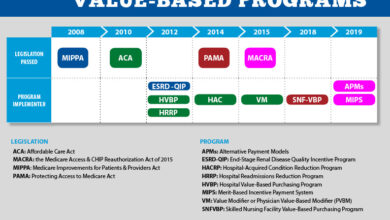
CMS CMMI, Poor Data, Health Equity, Payment Models
Cms cmmi poor data quality health equity payment models – CMS CMMI, poor data quality, health equity, and payment models: These four elements are inextricably linked, creating a complex challenge for the healthcare industry. We’re diving deep into how flawed data impacts equitable access to care and the effectiveness of value-based payment systems. Think inaccurate diagnoses leading to delayed treatment, biased algorithms perpetuating health disparities, and the struggle to measure true value in a system choked by unreliable information.
This is a story about data, equity, and the fight for better healthcare for everyone.
This post explores the multifaceted problem of poor data quality within the context of CMS regulations and CMMI frameworks. We’ll examine how inadequate data hinders the achievement of health equity goals under various payment models, and delve into practical strategies for improvement, including the role of technology and the crucial human element. Get ready for a journey into the heart of healthcare data – its challenges, its potential, and the vital need for change.
CMS and CMMI Frameworks in Healthcare
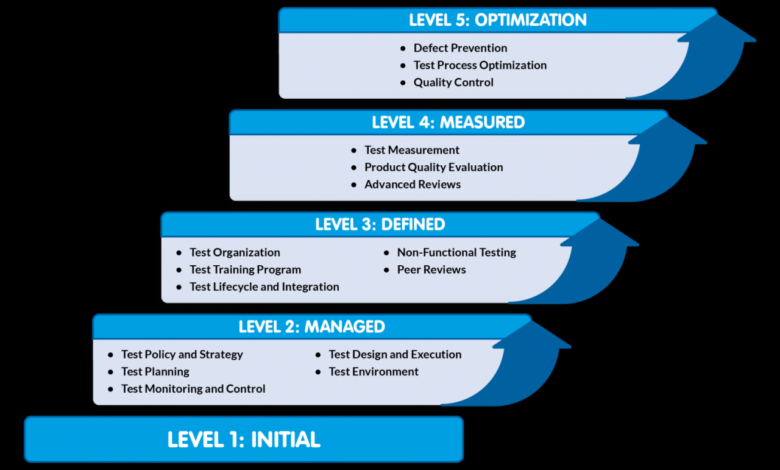
The intersection of CMS regulations and CMMI maturity levels presents a significant challenge for healthcare organizations striving for both regulatory compliance and operational excellence. While seemingly disparate, these frameworks share a common goal: improved performance and patient outcomes. Understanding their interplay is crucial for effective data management and achieving sustainable improvements in healthcare delivery.The impact of CMS regulations and CMMI maturity levels on data quality are intertwined.
CMS regulations, primarily focused on patient safety, billing accuracy, and data privacy (HIPAA), demand robust data management practices. Higher CMMI maturity levels, on the other hand, reflect a more mature and process-oriented approach to organizational management, including data management processes. Achieving a higher CMMI maturity level often directly translates to better data quality, as it necessitates improvements in processes like data collection, storage, analysis, and reporting.
However, the correlation isn’t always perfect, as a high CMMI level doesn’t automatically guarantee perfect data quality if the specific data quality requirements mandated by CMS aren’t adequately addressed.
Challenges in Achieving High CMMI Maturity and Superior Data Quality
Healthcare organizations face numerous hurdles in simultaneously achieving high CMMI maturity and superior data quality. These challenges often stem from legacy systems, siloed data, insufficient resources, and a lack of integrated data management strategies. For instance, updating legacy systems to meet both CMMI process requirements and CMS data reporting needs can be costly and time-consuming. Similarly, a lack of interoperability between different systems can hinder data integration and analysis, impacting both data quality and CMMI process assessments.
Furthermore, the complexity of healthcare data, coupled with stringent regulatory requirements, necessitates significant investment in skilled personnel and advanced technologies. Resistance to change within the organization, particularly from staff accustomed to existing (potentially inefficient) processes, can also impede progress.
Aligning CMS Compliance Requirements with CMMI Best Practices for Data Management
Aligning CMS compliance with CMMI best practices requires a strategic framework. This framework should begin with a comprehensive assessment of the organization’s current state, identifying gaps in both CMS compliance and CMMI maturity. This assessment should pinpoint specific data quality issues and their root causes. Next, a prioritized roadmap should be developed, outlining specific steps to address these gaps.
