
Why The Time Is Now For Medicare Advantage Networks
Why the time is now for building Medicare Advantage networks? It’s a question echoing louder than ever, driven by a perfect storm of factors. Our aging population is booming, healthcare costs are skyrocketing, and technological advancements are reshaping how we deliver care. This isn’t just about numbers; it’s about ensuring our seniors have access to high-quality, affordable healthcare in a system that’s increasingly strained.
Let’s dive into why building robust Medicare Advantage networks is no longer a luxury, but a necessity.
The rising tide of seniors entering Medicare, coupled with escalating healthcare expenses, paints a clear picture: the current system is struggling to keep up. Medicare Advantage plans, with their focus on cost-efficiency and coordinated care, offer a powerful solution. We’ll explore how these networks leverage technology, streamline access to specialists, and ultimately improve patient outcomes. The private sector’s role in innovation and competition will also be a key focus, along with the supportive government policies driving this crucial shift.
The Aging Population and Increased Demand
The United States is experiencing a dramatic shift in its population demographics, with a rapidly growing elderly population placing unprecedented strain on the healthcare system. This surge in the number of Medicare-eligible individuals necessitates a proactive approach to network development, ensuring access to quality and affordable care for this vulnerable segment of society. Understanding the scale of this demographic change is crucial for effective planning and resource allocation within the healthcare industry.The number of Americans aged 65 and older is projected to nearly double by 2060, reaching 95 million.
This represents a significant increase in the demand for Medicare services. The implications of this growth are far-reaching, impacting not only the financial sustainability of Medicare but also the availability and accessibility of healthcare resources across the nation. This burgeoning elderly population also brings with it a significant increase in chronic conditions requiring ongoing and often complex medical management.
Projected Growth of the Medicare-Eligible Population
The following table illustrates the projected growth rates of different age groups within the Medicare-eligible population. These projections highlight the disproportionate increase in the older segments of the population, emphasizing the need for a robust and scalable Medicare Advantage network. These figures are based on projections from the U.S. Census Bureau and the Centers for Medicare & Medicaid Services (CMS).
For example, the rapid growth in the 85+ age group signifies a sharp increase in individuals requiring higher levels of care, potentially straining existing resources and infrastructure.
| Age Group | 2023 Population (Millions) (Estimate) | 2033 Projected Population (Millions) | Projected Growth Rate (%) |
|---|---|---|---|
| 65-74 | 25 | 30 | 20 |
| 75-84 | 15 | 22 | 47 |
| 85+ | 7 | 15 | 114 |
Increased Healthcare Needs of the Aging Population
The aging population is associated with a higher prevalence of chronic diseases such as heart disease, cancer, diabetes, and Alzheimer’s disease. These conditions require ongoing medical care, medication management, and often specialized services, leading to a significant increase in healthcare utilization. Furthermore, the elderly are more susceptible to falls and other accidents, resulting in increased demand for emergency and rehabilitative care.
The increasing prevalence of dementia and Alzheimer’s disease, in particular, presents a substantial challenge to the healthcare system, demanding specialized facilities and trained personnel. For instance, the growing need for home healthcare services reflects the desire of many seniors to age in place, further increasing the demand on healthcare resources.
Implications for the Healthcare System
The combined effect of a growing elderly population and increased healthcare needs poses significant challenges to the healthcare system. These challenges include increased strain on healthcare professionals, potential shortages of specialists, increased demand for hospital beds and long-term care facilities, and escalating healthcare costs. Failure to proactively address these issues could lead to longer wait times for appointments, reduced access to care, and compromised quality of care for Medicare beneficiaries.
The potential for increased healthcare costs necessitates innovative strategies to ensure the financial sustainability of the Medicare program and the overall healthcare system. This includes exploring alternative care models, promoting preventative care, and investing in technology to improve efficiency and reduce costs.
