Expanded Federal Safety Net COVID-19 & Improved Health Access
Expanded federal safety net covid 19 improved health access – Expanded federal safety net COVID-19 improved health access – that’s a mouthful, right? But it speaks volumes about the massive upheaval and subsequent response to the pandemic. We’re diving into the heart of the matter: how emergency relief packages dramatically reshaped healthcare access, unemployment benefits, and food security. This wasn’t just about handing out checks; it was a societal experiment in crisis management, revealing both triumphs and shortcomings.
Get ready for a look at the programs, the impact, and the lingering questions we still grapple with today.
From the initial shock of lockdowns to the slow, uneven recovery, the pandemic exposed deep cracks in our social safety net. The massive influx of federal funds, while intended to alleviate suffering, created a complex tapestry of successes and failures. We’ll examine specific programs, their effectiveness, and the lasting effects on vulnerable populations. We’ll also explore the crucial role of telehealth and the persistent inequalities that continue to plague our healthcare system.
The Expansion of the Federal Safety Net During COVID-19
Source: mdpi-res.com
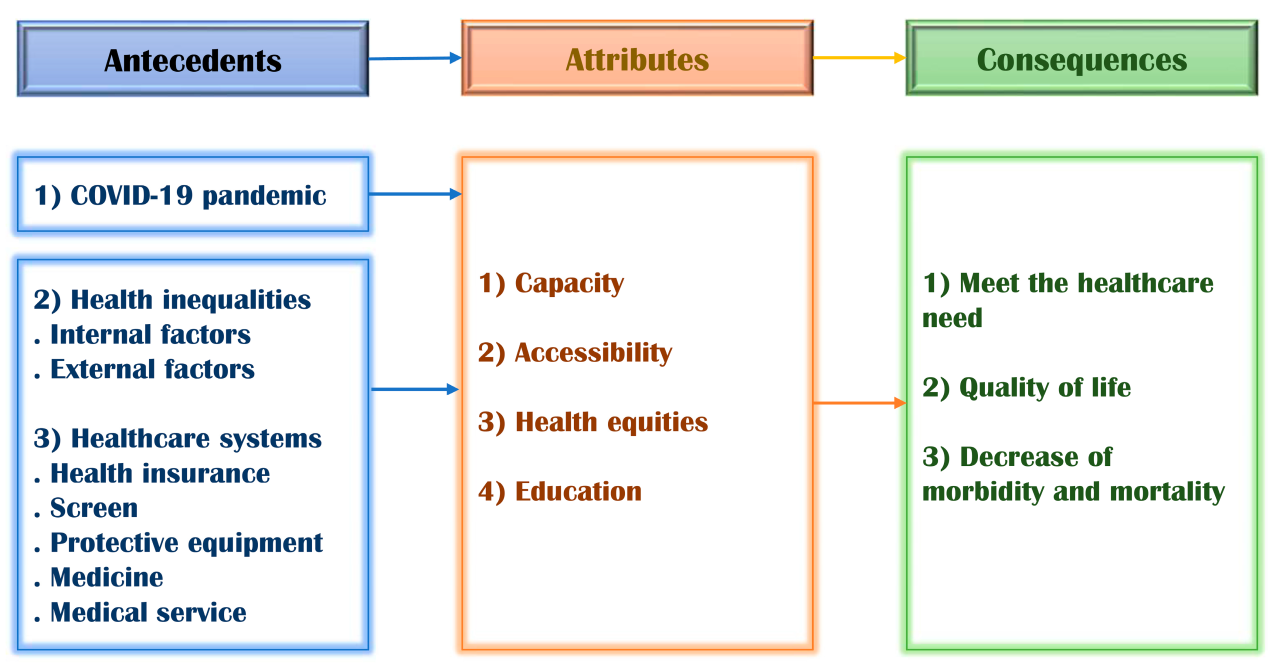
The COVID-19 pandemic presented an unprecedented challenge to the United States, necessitating a dramatic expansion of the federal safety net to protect millions of Americans from economic hardship and health crises. Several massive relief packages were enacted, significantly altering the landscape of social support programs and impacting access to essential services like healthcare, food, and unemployment benefits. This expansion, while largely successful in mitigating immediate suffering, also highlighted existing inequalities and the complexities of rapidly deploying large-scale social programs.The key provisions of these relief packages aimed to address the immediate and widespread economic fallout caused by the pandemic.
The expanded federal safety net during COVID-19 undeniably improved health access for many, but questions remain about long-term sustainability. This makes news about major healthcare systems like Mass General Brigham’s strategic moves, such as their recent buyout of a digital unit, Mass General Brigham Buyouts Digital Unit , all the more interesting. Will these kinds of investments ultimately strengthen or weaken the overall ability to provide care to those who need it most under a less-expanded safety net?
Lockdowns and business closures led to massive job losses, while the healthcare system struggled to cope with a surge in COVID-19 patients. The federal government responded with a series of legislative actions, including the Coronavirus Aid, Relief, and Economic Security (CARES) Act, the Consolidated Appropriations Act, and the American Rescue Plan Act. These acts provided direct financial assistance to individuals and businesses, expanded unemployment benefits, increased funding for healthcare programs, and boosted food assistance initiatives.
