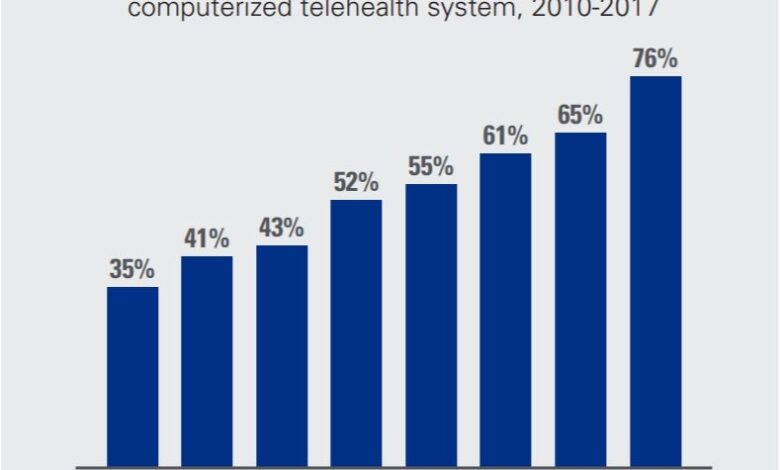
Telehealth Visits Billed Lower Epic Research Findings
Telehealth visits billed lower level service less complex than office visits epic research – that’s a mouthful, right? But it’s a crucial topic for anyone involved in telehealth, from doctors and billing staff to patients themselves. This post dives into a recent study exploring why telehealth visits often receive lower billing codes than in-person appointments, even when the service provided is similar.
We’ll unpack the complexities of CPT codes, reimbursement rates, and the role of electronic health record systems like Epic in this evolving landscape. Get ready to understand the financial implications for providers and the patient experience differences.
We’ll be examining the key factors contributing to this disparity, including the differences in time commitment, overhead costs, and the complexities involved in assessing the level of service provided during both telehealth and in-person visits. We’ll also explore how Epic Systems, a widely used EHR, handles the billing process for telehealth, comparing it to traditional office visit billing. Finally, we’ll look at the impact on healthcare providers and patients, exploring strategies to mitigate financial challenges and improve patient satisfaction.
Telehealth Billing Practices Compared to In-Person Visits: Telehealth Visits Billed Lower Level Service Less Complex Than Office Visits Epic Research

Source: healthyagingpoll.org
Telehealth billing differs significantly from in-person office visit billing, primarily due to variations in service delivery and associated costs. Understanding these differences is crucial for accurate reimbursement and maintaining financial stability in a practice offering both telehealth and in-person services. This post will clarify the key distinctions and provide examples to illustrate the complexities involved.
That recent Epic research showing telehealth visits billed at a lower service level than in-person visits really got me thinking. It highlights the complexities of healthcare reimbursement, especially considering the ongoing fight for affordable healthcare. Check out this article about the AHA’s court brief urging a stay to restore the Affordable Care Act’s preventive services: aha hospital groups court brief urging stay restore Affortable Care Act preventive.
The potential impact on telehealth access, given the already lower reimbursement rates, is significant and warrants further discussion.
CPT Codes for Telehealth and In-Person Visits
The Current Procedural Terminology (CPT) codes used for telehealth visits differ from those used for in-person office visits, even when the services rendered are identical. For example, a standard office visit might use CPT code 99213 (office or other outpatient visit, established patient, of moderate complexity), while the equivalent telehealth visit might use CPT code 99213 (office or other outpatient visit, established patient, of moderate complexity) with a telehealth modifier appended, such as -GT for a synchronous visit or -GQ for an asynchronous visit.
The modifier clarifies that the service was delivered remotely. The base code remains the same, reflecting the level of service complexity, but the modifier differentiates the method of delivery. Other examples include 99214 and 99215 for higher complexity visits, each having telehealth equivalents with appropriate modifiers. The specific code used depends on the type and duration of the visit, as well as the complexity of medical decision-making and the amount of documentation required.
Factors Influencing Lower Telehealth Billing
Several factors contribute to the generally lower reimbursement rates for telehealth services compared to in-person visits. One significant factor is the perceived reduction in time spent on patient interaction. While the actual time spent might be similar, the absence of physical examination components or the need for less extensive documentation in some cases can lead to lower billing.
