What is Metastatic Breast Cancer & How Are Innovations Transforming Treatment?
What is metastatic breast cancer and how are new innovations transforming its treatment? This question sits at the heart of a complex and evolving medical landscape. Metastatic breast cancer, where cancer cells have spread beyond the breast, was once considered a death sentence. But today, thanks to groundbreaking research and innovative therapies, the outlook is dramatically shifting.
We’ll delve into the realities of this disease, exploring both traditional and cutting-edge treatments, and offering a hopeful glimpse into the future of care.
We’ll unpack the science behind metastasis, explaining how breast cancer cells spread and the various ways this manifests in the body. Then, we’ll examine established treatments like chemotherapy and hormonal therapy, before diving into the exciting new world of immunotherapy, targeted therapies, and personalized medicine. We’ll also discuss the challenges that remain, such as drug resistance, and highlight the ongoing research pushing the boundaries of what’s possible.
What is Metastatic Breast Cancer?
Metastatic breast cancer, often called stage IV breast cancer, is a serious condition where cancer cells from the breast have spread to other parts of the body. This spread, known as metastasis, is a complex process involving the detachment of cancer cells from the primary tumor, their entry into the bloodstream or lymphatic system, their travel to distant sites, and their subsequent establishment of secondary tumors (metastases) in these new locations.
Understanding this process is crucial for comprehending the challenges of treating metastatic breast cancer.Metastatic Breast Cancer: The Process of MetastasisCancer cells from the original breast tumor can travel through the body via the bloodstream or the lymphatic system. Once they reach a new site, they can attach to the blood vessel walls, invade surrounding tissue, and begin to grow, forming secondary tumors.
These secondary tumors are genetically identical to the original breast cancer, meaning they share the same characteristics and respond similarly to treatments. The spread can occur over a period of time, with cancer cells potentially remaining dormant for years before forming new tumors. The unpredictable nature of this process underscores the complexity of managing metastatic disease.
Types of Metastatic Breast Cancer Based on Location of Spread
The location of the metastatic spread significantly impacts symptoms and treatment strategies. Common sites for metastasis include the bones, lungs, liver, brain, and skin. For instance, bone metastases can cause bone pain and fractures, while lung metastases might lead to shortness of breath. Liver metastases can affect liver function, and brain metastases can cause neurological symptoms. The spread to multiple sites is also common.
The specific location(s) of metastasis are crucial factors in determining the best course of treatment.
Common Symptoms and Signs of Metastatic Breast Cancer
Symptoms of metastatic breast cancer vary greatly depending on the location of the spread. However, some common signs include unexplained weight loss, persistent fatigue, bone pain, shortness of breath, persistent cough, jaundice (yellowing of the skin and eyes), neurological changes (such as headaches, seizures, or weakness), and skin lesions. It’s important to note that many of these symptoms can be caused by other conditions, but their persistence or severity warrants prompt medical evaluation.
Early detection and diagnosis are vital for effective management.
Staging Process for Metastatic Breast Cancer and Treatment Implications
Metastatic breast cancer is not staged in the same way as early-stage breast cancer. While the original breast cancer may have had a specific stage, once metastasis occurs, the cancer is classified as stage IV. However, further assessment is crucial to determine the extent of the spread, the specific locations of the metastases, and the patient’s overall health.
This information, along with the characteristics of the cancer cells (such as hormone receptor status and HER2 status), guides treatment decisions. Treatment options include systemic therapies (such as chemotherapy, hormonal therapy, targeted therapy, and immunotherapy), local therapies (such as radiation therapy and surgery), and supportive care to manage symptoms and improve quality of life. The treatment approach is highly individualized and tailored to each patient’s unique circumstances.
Regular monitoring is essential to track the disease’s progression and adjust treatment as needed.
Traditional Treatments for Metastatic Breast Cancer
Metastatic breast cancer, meaning cancer that has spread beyond the breast to other parts of the body, requires a multifaceted approach to treatment. The goal shifts from cure to managing the disease, extending life, and improving quality of life. Several traditional treatment modalities are used, often in combination, to achieve these aims.
