What is the Role of Continuous Glucose Monitors in Diabetes Management?
What is the role of continuous glucose monitor in diabetes management? It’s a question that’s revolutionizing how we approach this chronic condition. Imagine a world where you don’t have to constantly prick your finger, where your blood sugar levels are tracked 24/7, providing a detailed picture of your body’s response to food, exercise, and medication. That’s the power of continuous glucose monitoring (CGM), a technology that’s transforming diabetes care from reactive to proactive.
CGMs offer a wealth of benefits, from improved glycemic control and reduced hypoglycemic events to enhanced self-management and improved quality of life. This post delves into the mechanics of CGMs, their advantages and limitations, and how they’re shaping the future of diabetes management. We’ll explore the different types available, how they work, and how the data they provide empowers individuals to make informed decisions about their health.
Introduction to Continuous Glucose Monitors (CGMs): What Is The Role Of Continuous Glucose Monitor In Diabetes Management
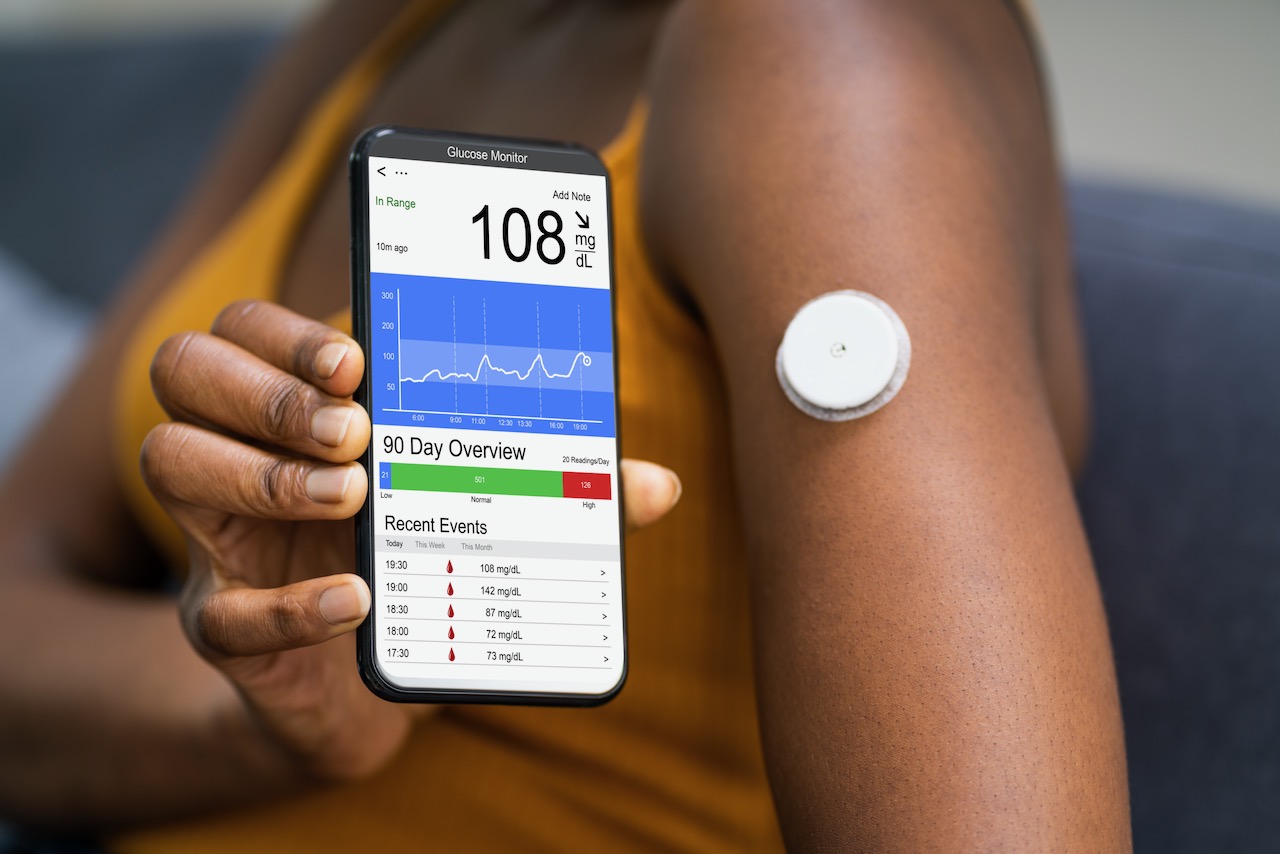
Continuous glucose monitoring (CGM) has revolutionized diabetes management, offering individuals with diabetes a more comprehensive understanding of their glucose levels throughout the day and night. Unlike traditional finger-stick blood glucose testing, which provides a snapshot in time, CGMs provide a continuous stream of glucose data, allowing for better detection of trends and patterns. This continuous data empowers individuals to make more informed decisions about their diabetes management, ultimately improving their overall health and well-being.CGMs function by using a small sensor inserted under the skin that measures glucose levels in the interstitial fluid.