Additionally, telehealth visits often involve lower overhead costs for the provider, such as reduced facility expenses, less staff time for room preparation and cleaning, and decreased supply costs. However, it’s crucial to note that while overhead might be lower, the technology and infrastructure required to support telehealth can represent a substantial investment for providers.
Telehealth Reimbursement Compared to Office Visit Reimbursement
The following table illustrates a comparison of reimbursement rates, acknowledging that these rates can vary widely based on payer contracts, geographic location, and specific service provided. These are illustrative examples and should not be considered definitive reimbursement values.
| Service Type | Telehealth Reimbursement | Office Visit Reimbursement | Percentage Difference |
|---|---|---|---|
| Established Patient, Low Complexity (e.g., 99211 equivalent) | $50 | $75 | -33% |
| Established Patient, Moderate Complexity (e.g., 99213 equivalent) | $100 | $150 | -33% |
| Established Patient, High Complexity (e.g., 99215 equivalent) | $175 | $250 | -30% |
| New Patient, Low Complexity (e.g., 99201 equivalent) | $70 | $100 | -30% |
Complexity Levels in Telehealth and Office Visits
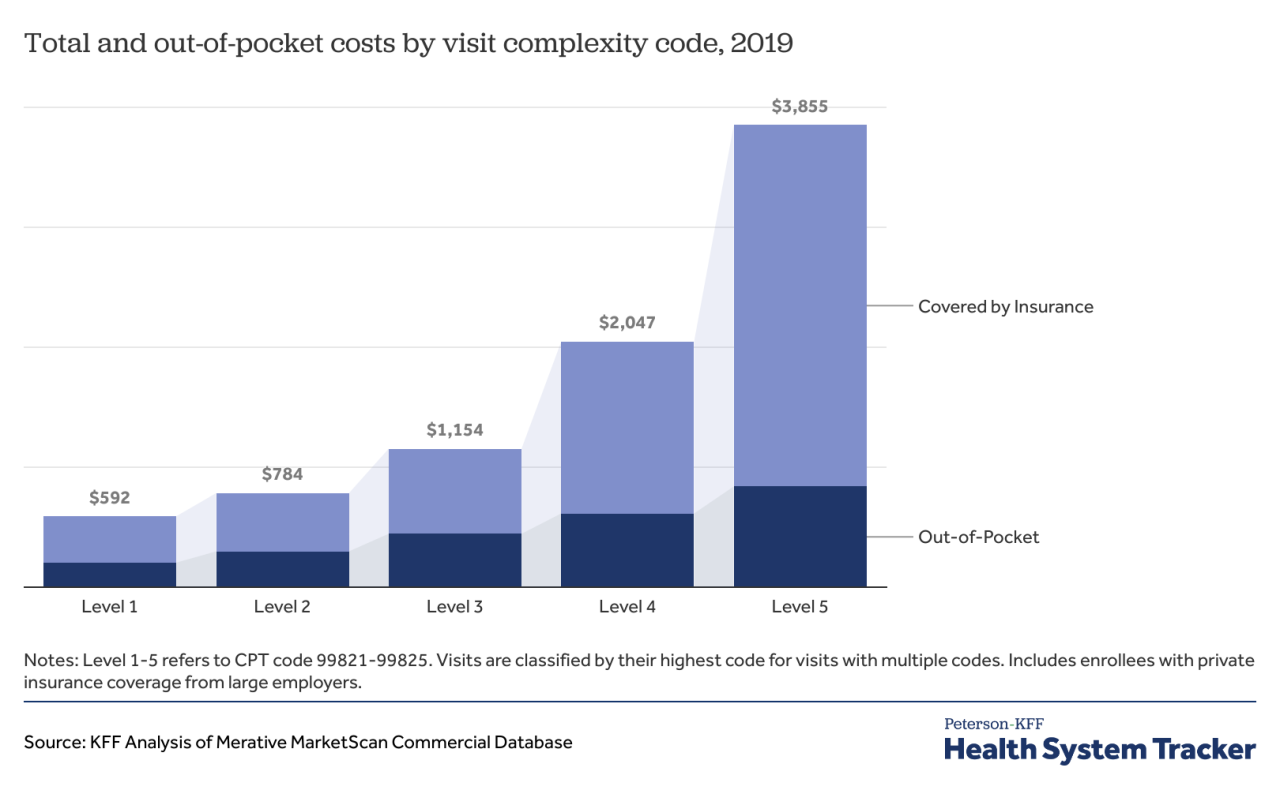
Source: healthsystemtracker.org
Determining the appropriate level of complexity for a medical visit, whether in-person or via telehealth, is crucial for accurate billing and reflects the physician’s time and effort. The complexity is based on several factors, including the patient’s medical history, the nature of the problem, the number of diagnoses, and the level of medical decision-making required. While the underlying principles are similar, the specific nuances can differ slightly between in-person and telehealth encounters.