Rising Healthcare Costs and the Need for Efficiency: Why The Time Is Now For Building Medicare Advantage Networks
Source: pointclickcare.com
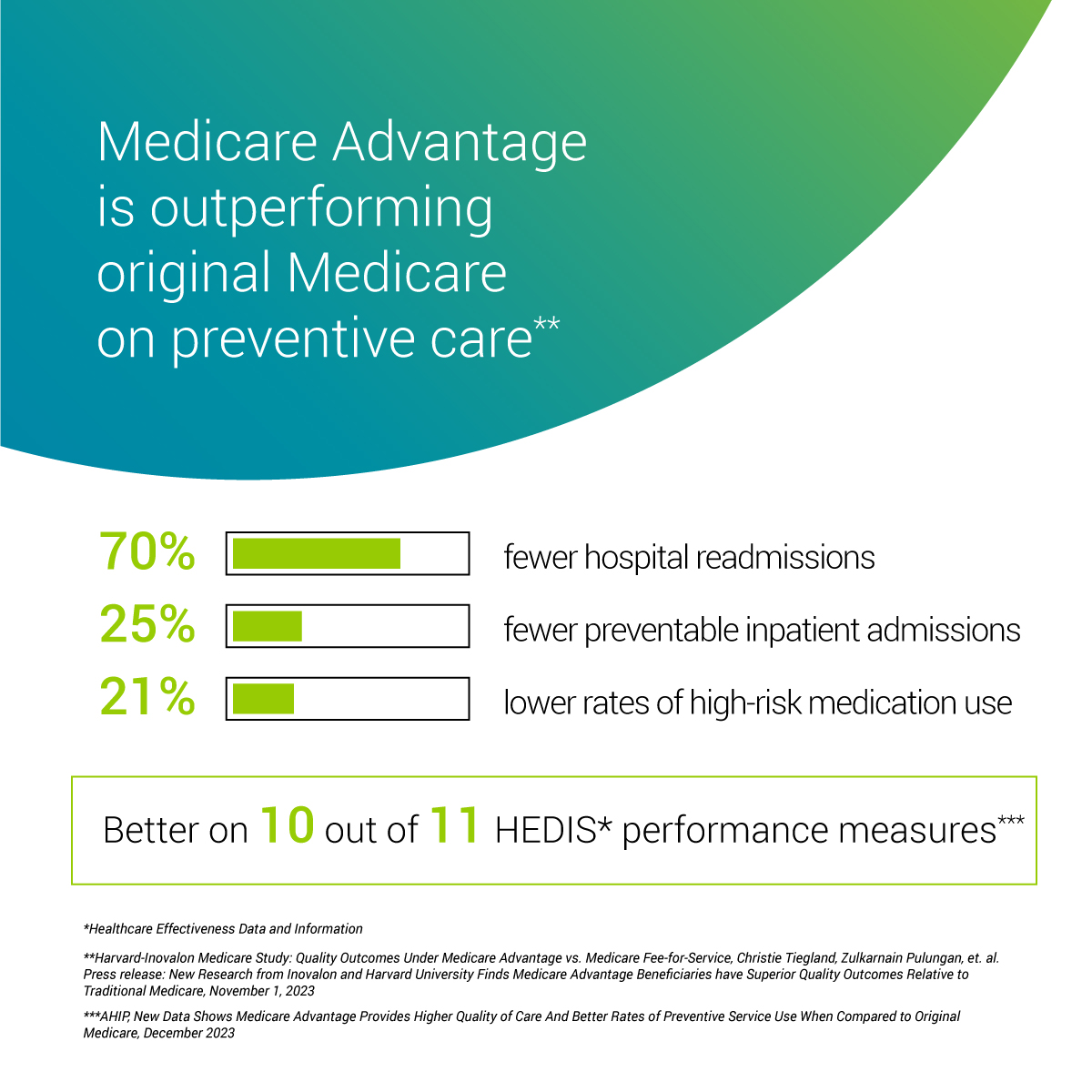
The cost of healthcare in the United States is a significant concern, impacting individuals, families, and the national economy. Traditional Medicare, while providing essential coverage, faces increasing pressure from rising medical expenses, leading to higher premiums and out-of-pocket costs for beneficiaries. This escalating cost necessitates a more efficient and sustainable approach to healthcare delivery for seniors, and Medicare Advantage plans offer a potential solution.Traditional Medicare’s costs have been climbing steadily.
