When to Test for Inflammation and Types of Tests Available
When to test for inflammation and types of test available – When to test for inflammation and types of tests available is a crucial question for anyone experiencing persistent aches, pains, or unusual fatigue. Inflammation, a complex bodily response to injury or infection, can manifest in subtle or dramatic ways. Understanding when to seek medical attention and what tests can pinpoint the source of your inflammation is key to effective treatment.
This post will explore common symptoms, diagnostic methods, and help you navigate the process of getting the answers you need. We’ll delve into the different types of tests, from simple blood work to advanced imaging, so you can better understand what to expect and what questions to ask your doctor.
We’ll cover everything from recognizing the signs of acute versus chronic inflammation to interpreting test results and exploring the various treatment options available. This isn’t just about medical jargon; it’s about empowering you to take control of your health. Whether you’re dealing with a nagging joint pain or a more serious condition, knowing when and how to test for inflammation can make all the difference.
Recognizing Symptoms of Inflammation: When To Test For Inflammation And Types Of Test Available
Inflammation is your body’s natural response to injury or infection, a complex process designed to protect and repair damaged tissues. Understanding the signs and symptoms of inflammation, both acute and chronic, is crucial for early diagnosis and appropriate management of various health conditions. While some symptoms are readily apparent, others can be subtle and easily overlooked, highlighting the importance of paying close attention to your body’s signals.Recognizing the symptoms of inflammation involves understanding the body’s typical reaction to injury or infection.
This reaction can manifest in different ways depending on the severity and duration of the inflammation, broadly categorized as acute or chronic. Acute inflammation is typically short-lived, lasting from a few days to a few weeks, while chronic inflammation persists for extended periods, sometimes even years.
Common Symptoms of Acute and Chronic Inflammation
Acute inflammation often presents with readily identifiable symptoms. These include pain, swelling, redness, heat, and loss of function in the affected area. Think of a sprained ankle – the swelling, redness, and pain are classic signs of acute inflammation. In contrast, chronic inflammation may present with less obvious symptoms. Fatigue, low-grade fever, persistent aches and pains, digestive issues, and skin problems can all be indicative of underlying chronic inflammation.
The subtlety of chronic inflammation makes early detection challenging, emphasizing the need for regular health check-ups and awareness of even seemingly minor persistent symptoms.
Examples of Inflammatory Conditions and Their Associated Symptoms
It’s helpful to see how different inflammatory conditions manifest. The following table provides examples, though it’s not exhaustive and symptom severity varies greatly between individuals. Always consult a healthcare professional for diagnosis and treatment.
| Condition | Acute Symptoms | Chronic Symptoms | Potential Causes |
|---|---|---|---|
| Appendicitis | Sudden, severe abdominal pain, nausea, vomiting, fever | Not applicable; typically resolved or treated acutely | Infection or blockage of the appendix |
| Asthma | Wheezing, coughing, shortness of breath, chest tightness | Persistent cough, wheezing, shortness of breath, frequent exacerbations | Allergens, irritants, genetic predisposition |
| Rheumatoid Arthritis | Joint pain, swelling, stiffness, redness, fever | Persistent joint pain, stiffness, swelling, deformity, fatigue, low-grade fever | Autoimmune response, genetic factors, environmental triggers |
| Psoriasis | Red, scaly patches on the skin, itching | Persistent scaly patches, itching, joint pain (psoriatic arthritis), fatigue | Autoimmune response, genetic factors, environmental triggers |
The Importance of Recognizing Subtle Symptoms
Many chronic inflammatory conditions initially present with subtle, often overlooked symptoms. These might include persistent fatigue, unexplained weight loss or gain, digestive problems like bloating or diarrhea, persistent headaches or migraines, and skin conditions like eczema or rashes. Dismissing these as minor inconveniences can delay diagnosis and treatment, potentially leading to more severe complications down the line. If you experience persistent symptoms, even if they seem insignificant, it’s crucial to seek medical attention to rule out underlying inflammatory conditions.
Early detection and intervention are key to managing inflammatory diseases effectively.