This roadmap needs to integrate CMS compliance requirements into the CMMI improvement process. For example, improvements in data collection processes (a key CMMI area) could directly address CMS requirements for accurate billing and patient safety reporting. Regular monitoring and evaluation are crucial, using metrics aligned with both CMS and CMMI goals. This framework necessitates a strong commitment to continuous improvement, with regular reviews and adjustments to the roadmap based on performance data.
Investing in training and education for staff on both CMS regulations and CMMI best practices is essential to ensure widespread understanding and buy-in. This integrated approach ensures that improvements made to enhance CMMI maturity also contribute directly to meeting CMS compliance requirements and improving overall data quality.
Poor Data Quality’s Impact on Healthcare
Poor data quality in healthcare has far-reaching and potentially devastating consequences. Inaccurate, incomplete, or inconsistent data undermines the very foundation of effective patient care, efficient operations, and meaningful research. The impact ripples across the entire healthcare ecosystem, affecting everyone from individual patients to healthcare systems and policymakers.
The consequences of poor data quality are not merely inconvenient; they can be life-threatening. Errors in patient records can lead to incorrect diagnoses, inappropriate treatments, and adverse drug events. Imagine a patient with a penicillin allergy whose record incorrectly states they have no allergies – the resulting allergic reaction could be fatal. This highlights the critical need for accurate and reliable data throughout the healthcare process.
Types of Data Quality Issues and Their Root Causes, Cms cmmi poor data quality health equity payment models
Several key data quality issues plague healthcare settings. These include inaccuracies (incorrect data entries), incompleteness (missing information), inconsistencies (contradictory data points across different systems), and lack of timeliness (delayed updates). Root causes are often multifaceted, encompassing human error, inadequate data entry processes, lack of standardized data formats, and integration challenges between disparate systems. For example, a physician’s hurried note-taking might lead to inaccurate medication dosages, while a lack of interoperability between an electronic health record (EHR) and a pharmacy system could result in a patient receiving the wrong medication.
Poor data governance and a lack of investment in data quality initiatives also play significant roles.
The CMS CMMI’s struggles with poor data quality directly impact the effectiveness of health equity payment models. Accurate data is crucial for fair allocation of resources, and the current situation highlights a significant challenge. This reminds me of the news about NextGen Healthcare exploring a sale, as reported by Reuters , which underscores how even large players in healthcare grapple with fundamental issues.
Ultimately, improving data quality is paramount to building truly equitable payment models within the CMS CMMI framework.
Impact of Poor Data Quality on Various Aspects of Healthcare
| Aspect of Healthcare | Impact of Poor Data Quality | Example | Consequences |
|---|---|---|---|
| Clinical Decision-Making | Incorrect diagnoses, inappropriate treatment plans, delayed care | A patient’s allergy information is missing from their record, leading to an adverse drug reaction. | Patient harm, increased healthcare costs, potential legal liability. |