Metastatic breast cancer, the spread of cancer beyond the breast, is a devastating diagnosis, but thankfully, innovative treatments like targeted therapies and immunotherapies are changing the game. Understanding these advancements is crucial, and it’s also important to consider other health risks; for example, learning about the risk factors that make stroke more dangerous can help us advocate for better overall health.
This holistic approach, focusing on both cancer treatment and preventative care, is vital for improving the quality of life for those facing metastatic breast cancer.
Chemotherapy
Chemotherapy uses drugs to kill cancer cells throughout the body. It’s a systemic treatment, meaning it reaches cancer cells wherever they may have spread. Different chemotherapy regimens exist, depending on the type of breast cancer, its hormone receptor status (ER, PR, HER2), and the patient’s overall health. Common chemotherapy drugs used in metastatic breast cancer include taxanes (like paclitaxel and docetaxel), anthracyclines (like doxorubicin and epirubicin), and alkylating agents (like cyclophosphamide).
The effectiveness of chemotherapy varies depending on the individual and the specific cancer. Side effects can be significant and may include nausea, vomiting, hair loss, fatigue, and decreased blood cell counts.
Hormonal Therapy
Hormonal therapy targets breast cancer cells that depend on hormones like estrogen or progesterone to grow. This treatment is particularly effective in hormone receptor-positive breast cancers (ER-positive or PR-positive). Hormonal therapy can involve medications like tamoxifen, aromatase inhibitors (like letrozole, anastrozole, and exemestane), and ovarian suppression. These therapies work by blocking the effects of hormones or reducing hormone production.
While generally less toxic than chemotherapy, side effects can still occur and include hot flashes, weight gain, fatigue, and increased risk of blood clots.
Targeted Therapy
Targeted therapies focus on specific molecules involved in cancer cell growth and survival. These therapies are often used in HER2-positive breast cancers. Trastuzumab (Herceptin) is a common example of a targeted therapy that blocks the HER2 protein, preventing cancer cell growth. Other targeted therapies may be used depending on the specific genetic makeup of the cancer. Targeted therapies can have fewer side effects than chemotherapy but can still cause fatigue, heart problems (in the case of some HER2-targeted therapies), and other side effects.
Radiation Therapy
Radiation therapy uses high-energy radiation to kill cancer cells in a specific area. In metastatic breast cancer, radiation therapy is often used to relieve symptoms caused by tumors pressing on organs or bones (palliative radiation). For example, radiation might be used to reduce pain from bone metastases or to improve breathing if a lung tumor is causing shortness of breath.
While radiation therapy targets a specific area, side effects such as skin irritation, fatigue, and nausea are possible.
Surgery
Surgery plays a limited role in the management of metastatic breast cancer. While surgery may be considered to remove a large, symptomatic tumor causing significant pain or other problems, it is generally not curative in metastatic disease. The goal of surgery in this context is often palliative, aimed at improving quality of life by relieving symptoms.
Supportive Care
Supportive care is crucial in managing the symptoms and side effects of metastatic breast cancer and its treatments. This includes managing pain, nausea, fatigue, and other symptoms through medication, physical therapy, and counseling. Nutritional support is also important to maintain strength and energy. Palliative care specialists play a vital role in providing holistic care, addressing the physical, emotional, and spiritual needs of patients and their families.
Supportive care is not just about managing symptoms; it’s about enhancing quality of life throughout the course of the disease.
Innovative Treatments Transforming Metastatic Breast Cancer Care

Source: wiserxcard.com
The fight against metastatic breast cancer is constantly evolving, fueled by groundbreaking research and the development of innovative treatment modalities. While traditional chemotherapy and hormone therapy remain cornerstones of treatment, new approaches are significantly improving outcomes and extending survival for patients. These advancements target cancer cells more precisely, minimizing harm to healthy tissues and offering new hope where previously there was limited option.
Emerging therapies are revolutionizing how we approach metastatic breast cancer. Instead of a one-size-fits-all approach, we’re seeing a move towards personalized medicine, tailoring treatments to the specific genetic makeup and characteristics of each patient’s tumor. This precision approach is leading to better responses and fewer side effects.
