
What is Guillain-Barré Syndrome? Doctor Explains Symptoms
What is gullain barre syndrome doctor explains symptoms – What is Guillain-Barré Syndrome? Doctor explains symptoms – that’s the burning question we’re tackling today. This rare neurological disorder can leave you feeling utterly baffled and terrified, so let’s dive in and demystify this condition. We’ll explore the symptoms, causes, diagnosis, and treatment, giving you a clearer understanding of what GBS is all about. Think of this as your friendly neighborhood guide to navigating this complex illness.
Guillain-Barré Syndrome (GBS) is a serious but thankfully uncommon condition that attacks the nervous system. It can cause muscle weakness and even paralysis, leaving many wondering what exactly is happening to their bodies. Understanding the different types of GBS, their symptoms, and the progression of the disease is key to effective management and a successful recovery. We’ll cover all of this and more, so keep reading!
Introduction to Guillain-Barré Syndrome (GBS): What Is Gullain Barre Syndrome Doctor Explains Symptoms
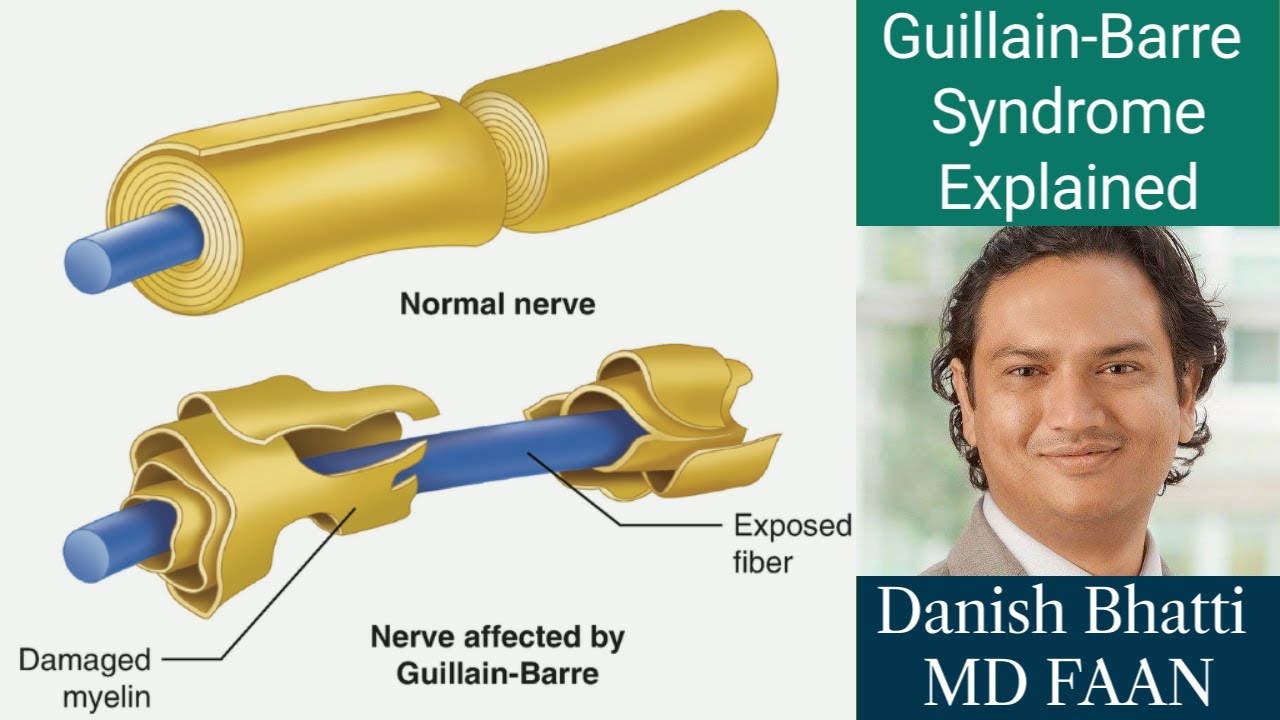
Guillain-Barré syndrome (GBS) is a rare but serious autoimmune disorder in which the body’s immune system mistakenly attacks part of the peripheral nervous system. This attack leads to inflammation that damages the myelin sheath, the protective covering around the nerves, and sometimes the nerve fibers themselves. The resulting damage disrupts communication between the brain and the body, causing a range of neurological symptoms.GBS is considered a rare condition, affecting approximately 1 to 2 people out of every 100,000 annually worldwide.
