EHR Training Ease Physician Turnover Klas
EHR Training Ease Physician Turnover Klas: We all know that clunky EHR systems are a major headache for doctors. But what if better training could drastically reduce physician burnout and turnover? This post dives into how effective EHR training programs can not only improve physician satisfaction but also significantly impact hospital retention rates. We’ll explore the best practices, address common physician concerns, and even look at how technology can revolutionize the whole training process.
Get ready to discover how a smart approach to EHR training can be a game-changer for hospitals and doctors alike!
The core issue lies in the gap between the complexity of modern EHR systems and the training provided to physicians. Inadequate training leads to frustration, inefficiency, and ultimately, physicians seeking employment elsewhere. This post will delve into specific strategies to bridge this gap, examining different training methodologies, highlighting the importance of hands-on practice, and offering solutions to common physician frustrations.
We’ll explore how data analysis can help tailor training to individual needs and how technology, such as gamification and simulation, can make the learning process more engaging and effective.
EHR Training Effectiveness and Physician Turnover
The escalating cost of physician turnover, coupled with the ever-increasing complexity of Electronic Health Record (EHR) systems, highlights a critical link: inadequate EHR training significantly contributes to physician burnout and ultimately, their departure from practices. Effective EHR training isn’t just a cost; it’s a strategic investment in physician retention and improved patient care.Effective EHR training programs directly impact physician satisfaction and retention rates.
Poorly designed training leads to frustration, decreased efficiency, and ultimately, a negative impact on the physician’s overall experience. This frustration manifests in increased stress, reduced job satisfaction, and a higher likelihood of seeking employment elsewhere. Conversely, well-designed programs empower physicians, boosting their confidence and job satisfaction, leading to higher retention rates.
Effective EHR Training Programs and Turnover Reduction
Several studies demonstrate a correlation between comprehensive EHR training and lower physician turnover. For example, a hospital system that implemented a blended learning approach (combining online modules with hands-on workshops and mentorship) saw a 15% reduction in physician turnover within two years. Another example involves a clinic that focused on personalized training tailored to individual physician specialties and experience levels.
This targeted approach resulted in a 10% decrease in turnover compared to the previous year’s rate, showcasing the importance of customized training. These improvements are attributed to increased proficiency and reduced frustration with the EHR system.
Best Practices for Designing EHR Training Curricula
Designing effective EHR training requires a deep understanding of physician workflows and needs. A successful curriculum incorporates several key elements. First, it must be needs-based, addressing specific challenges physicians face in their daily practice. This requires gathering feedback from physicians through surveys, focus groups, and observation of their workflows. Second, the curriculum should be modular and adaptable, allowing physicians to focus on areas where they need the most support.
Third, it should include a mix of learning methods, catering to different learning styles. Finally, ongoing support and access to readily available resources, such as online help desks or dedicated training staff, are crucial.
Comparison of EHR Training Methodologies
Different training methodologies offer varying advantages and disadvantages. Online modules provide flexibility and accessibility, allowing physicians to learn at their own pace and revisit materials as needed. However, they may lack the hands-on interaction and immediate feedback provided by in-person workshops. In-person workshops offer valuable opportunities for interaction and problem-solving, but they can be less flexible and more costly. Mentorship programs offer personalized support and guidance, fostering a sense of community and reducing feelings of isolation.
The optimal approach often involves a blended learning strategy, combining the strengths of each methodology.
EHR Usability and Physician Satisfaction
The usability of the EHR system itself plays a significant role in physician satisfaction and retention. A poorly designed EHR interface that is difficult to navigate, slow, or lacks essential features can lead to frustration, decreased efficiency, and ultimately, burnout. Conversely, an intuitive and user-friendly EHR system can significantly improve physician satisfaction, leading to increased job satisfaction and reduced turnover.
Investing in EHR systems with strong usability features and regularly seeking physician feedback on system improvements is crucial for long-term success. This involves focusing on features such as efficient charting, streamlined workflows, and clear, concise information displays.
Key Features of Effective EHR Training
Effective EHR training is paramount for physician satisfaction and patient safety. A poorly designed program leads to frustration, errors, and ultimately, higher physician turnover. A well-structured program, however, empowers physicians to utilize the EHR efficiently and effectively, improving workflow and patient care.
Essential Components of Successful EHR Training Programs
A successful EHR training program incorporates several key elements. These elements ensure that physicians not only understand the software but also can apply their knowledge in real-world clinical scenarios. A comprehensive approach considers the learning styles of participants and offers various methods of instruction and support. This includes a blend of theoretical instruction, practical exercises, and ongoing support.