When to Seek Medical Attention for Inflammation
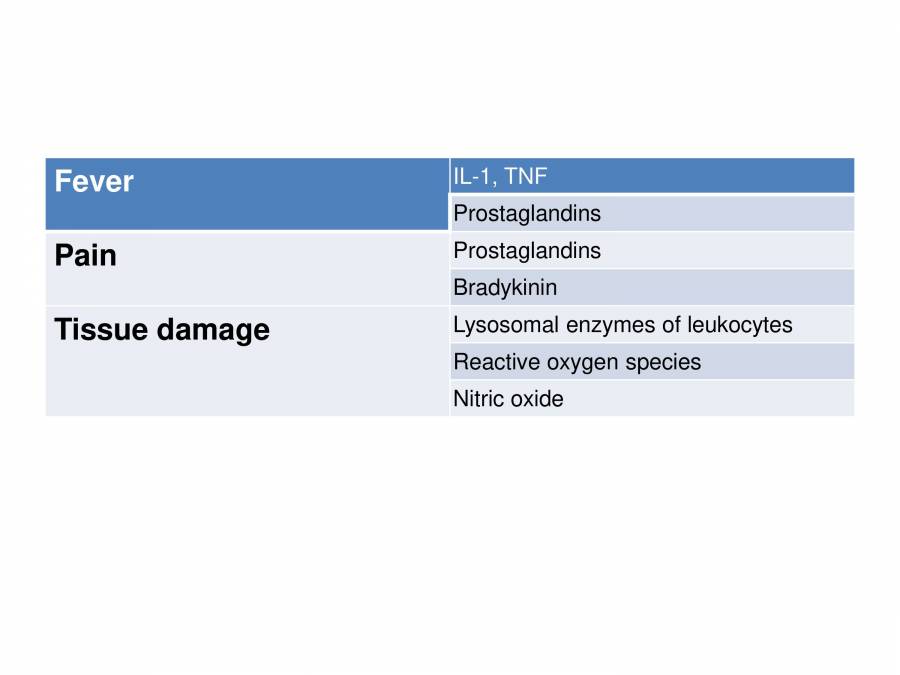
Source: learnpick.in
Inflammation is a natural bodily response to injury or infection, but persistent or severe inflammation can signal a serious underlying condition. Knowing when to seek medical attention is crucial for effective management and preventing potential complications. This section Artikels scenarios requiring immediate medical care and emphasizes the importance of persistent symptoms as indicators needing professional assessment.
While many inflammatory conditions resolve on their own with simple home remedies, some require prompt medical intervention. Delaying treatment can lead to worsening symptoms, irreversible damage, or even life-threatening complications. Therefore, understanding the signs that necessitate a doctor’s visit is paramount for maintaining good health.
Severe or Rapidly Worsening Symptoms
Severe inflammatory symptoms warrant immediate medical attention. This includes sudden, intense pain, high fever (over 101°F or 38.3°C), difficulty breathing, swelling that restricts movement or blood flow, and significant changes in mental state such as confusion or disorientation. For example, someone experiencing sudden, severe abdominal pain accompanied by high fever could be suffering from appendicitis or a similar serious condition requiring immediate surgery.
Similarly, rapidly spreading skin inflammation accompanied by blisters and fever might indicate a severe infection requiring aggressive antibiotic treatment. Ignoring these signs could have severe consequences.
Persistent or Worsening Symptoms Despite Treatment
If inflammatory symptoms persist for an extended period (longer than a week or two, depending on the condition) or worsen despite home treatment or over-the-counter medications, medical attention is necessary. This could indicate a chronic inflammatory condition or an underlying disease requiring specialized treatment. For instance, persistent joint pain and swelling unresponsive to over-the-counter pain relievers could suggest rheumatoid arthritis, which requires a rheumatologist’s assessment and ongoing management.
Similarly, persistent cough and shortness of breath despite using cough suppressants might indicate a chronic lung condition like asthma or bronchitis that needs professional evaluation and a tailored treatment plan.
Decision-Making Flowchart for Seeking Medical Attention
The following flowchart helps determine when to consult a doctor regarding inflammatory symptoms:
Start –> Are symptoms severe (high fever, difficulty breathing, severe pain)? –> Yes –> Seek immediate medical attention –> End
No –> Have symptoms persisted for more than a week or two, or worsened despite treatment? –> Yes –> Schedule an appointment with a doctor –> End
No –> Monitor symptoms and consider home remedies –> End
Types of Inflammation Tests
Inflammation, while a crucial part of our body’s defense system, can become problematic when it persists or becomes excessive. Diagnosing the type and severity of inflammation requires a range of tests, with blood tests playing a particularly significant role. These tests help doctors assess the overall inflammatory response and guide treatment decisions.