This data is then transmitted wirelessly to a receiver, usually a handheld device or smartphone app, displaying glucose readings in real-time, along with historical data and predictive algorithms. This allows users to see how their glucose levels respond to food, exercise, and medication, enabling proactive adjustments to their treatment plan.
Types of Continuous Glucose Monitors
Several types of CGMs are available, each with its own set of features and benefits. The primary distinction lies in whether the system requires calibration with finger-stick blood glucose tests or is entirely sensor-based. Some CGMs provide alerts for high and low glucose levels, while others offer advanced features like predictive algorithms and integration with insulin pumps. The choice of CGM depends on individual needs, preferences, and healthcare provider recommendations.
CGM Technology: A Historical Overview, What is the role of continuous glucose monitor in diabetes management
The development of CGM technology has been a significant advancement in diabetes care. Early attempts at continuous glucose monitoring involved bulky and invasive technologies. However, over time, miniaturization and advancements in sensor technology have led to smaller, more comfortable, and user-friendly devices. The initial CGMs required frequent calibration with finger-stick tests, but newer generations of CGMs have largely eliminated this need, making them more convenient for daily use.
This evolution has made CGM technology accessible to a broader range of individuals with diabetes, significantly improving their ability to manage their condition effectively. The ongoing development of CGM technology continues to focus on improving accuracy, extending sensor lifespan, and integrating with other diabetes management tools.
How CGMs Work
Continuous glucose monitors (CGMs) are revolutionary devices for diabetes management, offering real-time glucose data and significantly improving glycemic control. Understanding how they function is key to harnessing their full potential. This section delves into the physiological principles, measurement techniques, data transmission, and visualization methods employed by CGMs.
Physiological Principles of CGM Function
CGMs work by measuring the interstitial fluid glucose concentration, which closely reflects blood glucose levels. Interstitial fluid is the fluid surrounding cells in the body’s tissues. A small sensor, inserted just beneath the skin, uses electrochemical methods to detect changes in glucose concentration within this fluid. The sensor’s performance relies on the constant exchange between interstitial fluid and blood glucose, ensuring a relatively accurate representation of blood sugar levels.
It’s important to note that there’s a slight delay between blood glucose changes and the reflection in interstitial fluid glucose, typically around 5-10 minutes.
Glucose Measurement by CGM Sensors
CGMs primarily employ electrochemical sensors. These sensors contain a glucose oxidase enzyme that reacts with glucose in the interstitial fluid. This reaction generates an electrical current, the magnitude of which is directly proportional to the glucose concentration. The sensor then translates this electrical signal into a glucose reading, which is transmitted wirelessly to a receiver or smartphone. Different CGM systems may utilize slightly varying electrochemical techniques and sensor designs, but the underlying principle remains the same.
Data Transmission and Display
The measured glucose data is transmitted wirelessly from the sensor to a receiver or smartphone app via Bluetooth or other wireless protocols. This allows for continuous monitoring and immediate access to glucose information. The receiver or app displays the current glucose level, usually in mg/dL or mmol/L, along with a trend arrow indicating whether glucose is rising, falling, or stable.
Some CGMs also provide historical glucose data, allowing users to track patterns and trends over time.
