targeted therapies. Furthermore, research into the long-term consequences of CIP, including its impact on psychosocial development and overall quality of life, is essential for developing comprehensive support systems.
Understanding the Molecular Mechanisms of CIP
Research focusing on the precise molecular mechanisms underlying different forms of CIP is crucial. This includes a more detailed investigation into the specific roles of various genes and their protein products in nociception. This understanding could lead to the identification of novel therapeutic targets for specific CIP subtypes. For instance, studies focusing on the interaction between mutated genes and downstream signaling pathways could reveal potential points of intervention.
Furthermore, exploring the epigenetic modifications associated with CIP could unveil additional regulatory mechanisms impacting pain perception. Detailed analysis of specific gene mutations and their impact on protein function will provide a more complete picture of the disease mechanisms.
Developing Novel Therapeutic Strategies
Current treatment strategies for CIP primarily focus on managing complications and improving quality of life. However, there is a pressing need for therapies that directly address the underlying cause of the condition. Several potential avenues for therapeutic development warrant exploration. Gene therapy, for example, presents a promising approach for correcting genetic defects responsible for CIP. Research in this area is already underway, with some preclinical studies showing promising results in animal models.
Furthermore, exploring the potential of pharmacological interventions targeting specific signaling pathways affected in CIP could lead to the development of novel drugs to restore pain sensation or mitigate associated complications.
Improving the Quality of Life for Individuals with CIP
Research is also needed to improve the overall quality of life for individuals with CIP. This includes investigating the psychosocial impact of the condition and developing effective strategies for managing associated complications. Studies exploring the long-term physical and mental health outcomes of individuals with CIP, considering factors such as self-esteem, social interaction, and overall well-being, are critical. Furthermore, the development of tailored support programs and educational initiatives aimed at empowering individuals with CIP and their families is vital.
This includes providing access to comprehensive medical care, specialized education, and psychosocial support services. Longitudinal studies tracking individuals with CIP throughout their lifespan are needed to understand the long-term effects and identify areas where support is most needed.
Clinical Trial Design and Data Sharing
The rarity of CIP presents challenges for conducting large-scale clinical trials. Innovative strategies, such as international collaborations and the use of patient registries, are needed to overcome these limitations and accelerate the development of effective treatments. Furthermore, establishing standardized data collection methods and promoting open data sharing among researchers can facilitate the efficient analysis of clinical data and accelerate the pace of scientific discovery.
This collaborative approach is crucial for identifying trends and patterns that may not be apparent in smaller, isolated studies. A coordinated international effort will be vital to achieve significant progress in this area.
Ultimate Conclusion

Source: ytimg.com
Living with congenital insensitivity to pain presents unique and significant challenges, but understanding the condition is the first step towards better management and support. While a complete cure remains elusive, advancements in genetic research and improved multidisciplinary care strategies offer hope for a brighter future. The journey of those affected, along with their families and caregivers, highlights the resilience of the human spirit and the power of collaborative efforts to navigate the complexities of this rare disorder.
Let’s continue to advocate for research, raise awareness, and champion the needs of individuals living with CIP.
FAQ Insights
What is the life expectancy of someone with CIP?
Life expectancy can vary greatly depending on the severity of the condition and the presence of associated complications. With proper care and injury prevention, individuals with CIP can live relatively normal lifespans.
Are there different types of CIP?
Yes, several types of CIP exist, each caused by different genetic mutations affecting various parts of the pain pathway.
Can CIP be prevented?
Currently, there’s no way to prevent CIP as it’s primarily caused by genetic mutations.
How common is CIP?
CIP is extremely rare, with precise prevalence figures difficult to determine due to its varied presentation and underdiagnosis.