Complete Blood Count (CBC) in Inflammation Assessment
A complete blood count (CBC) is a fundamental blood test that provides a comprehensive overview of your blood’s components, including red blood cells, white blood cells, and platelets. While not a direct measure of inflammation, a CBC can offer valuable clues. Elevated white blood cell counts (leukocytosis), particularly neutrophils, often indicate an active inflammatory process, suggesting the body is fighting off an infection or dealing with tissue damage.
Changes in other blood cell parameters might also indirectly suggest inflammation, though interpretation requires clinical context and consideration of other symptoms. For example, anemia (low red blood cell count) can sometimes accompany chronic inflammatory conditions.
C-Reactive Protein (CRP) and Erythrocyte Sedimentation Rate (ESR) Tests
C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) are two common blood tests specifically designed to detect inflammation. CRP is a protein produced by the liver in response to inflammation. High CRP levels generally indicate ongoing inflammation, with levels rising significantly during acute infections or inflammatory diseases. ESR measures how quickly red blood cells settle at the bottom of a test tube.
A higher ESR rate usually indicates increased inflammation, as inflammatory proteins cause red blood cells to clump together and settle faster. Both CRP and ESR are nonspecific markers; meaning elevated levels can indicate various conditions, not just inflammation. Therefore, these tests are best used in conjunction with other diagnostic tools and clinical evaluation. Interpreting results requires considering factors like age, sex, and underlying health conditions.
For example, a slightly elevated CRP might be normal for an older individual, while a significantly elevated level in a younger person warrants further investigation.
Comparison of Blood Tests for Inflammation
Several blood tests help identify inflammation, each with its strengths and limitations. Understanding these differences is crucial for accurate diagnosis.
- Complete Blood Count (CBC): Provides a broad overview of blood components; indirectly suggests inflammation through changes in white blood cell counts and other parameters. Strengths: widely available, inexpensive, comprehensive blood picture. Limitations: nonspecific for inflammation; only indirectly indicates inflammatory processes.
- C-Reactive Protein (CRP): Directly measures a protein produced in response to inflammation. Strengths: sensitive to acute inflammation; can detect subtle changes. Limitations: nonspecific; can be elevated in various conditions besides inflammation; can be influenced by factors like infection or pregnancy.
- Erythrocyte Sedimentation Rate (ESR): Measures the rate at which red blood cells settle; reflects increased inflammation. Strengths: simple, inexpensive test; useful for monitoring inflammatory diseases. Limitations: nonspecific; less sensitive than CRP; influenced by factors like age, anemia, and pregnancy.
Types of Inflammation Tests
Source: activeatoms.com
Inflammation, while a crucial part of our body’s defense mechanism, can become problematic when chronic or severe. Diagnosing the underlying cause often requires more than just a physical exam and blood work. Imaging tests play a vital role in visualizing the affected areas and assessing the extent of inflammation, providing clinicians with a clearer picture of the condition.
These tests offer different advantages and are selected based on the suspected location and type of inflammation.
Imaging Tests for Detecting Inflammation
Several imaging techniques are invaluable in detecting and characterizing inflammation. Each method utilizes different principles and provides unique information about the inflamed tissue. The choice of imaging modality depends on factors like the location of suspected inflammation, the type of tissue involved, and the clinical question being addressed.
X-rays in Inflammation Detection
X-rays primarily reveal differences in tissue density. While not directly visualizing inflammation itself, they can indirectly indicate its presence. For instance, in cases of pneumonia (lung inflammation), an X-ray might show areas of consolidation (increased density) indicating fluid buildup in the lungs. Similarly, in osteoarthritis, X-rays can reveal joint space narrowing and bone spurs, indirect signs of chronic inflammation.
X-rays are relatively inexpensive and readily available, making them a first-line imaging option in many situations. However, their limited ability to visualize soft tissues restricts their use in detecting inflammation in organs like the liver or spleen.
Ultrasound in Inflammation Detection
Ultrasound uses high-frequency sound waves to create images of internal structures. In inflammation, ultrasound can detect changes in tissue texture, swelling, and fluid collections. It’s particularly useful for evaluating inflammation in superficial structures like tendons, muscles, and joints. For example, ultrasound can easily visualize tenosynovitis (inflammation of the tendon sheath), showing fluid accumulation around the tendon. Ultrasound is non-invasive, relatively inexpensive, and readily portable, making it suitable for bedside evaluations.
However, its image quality can be affected by overlying bone or air, limiting its use in certain areas.
