What is Placenta Accreta Symptoms, Types, Diagnosis & Treatment
What is placenta accreta symptoms types diagnosis and treatment? This seemingly clinical question actually opens the door to a fascinating and often complex medical journey. Placenta accreta, a condition where the placenta attaches too deeply into the uterine wall, can range from relatively manageable to life-threatening, depending on its severity and type. Understanding the symptoms, the different forms of accreta (increta and percreta), and the diagnostic and treatment options is crucial for both expectant mothers and healthcare providers.
This post delves into the specifics, offering a clearer picture of this condition and its implications.
We’ll explore the physiological differences between normal placental implantation and placenta accreta, examining the various risk factors that contribute to its development. We’ll also cover the spectrum of symptoms, from subtle changes to more alarming signs, and discuss the crucial role of prenatal care in early detection. The diagnostic process, involving ultrasounds, MRIs, and other imaging techniques, will be explained in detail, followed by a look at the available treatment options, including surgical interventions and their potential complications.
Finally, we’ll examine real-world case studies to illustrate the diverse challenges and successful outcomes associated with managing placenta accreta.
What is Placenta Accreta?
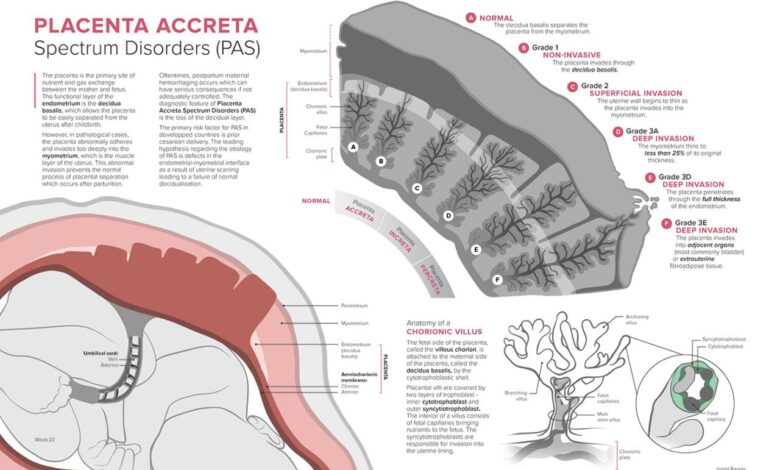
Placenta accreta is a serious pregnancy complication where the placenta implants too deeply into the uterine wall. Unlike a normal pregnancy, where the placenta attaches to the uterine lining but doesn’t penetrate it deeply, placenta accreta involves an abnormal invasion of the placental tissue into the myometrium (the muscular layer of the uterus). This can lead to significant bleeding during and after delivery, posing a serious threat to both the mother and the baby.
Placental Implantation and its Deviation in Placenta Accreta
In a normal pregnancy, the placenta implants in the upper part of the uterus, where the blood supply is rich and the uterine lining is thick enough to support the growing placenta without deep invasion. The placenta develops specialized cells that allow it to attach firmly but not penetrate the uterine muscle. However, in placenta accreta, this process goes awry.
The placental villi, which are finger-like projections that absorb nutrients, abnormally invade the myometrium. This abnormal invasion is the defining characteristic of placenta accreta and is the root cause of the associated complications. The depth of invasion varies, leading to different types of accreta.