CGM Data Visualization Methods
CGMs offer various ways to visualize glucose data, enhancing user understanding and management. These visualizations go beyond simple numerical readings, providing insights into glucose patterns and trends. Different manufacturers employ different visualization approaches.
| Feature | System A | System B | System C | System D |
|---|---|---|---|---|
| Glucose Value Display | Numerical value with trend arrow (↑, ↓, →) | Numerical value with color-coded background (green, yellow, red) | Numerical value and graphical representation of glucose level over time | Numerical value, trend arrow, and predictive algorithm for future glucose levels |
| Trend Visualization | Simple arrow indicating direction of glucose change | Color-coded graph showing glucose changes over the last few hours | Detailed graph with customizable timeframes | Graph showing predicted glucose levels based on current trend |
| Historical Data View | Daily and weekly glucose averages | Detailed graphs showing glucose levels over customizable periods | Ability to export data for sharing with healthcare providers | Detailed reports including time in range and other metrics |
| Alerts and Notifications | Alerts for high and low glucose levels | Customizable alerts based on user-defined thresholds | Notifications for rapid glucose changes | Predictive alerts based on the system’s algorithm |
CGMs and Blood Glucose Control
Continuous glucose monitors (CGMs) have revolutionized diabetes management, offering a wealth of data that significantly impacts blood glucose control and overall health. By providing real-time glucose readings, CGMs empower individuals with diabetes to make informed decisions about their treatment and lifestyle choices, leading to improved outcomes. This section will explore the benefits and limitations of CGMs in achieving better glycemic control.
Improved Glycemic Control with CGMs
CGMs offer several advantages in achieving better blood glucose control. The constant stream of glucose data allows for proactive adjustments to insulin therapy, preventing both high and low blood sugar levels. For example, a person using an insulin pump can adjust their basal insulin rate based on the CGM trends, preventing hyperglycemia. Similarly, someone experiencing a gradual increase in glucose levels can take preventative measures, like increasing physical activity or adjusting their meal plan, before the levels become dangerously high.
Managing diabetes effectively relies heavily on monitoring blood sugar levels, and a continuous glucose monitor (CGM) is a game-changer. It provides real-time data, helping individuals make informed decisions about insulin doses and lifestyle choices. Thinking about long-term health, it’s interesting to see how other health decisions impact our lives, like Karishma Mehta’s choice to freeze her eggs, as detailed in this article: karishma mehta gets her eggs frozen know risks associated with egg freezing.
Just like proactive egg freezing, using a CGM is all about taking control of your health journey and planning for the future.
This proactive approach contrasts sharply with the reactive nature of traditional finger-stick testing, which only provides a snapshot of glucose at a specific moment. The continuous data provided by CGMs enables a more nuanced understanding of individual glucose patterns, including responses to meals, exercise, and stress. This granular data allows for personalized adjustments to therapy, maximizing effectiveness and minimizing complications.
Reduction of Hypoglycemic Events with CGM Use
Hypoglycemia, or low blood sugar, is a serious complication of diabetes that can lead to severe consequences, including loss of consciousness and seizures. CGMs play a crucial role in reducing the frequency and severity of hypoglycemic events. The continuous monitoring allows individuals to identify and address low glucose levels promptly, before they become dangerous. Many CGMs offer alerts that notify the user when glucose levels fall below a pre-set threshold, providing ample time to intervene with glucose-raising strategies, such as consuming carbohydrates or adjusting insulin dosage.
This early warning system is especially beneficial for individuals with recurrent hypoglycemia or those who may be less aware of the symptoms of low blood sugar. Studies have consistently demonstrated a significant reduction in hypoglycemic events in individuals using CGMs compared to those relying solely on self-monitoring of blood glucose (SMBG).
Limitations of CGM Technology
While CGMs offer substantial benefits, it’s important to acknowledge their limitations. One common limitation is the potential for inaccurate readings. Factors such as sensor placement, scarring, and dehydration can affect the accuracy of the glucose data. Calibration with finger-stick blood glucose measurements is often required, adding another step to the monitoring process. Furthermore, CGMs are not perfect predictors of future glucose levels, and reliance solely on CGM data without considering other factors, such as food intake and physical activity, can lead to suboptimal glucose management.
The cost of CGMs and the associated supplies can also be a barrier for some individuals, although insurance coverage is becoming increasingly common. Finally, some individuals may experience skin irritation or allergic reactions to the sensor.