| Billing and Reimbursement | Claims denials, delayed payments, revenue loss | Inconsistent coding practices result in inaccurate billing codes, leading to rejected insurance claims. | Financial instability for healthcare providers, reduced access to care for patients. |
| Public Health Surveillance | Inaccurate epidemiological data, ineffective public health interventions | Incomplete or inaccurate reporting of infectious disease cases hinders effective outbreak management. | Increased disease transmission, compromised public health. |
| Healthcare Research | Biased research findings, unreliable conclusions, wasted resources | Inconsistent data collection methods across different studies lead to flawed analyses and unreliable results. | Ineffective interventions, misallocation of research funds. |
Health Equity and Payment Models
Source: aprika.com
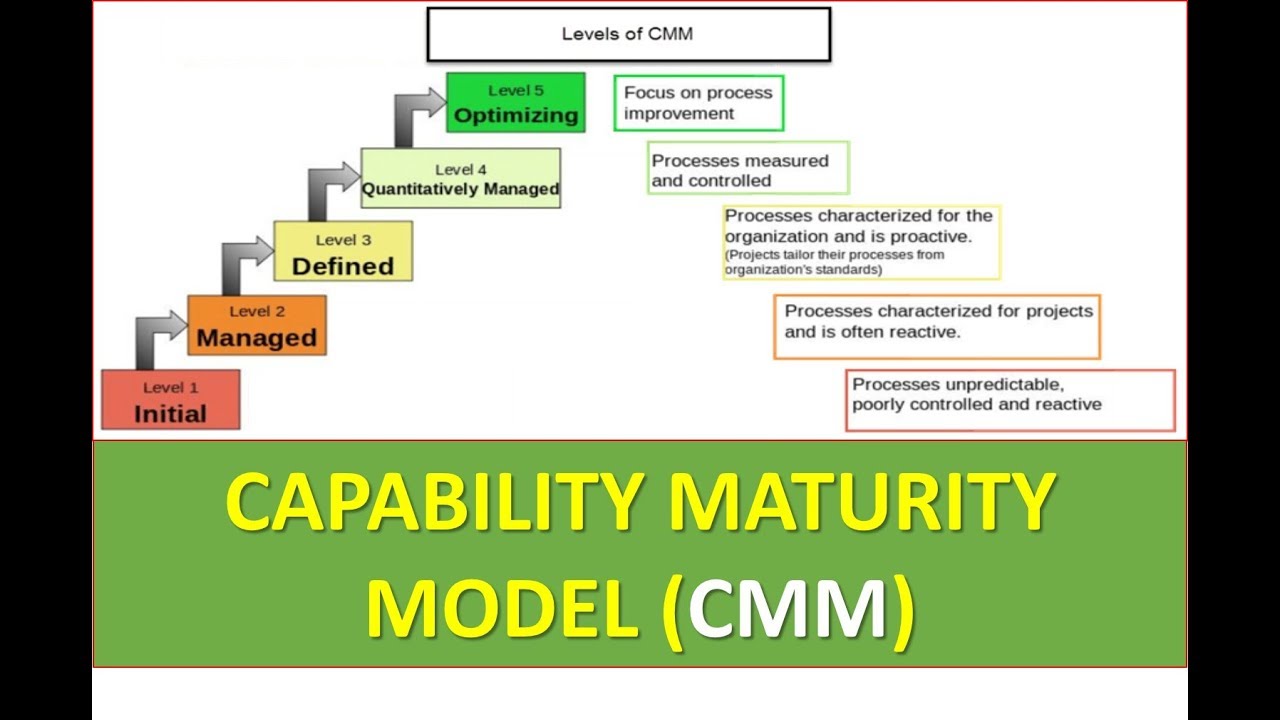
The intersection of data quality, health equity, and payment models is critical for achieving a truly equitable healthcare system. Accurate and unbiased data is essential for understanding and addressing health disparities, while effective payment models must incentivize providers to prioritize equitable care. Poor data quality, however, can undermine both understanding and incentivization, leading to the perpetuation of existing inequalities.Data quality significantly impacts the effectiveness of various payment models, particularly value-based care (VBC) models.
VBC models, which tie provider reimbursement to quality metrics and patient outcomes, rely heavily on accurate and complete data to measure performance and identify areas for improvement. If the data used to assess performance is flawed—reflecting existing biases or lacking information on specific populations—then VBC models may inadvertently penalize providers serving vulnerable populations or fail to adequately reward those delivering equitable care.
This can lead to a vicious cycle where disparities are not only perpetuated but potentially exacerbated.
Biased Data and the Perpetuation of Health Disparities
Inaccurate or biased data can significantly worsen existing health disparities. For example, if a dataset underrepresents minority populations, analyses based on that data will likely underestimate the prevalence of certain conditions or the effectiveness of specific interventions within those groups. This can lead to misallocation of resources, with less funding directed towards addressing the specific needs of underserved communities. Similarly, algorithms used in risk stratification or care management may perpetuate biases present in the training data, leading to unequal access to preventive services or timely interventions.
Consider a predictive model for readmission risk that uses socioeconomic status as a factor; if this data is incomplete or reflects historical biases in housing or employment opportunities, the model may unfairly flag patients from disadvantaged backgrounds for higher risk, even if their clinical profiles are otherwise similar to those of patients from more affluent backgrounds. This could lead to increased surveillance and potentially unnecessary interventions for one group, while others with similar clinical needs may be overlooked.
Strategies for Using Data to Improve Health Equity within Payment Models
Improving data quality is paramount to achieving health equity within various payment models. This requires a multi-pronged approach. Firstly, robust data collection protocols must be implemented to ensure comprehensive and representative data on all patient populations, paying special attention to underrepresented groups. Secondly, data governance frameworks need to be established to identify and mitigate biases within existing datasets.