For example, the Centers for Medicare & Medicaid Services (CMS) reported a significant increase in Part B premiums in recent years, reflecting the rising cost of physician services and medical technologies. Simultaneously, Part A premiums, while often covered by payroll taxes, are also subject to adjustments based on overall healthcare inflation. These rising costs place a considerable burden on both beneficiaries and the federal government.Medicare Advantage plans, also known as Part C, strive to control these escalating costs through a variety of mechanisms.
Instead of paying for services on a fee-for-service basis like traditional Medicare, Medicare Advantage plans negotiate contracts with healthcare providers, creating networks of doctors, hospitals, and other healthcare professionals. This network approach allows for greater bargaining power, potentially leading to lower costs for services. Additionally, these plans often incorporate preventive care and disease management programs, aiming to improve overall health and reduce the need for costly treatments down the line.Medicare Advantage’s Cost-Effectiveness Compared to Traditional MedicareThe cost-effectiveness of Medicare Advantage compared to traditional Medicare is a complex issue, with varying results depending on individual circumstances and plan specifics.
However, studies have shown that Medicare Advantage plans can often offer lower premiums and out-of-pocket costs than traditional Medicare, particularly for individuals who utilize a significant amount of healthcare services. This is because the managed care structure of Medicare Advantage plans incentivizes preventive care and efficient service delivery. Conversely, some individuals with specific healthcare needs might find traditional Medicare more suitable due to greater provider choice.
With the aging population and increasing healthcare costs, building robust Medicare Advantage networks is more crucial than ever. The recent Supreme Court decision, as reported in scotus overturns chevron doctrine healthcare , further underscores the need for proactive network development. This shift in regulatory power means greater uncertainty, making a strong, well-defined MA network a vital shield for both providers and beneficiaries.
Now is the time to invest and solidify these networks for a more stable future.
It’s crucial to carefully compare the costs and benefits of each option based on individual needs and healthcare utilization patterns.Cost-Saving Mechanisms Employed by Medicare Advantage NetworksThe cost savings achieved by Medicare Advantage networks stem from several key mechanisms. Understanding these mechanisms is crucial to grasping the potential of this approach in managing healthcare expenses.
- Negotiated Rates with Providers: Medicare Advantage plans leverage their large membership base to negotiate lower rates with healthcare providers, resulting in reduced costs for services.
- Preventive Care and Wellness Programs: By emphasizing preventive care and wellness initiatives, these plans aim to prevent costly illnesses and hospitalizations.
- Disease Management Programs: These programs focus on managing chronic conditions effectively, preventing complications and reducing the need for expensive treatments.
- Care Coordination: Improved care coordination, including streamlined referrals and communication among providers, enhances efficiency and reduces unnecessary testing or procedures.
- Utilization Management: Techniques to monitor and manage the use of healthcare services help to ensure that only necessary services are provided.
Technological Advancements and Improved Care Coordination
The rapid evolution of technology is revolutionizing healthcare, and Medicare Advantage plans are leveraging these advancements to enhance efficiency, improve patient care, and ultimately, control costs. This integration isn’t just about adopting new tools; it’s about fundamentally reshaping how care is delivered and experienced by the aging population. By embracing technology, Medicare Advantage networks can offer more proactive, personalized, and accessible healthcare.The use of technology within Medicare Advantage networks significantly impacts the quality and efficiency of care delivery.
This leads to better patient outcomes, improved satisfaction, and more sustainable healthcare spending. The key lies in integrating various technologies seamlessly to create a cohesive and comprehensive care ecosystem.
Telehealth and Remote Patient Monitoring Enhancements
Telehealth and remote patient monitoring (RPM) are transforming how healthcare is delivered, particularly for the Medicare Advantage population. Telehealth allows for virtual consultations, reducing the need for in-person visits and improving access to specialists for individuals in rural areas or with mobility limitations. RPM uses wearable devices and remote monitoring systems to track vital signs, activity levels, and other health metrics, allowing for early detection of potential problems and timely intervention.