CGM vs. Traditional Blood Glucose Monitoring
Let’s compare and contrast the advantages and disadvantages of CGMs and traditional blood glucose monitoring (SMBG) methods using finger-stick testing:
The choice between CGM and SMBG depends on individual needs and preferences, along with factors such as cost and insurance coverage. While SMBG remains a vital component of diabetes management, particularly for calibration purposes, CGMs provide a more comprehensive and proactive approach to glucose control.
| Feature | CGM | SMBG |
|---|---|---|
| Frequency of Monitoring | Continuous | Intermittent (typically 4-7 times daily) |
| Data Provided | Real-time glucose levels, trends, and alerts | Single glucose reading at a specific time |
| Predictive Capabilities | Provides trend information, but not perfect prediction | No predictive capabilities |
| Convenience | More convenient for frequent monitoring | Requires finger-pricks, which can be painful and inconvenient |
| Cost | Generally more expensive | Relatively inexpensive |
CGMs and Diabetes Management Strategies
Continuous glucose monitors (CGMs) have revolutionized diabetes management, moving beyond simple blood glucose readings to provide a dynamic picture of glucose levels throughout the day and night. This wealth of data empowers individuals with diabetes and their healthcare providers to make more informed decisions, leading to better control and improved quality of life. The integration of CGM data into personalized management plans is key to achieving optimal outcomes.
Personalized Diabetes Management Plans
CGMs provide a highly individualized approach to diabetes management. Unlike traditional methods relying on infrequent finger-stick blood glucose tests, CGMs offer a continuous stream of data, revealing patterns and trends that would otherwise be missed. This detailed information allows for the creation of a personalized plan tailored to an individual’s unique metabolic responses, activity levels, and dietary habits. For example, a CGM might reveal a specific food triggers a significant glucose spike in one person, while another individual might experience minimal impact.
This allows for adjustments to meal planning and portion sizes, ultimately leading to better blood sugar control. The data also helps identify individual responses to various types of exercise, enabling the development of a customized exercise plan that optimizes glucose control without risking hypoglycemia.
Adjusting Insulin Dosages
For individuals using insulin therapy, CGMs play a crucial role in optimizing insulin dosing. By continuously monitoring glucose levels, individuals can see the immediate impact of insulin injections or boluses. This real-time feedback allows for precise adjustments to insulin dosages, minimizing the risk of both hyperglycemia (high blood sugar) and hypoglycemia (low blood sugar). For example, if a CGM shows a rapid rise in glucose after a meal, a smaller insulin bolus might be sufficient in the future.
Conversely, if glucose levels drop unexpectedly, the individual can take corrective action to prevent a hypoglycemic event. This close monitoring significantly reduces the risk of severe glucose fluctuations and their associated complications.
CGMs are game-changers for diabetes management, providing real-time glucose data to help prevent dangerous highs and lows. However, consistently high blood sugar is a major risk factor for many health complications, including stroke; understanding the risk factors that make stroke more dangerous is crucial. By proactively managing glucose levels with a CGM, individuals with diabetes can significantly reduce their stroke risk and improve their overall health.
Informing Lifestyle Choices
CGM data extends beyond insulin management to provide valuable insights into the impact of lifestyle choices on blood glucose levels. By analyzing the relationship between glucose readings and diet, individuals can identify specific foods or eating patterns that lead to undesirable glucose fluctuations. This information empowers individuals to make informed dietary adjustments, such as reducing carbohydrate intake, choosing lower glycemic index foods, or altering meal timing.
Similarly, CGM data can help individuals understand how different types and intensities of exercise affect their glucose levels, enabling them to develop a personalized exercise regimen that optimizes glucose control and overall health. Tracking trends over time also helps identify patterns related to sleep, stress, and illness, allowing for proactive management strategies.
Integration with Other Diabetes Management Technologies
CGMs seamlessly integrate with other diabetes technologies, creating a comprehensive and interconnected system for managing diabetes. This integration simplifies the management process and enhances the accuracy and effectiveness of treatment.
| Technology | Integration Method | Benefits | Example |
|---|---|---|---|
| Insulin Pumps | Wireless data transfer via Bluetooth or similar technology | Automated insulin delivery based on CGM readings (closed-loop systems); improved precision and reduced risk of hypoglycemia. | Many insulin pump manufacturers offer direct integration with specific CGM models, allowing for automated insulin delivery based on real-time glucose data. |
| Smartphone Apps | Data synchronization via mobile app; data visualization and analysis tools. | Enhanced data tracking, remote monitoring by healthcare providers, personalized reports and insights. | Many CGM manufacturers provide dedicated smartphone apps that allow users to view their glucose data, set alarms, and generate reports. |
| Cloud-Based Data Platforms | Data upload and storage for remote access and analysis. | Data sharing with healthcare providers, remote monitoring, trend analysis, and data-driven insights. | Some CGMs allow users to upload their data to cloud-based platforms, allowing for easy sharing with doctors and diabetes educators. |
| Diabetes Management Software | Data import and analysis; generation of personalized reports and insights. | Detailed analysis of CGM data, identification of trends and patterns, personalized recommendations for improving glucose control. | Specialized software programs can analyze CGM data alongside other health metrics to provide comprehensive insights and personalized recommendations. |
CGMs and Patient Outcomes
Continuous glucose monitors (CGMs) have revolutionized diabetes management, profoundly impacting not only blood glucose control but also the overall quality of life for individuals living with diabetes. The constant stream of glucose data empowers patients to make informed decisions, fostering a sense of control and reducing the daily anxieties often associated with managing this chronic condition.CGMs significantly improve patient well-being by providing a more holistic view of glucose fluctuations, enabling proactive adjustments to diet, exercise, and medication.