While rare, its impact on those affected is significant, often leading to temporary or, in some cases, permanent disability. The unpredictable nature of the illness and the potential for severe complications make it a serious medical concern. The rarity, however, often means that many healthcare professionals have limited experience diagnosing and managing the condition, leading to delays in treatment.
Types of Guillain-Barré Syndrome
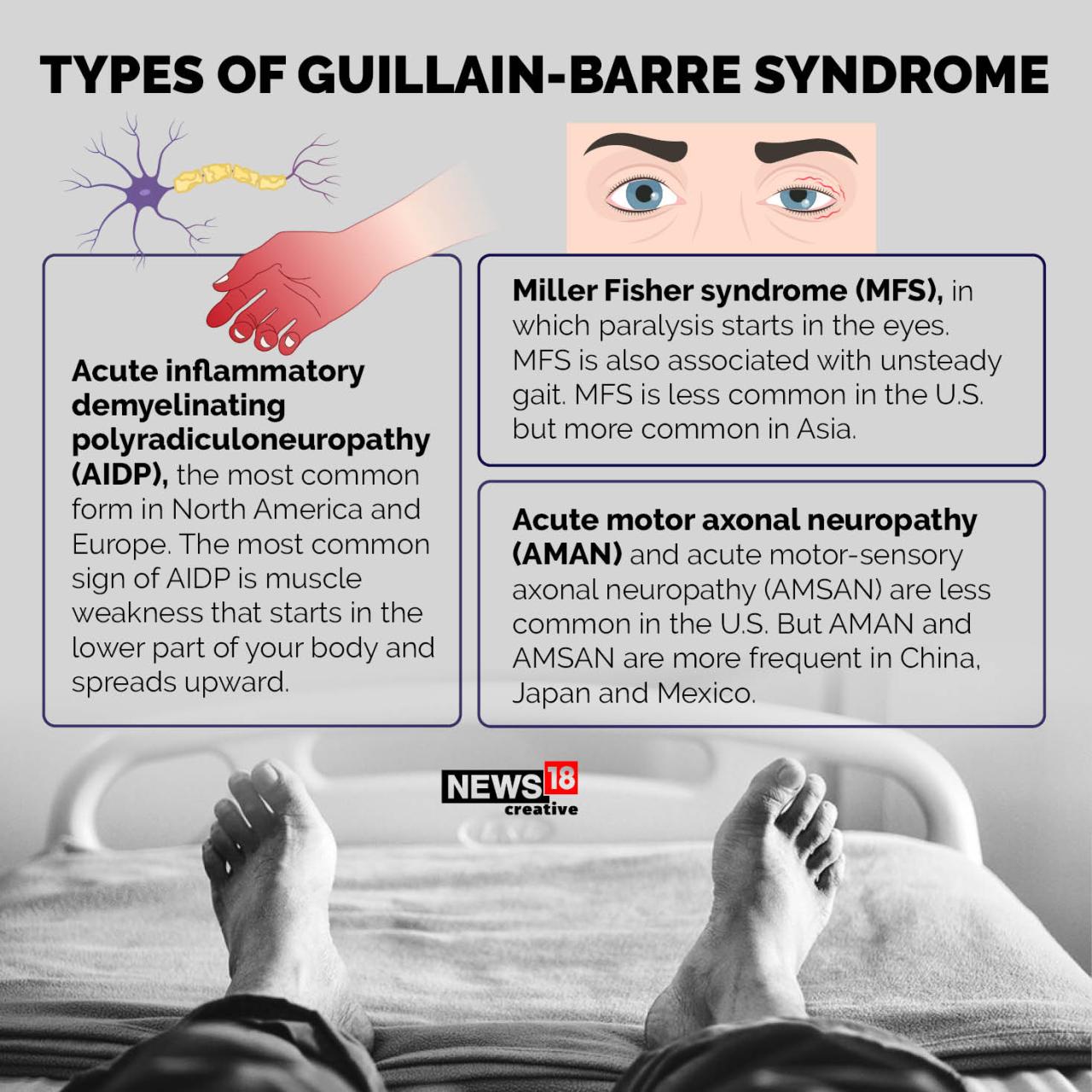
GBS isn’t a single disease, but rather a group of related disorders with variations in symptoms and progression. The classification of GBS types is complex and often involves detailed neurological examinations and nerve conduction studies. The most common forms include acute inflammatory demyelinating polyneuropathy (AIDP), acute motor axonal neuropathy (AMAN), and acute motor-sensory axonal neuropathy (AMSAN). These subtypes differ primarily in the part of the nerve affected (myelin sheath or nerve axon) and the resulting symptoms.