For example, a patient with congestive heart failure can have their weight and blood pressure monitored remotely, alerting their physician to any concerning changes before they escalate into a hospital visit. This proactive approach not only improves patient outcomes but also significantly reduces healthcare costs by preventing hospital readmissions and emergency room visits.
Technological Innovations Transforming Medicare Advantage Delivery
Several technological innovations are reshaping healthcare delivery within Medicare Advantage. Artificial intelligence (AI) is being used to analyze patient data, predict health risks, and personalize treatment plans. Machine learning algorithms can identify patterns in medical records to identify patients at high risk of developing certain conditions, allowing for proactive interventions. Predictive analytics, powered by AI, can forecast potential hospital readmissions, enabling proactive care management strategies.
Furthermore, the use of electronic health records (EHRs) facilitates seamless information sharing among providers, reducing medical errors and improving care coordination. The integration of these technologies creates a more holistic and efficient approach to patient care.
Technologies Used in Medicare Advantage and Their Impact
| Technology | Impact on Patient Care | Impact on Cost | Example |
|---|---|---|---|
| Telehealth | Improved access to care, increased convenience, reduced travel time | Reduced costs associated with in-person visits, fewer hospital readmissions | Virtual doctor consultations for chronic disease management |
| Remote Patient Monitoring (RPM) | Early detection of health problems, proactive interventions, improved self-management | Reduced hospitalizations, fewer emergency room visits, improved medication adherence | Continuous glucose monitoring for diabetes patients |
| Artificial Intelligence (AI) | Personalized treatment plans, risk prediction, improved diagnostic accuracy | Optimized resource allocation, reduced medical errors, improved efficiency | AI-powered diagnostic tools for early cancer detection |
| Electronic Health Records (EHRs) | Improved care coordination, reduced medical errors, better communication among providers | Streamlined administrative processes, reduced paperwork, improved data analysis | Centralized access to patient medical history across different healthcare settings |
Expanding Access to Care and Improved Patient Outcomes
Medicare Advantage (MA) plans are fundamentally reshaping healthcare access, particularly for seniors in underserved communities and those facing complex health needs. By offering a wider network of providers and comprehensive benefits, MA plans are proving instrumental in bridging the gap to better health outcomes. This enhanced access and coordinated care are driving positive changes in the lives of millions of beneficiaries.Medicare Advantage networks improve access to healthcare services, especially in underserved areas, by contracting with a larger and more geographically diverse range of providers than traditional Medicare.
This includes doctors, hospitals, and specialists, often extending coverage into rural and medically underserved areas where access to care might otherwise be limited. The competitive bidding process employed by MA plans often incentivizes providers to expand their services into these areas, making healthcare more readily available to those who need it most.
The aging population necessitates robust Medicare Advantage networks now more than ever. Proactive healthcare is key, and understanding potential health risks early is crucial. A fascinating study explores whether a simple eye test, as detailed in this article can eye test detect dementia risk in older adults , could help predict dementia. This highlights the need for comprehensive networks that incorporate preventative screenings, making early interventions possible and ultimately strengthening the value of Medicare Advantage.
Improved Care Coordination and Health Outcomes
MA plans frequently incorporate care coordination programs designed to improve patient outcomes. These programs often involve proactive outreach to beneficiaries, personalized care plans, and regular monitoring of health status. By actively managing a patient’s care, MA plans aim to prevent hospital readmissions, manage chronic conditions effectively, and improve overall health. This coordinated approach helps ensure patients receive the right care at the right time, leading to better health outcomes and reduced healthcare costs in the long run.
Successful programs often utilize technology, such as telehealth, to facilitate communication and monitoring between patients and their healthcare teams.
Access to Specialists and Preventative Care
Compared to traditional Medicare, MA plans often provide easier access to specialists. Traditional Medicare requires beneficiaries to navigate the referral process, potentially facing delays in seeing specialists. Many MA plans streamline this process, providing more direct access to specialists within their network. Similarly, MA plans frequently offer comprehensive preventative care services, such as annual wellness visits and screenings, at no additional cost to the beneficiary.