This proactive approach minimizes the risk of both hypoglycemic and hyperglycemic events, leading to improved health outcomes and a greater sense of security. This translates to a better quality of life, allowing individuals to participate more fully in daily activities and social interactions without the constant worry about their blood sugar levels.
Reduced Anxiety and Improved Confidence in Self-Management
The constant monitoring provided by a CGM significantly reduces the anxiety associated with unpredictable blood sugar swings. Imagine the relief of knowing your glucose levels at any given moment, without the need for finger-prick testing every few hours. This constant access to information empowers patients to take control of their diabetes management, fostering a sense of confidence and self-efficacy.
For example, a patient might adjust their insulin dose based on a CGM alert showing a rapid rise in glucose, preventing a potentially dangerous hyperglycemic episode. This proactive approach, enabled by the CGM, replaces reactive management with a more confident, proactive approach to their health. This increased confidence extends to other aspects of life, allowing individuals to feel more secure in their social and professional activities.
CGMs revolutionize diabetes management by providing real-time glucose data, empowering users to make informed dietary choices. Understanding how these choices impact blood sugar is crucial, and that’s where the question of nutritional needs comes in – check out this interesting article on how different genders might respond to food, are women and men receptive of different types of food and game changing superfoods for women , to better tailor your approach.
Ultimately, using a CGM and understanding your body’s response to food is key to effective diabetes management.
Long-Term Effects on Diabetes Complications
Studies have shown a strong correlation between consistent CGM use and a reduction in the risk of long-term diabetes complications. By providing early warnings of both hyperglycemia and hypoglycemia, CGMs allow for timely interventions, minimizing the damage caused by prolonged periods of high or low blood sugar. This preventative approach is crucial in reducing the risk of retinopathy, nephropathy, neuropathy, and cardiovascular disease, all serious complications associated with poorly managed diabetes.
While not a guaranteed prevention, the consistent data provided by CGMs empowers individuals and healthcare providers to make more informed decisions, ultimately leading to better long-term health outcomes. For instance, a patient consistently using a CGM might notice a gradual increase in their average glucose levels over several weeks, prompting a discussion with their doctor about medication adjustments or lifestyle changes before serious complications arise.
A Day in the Life with a CGM
Imagine Sarah, a 35-year-old woman with type 1 diabetes. Before her CGM, her days were filled with anxiety. Every meal was a gamble, every activity a potential blood sugar rollercoaster. She constantly worried about hypoglycemia, carrying glucose tablets everywhere she went. Now, with her CGM, Sarah feels a sense of liberation.
She wakes up, checks her glucose level on her CGM display, and adjusts her insulin dose accordingly. Throughout the day, she receives alerts if her glucose is rising or falling too quickly, giving her time to make adjustments and prevent extreme highs or lows. During a lunchtime meeting, a subtle vibration from her CGM alerts her to a slightly elevated glucose.
She discreetly checks her readings, then chooses a smaller portion of dessert and takes a short walk, confidently managing her levels without interrupting the meeting. In the evening, she can enjoy a relaxed dinner with friends, knowing her CGM will alert her to any potential problems. This constant monitoring removes the constant fear and allows her to live a more spontaneous and fulfilling life, free from the constant worry of her diabetes.
The peace of mind provided by the CGM has significantly improved her quality of life, enabling her to focus on work, relationships, and hobbies without the constant shadow of diabetes.
Future Directions in CGM Technology
Source: stanford.edu
The field of continuous glucose monitoring (CGM) is rapidly evolving, driven by ongoing research and technological advancements. Current limitations, such as sensor lifespan and accuracy, are being actively addressed, paving the way for even more sophisticated and user-friendly devices that will revolutionize diabetes management. This section explores the exciting possibilities on the horizon for CGM technology.