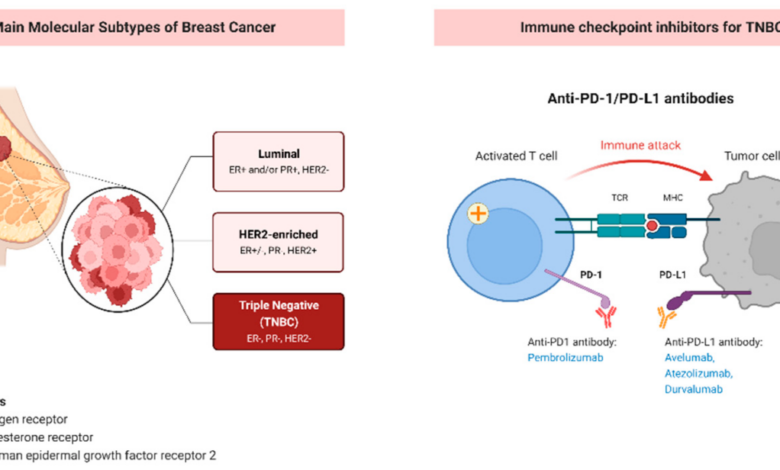
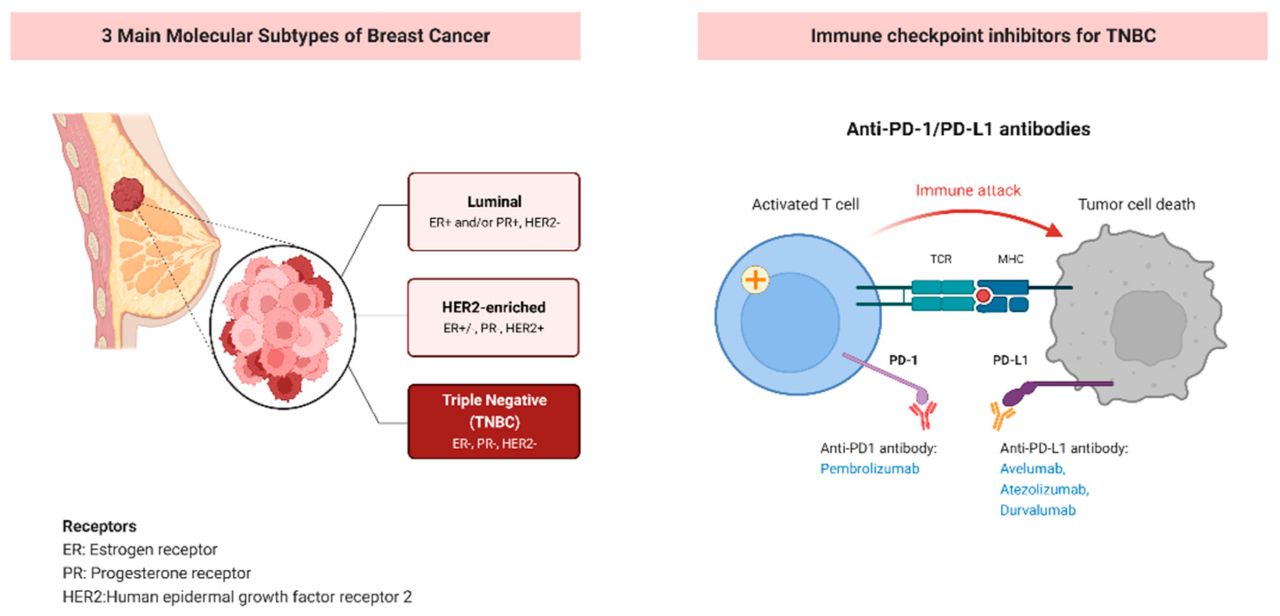
Immunotherapy in Metastatic Breast Cancer
Immunotherapy harnesses the power of the body’s own immune system to fight cancer. These treatments work by either boosting the immune system’s ability to recognize and destroy cancer cells or by blocking signals that prevent the immune system from attacking the tumor. One example is the use of checkpoint inhibitors, such as pembrolizumab and atezolizumab, which block proteins that normally keep the immune system in check.