Criteria for Determining Complexity Levels
The evaluation of visit complexity involves a multi-faceted assessment. For both in-person and telehealth visits, key factors include the extent of the patient’s history, the number and complexity of problems addressed, the amount of counseling and coordination of care required, and the risk of the medical decision-making involved. Documentation of these factors is critical for justifying the chosen billing code.
Specifically, the Evaluation and Management (E/M) coding guidelines published by the American Medical Association (AMA) provide a framework for this assessment, although the specific application may vary depending on the payer.
So, the Epic research showing telehealth visits billed at a lower service level than in-person visits got me thinking about the wider implications for healthcare. It highlights the need for robust systems, especially considering the hhs healthcare cybersecurity framework hospital requirements cms mandates for data security. After all, secure telehealth platforms are crucial to ensuring patient privacy, no matter the billing structure.
Examples of Complexity Levels in Telehealth and Office Visits
To illustrate, let’s compare low, moderate, and high-complexity visits across both settings. Note that these are illustrative examples and specific circumstances will influence the final coding decision.
Low Complexity: A telehealth visit involving a routine medication refill for a patient with well-controlled hypertension, requiring minimal discussion and review of vitals (if obtained remotely). The office visit equivalent would be a brief follow-up visit with similar characteristics. Both scenarios would likely be coded at a lower level.
Moderate Complexity: A telehealth visit addressing a new onset of symptoms (e.g., persistent cough), requiring a detailed history, review of systems, and ordering of basic diagnostic tests. The office visit equivalent might involve a similar history-taking process, a physical exam, and ordering of tests. Both would fall into a moderately complex billing category.
High Complexity: A telehealth visit involving a complex chronic disease management (e.g., diabetes with multiple complications), requiring extensive discussion of treatment plans, coordination of care with specialists, and detailed counseling. The in-person equivalent would involve a comprehensive review of systems, a detailed physical exam, and extensive documentation of the management plan. This would necessitate the use of a higher level billing code for both visit types.
Documentation Requirements Based on Complexity Levels
The level of detail required in medical documentation directly correlates with the complexity of the visit. Low-complexity visits require concise documentation of the reason for the visit, brief notes on the patient’s history, and the plan of care. Moderate-complexity visits demand more detailed documentation, including a more comprehensive review of systems, a detailed problem list, and a more elaborate treatment plan.
High-complexity visits require even more extensive documentation, reflecting the significant time and effort invested in managing the patient’s complex medical needs. Regardless of the setting (telehealth or in-person), thorough and accurate documentation is essential for supporting the billing code chosen. Incomplete or poorly documented visits risk audit issues and payment denials.
Flowchart for Determining Telehealth Billing Codes
The following flowchart Artikels the decision-making process for determining the appropriate billing code for a telehealth visit. This is a simplified representation and should be used in conjunction with the official E/M coding guidelines.
[Flowchart Description]: The flowchart would begin with a box asking: “What is the primary reason for the telehealth visit?”. This would branch to three separate paths: Low Complexity (e.g., medication refill, simple follow-up), Moderate Complexity (e.g., new symptom evaluation, minor acute illness), and High Complexity (e.g., chronic disease management, multiple complex issues). Each path would lead to a box indicating the appropriate level of documentation and the corresponding billing code(s).
The flowchart would conclude with a box confirming the documentation has been completed and the appropriate code has been selected.