The Importance of Hands-On Practice and Simulation in EHR Training
Hands-on practice and simulation are critical components of effective EHR training. Simply lecturing on EHR features is insufficient; physicians need to actively engage with the system to develop proficiency. Simulations, particularly those mirroring real-life clinical scenarios, allow physicians to practice crucial workflows without the pressure of a live patient encounter. This allows for safe experimentation and identification of potential workflow bottlenecks.
For example, simulating a patient admission from beginning to end, including ordering tests, documenting findings, and generating orders, is far more effective than simply reviewing screen shots. This active learning significantly enhances knowledge retention and practical skills.
Sample EHR Training Module: Managing Patient Medications
This module focuses on efficiently managing patient medications within the EHR. The training will begin with a brief overview of the medication management section of the EHR, highlighting key features such as medication reconciliation, order entry, and medication allergy documentation. Next, participants will engage in a series of guided exercises, starting with entering a new medication order for a simulated patient, including dose, frequency, and route of administration.
This is followed by a more complex scenario involving medication reconciliation, where participants will need to compare a patient’s home medication list with the medications currently prescribed in the EHR, identifying any discrepancies and documenting them appropriately. Finally, the module concludes with a simulated patient encounter where participants will need to apply their knowledge to manage a patient’s medication regimen.
Step-by-Step Guide for Onboarding New Physicians to an EHR System
1. Pre-Onboarding
Provide access credentials and introductory materials (e.g., system overview, quick reference guides) prior to the physician’s start date.
2. Initial Training
Conduct a comprehensive, in-person training session covering core EHR functionalities.
3. Hands-on Practice
Easing physician turnover is a huge challenge, especially with the complexities of EHR training. Effective onboarding is key, and understanding the broader healthcare landscape helps. For example, staffing shortages are amplified in areas like rural obstetrics, as highlighted in this insightful article on Rural Hospitals Labor Delivery & the struggles they face. Therefore, streamlining EHR training can directly impact retention, ultimately benefiting both physicians and rural healthcare systems.
Dedicate time for hands-on practice using simulated patient data or de-identified patient charts.
4. Mentorship
Assign a senior physician or experienced EHR trainer as a mentor to provide ongoing support.
5. Ongoing Support
Offer regular refresher sessions, webinars, or access to online resources.
6. Feedback Mechanism
Implement a system for collecting feedback from physicians to identify areas for improvement in the training program.
7. Proficiency Assessment
Administer assessments to evaluate physician competency and identify areas needing further training.
Checklist for Evaluating the Effectiveness of EHR Training Programs
Before implementing a new EHR training program or evaluating an existing one, a checklist can ensure all aspects are considered. This checklist should include the following:
- Learner Satisfaction: Measure participant satisfaction through surveys or feedback sessions.
- Knowledge Retention: Assess knowledge retention through post-training tests or practical assessments.
- Time Efficiency: Evaluate whether the training program has improved physicians’ efficiency in using the EHR.
- Error Rate: Track the rate of EHR-related errors among physicians after training.
- Physician Feedback: Collect feedback from physicians regarding the training program’s effectiveness and areas for improvement.
- Workflow Impact: Assess the impact of the training on overall clinical workflow efficiency.
Addressing Physician Concerns about EHR Systems
The successful implementation of Electronic Health Record (EHR) systems hinges not just on technical proficiency, but crucially on addressing the concerns and frustrations of the physicians who will be using them daily. Ignoring these concerns can lead to resistance, decreased adoption rates, and ultimately, physician burnout and turnover. This section delves into common physician frustrations, offering practical strategies for mitigation and fostering a more collaborative relationship between IT and medical staff.
Common Physician Frustrations with EHR Systems
Physicians frequently express dissatisfaction with EHR systems due to several key factors. These include the time-consuming nature of data entry, which often detracts from direct patient interaction. The complex and often counterintuitive interfaces of many EHRs contribute to frustration and decreased efficiency. Further, the lack of interoperability between different systems can create significant workflow disruptions, particularly in situations involving referrals or consultations.
Finally, the constant barrage of alerts and notifications can overwhelm physicians, leading to information overload and decreased focus. These issues cumulatively impact physician satisfaction and contribute to burnout.