Types of Placenta Accreta
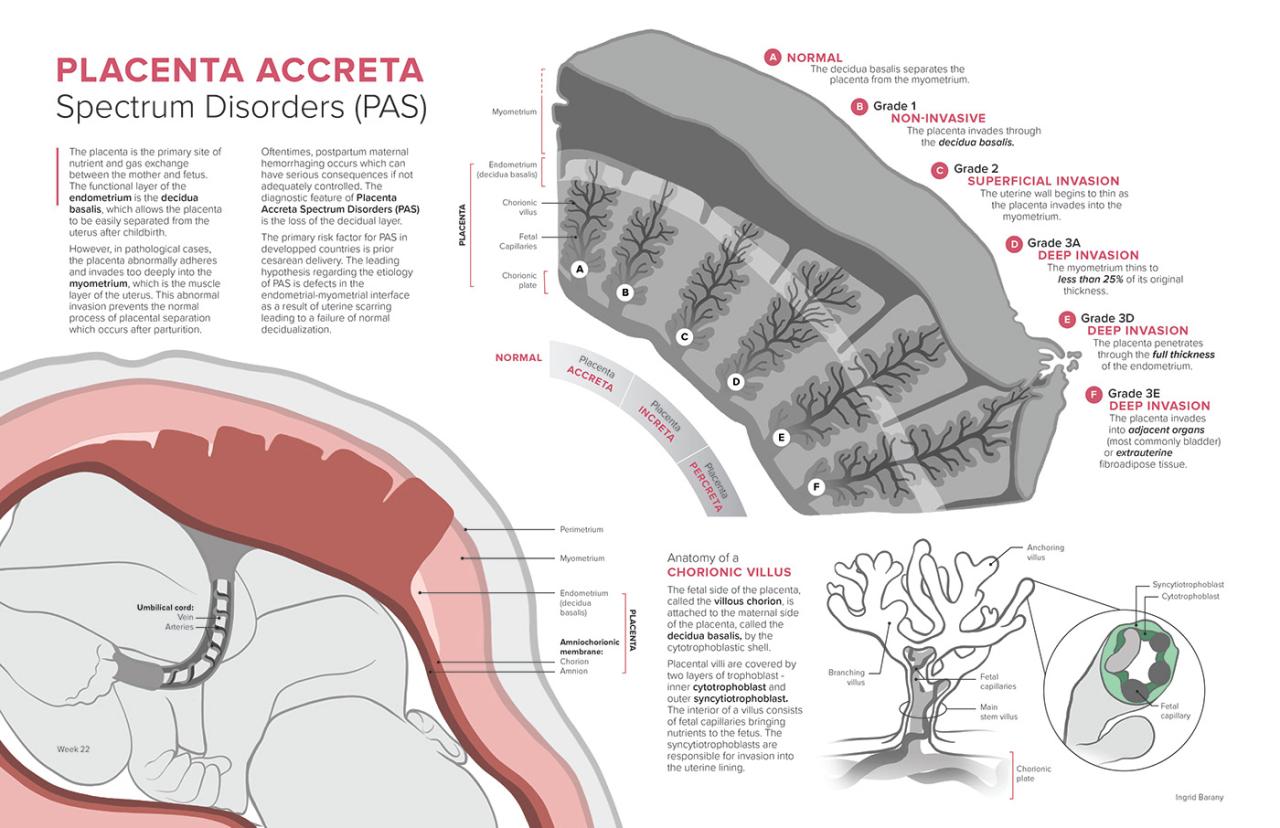
Placenta accreta is categorized based on the depth of placental invasion into the uterine wall. The three main types are accreta, increta, and percreta.
| Type | Placental Invasion | Risk Factors | Associated Complications |
|---|---|---|---|
| Accreta | Placenta attaches to the myometrium but doesn’t invade it. | Prior uterine surgery (e.g., C-section, myomectomy), placenta previa, uterine scarring, advanced maternal age. | Postpartum hemorrhage (PPH), uterine atony, hysterectomy. |
| Increta | Placenta invades the myometrium. | Same as accreta, plus previous uterine curettage. | More severe PPH than accreta, increased risk of hysterectomy, potential for uterine rupture. |
| Percreta | Placenta penetrates the entire uterine wall and may invade adjacent organs (bladder, bowel). | Same as increta, often associated with multiple prior pregnancies and surgeries. | Life-threatening PPH, extensive surgical intervention, potential for bowel or bladder injury, hysterectomy, and even death. |
Underlying Causes and Risk Factors
The exact cause of placenta accreta isn’t fully understood, but several factors significantly increase the risk. These include:* Previous Cesarean Sections: The most significant risk factor. Scar tissue from previous C-sections disrupts the normal uterine lining, providing an abnormal environment for placental implantation.
Placenta Previa When the placenta covers the cervix, it’s more likely to implant abnormally deep.
Prior Uterine Surgery Any previous uterine surgery, including myomectomy (removal of fibroids) or dilation and curettage (D&C), increases the risk.
Multiple Pregnancies Repeated pregnancies and deliveries can lead to scarring and thinning of the uterine wall.
Advanced Maternal Age Older mothers have a slightly increased risk.
Uterine Anomalies Congenital abnormalities of the uterus can also increase the risk.
Symptoms of Placenta Accreta

Source: com.au
Placenta accreta is a serious pregnancy complication where the placenta attaches too deeply into the uterine wall. Because the symptoms can be subtle and often mimic those of a normal pregnancy, early detection is crucial. The severity and presentation of symptoms can vary greatly depending on the type and extent of the accreta, and some women may experience no noticeable symptoms at all.
Regular prenatal care is therefore essential for early identification and management.
Symptom Presentation Across Trimesters
The symptoms of placenta accreta are not always readily apparent and can manifest differently depending on the severity and the stage of pregnancy. While some women may experience no symptoms, others might notice issues throughout the pregnancy. It’s important to remember that experiencing these symptoms doesn’t automatically mean you have placenta accreta; however, they warrant immediate medical attention.