MRI in Inflammation Detection, When to test for inflammation and types of test available
Magnetic Resonance Imaging (MRI) uses a powerful magnetic field and radio waves to create detailed images of soft tissues. MRI is exceptionally sensitive in detecting inflammation, revealing changes in tissue composition and fluid content. It’s particularly valuable for assessing inflammation in the brain, spinal cord, joints, and internal organs. For example, MRI can clearly show the extent of inflammation in multiple sclerosis, a disease affecting the brain and spinal cord.
While MRI provides exquisite detail, it’s more expensive and time-consuming than other imaging techniques, and the presence of certain metallic implants can preclude its use.
CT Scans in Inflammation Detection
Computed Tomography (CT) scans use X-rays to create cross-sectional images of the body. While not as sensitive as MRI for detecting subtle inflammation, CT scans are better at visualizing bone and calcifications. They are frequently used to assess inflammation in the abdomen and pelvis, where they can detect abscesses (collections of pus) or inflammatory changes in organs like the intestines or appendix.
CT scans are faster than MRI and provide good anatomical detail, but they involve higher radiation exposure compared to ultrasound or MRI.
Comparison of Imaging Techniques
| Imaging Technique | Cost | Invasiveness | Types of Inflammation Detectable |
|---|---|---|---|
| X-ray | Low | Non-invasive | Indirect signs in bone and lung; limited soft tissue visualization |
| Ultrasound | Moderate | Non-invasive | Superficial soft tissue inflammation (tendons, muscles, joints) |
| MRI | High | Non-invasive | Wide range of inflammation, particularly in soft tissues (brain, spinal cord, joints, organs) |
| CT Scan | Moderate to High | Non-invasive | Inflammation in abdomen and pelvis, bone and calcifications; less sensitive for soft tissue inflammation than MRI |
Types of Inflammation Tests
Beyond the common blood tests and imaging techniques, several other diagnostic methods play a crucial role in pinpointing the cause and extent of inflammation. These advanced tests offer a more detailed picture, often necessary for complex or atypical cases. They help clinicians differentiate between various inflammatory conditions and guide treatment strategies effectively.
Synovial Fluid Analysis
Synovial fluid, the lubricating fluid found in joints, provides valuable insights into inflammatory joint diseases like arthritis. Analysis of this fluid involves examining its appearance, viscosity, and cellular components. A cloudy, viscous fluid with high white blood cell counts suggests inflammation. Further analysis can identify the presence of crystals (such as uric acid crystals in gout) or infectious agents, helping to differentiate between various types of arthritis.
For instance, a sample showing high levels of neutrophils might indicate septic arthritis, while the presence of monosodium urate crystals confirms gout. The results of synovial fluid analysis, combined with clinical findings and imaging, are essential for accurate diagnosis and treatment planning.
Biopsies
In situations where inflammation affects specific tissues or organs, a biopsy can be invaluable. A biopsy involves removing a small tissue sample for microscopic examination. This allows pathologists to identify the type of inflammatory cells present, the extent of tissue damage, and the presence of any infectious agents or abnormal cells. For example, a skin biopsy might reveal the presence of specific inflammatory cells in psoriasis or a bowel biopsy could help diagnose inflammatory bowel disease (IBD).
The microscopic analysis of the tissue sample can provide detailed information about the nature of the inflammatory process and aid in determining the underlying cause. The specific type of biopsy (e.g., needle biopsy, incisional biopsy) will depend on the location and accessibility of the affected tissue.
Other Diagnostic Methods
Several other less common, but sometimes crucial, diagnostic methods exist for characterizing inflammation. These include:
- Endoscopy: Visual examination of internal organs (e.g., esophagus, stomach, colon) using a flexible tube with a camera. This technique can directly visualize inflamed tissue and allow for the collection of biopsies for further analysis. For example, endoscopy is frequently used to assess inflammation in the gastrointestinal tract.
- Laparoscopy: A minimally invasive surgical procedure involving small incisions to examine the abdominal cavity. This is particularly useful for investigating abdominal inflammation of unclear origin.
- Specialized Blood Tests: Beyond the basic inflammatory markers (CRP and ESR), there are more specific blood tests that can detect markers associated with particular inflammatory conditions. For example, tests for antineutrophil cytoplasmic antibodies (ANCA) are helpful in diagnosing vasculitis.
The choice of diagnostic method depends on the suspected cause and location of the inflammation, as well as the patient’s overall clinical presentation. Often, a combination of tests is necessary to arrive at an accurate diagnosis.