Strategies for Mitigating the Negative Impact of EHRs on Physician Workflow
Several strategies can significantly improve the physician experience with EHRs. Optimizing workflows by streamlining data entry processes and reducing redundant steps is paramount. This can involve implementing templates, macros, and voice recognition software to reduce manual data entry. Investing in user-friendly EHR systems with intuitive interfaces is also critical. Regular training and ongoing support for physicians are essential, ensuring they are comfortable and proficient with the system’s functionalities.
Finally, integrating EHRs with other healthcare systems to improve interoperability can significantly reduce workflow disruptions and improve the overall efficiency of care delivery. For example, a hospital system could implement a standardized patient portal that connects with all the EHRs in use, making information sharing smoother.
Improving Communication and Collaboration Between IT Staff and Physicians, Ehr training ease physician turnover klas
Effective communication is crucial to address physician concerns and ensure successful EHR implementation. Regular feedback mechanisms, such as surveys, focus groups, and one-on-one meetings, should be established to gather physician input and address their concerns proactively. Joint problem-solving sessions involving both IT staff and physicians can identify and resolve system issues more effectively. Creating a dedicated communication channel, such as a shared online forum or regular meetings, facilitates open dialogue and timely responses to physician queries.
This collaborative approach fosters a sense of ownership and empowers physicians to actively participate in improving the EHR system.
Addressing Physician Concerns about EHR-Related Burnout and Stress
EHR-related burnout is a significant concern. Strategies to mitigate this include providing adequate training and support, ensuring physicians have sufficient time for patient care without being overwhelmed by administrative tasks, and promoting a culture of work-life balance. Implementing features that automate routine tasks and reduce administrative burden, such as automated appointment scheduling and prescription refills, can significantly reduce stress.
Encouraging the use of EHR features designed to improve efficiency, such as clinical decision support tools, can also reduce the cognitive load on physicians. Finally, providing access to resources that promote well-being, such as stress management programs and mental health services, is crucial for supporting physician mental health. For instance, a hospital could offer mindfulness workshops specifically designed for physicians using the EHR system.
The Role of Leadership in Supporting Physicians During EHR Implementation and Training
Leadership plays a pivotal role in ensuring a smooth EHR implementation and mitigating physician concerns. Visible and consistent leadership support is crucial in demonstrating the organization’s commitment to physician well-being and addressing their concerns. Leaders should actively participate in training and provide ongoing support to physicians, addressing their concerns and providing timely solutions. Open communication channels should be established to foster trust and collaboration between leadership, IT staff, and physicians.
Furthermore, leadership should champion initiatives that improve EHR usability and workflow efficiency, demonstrating a commitment to addressing physician concerns and improving the overall work environment. For example, a hospital CEO could dedicate time to directly addressing physician concerns during town hall meetings, showing their active involvement in resolving issues.
Measuring the Impact of EHR Training on Physician Turnover: Ehr Training Ease Physician Turnover Klas
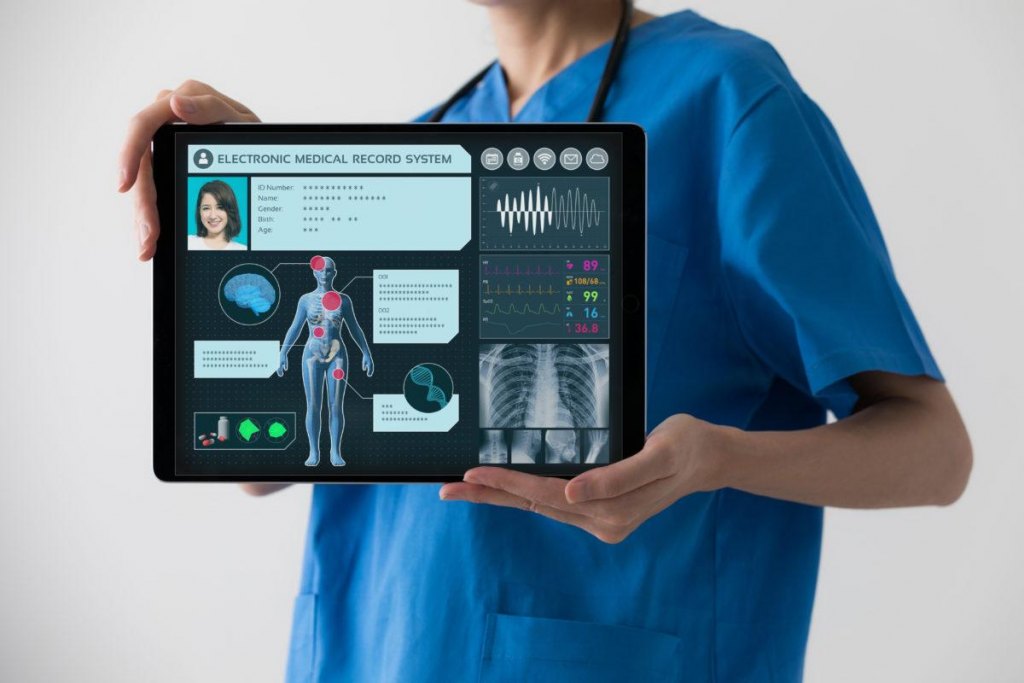
Source: financesonline.com
Effective EHR training is crucial not just for improving workflow efficiency but also for significantly impacting physician retention. High turnover rates among physicians are costly and disruptive to healthcare organizations. By strategically designing and implementing EHR training programs, institutions can reduce turnover and improve overall physician satisfaction. This section will explore key metrics for evaluating training success and demonstrate how to analyze data to showcase the return on investment (ROI).