- First Trimester: Symptoms are often absent in the first trimester. However, some women may experience unusually heavy bleeding during the early stages of pregnancy, which might be a subtle early sign, though this is not always the case.
- Second Trimester: As the placenta grows and embeds more deeply, some women may start experiencing painless vaginal bleeding, especially after a vaginal exam or sexual intercourse. This is a key indicator and requires immediate medical evaluation. The bleeding might be light spotting or heavier bleeding, varying greatly between individuals.
- Third Trimester: This is when symptoms are most likely to become noticeable. Painless vaginal bleeding is the most common sign. The bleeding can range from light spotting to heavy, life-threatening hemorrhage. Additionally, some women may experience an abnormally enlarged uterus, which can be detected during a routine ultrasound. In severe cases, the placenta may partially or completely detach prematurely, leading to potentially life-threatening complications for both the mother and the baby.
Variability in Symptom Severity and Type
The symptoms of placenta accreta can vary widely based on the type and severity of the condition. Placenta increta (where the placenta invades the myometrium) and placenta percreta (where the placenta penetrates the myometrium and potentially into adjacent organs) generally present with more severe symptoms than placenta accreta (where the placenta attaches deeply to the myometrium).For example, a woman with mild placenta accreta might only experience light bleeding during the third trimester, while a woman with placenta percreta might experience severe, life-threatening bleeding throughout the later stages of pregnancy.
The intensity of bleeding is not always directly correlated with the severity of the condition, however, emphasizing the need for vigilant monitoring and prompt medical intervention. In some cases, a woman might not experience any bleeding until labor or postpartum.
Asymptomatic Cases and the Importance of Routine Prenatal Care
It’s crucial to understand that some women with placenta accreta may not experience any symptoms throughout their pregnancy. This highlights the critical importance of routine prenatal care, including regular ultrasound examinations. Ultrasound scans are the primary diagnostic tool for identifying placenta accreta, allowing for early intervention and planning for safe delivery. A seemingly uncomplicated pregnancy can rapidly become critical if placenta accreta is undetected.
Regular monitoring allows healthcare providers to identify the condition and prepare a safe birthing plan, minimizing risks.
Diagnosis of Placenta Accreta: What Is Placenta Accreta Symptoms Types Diagnosis And Treatment
Diagnosing placenta accreta can be challenging, requiring a multi-modal approach combining several imaging techniques and clinical assessment. Early and accurate diagnosis is crucial for planning appropriate management and minimizing potential complications during delivery. The severity of accreta (i.e., accreta, increta, percreta) significantly impacts the management strategy, highlighting the importance of precise diagnostic imaging.
Ultrasound in the Diagnosis of Placenta Accreta
Transvaginal ultrasound (TVUS) is typically the first-line imaging modality used to screen for placenta accreta. Sonographers look for specific sonographic findings suggestive of abnormal placental implantation. These include the absence of a clear sonolucent retroplacental space (the space between the placenta and the uterine myometrium), an irregular placental margin, and increased placental vascularity. However, TVUS has limitations; it may not always accurately distinguish between different types of accreta or detect subtle cases.
The accuracy of TVUS is influenced by factors like operator experience and the quality of the ultrasound equipment. Three-dimensional (3D) ultrasound and color Doppler imaging can provide additional information but still aren’t foolproof. For instance, a lack of a retroplacental space isn’t always indicative of accreta, and other conditions can mimic the appearance of accreta on ultrasound.
MRI in Confirming the Diagnosis and Assessing Placental Invasion
Magnetic resonance imaging (MRI) is considered the gold standard for diagnosing and characterizing placenta accreta. MRI offers superior soft tissue contrast resolution compared to ultrasound, allowing for a more precise assessment of the extent of placental invasion into the myometrium and even into adjacent organs (in cases of percreta). Specific MRI sequences, such as T2-weighted images, are particularly useful in visualizing the placental interface and identifying the absence of the normal myometrial layer.
MRI can also help differentiate between different types of accreta, assess the involvement of adjacent structures like the bladder or rectum, and provide crucial information for surgical planning. However, MRI is more expensive and time-consuming than ultrasound, and it may not be readily available to all patients. Additionally, MRI requires patient cooperation and can be challenging in patients with claustrophobia or significant obesity.
Understanding placenta accreta, its symptoms, diagnosis, and treatment options is crucial for expectant mothers. The advancements in organ transplantation, like the recent fda approves clinical trials for pig kidney transplants in humans , highlight the incredible progress in medical science. This reminds us how vital ongoing research is across various medical fields, including the ongoing efforts to improve care and outcomes for conditions like placenta accreta.