For instance, AIDP primarily affects the myelin sheath, leading to demyelination, while AMAN and AMSAN directly damage the nerve axons.
Clinical Manifestations of Different GBS Types
The symptoms of GBS vary depending on the type and severity of the condition. Generally, symptoms begin with weakness or tingling in the extremities, often starting in the feet and hands and gradually spreading upwards. This weakness can progress rapidly, leading to paralysis in some cases. Other common symptoms include muscle pain, decreased reflexes, difficulty with balance and coordination, and sometimes even respiratory difficulties if the paralysis affects the muscles involved in breathing.
So, I’ve been researching Guillain-Barré syndrome lately – a doctor explained the symptoms as a progressive weakness starting in the feet. It’s crazy how the body can attack itself! This made me think about organ transplantation, and I saw this amazing news: the FDA approved clinical trials for pig kidney transplants in humans – check it out fda approves clinical trials for pig kidney transplants in humans – which is incredible progress in overcoming organ shortage.
Getting back to GBS, understanding autoimmune diseases is a huge step towards better treatments.
In AIDP, the onset of symptoms is often more gradual, with the potential for more significant sensory involvement. In contrast, AMAN and AMSAN may have a more rapid onset of primarily motor weakness. The variation in symptom presentation underscores the importance of thorough neurological evaluation for accurate diagnosis and appropriate management.
Symptoms of Guillain-Barré Syndrome
Guillain-Barré syndrome (GBS) is a rare but serious autoimmune disorder that attacks the peripheral nervous system. Understanding the symptoms is crucial for early diagnosis and treatment, as the progression can be rapid and potentially life-threatening. The symptoms themselves are highly variable, but generally follow a predictable pattern.
Early Symptoms of Guillain-Barré Syndrome
The onset of GBS symptoms is often gradual, beginning with mild weakness or tingling in the extremities, usually the feet and legs. This initial phase can be easily missed, often mistaken for the flu or other common illnesses. The symptoms can progress rapidly over days or weeks, leading to more significant neurological impairment.
| Motor Symptoms | Sensory Symptoms | Autonomic Symptoms | Other Symptoms |
|---|---|---|---|
| Weakness in the legs, progressing to arms and upper body | Tingling or numbness in the extremities | Changes in blood pressure | Difficulty swallowing or speaking (dysphagia/dysarthria) |
| Difficulty walking or climbing stairs | Pain, often described as deep aching pain | Changes in heart rate | Facial weakness |
| Loss of reflexes | Muscle tenderness | Urinary retention or incontinence | Double vision or blurry vision |
| Paralysis | Sensitivity to touch | Constipation or diarrhea | Severe fatigue |
Progressive Nature and Severity of GBS Symptoms
GBS is characterized by its progressive nature. What starts as mild weakness can rapidly escalate to complete paralysis, affecting breathing and other vital functions. In severe cases, patients may require mechanical ventilation to assist with breathing. The speed of progression varies greatly among individuals, with some experiencing a more rapid decline than others. The severity also varies; some individuals may experience mild weakness, while others may become completely paralyzed.
For example, one patient might experience only mild weakness in their legs for a few weeks, while another might become completely paralyzed within days, requiring intensive care.
Less Common or Atypical GBS Symptoms
While the symptoms listed above are common, GBS can present with a wide range of atypical manifestations. These can include ophthalmoplegia (paralysis of the eye muscles), ataxia (loss of coordination), and even cognitive changes. For instance, some individuals may primarily experience facial weakness or difficulty swallowing as their initial symptom, rather than weakness in the limbs. The variability in presentation underscores the importance of considering GBS in the differential diagnosis of various neurological conditions.