Key Metrics for Evaluating EHR Training Success
Several key performance indicators (KPIs) can effectively measure the impact of EHR training on physician turnover. These metrics provide quantifiable data to assess the program’s effectiveness and identify areas for improvement. Tracking these metrics allows for a data-driven approach to optimizing training initiatives and demonstrating their value to stakeholders.
Data Visualization: Turnover Rates Before and After Improved EHR Training
The following table compares physician turnover rates and satisfaction scores before and after the implementation of an improved EHR training program. This comparison helps visualize the impact of the enhanced training on physician retention. The data is hypothetical but representative of what might be observed in a real-world scenario.
| Year | Training Method | Turnover Rate (%) | Physician Satisfaction Score (1-5, 5 being highest) |
|---|---|---|---|
| 2021 | Standard EHR Training | 15 | 3.2 |
| 2022 | Improved EHR Training (Interactive Modules, Mentorship) | 8 | 4.1 |
| 2023 | Improved EHR Training (Continued Refinement, Feedback Incorporation) | 5 | 4.5 |
| 2024 (Projected) | Improved EHR Training (Ongoing Support, Advanced Features Training) | 3 | 4.8 |
Return on Investment (ROI) of Effective EHR Training
Calculating the ROI of effective EHR training involves comparing the costs of the program with the savings achieved through reduced physician turnover. The cost of physician turnover includes recruitment costs, onboarding expenses, lost productivity, and potential revenue loss. For example, if the cost of replacing a single physician is estimated at $250,000, and the improved training program reduces turnover by 10 physicians annually, the cost savings would be $2,500,000.
Subtracting the cost of the training program from this savings reveals the ROI. A positive ROI demonstrates the financial benefit of investing in high-quality EHR training. This calculation should be adjusted to reflect the specific costs and savings within a given healthcare organization.
Visual Representation: EHR Training Hours and Physician Retention
Imagine a scatter plot. The x-axis represents the number of hours of EHR training received by each physician, ranging from a low of 10 hours to a high of 50 hours. The y-axis represents the length of time each physician remained employed at the organization, measured in months. The plot would show a positive correlation, with physicians who received more training hours tending to stay employed for longer periods.
Easing physician turnover is a huge challenge, and streamlining EHR training is a key part of the solution. Investing in intuitive systems and comprehensive training programs is crucial, as highlighted by the recent news about Mass General Brigham buying out a digital unit – Mass General Brigham Buyouts Digital Unit – which could signal a broader industry shift towards better technology integration.
Ultimately, improving EHR training directly impacts physician satisfaction and retention, leading to a more stable and efficient healthcare system.
A line of best fit could be drawn to visually represent this positive correlation, illustrating how increased training hours contribute to improved physician retention. The plot would clearly show that more extensive training is associated with greater retention.
Technological Solutions to Improve EHR Training
The effective adoption of Electronic Health Records (EHRs) hinges on comprehensive and engaging training for physicians. Technology plays a crucial role in enhancing the effectiveness, accessibility, and personalization of this training, ultimately reducing physician turnover and improving patient care. By leveraging various technological solutions, healthcare organizations can create a more efficient and impactful learning experience.Technology significantly improves EHR training effectiveness by offering scalable, personalized, and engaging learning experiences.