Clinical trials have shown promising results in certain subtypes of metastatic breast cancer, particularly those with high levels of PD-L1, a protein that indicates a higher likelihood of response to checkpoint inhibitors. While not effective for all patients, for those who respond, immunotherapy can lead to durable responses and improved survival, often with manageable side effects compared to traditional chemotherapy.
Antibody-Drug Conjugates (ADCs)
Antibody-drug conjugates represent another significant advance. ADCs are essentially “smart bombs” that deliver chemotherapy directly to cancer cells. A monoclonal antibody, specifically designed to target cancer cells, is attached to a potent chemotherapy drug. This targeted delivery minimizes the drug’s impact on healthy cells, reducing side effects and improving efficacy. Trastuzumab emtansine (Kadcyla) is a prime example, targeting HER2-positive breast cancer.
Clinical trials have demonstrated improved progression-free survival and overall survival compared to traditional chemotherapy regimens in this patient population. However, ADCs are not without side effects, including fatigue, nausea, and low blood cell counts, though often less severe than those seen with traditional chemotherapy.
Novel Targeted Therapies
Beyond ADCs, several other targeted therapies are making an impact. These drugs focus on specific molecules or pathways within cancer cells that are crucial for their growth and survival. For example, CDK4/6 inhibitors, such as palbociclib, ribociclib, and abemaciclib, target proteins involved in cell cycle regulation, slowing down or stopping the growth of cancer cells. These have shown significant benefits in hormone receptor-positive, HER2-negative metastatic breast cancer, improving progression-free survival when combined with endocrine therapy.
These therapies are generally well-tolerated, with side effects such as fatigue, nausea, and low blood counts, but often manageable.
Comparative Table of Treatment Modalities
| Treatment Type | Mechanism of Action | Efficacy Rate (Illustrative Examples) | Side Effects |
|---|---|---|---|
| Traditional Chemotherapy (e.g., Doxorubicin) | Damages DNA in rapidly dividing cells | Variable, depending on the type and stage of cancer; response rates can range from 30-70% | Nausea, vomiting, hair loss, fatigue, immunosuppression, risk of heart damage |
| Immunotherapy (e.g., Pembrolizumab) | Enhances the immune system’s ability to recognize and kill cancer cells | Response rates vary significantly; some trials show response rates of 20-30% in specific breast cancer subtypes | Fatigue, rash, diarrhea, colitis, pneumonitis |
| Antibody-Drug Conjugates (e.g., Trastuzumab emtansine) | Targeted delivery of chemotherapy to cancer cells | Improved progression-free survival and overall survival demonstrated in clinical trials for HER2-positive breast cancer | Fatigue, nausea, low blood cell counts, liver toxicity |
| Targeted Therapy (e.g., Palbociclib) | Inhibits specific proteins involved in cancer cell growth | Significant improvement in progression-free survival in hormone receptor-positive, HER2-negative metastatic breast cancer when combined with endocrine therapy | Fatigue, nausea, neutropenia |
Impact of Genomics and Personalized Medicine

Source: dana-farber.org
The fight against metastatic breast cancer is increasingly reliant on precision medicine, a strategy that tailors treatment to the unique genetic makeup of each tumor. This shift from a “one-size-fits-all” approach to a highly individualized strategy is revolutionizing how we approach this challenging disease, improving outcomes and reducing unnecessary toxicities. Genomic testing plays a pivotal role in this transformation.Genomic testing helps tailor treatment strategies by identifying specific genetic alterations within the cancer cells.
These alterations can be mutations in genes that drive cancer growth, changes in the number of copies of certain genes, or alterations in the expression of genes. This information is crucial for selecting the most effective therapies and avoiding those that are unlikely to benefit the patient.
The Role of Biomarkers in Predicting Treatment Response and Identifying Potential Drug Targets
Biomarkers, measurable indicators of a biological state, act as signposts guiding treatment decisions. For instance, the presence of the HER2 protein on breast cancer cells indicates responsiveness to HER2-targeted therapies like trastuzumab. Similarly, the hormone receptor status (estrogen receptor, progesterone receptor) determines the suitability of hormone therapy. Beyond these established biomarkers, ongoing research continues to identify novel biomarkers predictive of response to newer targeted therapies or immunotherapies.