Role of Doppler Ultrasound and Magnetic Resonance Angiography
Doppler ultrasound provides information about the placental blood flow. Abnormal vascular patterns, such as increased vascularity or the presence of abnormal vessels, can be suggestive of placenta accreta. However, Doppler ultrasound alone is not sufficient for definitive diagnosis. Magnetic resonance angiography (MRA) is a specialized MRI technique that can visualize the placental vasculature in detail. This can be particularly helpful in cases of suspected percreta, where the placenta invades adjacent organs and may involve their blood vessels.
MRA can help determine the extent of vascular involvement and guide surgical planning to minimize blood loss during intervention.
Diagnostic Flowchart for Suspected Placenta Accreta
The diagnostic process for suspected placenta accreta typically follows a stepwise approach:
1. Initial Screening Clinical suspicion arises based on risk factors (e.g., prior cesarean section, placenta previa).
2. Transvaginal Ultrasound (TVUS) Initial imaging assessment to identify potential sonographic features of accreta.
3. High-Risk Ultrasound Findings If suspicious findings are present on TVUS, further investigation is warranted.
4. MRI Confirmatory imaging to determine the type and extent of placental invasion.
5. Doppler Ultrasound/MRA (if indicated) To assess placental vascularity and plan for potential surgical intervention.
6. Diagnosis Confirmation Integration of clinical findings, ultrasound, and MRI results to confirm the diagnosis and determine the severity of accreta.
Treatment Options for Placenta Accreta
Placenta accreta, a serious pregnancy complication, requires careful consideration of various treatment approaches. The optimal strategy depends on several factors, including the severity of the condition, gestational age at diagnosis, maternal health, and the patient’s preferences. Treatment options range from expectant management to extensive surgical interventions, each carrying its own set of risks and benefits.
Expectant Management
Expectant management is rarely the preferred approach for placenta accreta, and is generally considered only in very specific circumstances. It might be considered in cases of very mild accreta detected late in pregnancy where the risks of immediate intervention outweigh the potential benefits. However, close monitoring is crucial, as expectant management carries a significant risk of postpartum hemorrhage (PPH).
This approach involves carefully observing the mother’s condition and preparing for potential complications during delivery.
Conservative Management
Conservative management involves interventions aimed at minimizing bleeding and improving maternal health before a definitive surgical procedure. This might include optimizing maternal blood volume and coagulation status, as well as administering medications to prepare for surgery. This is often a bridging strategy before more definitive surgical intervention.
Surgical Intervention
Surgical intervention is the most common treatment for placenta accreta, with the specific procedure depending on the severity of the condition and the patient’s overall health. The two main surgical techniques are hysterectomy and uterine artery embolization (UAE).
Hysterectomy
Hysterectomy, the surgical removal of the uterus, is often the preferred method for managing placenta accreta, particularly in cases of severe involvement. This is because it effectively addresses the source of bleeding by removing the affected uterus.
- Advantages: Generally effective in controlling hemorrhage, relatively straightforward procedure for experienced surgeons.
- Disadvantages: Permanent loss of fertility, potential for significant blood loss during surgery, increased risk of surgical complications (e.g., injury to surrounding organs).
Uterine Artery Embolization (UAE)
UAE is a less invasive procedure where small particles are injected into the uterine arteries to block blood flow to the placenta, reducing bleeding. It’s sometimes used as a pre-operative step to reduce blood loss during a subsequent hysterectomy or in cases where a hysterectomy is deemed too high-risk.
- Advantages: Less invasive than hysterectomy, preserves fertility (potentially), can reduce blood loss during surgery.
- Disadvantages: May not be effective in all cases, potential for incomplete embolization leading to persistent bleeding, risk of complications such as infection or damage to surrounding tissues.
Factors Influencing Treatment Choice
The choice of treatment for placenta accreta is a complex decision, carefully weighed against several factors. These include:
- Gestational age at diagnosis: Earlier diagnosis allows for better planning and potentially less invasive interventions.
- Severity of accreta: Mild accreta may allow for less invasive approaches, while severe cases often necessitate hysterectomy.
- Maternal health: Pre-existing medical conditions or overall health status can influence the choice of surgery and anesthesia.
- Patient preferences: The patient’s wishes regarding fertility preservation should be considered whenever possible.
Complications of Treatment and Management
Each treatment approach carries potential complications. Hysterectomy can lead to significant blood loss, infection, or damage to adjacent organs. UAE may result in incomplete embolization, requiring further intervention. Expectant management carries a high risk of postpartum hemorrhage. Careful monitoring and prompt management of complications are crucial in all cases.