Improved Accuracy and Sensor Longevity
Researchers are constantly working to enhance the accuracy and longevity of CGM sensors. Current efforts focus on improving the sensor’s ability to accurately measure glucose levels in various physiological conditions, such as during exercise or after meals. This involves developing more sophisticated algorithms and incorporating advanced materials that minimize interference from other substances in interstitial fluid. For example, some research explores the use of novel biosensors that are less prone to drift and provide more stable readings over longer periods.
Simultaneously, the development of longer-lasting sensors is a major goal. Current sensors typically last for a week or two; however, the development of sensors that can last for several weeks or even months would significantly improve patient convenience and reduce the burden of frequent sensor changes. This could involve using more durable materials and designing sensors that are less susceptible to degradation over time.
Non-Invasive CGM Technologies
The current gold standard for CGM involves a small sensor inserted under the skin. However, the development of non-invasive methods for continuous glucose monitoring represents a significant advancement. Several approaches are being explored, including optical sensors that measure glucose levels through the skin using near-infrared light, and electrochemical sensors that detect glucose in sweat. These technologies, if successful, would eliminate the need for needles and injections, making CGM more accessible and less invasive for patients.
For instance, imagine a small, wearable patch that seamlessly integrates into clothing and continuously monitors glucose levels without any painful insertion procedures. This could significantly increase CGM adoption rates, particularly among individuals hesitant to use invasive technologies.
Advanced Data Integration and Personalized Diabetes Management
The future of CGM involves more than just accurate glucose readings; it’s about seamlessly integrating that data into a comprehensive diabetes management system. This includes connecting CGMs with insulin pumps, smartphone apps, and other healthcare devices to create a closed-loop system that automatically adjusts insulin delivery based on real-time glucose levels. This automated approach could significantly reduce the burden of manual insulin adjustments and improve glycemic control.
Moreover, advanced data analytics can be used to personalize diabetes management strategies based on individual patient data. This involves using machine learning algorithms to identify patterns in glucose data and predict future glucose levels, allowing for proactive interventions and personalized treatment plans. For example, a system could analyze a patient’s glucose data to predict the likelihood of hypoglycemia during exercise and provide personalized recommendations to prevent it.
Predictive Capabilities and Early Warning Systems
Future CGMs are likely to incorporate sophisticated predictive capabilities. By analyzing glucose trends and patterns, these devices could predict future glucose levels and alert patients to potential hypoglycemic or hyperglycemic events before they occur. This could provide patients with valuable time to take preventative measures, such as adjusting their insulin dose or consuming a carbohydrate snack. This predictive capability would be particularly beneficial for individuals with type 1 diabetes who are at higher risk of severe hypoglycemia.
Imagine a CGM that provides a clear, proactive warning several hours in advance of a predicted hypoglycemic event, enabling individuals to take preventative measures and avoid dangerous situations. This represents a significant improvement over current systems that primarily focus on reactive monitoring.
Outcome Summary
Source: ssl-images-amazon.com
Living with diabetes doesn’t have to mean living with constant worry. Continuous glucose monitors are proving to be a game-changer, offering a level of control and insight that was previously unimaginable. While not a perfect solution, the benefits of CGMs in improving glycemic control, reducing hypoglycemic events, and enhancing quality of life are undeniable. As technology continues to advance, the future of CGM looks incredibly bright, promising even greater accuracy, convenience, and integration with other diabetes management tools.
If you’re living with diabetes, talking to your doctor about whether a CGM is right for you is a conversation worth having.
Key Questions Answered
What are the potential side effects of using a CGM?
Some users experience minor skin irritation at the sensor insertion site. Rarely, more serious complications can occur, so it’s important to follow your doctor’s instructions and report any concerns.
How much does a CGM cost?
The cost varies depending on the type of CGM and your insurance coverage. Many insurance plans cover at least part of the cost, but it’s essential to check with your provider.
How often do I need to change the CGM sensor?
Sensor lifespan varies depending on the brand and model, typically ranging from 7 to 14 days. You’ll need to replace the sensor according to the manufacturer’s instructions.
Can I use a CGM if I’m not on insulin?
Yes, CGMs can benefit individuals with diabetes who are not on insulin by providing valuable insights into their blood sugar patterns and helping them manage their condition through diet and exercise.