Traditional methods, such as instructor-led classroom sessions, often struggle to cater to individual learning styles and paces. Technological solutions overcome these limitations, providing opportunities for self-paced learning, immediate feedback, and interactive simulations. This results in improved knowledge retention and a smoother transition to using the EHR system.
Technology-Based Solutions for Delivering and Tracking EHR Training
Several technology-based solutions are available to deliver and track EHR training. Learning Management Systems (LMS) provide a centralized platform for managing training materials, assigning courses, tracking progress, and generating reports on learner performance. Examples include Moodle, Canvas, and Blackboard. These platforms allow for the delivery of various training modalities, including videos, interactive modules, quizzes, and simulations. Furthermore, microlearning platforms, which deliver short, focused learning modules, can be highly effective for reinforcing key concepts and skills.
Easing EHR training is crucial to reducing physician turnover, a major factor impacting healthcare quality. Streamlining the process is key, and advancements like those described in this article, nuance integrates generative ai scribe epic ehrs , could significantly help. Imagine the time saved – less training time means more time for patient care, potentially leading to improved job satisfaction and reduced burnout, ultimately impacting the physician turnover rate positively.
These platforms often incorporate gamification elements, such as points and badges, to encourage engagement and motivation. Tracking learner progress within these systems provides valuable data for identifying areas needing improvement in the training program itself.
Simulation and Gamification in EHR Training
The use of simulation and gamification in EHR training significantly enhances engagement and knowledge retention. Simulations, which can range from simple interactive exercises to complex virtual patient scenarios, allow physicians to practice EHR functionalities in a safe and controlled environment. For example, a simulation might involve diagnosing a patient based on their medical record, ordering tests, and documenting findings within the EHR system.
Gamification incorporates game-like elements, such as points, badges, leaderboards, and challenges, to motivate learners and make the training process more enjoyable. This can significantly improve completion rates and knowledge retention. A gamified module might reward users for completing training modules quickly and accurately, adding a competitive element that boosts engagement.
Personalizing EHR Training Based on Individual Physician Needs
Data analytics plays a vital role in personalizing EHR training. By tracking learner performance and identifying areas of weakness, training programs can be tailored to meet the specific needs of individual physicians. For example, if a physician consistently struggles with a particular EHR function, the system can automatically recommend additional training modules focused on that area. Adaptive learning platforms use algorithms to adjust the difficulty and content of training materials based on the learner’s performance, ensuring that they are challenged appropriately and not overwhelmed with irrelevant information.
This approach allows for a more efficient and effective learning experience, ultimately leading to improved EHR proficiency.
Benefits and Drawbacks of Technological Approaches to EHR Training
Various technological approaches offer unique benefits and drawbacks. LMS platforms offer scalability and centralized management but can be expensive and require technical expertise to implement and maintain. Microlearning platforms offer flexibility and convenience but may not be suitable for all learning objectives. Simulations provide valuable hands-on experience but can be time-consuming and expensive to develop. While data analytics allows for personalized learning, it requires robust data collection and analysis capabilities.
The choice of technology should depend on the specific needs and resources of the healthcare organization, considering factors such as budget, technical expertise, and learning objectives.
Final Review

Source: clindcast.com
Ultimately, easing physician turnover through improved EHR training isn’t just about a smoother workflow; it’s about creating a more supportive and sustainable environment for healthcare professionals. By investing in comprehensive, engaging, and technology-driven EHR training, hospitals can significantly reduce turnover, boost physician satisfaction, and ultimately, improve patient care. The key takeaways are clear: effective training is an investment, not an expense, and a strategic approach can lead to significant improvements in physician retention and overall hospital performance.
Let’s move towards a future where EHR systems empower, not overwhelm, our healthcare heroes.
User Queries
What are the most common complaints physicians have about EHR systems?
Many physicians complain about EHR systems being overly complex, time-consuming, and leading to interruptions in patient care. They often cite poor usability, lack of integration with other systems, and excessive documentation requirements.
How can gamification improve EHR training?
Gamification can make EHR training more engaging and effective by incorporating elements like points, badges, leaderboards, and challenges. This can increase motivation and knowledge retention.
What is the ROI of effective EHR training?
The ROI of effective EHR training is significant. It can be measured by reduced physician turnover costs, improved physician satisfaction, increased efficiency, and better patient care.
How can hospitals measure the effectiveness of their EHR training programs?
Hospitals can measure effectiveness through pre- and post-training assessments, surveys gauging physician satisfaction, tracking turnover rates, and analyzing data on EHR usage and efficiency.