Epic Systems and Telehealth Billing
Navigating the complexities of telehealth billing can be daunting, especially when using a robust Electronic Health Record (EHR) system like Epic. Understanding how Epic handles telehealth billing is crucial for accurate coding and timely reimbursement. This post will delve into the specific features and workflows within Epic that streamline the process, focusing on low-complexity telehealth visits.Epic offers a comprehensive suite of tools designed to manage the entire billing cycle for telehealth visits, from documentation to claim submission.
The system’s strength lies in its integration, allowing for seamless data flow between different modules, reducing manual data entry and minimizing the potential for errors. This efficiency is particularly valuable when dealing with the nuances of telehealth billing, which often require specific documentation to justify the level of service provided.
Epic Features for Telehealth Documentation and Coding
Epic utilizes several key features to facilitate the documentation and coding of telehealth encounters. The primary tool is the encounter note, where providers document the patient’s history, examination findings, and the plan of care. Within the note, specific fields or checkboxes are often available to designate the visit as a telehealth encounter, automatically triggering the appropriate CPT codes or modifiers.
Moreover, Epic’s charge entry module allows for direct selection of telehealth-specific codes, ensuring accurate billing. The system also offers robust reporting capabilities, allowing practices to track telehealth billing performance and identify potential areas for improvement. For example, a report could easily track the number of telehealth visits billed, the average reimbursement rate, and the percentage of claims denied.
Workflow Comparison: Telehealth vs. Traditional Office Visits in Epic
While the core workflow for billing in Epic remains largely consistent between telehealth and in-person visits, key differences exist. In a traditional office visit, the provider typically sees the patient in person, documents the encounter, and the billing staff subsequently enters the charges into Epic based on the documentation. For telehealth visits, the workflow is similar, but the initial encounter is conducted remotely via video conferencing or telephone.
The documentation process remains crucial, and the provider must meticulously document the interaction to support the billing codes. The key difference lies in the selection of the appropriate CPT code and the use of telehealth modifiers, which indicate that the service was delivered remotely. The billing staff must ensure these modifiers are correctly applied to the claim.
Step-by-Step Guide: Billing a Low-Complexity Telehealth Visit in Epic
The following steps Artikel the process of billing a low-complexity telehealth visit using Epic. Remember that specific steps might vary slightly depending on your organization’s Epic configuration.
- Document the Encounter: The provider documents the telehealth visit in the patient’s chart, noting the date, time, method of communication (video or phone), and the details of the patient interaction. The level of complexity is determined based on the time spent, medical decision-making, and the complexity of the medical problem. For a low-complexity visit, this documentation should reflect a brief interaction focused on a well-defined problem.
- Select the Appropriate CPT Code and Modifier: Based on the documentation, the appropriate CPT code for the telehealth visit is selected. For low-complexity visits, this is typically a 99211 equivalent code. A telehealth modifier (e.g., GT) must also be added to indicate that the service was provided remotely. This ensures proper reimbursement from payers.
- Charge Entry: The billing staff enters the charge in Epic’s charge entry module, selecting the CPT code and modifier. They should review the charge for accuracy before submitting the claim.
- Claim Submission: Epic automatically generates and submits the claim to the payer. The billing staff can monitor the claim status within Epic to ensure it is processed correctly.
- Review and Follow Up: The billing staff should regularly review claim denials and take appropriate action to correct any errors and ensure timely payment.
Impact of Lower Billing on Healthcare Providers
The shift towards telehealth has brought about significant changes in healthcare delivery, but the lower reimbursement rates for telehealth services compared to in-person visits pose a considerable challenge for many healthcare providers. This disparity impacts their financial stability, potentially affecting their ability to provide quality care and maintain access for patients. Understanding these financial implications is crucial for navigating the evolving landscape of healthcare reimbursement.Lower telehealth reimbursement rates directly reduce the revenue generated per patient encounter.
This can be particularly problematic for practices heavily reliant on telehealth, or those with a higher percentage of patients utilizing this service due to geographic location or other factors. The financial strain can lead to reduced profitability, impacting the ability to cover operational costs, invest in technology upgrades, and compensate staff adequately. This financial pressure may even force some providers to reduce telehealth services or cease offering them altogether.
The recent Epic research highlighting that telehealth visits are often billed at a lower service level than in-person visits due to perceived lower complexity is a real concern. This issue is further complicated by the current healthcare staffing crisis, as highlighted in this article about healthcare executives say talent acquisition labor shortages business risk , impacting the ability to properly manage and code these virtual encounters.