The CMS CMMI program’s struggles with poor data quality directly impact the effectiveness of health equity payment models. Accurate data is crucial for fair allocation of resources, and current inconsistencies highlight a major challenge. This issue is further underscored by Walgreens’ recent move, as reported in this article walgreens raises healthcare segment outlook summit acquisition , showing the corporate sector’s growing interest in healthcare’s future.
Ultimately, improving data quality is essential for both private sector investment and the success of equitable payment models within the CMS CMMI framework.
This might involve employing statistical techniques to adjust for known biases or using alternative data sources to supplement existing ones. Thirdly, transparency and accountability mechanisms should be established to track progress in addressing health equity and hold stakeholders accountable for achieving equitable outcomes. For example, VBC programs could incorporate specific equity metrics into their performance measures, incentivizing providers to improve outcomes for all patient populations.
This could include targets for reducing disparities in access to care, quality of care, and health outcomes. Finally, investments in data infrastructure and analytical capabilities are crucial for enabling the effective use of data to drive improvements in health equity. This includes not only collecting better data but also developing the analytical capacity to interpret it effectively and use it to inform decision-making.
Data Quality Improvement Strategies
Improving data quality in healthcare is crucial for effective decision-making, accurate reimbursement, and ultimately, better patient care. A comprehensive strategy requires a multi-faceted approach encompassing data governance, validation, cleansing, and ongoing monitoring. This involves establishing clear responsibilities, implementing robust processes, and leveraging data visualization tools to identify and address weaknesses proactively.A comprehensive data quality improvement plan needs to be tailored to the specific needs and resources of each healthcare organization.
However, some common elements are essential for success.
Data Quality Improvement Plan
A robust data quality improvement plan should define specific, measurable, achievable, relevant, and time-bound (SMART) goals. For example, a hospital might aim to reduce the rate of missing patient allergy information by 20% within six months. This goal is then broken down into actionable steps, including staff training on proper data entry procedures, implementation of automated data validation checks, and regular audits of data completeness.
Key performance indicators (KPIs) should be tracked and reported regularly to monitor progress and identify areas needing further attention. Timelines should be established for each phase of the improvement plan, with milestones clearly defined and communicated to all stakeholders. For example, the initial training phase might be completed within one month, followed by implementation of data validation tools within two months, and regular audits commencing in month three.
Best Practices for Data Governance, Validation, and Cleansing
Effective data governance is paramount. This involves establishing clear roles and responsibilities for data management, defining data quality standards, and implementing processes for data validation and cleansing. Data governance also necessitates regular reviews and updates to ensure the plan remains relevant and effective.
- Data Governance: Establish a data governance council with representatives from various departments to oversee data quality initiatives. Define clear data ownership and accountability. Develop and implement data quality policies and procedures.
- Data Validation: Implement automated checks to ensure data accuracy and completeness at the point of entry. Use data profiling techniques to identify data anomalies and inconsistencies. Regularly review and update validation rules to reflect changes in data requirements.
- Data Cleansing: Develop a standardized process for identifying and correcting inaccurate, incomplete, or inconsistent data. Prioritize data cleansing efforts based on the criticality of the data and the potential impact of errors. Use data cleansing tools to automate the process where possible.
Data Visualization for Identifying and Addressing Data Quality Issues
Data visualization is a powerful tool for identifying patterns and trends in data that may indicate quality problems. By visually representing data, we can quickly spot outliers, inconsistencies, and missing values that might otherwise be missed in a spreadsheet.
- Example 1: A bar chart showing the number of patients with missing allergy information by department can highlight areas needing immediate attention. A high number of missing allergies in the emergency department might indicate a need for additional training and improved data entry procedures in that specific area.
- Example 2: A scatter plot showing the relationship between patient age and length of hospital stay can reveal unexpected patterns or outliers. A cluster of unusually long stays for a particular age group might indicate a data quality issue or a need for further investigation into patient care pathways.
- Example 3: A heatmap visualizing missing data across different data fields can quickly identify fields with consistently low completion rates. This allows for focused efforts on improving data capture in those specific areas. For instance, a heatmap showing consistently low completion rates for social determinant of health data fields could highlight the need for better data collection processes in this area.