Causes and Risk Factors of GBS
Guillain-Barré Syndrome (GBS) is a complex neurological disorder, and while its exact cause remains elusive, significant progress has been made in understanding the factors that contribute to its development. Research points to a connection between GBS and preceding infections, suggesting an autoimmune mechanism as the primary driver. However, the specific triggers and risk factors vary, making it crucial to understand the diverse possibilities.
The prevailing theory suggests that GBS is triggered by an autoimmune response. This means the body’s immune system mistakenly attacks its own nerve cells, specifically the myelin sheath that insulates and protects the nerves. This attack leads to inflammation and demyelination, resulting in the characteristic symptoms of weakness, numbness, and paralysis. While many cases follow a viral or bacterial infection, the exact mechanism by which the infection triggers this autoimmune response is still under investigation.
Several theories attempt to explain this complex interplay.
Infectious Triggers
A significant number of GBS cases are preceded by an infection, most commonly viral. These infections can include Campylobacter jejuni (a common bacterial cause of food poisoning), cytomegalovirus (CMV), Epstein-Barr virus (EBV), influenza, and Zika virus. The immune system, in its response to the infection, may cross-react with components of the peripheral nerves, initiating the autoimmune attack. This is often referred to as molecular mimicry, where the immune system mistakes a component of the nerve for the infectious agent.
The timing between the infection and the onset of GBS symptoms varies, but it often occurs within a few weeks. The exact mechanism by which these infections trigger GBS is an active area of research.
Genetic Predisposition
While not a direct cause, genetic factors may influence an individual’s susceptibility to GBS. Studies suggest that certain genes might increase the risk of developing the condition, possibly by influencing the immune response or the body’s ability to repair damaged nerves. However, the specific genes involved and their precise roles are not yet fully understood. Research continues to explore the complex interplay between genetic predisposition and environmental triggers in the development of GBS.
Other Risk Factors
Besides infections and genetics, several other factors may increase the risk of GBS. These include surgery, particularly those involving the abdomen or pelvis; certain medical conditions, such as lymphoma or HIV; and vaccination, although the link between vaccination and GBS is generally considered weak and statistically insignificant for most vaccines. The increased risk associated with these factors is often subtle, and more research is needed to fully elucidate their contribution to GBS development.
It’s important to note that these risk factors do not guarantee the development of GBS, but they may slightly increase the probability.
Comparison of Etiological Theories
Several theories attempt to explain the etiology of GBS. The dominant theory centers on the autoimmune response triggered by preceding infections, as described above. Another theory proposes that GBS may be triggered by a direct invasion of the peripheral nerves by the infectious agent itself, leading to nerve damage. While less prominent, this theory suggests a more direct, non-immune-mediated mechanism.
A third theory focuses on genetic predisposition, suggesting that individuals with certain genetic profiles might be more susceptible to developing GBS after exposure to a trigger. These theories are not mutually exclusive, and it’s likely that a combination of factors contributes to the development of GBS in individual cases.
Diagnosis of Guillain-Barré Syndrome
Diagnosing Guillain-Barré Syndrome (GBS) requires a careful evaluation of the patient’s symptoms, medical history, and the results of specific diagnostic tests. There’s no single test that definitively confirms GBS; instead, diagnosis relies on a combination of clinical findings and supportive evidence from neurological examinations and specialized studies. The process aims to rule out other conditions with similar symptoms, ensuring the correct treatment is initiated promptly.
Clinical Evaluation and Neurological Examination
The diagnostic journey begins with a thorough medical history, including the onset and progression of symptoms. Doctors will ask detailed questions about the nature and timeline of weakness, numbness, tingling, and other neurological changes. A comprehensive neurological examination follows, assessing muscle strength, reflexes, coordination, and sensation. The physician observes for signs of ascending paralysis, a characteristic feature of GBS, noting the extent of muscle weakness and its progression.
So, I was just reading about Guillain-Barré syndrome – a doctor explained the symptoms as a progressive muscle weakness – and it got me thinking about how unpredictable health can be. It made me remember that article I read about Karishma Mehta getting her eggs frozen, and the karishma mehta gets her eggs frozen know risks associated with egg freezing process, highlighting the importance of understanding the risks involved in medical procedures, just like with Guillain-Barré.