Ultimately, this discrepancy in billing could affect revenue and needs further investigation to ensure fair compensation for telehealth services.
Financial Implications for Healthcare Providers
The reduced revenue from lower telehealth reimbursement rates creates a significant financial burden. For example, a practice that relies heavily on telehealth might see a 20-30% reduction in revenue per patient compared to an in-person visit, depending on the specific service and payer. This can quickly accumulate, impacting the practice’s bottom line and potentially leading to staff layoffs, reduced operating hours, or limitations on the types of telehealth services offered.
The impact is magnified for smaller practices with fewer resources to absorb these financial losses. Larger hospital systems might experience similar pressures but often have more resources to offset these losses.
Strategies to Mitigate Financial Impact, Telehealth visits billed lower level service less complex than office visits epic research
Providers can employ several strategies to mitigate the financial impact of lower telehealth reimbursement. One approach is to increase patient volume through efficient scheduling and effective marketing strategies focused on the convenience and accessibility of telehealth. Negotiating favorable contracts with payers to secure higher reimbursement rates for specific telehealth services is also crucial. This requires careful analysis of the market and the willingness to demonstrate the value of telehealth services through data on patient outcomes and cost savings.
Diversifying revenue streams by offering additional services such as preventative care or chronic disease management through telehealth can also help to offset lower reimbursement rates for individual visits. Finally, optimizing operational efficiency through streamlined workflows and the use of telehealth-specific technologies can reduce costs and improve profitability.
Effects on Access to Telehealth Services
The financial pressures caused by lower telehealth reimbursement rates can inadvertently limit patient access to these services. If providers reduce telehealth offerings due to financial constraints, patients in rural areas or those with mobility challenges may find it more difficult to receive necessary care. This can exacerbate existing health disparities and negatively impact overall health outcomes. The reduced availability of telehealth services might also discourage patients from seeking care, leading to delayed diagnoses and treatment, potentially resulting in more serious health complications.
Impact on the Overall Healthcare System
Changes in telehealth billing policies have far-reaching implications for the healthcare system. If lower reimbursement rates lead to a widespread reduction in telehealth services, it could hinder the adoption of this valuable tool for improving access to care, particularly for underserved populations. This could impact the overall efficiency and cost-effectiveness of the healthcare system, potentially increasing hospital readmissions and emergency room visits due to delayed or inadequate care.
Furthermore, consistent and equitable reimbursement policies are needed to ensure the long-term sustainability and widespread adoption of telehealth as a critical component of modern healthcare delivery.
Patient Experience and Telehealth Visits
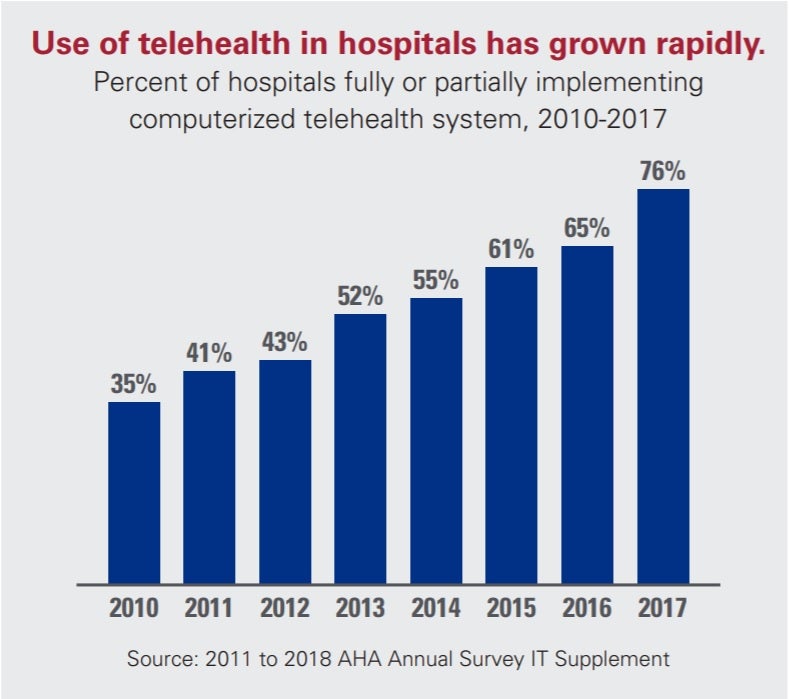
Source: aha.org
Telehealth has revolutionized healthcare access, particularly for low-complexity issues. Understanding the patient experience during these virtual visits is crucial for optimizing the system and ensuring patient satisfaction. This section delves into the typical experience, comparing it to in-person visits and highlighting both advantages and disadvantages.The typical patient experience during a low-complexity telehealth visit usually begins with scheduling the appointment, often through a patient portal or phone call.