Technology’s Role in Enhancing Data Quality
Source: blogspot.com
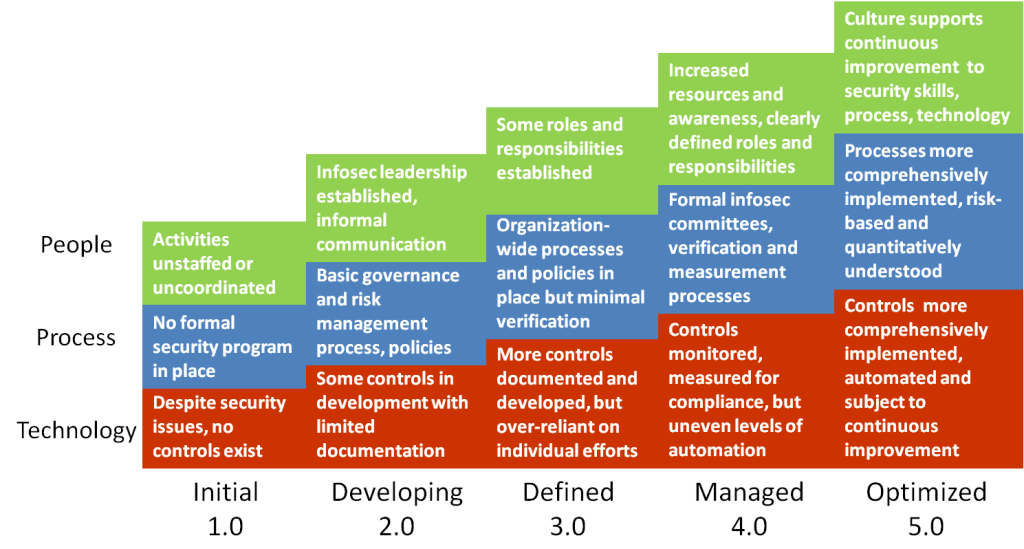
The healthcare industry is drowning in data, but ironically, often lacks the high-quality information needed for effective decision-making. Poor data quality leads to inaccurate diagnoses, inefficient treatments, and ultimately, poorer patient outcomes. Fortunately, advancements in technology offer powerful tools to address this critical challenge. Leveraging technologies like artificial intelligence (AI), machine learning (ML), and robust data analytics platforms can significantly improve data quality, leading to more equitable and effective healthcare systems.Technology offers a multifaceted approach to enhancing data quality.
AI and ML algorithms can be trained to identify patterns and anomalies within large datasets, flagging potential errors or inconsistencies that might otherwise go unnoticed by human reviewers. Data analytics tools provide the means to visualize and interpret this data, revealing trends and insights that can inform data quality improvement strategies. The combination of these technologies creates a powerful synergy for transforming raw data into reliable, actionable information.
AI and ML for Error Detection and Correction
AI and ML algorithms are particularly adept at identifying and correcting errors, inconsistencies, and biases within healthcare data. For example, ML models can be trained to detect inconsistencies in patient demographics, medical history, or billing codes. These models can compare data points against established norms and flag discrepancies for review. Similarly, AI can be used to identify potential biases in data collection, ensuring fairer and more equitable healthcare outcomes.
For instance, an AI system could identify if certain demographic groups are underrepresented in clinical trials or if specific diagnostic tools are less accurate for particular patient populations. Addressing these biases is crucial for ensuring health equity. Imagine an AI system analyzing medical imaging data and flagging potential misinterpretations due to subtle biases embedded within the algorithm itself – a timely detection that would improve accuracy and fairness.
Data Analytics for Identifying and Addressing Data Quality Issues
Data analytics plays a vital role in identifying and addressing root causes of poor data quality. By visualizing data trends, analysts can pinpoint areas where data quality is particularly poor. For example, data analytics can reveal patterns of missing data, inconsistencies in coding practices, or areas where data entry errors are most frequent. This information allows healthcare organizations to target their data quality improvement efforts effectively.
A specific example could be using data analytics to identify that a particular hospital department has a significantly higher rate of missing patient allergy information compared to other departments. This allows for focused training or system improvements in that specific area.