It really emphasizes how crucial it is to be informed about potential health issues, whether they’re rare or more common.
They’ll also assess for any other neurological abnormalities that might point towards alternative diagnoses. For example, the absence of fever might suggest a less likely association with an infectious trigger, although this is not definitive.
Nerve Conduction Studies (NCS) and Electromyography (EMG)
Nerve conduction studies (NCS) and electromyography (EMG) are crucial diagnostic tools. NCS measures the speed at which electrical signals travel along nerves. In GBS, these signals are significantly slowed down, reflecting the damage to the myelin sheath surrounding the nerves. EMG assesses the electrical activity of muscles, revealing whether nerve damage is causing muscle weakness. The results from NCS and EMG provide objective evidence of nerve dysfunction, a hallmark of GBS.
A typical finding would be slowed nerve conduction velocities across multiple nerves.
Lumbar Puncture (Spinal Tap)
A lumbar puncture, or spinal tap, involves extracting cerebrospinal fluid (CSF) for analysis. In GBS, the CSF often shows elevated levels of protein, a phenomenon known as albuminocytological dissociation. This means that the protein levels are increased, but the white blood cell count remains normal or only slightly elevated. This finding helps distinguish GBS from other inflammatory conditions of the nervous system where the white blood cell count would be significantly higher.
The absence of this finding, however, does not rule out GBS.
Diagnostic Flowchart
The diagnostic process for GBS can be visualized using a flowchart:“`[Start] –> [Clinical Evaluation & History] –> [Neurological Examination] –> [Suspicion of GBS?] |—Yes—>[NCS & EMG] –>[Slowed Nerve Conduction Velocities?] | |—Yes—>[Lumbar Puncture] –>[Albuminocytological Dissociation?] | |—No—>[Consider Alternative Diagnoses] |—No—>[Consider Alternative Diagnoses] |—Yes—>[GBS Diagnosis] |—No—>[Further Investigations/Alternative Diagnoses][End]“`This flowchart illustrates the sequential steps involved.
The presence of suggestive symptoms, confirmed by NCS/EMG findings, and supportive CSF analysis significantly increases the likelihood of a GBS diagnosis. However, alternative diagnoses must always be considered, especially if the typical findings are absent or inconclusive.
Treatment and Management of GBS
Source: ytimg.com
Guillain-Barré Syndrome (GBS) requires prompt and comprehensive medical intervention. Treatment focuses on managing symptoms, supporting vital functions, and promoting recovery. The approach is individualized based on the severity of the illness and the patient’s specific needs.Treatment for GBS primarily aims to reduce the immune system’s attack on the nerves and to support the body’s functions while the nerves recover.
This often involves a combination of therapies, with the most effective approach varying depending on the individual case.
Plasmapheresis and Intravenous Immunoglobulin Therapy
Plasmapheresis and intravenous immunoglobulin (IVIg) are the two main treatments for GBS. Plasmapheresis filters the blood to remove antibodies that are attacking the nerves. IVIg introduces healthy antibodies into the bloodstream to help neutralize the harmful antibodies. Both therapies aim to accelerate recovery and reduce the severity of the illness. Studies show that early treatment with either plasmapheresis or IVIg significantly improves outcomes for many GBS patients.
For example, a large clinical trial demonstrated a faster recovery time and reduced need for respiratory support in patients receiving IVIg compared to those receiving placebo.
Supportive Care and Managing Complications
Supportive care is crucial in managing GBS. This involves monitoring vital signs, providing respiratory support if breathing becomes difficult (e.g., through mechanical ventilation), managing pain, and preventing complications such as blood clots and pressure sores. Patients may require assistance with eating, bathing, and mobility. Close monitoring for complications like cardiac arrhythmias, autonomic dysfunction (affecting blood pressure and heart rate), and urinary retention is also vital.
For instance, a patient with severe GBS might require a tracheostomy to assist with breathing and a urinary catheter to manage bladder function.