Identifying these biomarkers allows clinicians to select the most appropriate treatment from the start, maximizing efficacy and minimizing the side effects associated with ineffective treatments. This targeted approach also helps researchers develop drugs specifically designed to target these newly identified biomarkers.
Advantages and Limitations of Personalized Medicine in Metastatic Breast Cancer Treatment
Personalized medicine offers several significant advantages. Primarily, it increases the likelihood of selecting the most effective treatment from the outset, improving patient outcomes and quality of life. By avoiding ineffective treatments, it also reduces unnecessary side effects and toxicity. Furthermore, it allows for earlier intervention with targeted therapies, potentially slowing disease progression.However, personalized medicine is not without its limitations.
The cost of comprehensive genomic testing can be substantial, potentially creating access barriers for some patients. Furthermore, not all genetic alterations have known targeted therapies, and in some cases, the clinical significance of certain genomic findings remains unclear. Finally, the interpretation of genomic data requires specialized expertise, highlighting the need for robust infrastructure and trained professionals to support the widespread adoption of personalized medicine.
A Hypothetical Case Study Illustrating the Application of Genomic Information in Guiding Treatment Decisions
Consider a 55-year-old woman, Sarah, diagnosed with metastatic breast cancer. Traditional tests reveal her tumor is ER-positive, PR-positive, and HER2-negative. However, genomic testing reveals a mutation in the ESR1 gene, a gene frequently mutated in hormone receptor-positive breast cancers that have developed resistance to endocrine therapy. This information is crucial because it explains why her initial endocrine therapy failed.
Armed with this knowledge, her oncologist can adjust her treatment plan to include a therapy specifically targeting ESR1 mutations, offering a significantly improved chance of response and disease control compared to continuing with an ineffective treatment. This illustrates how genomic testing allows for dynamic treatment adjustments based on the evolving characteristics of the cancer.
Future Directions and Research: What Is Metastatic Breast Cancer And How Are New Innovations Transforming Its Treatment
Source: mdpi.com
Metastatic breast cancer, where cancer spreads beyond the breast, is a serious challenge, but thankfully, innovative treatments like targeted therapies and immunotherapies are offering new hope. It’s amazing how advancements are happening across different medical fields; for instance, research is exploring whether a simple eye test, as discussed in this fascinating article can eye test detect dementia risk in older adults , could provide early warnings of other serious conditions.
This highlights the power of medical innovation to improve lives, and similar breakthroughs are constantly pushing the boundaries of metastatic breast cancer treatment.
The fight against metastatic breast cancer is far from over. While significant advancements have been made, ongoing research holds the key to unlocking even more effective treatments and improving the lives of those affected. Scientists are tirelessly exploring new avenues, focusing on personalized approaches and innovative therapies to target the disease more precisely and minimize side effects. The future of metastatic breast cancer treatment is bright, fueled by a relentless pursuit of better outcomes.The landscape of metastatic breast cancer research is incredibly dynamic.
Several key areas are driving the development of new therapies and strategies, promising significant improvements in patient survival and quality of life. These advancements build upon the successes of targeted therapies and immunotherapies, pushing the boundaries of what’s possible in cancer treatment.
Targeted Therapies and Drug Combinations
Researchers are actively investigating novel targeted therapies that specifically attack cancer cells while sparing healthy tissues. This approach minimizes side effects and improves treatment efficacy. One promising area is the development of drugs that inhibit specific signaling pathways crucial for cancer cell growth and survival. Furthermore, combining different targeted therapies, creating synergistic effects, is showing great promise. For instance, combining a CDK4/6 inhibitor with a hormone therapy or a PARP inhibitor has shown improved outcomes in certain subtypes of metastatic breast cancer.
The careful selection and combination of these therapies are leading to more effective and personalized treatment regimens.