This proactive approach to healthcare helps identify and address potential health problems early, preventing more serious and costly issues down the line. The inclusion of these services in MA plans contributes to better preventative care adherence among beneficiaries.
Successful Initiatives Improving Patient Outcomes
Several successful initiatives demonstrate the positive impact of MA networks on patient outcomes. For example, some plans have implemented programs focusing on chronic disease management for conditions like diabetes and heart disease. These programs involve regular monitoring, education, and support, resulting in improved blood sugar control, blood pressure management, and reduced hospitalizations. Another example is the use of telehealth technology by certain MA plans, allowing for remote monitoring of patients with chronic conditions and providing timely intervention when needed.
This approach reduces the need for frequent in-person visits, improving convenience and access for beneficiaries, especially those in rural areas. The expansion of mental health services through MA networks is also a noteworthy success, providing more accessible and affordable care to beneficiaries struggling with mental health challenges. These examples illustrate the potential of MA plans to improve patient outcomes through comprehensive and coordinated care.
The Role of Private Sector Innovation and Competition

Source: ytimg.com
The private sector plays a vital role in the success of Medicare Advantage, injecting much-needed competition and innovation into a system that, without it, might struggle to keep pace with evolving healthcare needs and technological advancements. The involvement of private insurance companies offers a dynamic alternative to the traditional fee-for-service Medicare model, ultimately benefiting both beneficiaries and the overall healthcare system.Private sector participation fosters a competitive environment where insurance companies strive to offer the most attractive plans to attract and retain enrollees.
This competition isn’t just about price; it extends to the breadth and quality of benefits, the accessibility of care, and the overall member experience. The pressure to stand out compels insurers to constantly refine their offerings, leading to improvements in care coordination, technological integration, and patient satisfaction.
Medicare Advantage Plan Variety and Benefits
Different Medicare Advantage providers offer a wide spectrum of plans, each designed to cater to specific needs and preferences. For example, some plans might focus on comprehensive coverage with low out-of-pocket costs, while others might emphasize access to specialized care or a particular network of providers. A retiree living in a rural area might prioritize a plan with extensive telehealth options, while a city dweller might value a plan with a large network of local specialists.
This variety ensures that beneficiaries can find a plan that aligns with their individual circumstances and healthcare requirements. Some plans might include vision, dental, and hearing benefits not typically covered under original Medicare, making them particularly attractive to seniors. Others might feature wellness programs, gym memberships, or other perks designed to promote healthy aging.
Advantages of Multiple Private Sector Providers
The presence of multiple private sector providers within Medicare Advantage creates a robust and dynamic market. This competition drives innovation and improves the quality of care for several key reasons:
- Increased Choice and Customization: Beneficiaries have a wider range of plans to choose from, ensuring a better fit for their individual needs and preferences.
- Lower Costs Through Competition: The competitive pressure to attract enrollees often leads to more affordable premiums and lower out-of-pocket costs.
- Improved Quality of Care: Plans compete to offer superior care coordination, access to specialists, and other value-added services to attract and retain members.
- Enhanced Innovation: The drive to differentiate themselves pushes insurers to adopt new technologies and implement innovative care delivery models.
- Greater Accountability: Competition encourages plans to be more responsive to beneficiary needs and concerns, improving customer service and plan administration.
Government Policies and Incentives Supporting Medicare Advantage
The growth of Medicare Advantage (MA) isn’t accidental; it’s a direct result of deliberate government policies and incentives designed to encourage private sector participation in providing healthcare to seniors. These policies aim to improve efficiency, competition, and ultimately, the quality of care received by Medicare beneficiaries. Understanding these incentives is crucial to grasping the current landscape of MA and its future trajectory.Government policies supporting Medicare Advantage are multifaceted, encompassing financial incentives, regulatory frameworks, and strategic initiatives aimed at expanding access and improving quality.
These policies have significantly shaped the market, leading to the growth we see today. This influence is evident in the increasing number of beneficiaries choosing MA plans and the expansion of plan offerings across the country.