Long-Term Effects and Rehabilitation Strategies, What is gullain barre syndrome doctor explains symptoms
While many people recover fully from GBS, some experience lingering effects. These can include muscle weakness, fatigue, numbness, pain, and difficulty with coordination. The extent of long-term effects varies widely depending on the severity of the initial illness and the individual’s response to treatment. Rehabilitation plays a vital role in recovery. This typically involves physical therapy, occupational therapy, and speech therapy, tailored to address specific challenges faced by the individual.
Physical therapy focuses on improving strength, mobility, and range of motion. Occupational therapy helps with adapting daily activities, and speech therapy can address swallowing difficulties or communication problems. A patient might undergo months or even years of rehabilitation to regain lost function and improve their quality of life. For example, a patient with residual weakness in their legs might benefit from intensive physical therapy, including exercises to strengthen leg muscles and gait training with assistive devices like a walker or crutches.
Illustrative Case Study
Source: cnbctv18.com
This case study presents a hypothetical example of a patient experiencing Guillain-Barré Syndrome (GBS), highlighting the progression of symptoms, diagnostic process, treatment, and recovery. It’s important to remember that GBS affects individuals differently, and this is just one possible presentation.
Sarah, a 35-year-old previously healthy woman, began experiencing symptoms that started subtly. Initially, she noticed a tingling sensation in her feet, which she initially dismissed as fatigue. Over the next few days, the tingling progressed to weakness, making it difficult to walk without stumbling. This weakness spread rapidly, affecting her legs and eventually her arms. She also reported difficulty swallowing and breathing.
Patient Presentation and Diagnosis
Sarah’s symptoms presented a classic picture of GBS. The ascending paralysis, coupled with the sensory disturbances, raised immediate concern.
- Onset of Symptoms: Tingling in feet progressing to weakness in legs and arms over several days.
- Neurological Examination: Revealed diminished reflexes, muscle weakness, and sensory loss in the extremities.
- Laboratory Tests: Elevated protein levels in cerebrospinal fluid (CSF) and electromyography (EMG) studies confirmed demyelination.
- Diagnosis: Guillain-Barré Syndrome (GBS), Acute Inflammatory Demyelinating Polyneuropathy (AIDP) subtype.
Patient Experience and Emotional Challenges
Sarah’s experience with GBS was incredibly challenging, both physically and emotionally. The rapid progression of her weakness was terrifying. The fear of losing the ability to breathe independently was particularly distressing. She also experienced significant emotional distress, including anxiety, depression, and frustration due to her dependence on others for even basic tasks.
The isolation of being confined to a hospital bed and the constant worry about her future were significant burdens. Support from her family, friends, and medical team was crucial in helping her navigate this difficult period.
Treatment and Recovery Process
Sarah’s treatment plan involved a multidisciplinary approach focusing on supportive care and immunotherapy. Her progress was closely monitored, and adjustments were made as needed.
| Timeline | Treatment | Symptoms | Outcome |
|---|---|---|---|
| Days 1-7 | Intravenous Immunoglobulin (IVIG) therapy initiated. Respiratory support with non-invasive ventilation. | Progressive weakness in limbs, difficulty swallowing, mild respiratory distress. | Slowed progression of weakness. |
| Weeks 2-4 | Continued IVIG therapy. Physical and occupational therapy started. | Plateau in weakness, continued difficulty swallowing, improved respiratory function. | Gradual improvement in limb strength. |
| Months 5-6 | Physical and occupational therapy continued. Gradual weaning from respiratory support. | Significant improvement in limb strength, improved swallowing, able to walk with assistance. | Increased independence in daily activities. |
| Months 7-12 | Continued outpatient physical and occupational therapy. | Continued improvement in strength and mobility. Some residual weakness remained. | Return to work on a modified schedule. Continued progress in regaining strength. |
Prevention and Future Research

Source: ytimg.com
So, my doctor explained Guillain-Barré Syndrome (GBS) as a rare autoimmune disorder attacking the nervous system, causing weakness and paralysis. It’s crucial to remember that while GBS affects the nerves, understanding vascular health is also key, as conditions like stroke pose significant dangers. Learning about the risk factors that make stroke more dangerous helps highlight the importance of overall health.
Returning to GBS, early diagnosis and treatment are vital to improve outcomes, which emphasizes the need for proactive healthcare.