Immunotherapy Advancements
Immunotherapy, which harnesses the power of the body’s own immune system to fight cancer, continues to revolutionize cancer treatment. Ongoing research focuses on enhancing the effectiveness of existing immunotherapies, such as checkpoint inhibitors, and developing novel approaches, including adoptive cell therapies (ACT) and oncolytic viruses. ACT involves removing immune cells from a patient’s blood, modifying them to better target cancer cells, and then reinfusing them.
Oncolytic viruses, engineered to selectively infect and kill cancer cells, are another area of intense investigation. Clinical trials are evaluating the efficacy and safety of these approaches in various subtypes of metastatic breast cancer.
Liquid Biopsies and Early Detection
Liquid biopsies, which analyze circulating tumor DNA (ctDNA) and other biomarkers in blood samples, offer a less invasive way to monitor disease progression and response to treatment. This technology allows for early detection of relapse and the identification of resistance mechanisms, enabling timely adjustments to treatment strategies. The potential of liquid biopsies to personalize treatment and improve patient outcomes is immense.
For example, early detection of resistance mutations through liquid biopsies can allow clinicians to switch to a different targeted therapy before the disease progresses significantly.
Understanding Tumor Microenvironment, What is metastatic breast cancer and how are new innovations transforming its treatment
The tumor microenvironment, the complex network of cells and molecules surrounding cancer cells, plays a crucial role in cancer growth and metastasis. Research is focusing on understanding the intricate interactions within the microenvironment and developing therapies that target these interactions. This includes investigating the role of immune cells, stromal cells, and extracellular matrix components in tumor progression and exploring ways to manipulate the microenvironment to inhibit cancer growth.
For example, therapies targeting the tumor vasculature (blood supply) are being developed to starve cancer cells of nutrients and oxygen.
Promising Future Directions in Research
- Development of more effective and less toxic targeted therapies.
- Advancements in immunotherapy, including improved checkpoint inhibitors and adoptive cell therapies.
- Wider application of liquid biopsies for early detection and personalized treatment.
- Targeted therapies focusing on the tumor microenvironment.
- Development of novel drug delivery systems for improved efficacy and reduced side effects.
- Exploration of combination therapies to enhance treatment effectiveness.
- Improved understanding of the genetic drivers of metastatic breast cancer to enable more precise targeting.
Challenges and Opportunities
The fight against metastatic breast cancer is a complex and evolving battle. While significant advancements have revolutionized treatment approaches, substantial hurdles remain. Understanding these challenges and capitalizing on emerging opportunities is crucial for improving patient outcomes and quality of life. The journey to effective and accessible care is paved with both significant obstacles and promising avenues for progress.
One of the most significant challenges is the inherent heterogeneity of metastatic breast cancer. This means that the disease manifests differently in each individual, making it difficult to develop one-size-fits-all treatments. Furthermore, the development of drug resistance is a major obstacle. Cancer cells are remarkably adept at adapting to therapies, eventually rendering even the most effective drugs ineffective.
This necessitates the development of novel treatment strategies and a more personalized approach to care. Treatment-related toxicities also pose a significant challenge, impacting patients’ quality of life and sometimes necessitating treatment interruptions or cessation altogether. The balance between maximizing therapeutic benefit and minimizing side effects is a delicate one that requires careful consideration and ongoing monitoring.
Drug Resistance Mechanisms and Overcoming Them
Drug resistance in metastatic breast cancer is a multifaceted problem stemming from various genetic and epigenetic alterations within cancer cells. These alterations can lead to changes in drug targets, increased drug efflux, or activation of alternative survival pathways. For example, the overexpression of certain proteins can pump chemotherapy drugs out of cancer cells before they can exert their effect.
Overcoming drug resistance requires a multi-pronged approach, including the development of novel drugs that target different pathways, the combination of multiple drugs to prevent the emergence of resistance, and the use of targeted therapies that specifically attack cancer cells with certain genetic mutations. Research focusing on understanding the precise mechanisms of drug resistance is paramount in developing effective countermeasures.