Interpreting Test Results and Next Steps
Understanding your inflammation test results is crucial for effective management. These results, combined with your symptoms and medical history, will guide your doctor in determining the best course of action. It’s important to remember that test results are just one piece of the puzzle; your doctor will consider the whole picture to reach a diagnosis and create a treatment plan.Interpreting test results often involves looking at specific markers, such as C-reactive protein (CRP) levels, erythrocyte sedimentation rate (ESR), and the presence of specific antibodies.
Elevated CRP and ESR often suggest the presence of inflammation, but they don’t pinpoint the cause. Antibody tests can help identify specific autoimmune conditions causing inflammation. For example, a positive rheumatoid factor (RF) test might indicate rheumatoid arthritis. The significance of these results varies depending on the individual and other clinical factors. A normal result doesn’t necessarily rule out inflammation, as some conditions may not show up in standard blood tests.
Treatment Strategies Based on Inflammation Test Results
The next steps after a diagnosis of inflammation depend heavily on the underlying cause and the severity of the inflammation. Treatment might involve medication, lifestyle changes, or a combination of both. For example, a patient with elevated CRP levels and diagnosed with osteoarthritis might receive pain management medication and physical therapy. In contrast, someone with elevated inflammatory markers and a suspected autoimmune disease would likely undergo more extensive testing and might require immunosuppressant medications.
- Non-steroidal anti-inflammatory drugs (NSAIDs): These are commonly used to reduce pain and inflammation, often as a first-line treatment for conditions like osteoarthritis or minor injuries. Examples include ibuprofen and naproxen. Side effects can include stomach upset and increased risk of bleeding.
- Corticosteroids: These powerful anti-inflammatory drugs are used for more severe inflammation. They can be administered orally, injected directly into the affected joint, or given intravenously. Long-term use carries significant side effects, so they are typically reserved for short-term treatment or severe cases.
- Disease-Modifying Antirheumatic Drugs (DMARDs): Used in autoimmune diseases like rheumatoid arthritis, these drugs aim to slow the progression of the disease and reduce inflammation. They often take several weeks or months to show effects. Methotrexate is a commonly used DMARD.
- Biologics: These are targeted therapies that specifically block certain molecules involved in the inflammatory process. They are often used for severe autoimmune diseases that haven’t responded to other treatments. Examples include TNF inhibitors (like infliximab) and interleukin-1 receptor antagonists.
- Lifestyle Modifications: These play a crucial role in managing inflammation, especially in conditions like obesity-related inflammation or inflammatory bowel disease. This can include weight loss, dietary changes (e.g., reducing processed foods, sugar, and saturated fats), regular exercise, and stress management techniques.
Examples of How Test Results Influence Treatment
Let’s consider two hypothetical patients: Patient A: Presents with knee pain and swelling. ESR and CRP levels are slightly elevated. X-rays show mild osteoarthritis. Treatment would likely involve NSAIDs, physical therapy, and weight management if needed. Patient B: Presents with widespread joint pain, fatigue, and fever.
ESR and CRP levels are significantly elevated. Rheumatoid factor (RF) and anti-citrullinated peptide antibodies (ACPA) are positive. This suggests rheumatoid arthritis. Treatment might begin with methotrexate, possibly supplemented with a biologic if the disease is severe or doesn’t respond adequately to methotrexate.The contrast highlights how different test results lead to tailored treatment approaches. The initial tests provide critical information to guide the diagnosis and subsequent treatment strategy.
Further testing might be needed to refine the diagnosis and monitor treatment response.
Factors Affecting Inflammation Testing
Getting accurate results from inflammation tests isn’t always straightforward. Several factors can influence the outcome, potentially leading to misinterpretations if not properly considered. Understanding these influences is crucial for both healthcare providers and patients to ensure appropriate diagnosis and treatment. This section will explore some key factors that can affect the accuracy and interpretation of inflammation tests.
Age, underlying health conditions, and medications all play significant roles in shaping inflammation test results. For example, certain inflammatory markers may naturally increase with age, leading to potentially elevated readings in older individuals even in the absence of disease. Similarly, pre-existing conditions like autoimmune diseases or chronic infections can significantly alter inflammatory markers, making it challenging to isolate inflammation related to a specific condition.
Finally, numerous medications, including steroids and some immunosuppressants, can directly impact inflammatory responses, potentially masking or artificially lowering inflammation levels.