Building Medicare Advantage networks is crucial now, more than ever, to address the growing senior population’s healthcare needs. Effective network design requires considering diverse health issues; for instance, many seniors experience carpal tunnel syndrome, and thankfully, there are non-surgical options like those detailed on this helpful resource: ways to treat carpal tunnel syndrome without surgery. Understanding these diverse needs allows for the creation of comprehensive and supportive Medicare Advantage networks, ensuring better care for everyone.
Medicare Payment Rates and Risk Adjustment
Medicare Advantage plans receive payments from the Centers for Medicare & Medicaid Services (CMS) based on a capitated payment system. This means CMS pays a predetermined amount per beneficiary per month, regardless of the actual services provided. This payment model incentivizes plans to manage costs effectively and provide preventive care to avoid expensive hospitalizations and other high-cost interventions.
Furthermore, a risk adjustment mechanism ensures that plans receive higher payments for individuals with more complex health needs. This system encourages insurers to focus on managing chronic conditions and improving the overall health of their enrollees. For example, a plan with a higher proportion of beneficiaries with diabetes would receive a higher payment per member compared to a plan with a healthier population.
Marketing and Enrollment Support
Government regulations support marketing and enrollment efforts for Medicare Advantage plans, ensuring transparency and consumer protection. This includes requirements for clear and accurate plan information, standardized benefit descriptions, and unbiased counseling services to help beneficiaries make informed choices. This ensures that beneficiaries are well-informed about their plan options and can select the plan that best meets their individual needs.
CMS also actively promotes Medicare Savings Programs (MSPs) which help low-income seniors afford Medicare premiums and cost-sharing.
Quality Improvement Programs and Reporting, Why the time is now for building medicare advantage networks
CMS employs a variety of quality improvement programs and initiatives that monitor and incentivize high-quality care in Medicare Advantage. These programs use quality metrics to evaluate plans, and publicly report this information. Plans that consistently achieve high scores on quality measures may receive bonuses or other incentives, while those failing to meet standards may face penalties. This accountability mechanism promotes better care and encourages continuous improvement within MA plans.
Star ratings, a widely recognized system, are a prime example of this approach, impacting consumer choice and plan reimbursement.
Visual Representation: Government Policies and MA Growth
Imagine a graph with two axes. The horizontal axis represents time (years), showing a steady increase over time. The vertical axis represents the number of Medicare Advantage enrollees. The graph shows an upward-sloping line representing the growth of MA enrollment. Superimposed on this line are several arrows pointing upward, each labeled with a key government policy: “Risk Adjustment,” “Capitated Payments,” “Quality Improvement Programs,” and “Marketing Support.” These arrows visually represent the positive influence of these policies on MA enrollment growth, showing how they contribute to the overall upward trend.
The graph clearly demonstrates the correlation between government policies and the expanding Medicare Advantage market.
Summary
In conclusion, the case for building Medicare Advantage networks is undeniably strong. The convergence of demographic shifts, escalating costs, technological innovation, and supportive government policies creates a compelling argument for prioritizing this approach. By embracing the potential of Medicare Advantage, we can not only address the immediate challenges facing our healthcare system but also pave the way for a more sustainable, efficient, and ultimately, more compassionate system of care for our aging population.
It’s not just about the future; it’s about ensuring the well-being of our loved ones today.
Questions and Answers
What are the biggest challenges facing traditional Medicare?
Traditional Medicare faces challenges with rising costs, fragmented care coordination, and limited access to certain specialists in some areas.
How do Medicare Advantage plans address cost concerns?
Medicare Advantage plans often negotiate lower rates with providers, utilize preventative care to reduce future costs, and manage care more efficiently through coordinated networks.
Are there downsides to Medicare Advantage?
Some plans may have limited provider networks, requiring beneficiaries to choose doctors within a specific group. There might also be out-of-pocket costs depending on the plan.
How does technology improve Medicare Advantage?
Telehealth, remote patient monitoring, and data analytics are improving care access, coordinating treatments, and leading to better health outcomes for beneficiaries.