Post-operative care often involves close monitoring of vital signs, blood loss, and potential infections. Blood transfusions and intensive care may be necessary to manage severe complications.
Illustrative Examples
Source: behance.net
Understanding placenta accreta is best achieved through examining real-world cases. The following examples showcase both a successful and a challenging management scenario, highlighting the variability in presentation and treatment. It’s crucial to remember that these are just examples, and individual cases can vary significantly.
Successful Placenta Accreta Management
A 32-year-old woman, gravida 3 para 2, presented at 36 weeks gestation with a suspected placenta accreta. Her previous pregnancies had been uncomplicated. A prior ultrasound at 20 weeks had shown a low-lying placenta, but no clear evidence of invasion. However, at 36 weeks, a repeat ultrasound revealed a placenta completely covering the internal cervical os, with sonographic evidence suggestive of placental invasion into the myometrium.
The ultrasound image showed a heterogeneous placental texture with areas of increased vascularity and absence of a clear hypoechoic myometrial layer between the placenta and the uterine wall. MRI confirmed the diagnosis of placenta accreta, showing the extent of myometrial invasion. A multidisciplinary team, including obstetricians, interventional radiologists, and hematologists, planned a conservative management approach. A planned cesarean delivery at 37 weeks was performed with immediate uterine artery embolization to minimize blood loss.
Understanding placenta accreta, a serious pregnancy complication involving the placenta’s deep attachment to the uterine wall, requires knowing its symptoms, types, diagnosis, and treatment options. It’s a stark contrast to the choices faced by women like Karishma Mehta, who, as detailed in this article karishma mehta gets her eggs frozen know risks associated with egg freezing , are proactively managing their reproductive health.
Returning to placenta accreta, early detection is key for successful management and minimizing risks to both mother and baby.
The patient received prophylactic blood transfusions. The procedure was successful, and the patient experienced minimal blood loss. Postpartum, she received close monitoring for potential complications, but recovered well without significant issues.
Challenging Placenta Accreta Case, What is placenta accreta symptoms types diagnosis and treatment
A 38-year-old woman, gravida 4 para 3, presented at 34 weeks gestation with a suspected placenta increta. She had a history of two prior cesarean sections. Ultrasound showed a placenta completely covering the internal cervical os, with evidence of invasion extending deep into the myometrium. The ultrasound image depicted a severely heterogeneous placental texture with numerous lacunae and extensive vascularity extending into the myometrium.
Understanding placenta accreta, its symptoms, diagnosis, and treatment is crucial for maternal health. Proper nutrition plays a vital role in pregnancy outcomes, and I found this article fascinating: are women and men receptive of different types of food and game changing superfoods for women. This highlights how diet impacts overall well-being, a factor that’s equally important when considering the complexities of managing a condition like placenta accreta.
MRI further confirmed the diagnosis of placenta increta, demonstrating significant myometrial invasion and involvement of the uterine serosa. The patient was considered high risk for significant hemorrhage. A multidisciplinary team decided on a planned cesarean hysterectomy at 36 weeks, given the extensive invasion and high risk of complications associated with conservative management. During the procedure, significant hemorrhage occurred, requiring massive blood transfusion.
Postoperative recovery was prolonged due to the significant blood loss and the need for intensive care. The patient experienced some short-term complications, including anemia and a prolonged hospital stay. However, she ultimately recovered fully.
Final Conclusion
Navigating the world of placenta accreta requires a multi-faceted approach, encompassing thorough understanding, early detection, and appropriate medical intervention. While the condition can present significant challenges, advancements in diagnostic imaging and surgical techniques offer improved outcomes for many affected individuals. Remember, regular prenatal care is paramount in identifying potential complications early on. This allows for proactive planning and the best possible management strategy, ensuring the well-being of both mother and child.
This post serves as a starting point for understanding this complex condition; always consult with your healthcare provider for personalized advice and care.
FAQ Overview
Can placenta accreta be prevented?
While there’s no guaranteed prevention, minimizing risk factors like previous uterine surgery (e.g., C-sections) and managing conditions like placenta previa can help reduce the likelihood.
What is the long-term outlook after placenta accreta treatment?
The long-term outlook varies depending on the severity of the condition and the chosen treatment. Many women experience full recovery, though some might have fertility challenges or require further procedures.
Is placenta accreta hereditary?
There’s no definitive evidence suggesting placenta accreta is directly inherited. However, certain risk factors like uterine scarring can be influenced by family history.
How common is placenta accreta?
The incidence of placenta accreta is increasing, likely due to factors like rising C-section rates. The exact prevalence varies, but it’s considered a relatively rare but significant complication.