Harnessing Technological Advancements for Improved Treatment
New technologies are offering unprecedented opportunities in the fight against metastatic breast cancer. Liquid biopsies, for instance, allow for the non-invasive monitoring of circulating tumor DNA (ctDNA), providing real-time insights into disease progression and response to therapy. This allows for earlier detection of resistance and facilitates timely adjustments to treatment strategies. Advances in imaging techniques, such as PET/CT scans, provide more precise visualization of tumor burden and metastasis, aiding in treatment planning and monitoring.
Furthermore, the development of novel drug delivery systems, such as nanoparticles, can enhance drug efficacy and reduce toxicity by targeting drugs specifically to cancer cells. These technological advancements hold immense promise for improving the precision and effectiveness of metastatic breast cancer treatment.
Expanding Access to Innovative Therapies and Supportive Care
Ensuring equitable access to innovative treatments and comprehensive supportive care is paramount. High costs associated with novel therapies can create significant barriers for many patients. Moreover, access to specialized healthcare professionals and facilities equipped to deliver these advanced treatments is not universally available. Addressing these disparities requires a multi-faceted approach, including policy changes to improve affordability, investment in infrastructure to expand access to specialized care, and initiatives to raise awareness and educate patients and healthcare providers about available resources.
Supportive care, encompassing psychosocial support, pain management, and nutritional counseling, is equally crucial for improving the quality of life for patients undergoing treatment for metastatic breast cancer.
Strategies to Address Challenges and Seize Opportunities
Effectively navigating the challenges and capitalizing on the opportunities in metastatic breast cancer care necessitates a collaborative and comprehensive approach.
Metastatic breast cancer, where cancer spreads beyond the breast, is a devastating disease, but breakthroughs are happening! New targeted therapies and immunotherapies are offering hope, alongside innovative surgical techniques. It’s amazing to see the progress in medicine, like the recent news that the FDA approved clinical trials for pig kidney transplants in humans, fda approves clinical trials for pig kidney transplants in humans , which shows the incredible potential of xenotransplantation.
This drive for innovative solutions mirrors the fight against metastatic breast cancer, constantly pushing for better treatments and improved patient outcomes.
- Invest in research focused on understanding and overcoming drug resistance mechanisms: This includes exploring novel drug targets, developing combination therapies, and investigating the role of the tumor microenvironment in resistance.
- Promote the development and adoption of advanced diagnostic tools: This includes liquid biopsies, advanced imaging techniques, and genomic profiling to personalize treatment strategies.
- Expand access to innovative therapies and supportive care: This requires addressing cost barriers, improving infrastructure, and enhancing healthcare provider training.
- Develop robust clinical trial networks: This will ensure that patients have access to the latest therapies and contribute to the advancement of knowledge in the field.
- Implement comprehensive patient support programs: This should encompass psychosocial support, pain management, and nutritional counseling to improve patients’ quality of life.
- Foster collaboration between researchers, clinicians, and patient advocates: This collaborative approach is essential for accelerating progress in metastatic breast cancer care.
Wrap-Up
The fight against metastatic breast cancer is far from over, but the progress made in recent years is truly inspiring. While challenges remain, the development of innovative treatments, combined with a deeper understanding of the disease at a genetic level, offers unprecedented hope. The future of metastatic breast cancer care is bright, promising more effective therapies with fewer side effects and a significantly improved quality of life for those affected.
This journey continues, driven by research, innovation, and the unwavering dedication of medical professionals and patient advocates alike.
FAQ Explained
What is the survival rate for metastatic breast cancer?
Survival rates vary greatly depending on factors like the type and stage of cancer, the patient’s overall health, and the response to treatment. It’s crucial to discuss prognosis with your oncologist for personalized information.
How is metastatic breast cancer diagnosed?
Diagnosis involves a combination of imaging tests (like mammograms, CT scans, and PET scans), biopsies, and blood tests to confirm the presence of cancer cells and determine the extent of spread.
Are there support groups for people with metastatic breast cancer?
Yes, many organizations offer support groups both in person and online. Connecting with others facing similar challenges can be incredibly beneficial.
What are the long-term side effects of treatment for metastatic breast cancer?
Long-term side effects vary depending on the specific treatments received and can include fatigue, heart problems, nerve damage, and others. Open communication with your medical team is crucial to manage these effects.