Age’s Influence on Inflammation Test Results
Age significantly impacts the body’s inflammatory response. Older adults often exhibit higher levels of certain inflammatory markers, such as C-reactive protein (CRP), even when they are healthy. This age-related increase reflects the natural aging process and the accumulation of low-grade chronic inflammation over time. Therefore, interpreting CRP levels in older adults requires careful consideration of age-specific reference ranges. A CRP level considered elevated in a younger individual might fall within the normal range for an older person.
This highlights the importance of considering an individual’s age when interpreting inflammation test results.
Knowing when to test for inflammation is crucial, with blood tests like CRP and ESR being common methods. Interestingly, research suggests that eye exams might also offer clues about health risks; check out this article on whether can eye test detect dementia risk in older adults. Beyond blood work, imaging techniques like MRI can also detect inflammation in specific areas of the body.
So, considering various testing options is key for a comprehensive health assessment.
Impact of Underlying Health Conditions
Pre-existing health conditions substantially influence inflammation test results. Conditions like rheumatoid arthritis, lupus, inflammatory bowel disease, and infections often cause significantly elevated levels of inflammatory markers. The presence of these conditions can confound the interpretation of tests designed to assess inflammation related to a specific concern. For instance, a patient with rheumatoid arthritis undergoing testing for suspected appendicitis might have elevated CRP levels due to their arthritis, potentially obscuring the inflammation associated with the appendicitis.
Accurate interpretation requires careful consideration of the patient’s complete medical history and clinical presentation.
Medication Effects on Inflammation Test Results
Many medications can affect the body’s inflammatory response, leading to altered inflammation test results. Steroids, for example, are potent anti-inflammatory drugs that significantly suppress the immune system and lower inflammatory marker levels. This can lead to falsely low readings, masking underlying inflammation. Similarly, certain immunosuppressants used in organ transplantation or to treat autoimmune diseases can also reduce inflammatory markers.
Wondering when to test for inflammation? Blood tests like CRP and ESR are common, but sometimes more specialized tests are needed. Understanding the underlying causes is crucial, especially considering how inflammation can impact neurological conditions. For example, managing inflammation might be part of a broader approach to care, as outlined in this helpful article on strategies to manage Tourette syndrome in children , where inflammation could play a role.
Back to testing: your doctor can help determine the best approach based on your individual symptoms and medical history.
A complete medication history is essential for accurate interpretation of inflammation test results to avoid misdiagnosis.
Importance of a Complete Medical History
Providing a thorough medical history to healthcare professionals is paramount before undergoing inflammation testing. This includes details about all current medications (including over-the-counter drugs and supplements), pre-existing health conditions, recent infections, and any relevant family history. This comprehensive information allows healthcare providers to account for potential confounding factors and interpret the results accurately. Omitting crucial information can lead to inaccurate diagnoses and inappropriate treatment decisions.
Potential Sources of Error in Inflammation Testing
Several factors can introduce errors or inaccuracies into inflammation testing. Pre-analytical errors, such as improper sample collection or storage, can affect the accuracy of the results. Analytical errors, stemming from issues with the laboratory equipment or testing methods, can also occur. Finally, biological variation in inflammatory marker levels between individuals and even within the same individual at different times can lead to inconsistencies in results.
Careful adherence to standardized procedures throughout the testing process is essential to minimize these sources of error.
Epilogue
Navigating the world of inflammation testing can feel overwhelming, but understanding the available options and when to utilize them empowers you to proactively manage your health. Remember, early detection and appropriate testing are crucial for effective treatment. This post aimed to provide a clear and concise guide to help you understand when to seek medical attention, the different types of tests available, and how to interpret the results.
Don’t hesitate to discuss your concerns with your doctor – they are your best resource in understanding your individual situation and developing a personalized treatment plan. Your health journey is unique, and understanding inflammation is a significant step towards better well-being.
FAQ Insights
What if my inflammation test results are normal, but I still feel unwell?
Normal test results don’t always rule out inflammation. Other factors could be contributing to your symptoms. It’s crucial to discuss your persistent symptoms with your doctor to explore alternative explanations and further investigations.
How long does it take to get inflammation test results?
The turnaround time varies depending on the test. Simple blood tests may be available within a day or two, while imaging tests can take longer.
Are there any risks associated with inflammation testing?
Most inflammation tests carry minimal risks. However, some imaging tests, like CT scans, involve exposure to radiation. Your doctor will discuss any potential risks specific to your situation.
Can I test for inflammation at home?
While some at-home tests claim to detect inflammation markers, they are generally not as reliable as tests conducted in a clinical setting. For accurate diagnosis, it’s best to consult a healthcare professional.