The visit itself involves connecting via video conferencing software, where the patient describes their symptoms and answers the provider’s questions. The provider may perform a virtual examination, using the camera to assess the patient’s condition. The visit concludes with a diagnosis, treatment plan, and instructions for follow-up, all delivered virtually. The entire process, for simpler issues, can be significantly shorter than an in-person visit.
Patient Satisfaction Levels in Telehealth vs. In-Person Visits
Studies comparing patient satisfaction between telehealth and in-person visits for low-complexity issues show mixed results. While many patients appreciate the convenience and time savings of telehealth, some find the lack of physical examination limiting and prefer the personal interaction of an in-person visit. Factors influencing satisfaction include the patient’s comfort level with technology, the provider’s communication style, and the specific nature of the health concern.
For example, a patient with a simple rash might find telehealth perfectly adequate, while a patient with chronic pain might prefer a more thorough in-person assessment. Ultimately, patient satisfaction depends on individual needs and preferences.
Challenges and Benefits of Lower Complexity Telehealth Visits from a Patient Perspective
Lower complexity telehealth visits present both challenges and benefits for patients. Challenges can include technological difficulties (poor internet connection, unfamiliar software), feelings of impersonal interaction, and limitations in the physical examination. Benefits include increased convenience, reduced travel time and costs, and potentially faster access to care. For patients in rural areas or those with mobility issues, telehealth offers a significant improvement in access to healthcare services.
Furthermore, the ability to easily schedule appointments during off-peak hours enhances flexibility for busy individuals.
Advantages and Disadvantages of Lower-Complexity Telehealth Visits from the Patient Viewpoint
Let’s summarize the advantages and disadvantages from the patient’s perspective in a bullet-point list:
- Advantages:
- Increased convenience and flexibility in scheduling.
- Reduced travel time and costs.
- Faster access to care, especially for non-urgent issues.
- Improved access for patients with mobility limitations or residing in remote areas.
- Potentially lower overall cost compared to in-person visits (depending on insurance coverage).
- Disadvantages:
- Potential for technological difficulties (internet connectivity, software issues).
- Limited physical examination capabilities.
- May feel less personal than an in-person visit.
- Not suitable for all health concerns requiring a thorough physical examination.
- Potential for communication barriers if technology is unreliable.
Final Summary
So, the bottom line? The research clearly shows that telehealth visits are frequently billed at a lower level than comparable office visits, impacting both providers and patients. Understanding the reasons behind this – from differences in CPT codes and documentation requirements to the inherent complexities of assessing service level remotely – is crucial for navigating this changing healthcare landscape.
By recognizing these challenges and exploring potential solutions, we can work towards a fairer and more sustainable system that supports both high-quality care and equitable reimbursement for telehealth services. Let’s keep the conversation going – what are your thoughts and experiences?
Query Resolution
What are the most common reasons for lower telehealth reimbursement?
Lower reimbursement is often attributed to factors like reduced time spent with the patient, decreased overhead costs for the provider, and the perceived lower complexity of some telehealth encounters compared to in-person visits.
How does patient complexity impact telehealth billing?
Just like in-person visits, the complexity of a telehealth visit influences billing. More complex cases with extensive documentation and decision-making will generally receive higher reimbursement.
Can I negotiate telehealth billing rates with insurance companies?
Negotiating rates can be challenging but is sometimes possible, especially for providers with high patient volumes or specialized services. It’s often beneficial to consult with billing specialists.
Are there any resources available to help providers optimize telehealth billing?
Yes, many resources are available, including professional billing services, online guides, and webinars focused on telehealth billing best practices and compliance.