Implementing Data Quality Improvement Technology: A Flowchart
The successful implementation of data quality improvement technology requires a structured approach. The following flowchart illustrates a typical process:[Imagine a flowchart here. The flowchart would begin with “Initiate Project,” branching to “Needs Assessment” and “Technology Selection.” “Needs Assessment” would lead to “Data Mapping and Profiling,” which feeds into “Technology Selection.” “Technology Selection” branches to “Implementation” and “Training.” “Implementation” leads to “Data Validation and Testing,” which feeds into “Monitoring and Evaluation.” “Monitoring and Evaluation” feeds back into “Needs Assessment,” creating a continuous improvement cycle.
The final branch from “Monitoring and Evaluation” is “Deployment.”]The flowchart depicts a cyclical process, highlighting the importance of continuous monitoring and evaluation to ensure the technology remains effective and efficient in maintaining high data quality standards. Each stage involves specific actions and deliverables, ensuring a structured and systematic approach to implementing data quality improvements.
The Human Factor in Data Quality: Cms Cmmi Poor Data Quality Health Equity Payment Models
High-quality healthcare data isn’t just about sophisticated technology; it’s fundamentally about the people who collect, manage, and interpret it. The human element is crucial, impacting data accuracy, completeness, and ultimately, the effectiveness of healthcare delivery and equitable payment models. A strong focus on training, clear roles and responsibilities, and a supportive organizational culture are essential for achieving optimal data quality.The importance of a well-trained workforce cannot be overstated.
Inaccurate or incomplete data entry, stemming from insufficient knowledge or unclear procedures, can undermine the entire system. This impacts everything from billing accuracy to patient safety. For instance, incorrect coding of diagnoses can lead to inaccurate reimbursement, impacting both the provider and the patient’s access to care. Similarly, incomplete patient allergy information could have life-threatening consequences.
Training and Education for Data Quality Improvement
Effective training programs must go beyond basic data entry skills. They should encompass a comprehensive understanding of data standards, coding systems (like ICD-10 and CPT), and the implications of data errors. Regular refresher courses and updates on evolving regulations are also critical. Interactive training modules, hands-on exercises, and simulated scenarios can greatly enhance knowledge retention and practical application.
Furthermore, clear documentation of procedures and easily accessible reference materials should be readily available to all staff involved in data handling. This ensures consistency and minimizes the chance of errors due to ambiguity.
Healthcare Professionals’ Role in Ensuring Data Accuracy and Completeness
Healthcare professionals, from physicians and nurses to administrative staff, play a pivotal role in ensuring data accuracy and completeness. Physicians are responsible for accurate documentation of diagnoses, procedures, and patient history. Nurses contribute through meticulous recording of vital signs, medication administration, and patient observations. Administrative staff play a critical role in accurate data entry and maintaining the integrity of the electronic health record (EHR).
Regular audits and feedback mechanisms, combined with clear accountability for data quality, can significantly improve performance. For example, a hospital might implement a system where data entry errors are flagged and addressed promptly, with regular feedback provided to the staff involved.
Fostering a Culture of Data Quality
Cultivating a culture of data quality requires a multi-pronged approach. Leadership commitment is paramount, demonstrating the organization’s dedication to data integrity through both words and actions. This involves allocating sufficient resources for training, technology upgrades, and ongoing quality improvement initiatives. Open communication channels and a non-punitive environment are essential for encouraging staff to report errors and participate in improvement efforts.
Regular feedback sessions, team meetings dedicated to data quality discussions, and recognition programs for individuals and teams who consistently demonstrate excellence in data management can further strengthen this culture. This creates a collaborative environment where data quality is viewed not just as a task, but as a shared responsibility crucial to patient care and organizational success.
Future Trends in Data Quality and Health Equity
The convergence of advanced technologies, evolving payment models, and a growing emphasis on health equity is reshaping the healthcare landscape. This necessitates a profound shift in how we approach data quality, moving beyond simple accuracy to encompass completeness, timeliness, and relevance in the context of social determinants of health. The future of data quality is inextricably linked to the future of equitable healthcare access and outcomes.The coming years will witness a significant acceleration in the adoption of data quality management practices that are proactive, predictive, and patient-centered.
This shift will involve a move away from reactive, error-correction approaches to a more holistic system that embeds data quality principles into every aspect of healthcare operations, from data collection to analysis and reporting. This will require substantial investment in both technology and workforce development.