Guillain-Barré Syndrome (GBS) remains a challenging neurological condition, highlighting the urgent need for both preventative strategies and advancements in treatment. While a complete prevention strategy is currently unavailable, ongoing research offers hope for improved understanding and management of this debilitating illness. This section explores current research directions and potential preventative measures.Current research efforts are focused on several key areas.
Scientists are actively investigating the precise mechanisms that trigger GBS, particularly the role of preceding infections and the body’s autoimmune response. This deeper understanding could pave the way for targeted therapies and preventative measures. Another significant area of focus is the development of novel treatments, including immunomodulatory therapies and potential therapies aimed at repairing nerve damage. Clinical trials are underway evaluating the efficacy of various treatments, aiming to improve patient outcomes and reduce long-term disability.
Furthermore, research is being conducted to identify reliable biomarkers that can predict the severity and prognosis of GBS, allowing for more personalized treatment strategies.
Understanding the Role of Infections
The link between GBS and preceding infections, particularly Campylobacter jejuni, is well-established. Research continues to delve into the specific bacterial components or viral infections that trigger the autoimmune response in susceptible individuals. This includes studying the genetic predisposition of individuals who develop GBS following infection. Identifying these triggers could lead to the development of vaccines or prophylactic treatments to prevent GBS in high-risk populations.
For instance, studies are exploring the potential of vaccines against common infectious agents like Campylobacter to reduce the incidence of GBS.
Improving Treatment Strategies
Current treatments primarily focus on supportive care and immunomodulatory therapies such as intravenous immunoglobulin (IVIg) and plasma exchange. However, these treatments are not universally effective, and some patients experience significant residual disability. Research is exploring novel therapeutic approaches, including the use of stem cells to regenerate damaged nerves, and the development of targeted therapies that modulate the autoimmune response more effectively.
Clinical trials are constantly evaluating new drugs and treatment protocols to improve outcomes for GBS patients. For example, some studies are investigating the use of certain anti-inflammatory drugs in conjunction with IVIg.
Identifying Predictive Biomarkers
Early and accurate diagnosis is crucial for effective GBS management. Research is focused on identifying reliable biomarkers that can predict the severity and prognosis of the disease. These biomarkers could help clinicians personalize treatment strategies and improve patient outcomes. Such biomarkers could range from specific blood protein levels to neurophysiological measurements, offering more precise assessments of disease progression and response to treatment.
Early identification of high-risk individuals could also allow for preventative measures.
Preventative Measures
While a definitive way to prevent GBS is not yet available, some measures might reduce the risk. Maintaining good hygiene practices to minimize the risk of infections, particularly those linked to GBS, is essential. Prompt treatment of infections, particularly gastrointestinal and respiratory infections, is also crucial. Further research is needed to fully elucidate the interaction between genetic predisposition, environmental factors, and the development of GBS.
Understanding these interactions could potentially lead to more effective prevention strategies in the future. For example, individuals with a family history of GBS might benefit from proactive strategies for preventing infections.
Epilogue
So, there you have it – a glimpse into the world of Guillain-Barré Syndrome. While it’s a challenging illness, understanding its symptoms, causes, and treatment options empowers both patients and their loved ones. Remember, early diagnosis and appropriate medical intervention are crucial for better outcomes. If you suspect you or someone you know might have GBS, don’t hesitate to seek immediate medical attention.
This isn’t just about medical facts; it’s about regaining control, fostering hope, and navigating the journey towards recovery.
Popular Questions
What is the prognosis for Guillain-Barré Syndrome?
Prognosis varies greatly depending on the severity of the case and the individual’s response to treatment. Many people recover fully, while others may experience some lingering weakness or other long-term effects.
Is Guillain-Barré Syndrome contagious?
No, Guillain-Barré Syndrome is not contagious. It’s an autoimmune disorder, meaning the body’s immune system mistakenly attacks its own nerves.
Are there any specific dietary recommendations for someone with GBS?
A balanced diet rich in fruits, vegetables, and lean protein is recommended. Nutritional needs may vary based on individual circumstances, so consulting a dietitian or nutritionist is beneficial.
How long does it take to recover from GBS?
Recovery time varies widely, ranging from weeks to months or even years in some severe cases. Many patients require extensive rehabilitation therapy.