Artificial Intelligence and Machine Learning in Data Quality Management
AI and machine learning (ML) are poised to revolutionize data quality management. These technologies can automate many aspects of data cleaning, validation, and standardization, significantly reducing the burden on human resources. For example, ML algorithms can identify and flag inconsistencies or errors in patient records far more efficiently than manual review, allowing for quicker correction and improved data integrity.
Furthermore, AI can predict potential data quality issues before they arise, enabling proactive interventions and preventing costly downstream problems. The application of AI to health equity initiatives, like identifying biases in algorithms or predicting health disparities, is also a crucial development. Imagine a system where AI proactively identifies patients at high risk of developing a particular condition based on their socioeconomic status and other relevant factors, allowing for timely interventions and preventative care.
Interoperability and Data Sharing
Enhanced data interoperability is crucial for improving data quality and promoting health equity. Seamless data exchange between different healthcare systems, providers, and payers allows for a more comprehensive view of a patient’s health journey, reducing data silos and improving the accuracy of information. This is particularly important for patients who receive care from multiple providers or across different settings.
For instance, a patient with chronic conditions might receive care from a primary care physician, a specialist, and a hospital. With interoperable systems, all these providers can access the same complete and accurate data, ensuring continuity of care and preventing potential errors or inconsistencies. However, robust data governance and privacy protocols are essential to ensure ethical and responsible data sharing.
The CMS CMMI’s struggles with poor data quality directly impact the effectiveness of health equity payment models. Improving data analysis is crucial, and I was intrigued to learn about how Google Cloud Healthcare, as discussed in this insightful article on google cloud healthcare amy waldron generative AI , is using AI to address similar challenges. This could offer valuable solutions for cleaning and analyzing the messy datasets hindering fair and effective health equity initiatives within the CMS CMMI framework.
The Rise of Real-World Evidence (RWE)
The increasing use of RWE in clinical research and healthcare decision-making highlights the importance of high-quality data. RWE, which is derived from various sources such as electronic health records, claims data, and wearable sensors, can provide valuable insights into the effectiveness and safety of healthcare interventions in real-world settings. The quality of this data is paramount, as flawed or incomplete data can lead to inaccurate conclusions and potentially harmful healthcare decisions.
The future will likely see more sophisticated methods for collecting, validating, and analyzing RWE, ensuring its reliability and relevance for improving health outcomes, particularly in under-served communities. A specific example would be leveraging RWE to assess the effectiveness of a new diabetes management program in a low-income neighborhood, using data from local clinics and community health centers.
A Future Healthcare System with Exemplary Data Quality and Equitable Access
Imagine a future where every individual has a comprehensive, accurate, and readily accessible digital health record that seamlessly integrates with all aspects of their care. This record includes not only clinical data but also social determinants of health, such as housing stability, food security, and access to transportation. AI-powered tools analyze this data to identify potential health risks and proactively suggest personalized interventions.
Providers have real-time access to this information, allowing for coordinated and holistic care. Payment models incentivize equitable access and high-quality care, rewarding providers for improving health outcomes in underserved communities. This system leverages advanced analytics to identify and address health disparities, ensuring that all individuals have equal opportunities to achieve optimal health, regardless of their background or socioeconomic status.
This isn’t just about collecting data; it’s about using data to create a truly equitable and effective healthcare system.
Last Recap
Source: embracethered.com
Ultimately, improving data quality in healthcare isn’t just about fixing numbers; it’s about building a fairer, more effective system. By understanding the interconnectedness of CMS requirements, CMMI best practices, health equity, and payment models, we can begin to address the root causes of poor data and pave the way for a future where everyone has access to high-quality, equitable care.
The journey is complex, but the potential rewards – better health outcomes for all – are immeasurable. Let’s start building a better data-driven healthcare system, one accurate record at a time.
Essential FAQs
What are the legal implications of using biased data in healthcare?
Using biased data can lead to legal challenges related to discrimination and violations of patient rights. Regulations like HIPAA and the Affordable Care Act impose strict requirements for data privacy and non-discrimination.
How can small healthcare organizations afford to implement data quality improvement initiatives?
Small organizations can leverage cost-effective solutions like cloud-based data management tools, prioritize data quality training for staff, and focus on addressing the most critical data quality issues first. Grants and partnerships can also be explored.
What are some examples of data visualization tools useful for identifying data quality problems?
Tools like Tableau, Power BI, and even simpler spreadsheet software can be used to create charts and dashboards that highlight inconsistencies, outliers, and missing data points, making it easier to identify areas needing improvement.