Impact on Healthcare Access
The expansion of the federal safety net significantly improved healthcare access for many Americans. The CARES Act, for example, provided substantial funding for testing and treatment of COVID-19, expanded telehealth coverage under Medicare and Medicaid, and increased funding for the Public Health Service. The American Rescue Plan Act further expanded access to affordable healthcare by increasing subsidies for health insurance purchased through the Affordable Care Act (ACA) marketplaces.
This led to a notable increase in the number of Americans with health insurance coverage, reducing financial barriers to accessing essential medical care, including preventive services and treatment for chronic conditions. Increased funding also supported the development and distribution of COVID-19 vaccines, a crucial step in mitigating the pandemic’s impact.
Impact on Food Assistance
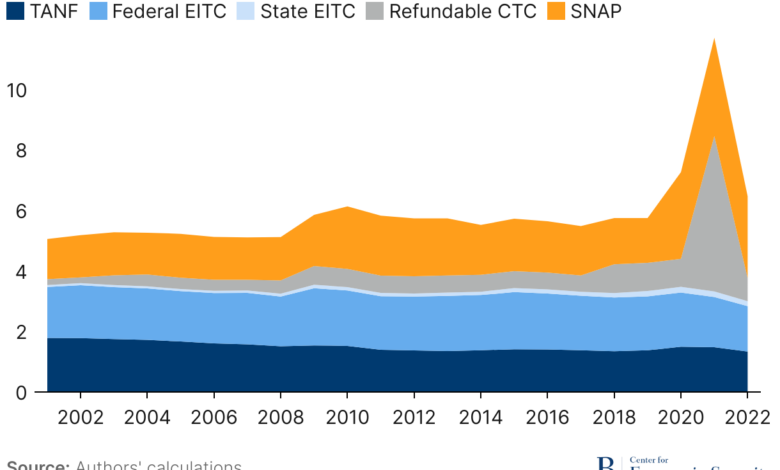
The pandemic exacerbated existing food insecurity issues, leading to a substantial increase in demand for food assistance programs. The relief packages responded by increasing benefits and expanding eligibility for programs like the Supplemental Nutrition Assistance Program (SNAP), formerly known as food stamps. Increased funding allowed states to provide larger benefit amounts to SNAP recipients and temporarily eased eligibility requirements, ensuring that more families had access to nutritious food during a time of economic uncertainty.
Additionally, funding was allocated to support food banks and other community-based organizations that provide emergency food assistance, bolstering their capacity to meet the surging demand.
Impact on Unemployment Benefits
The unprecedented job losses caused by the pandemic necessitated a significant expansion of unemployment insurance benefits. The CARES Act created the Pandemic Unemployment Assistance (PUA) program, providing benefits to individuals who were not typically eligible for traditional unemployment insurance, such as self-employed workers and gig economy workers. It also added $600 per week in federal unemployment benefits to existing state programs, providing crucial financial support to millions of unemployed Americans.
The extension and modification of these programs through subsequent relief packages helped to alleviate the economic hardship faced by many during the pandemic’s early stages. However, the complexities of administering these expanded programs, along with varying state-level implementations, presented significant challenges.
Key Programs Expanded or Implemented During COVID-19
The following table details some of the key programs expanded or implemented during the COVID-19 pandemic:
| Program Name | Funding Source | Target Population | Key Benefits |
|---|---|---|---|
| Supplemental Nutrition Assistance Program (SNAP) | CARES Act, Consolidated Appropriations Act, American Rescue Plan Act | Low-income individuals and families | Increased benefit amounts, expanded eligibility |
| Pandemic Unemployment Assistance (PUA) | CARES Act | Self-employed workers, gig workers, and others ineligible for traditional unemployment insurance | Weekly unemployment benefits |
| Coronavirus Aid, Relief, and Economic Security (CARES) Act Direct Payments | CARES Act | Eligible individuals and families | Direct cash payments |
| Affordable Care Act (ACA) Subsidies | American Rescue Plan Act | Individuals purchasing health insurance through the ACA marketplaces | Increased subsidies, lowering the cost of health insurance |
Improved Health Access
The expansion of the federal safety net during the COVID-19 pandemic significantly impacted healthcare access, particularly for vulnerable populations. While the increased funding and broadened eligibility criteria aimed to improve health outcomes, the reality was a complex interplay of successes and challenges. This section explores the impact of these changes on mortality rates and preventative care access, highlighting the obstacles encountered in reaching underserved communities and the crucial role of telehealth in bridging the healthcare gap.The expanded safety net demonstrably improved access to care for many, leading to reduced mortality rates in some demographic groups.
Studies have shown a correlation between increased access to testing, treatment, and hospitalization due to expanded Medicaid and other safety net programs, and a decrease in COVID-19 related deaths, particularly among low-income individuals. However, disparities persisted, highlighting the challenges in achieving equitable access. Increased preventative care utilization was also observed, particularly for chronic conditions like diabetes and hypertension, which are exacerbated by COVID-19.
This improved management of chronic diseases potentially contributed to reduced overall mortality beyond just COVID-19 related deaths.
The expanded federal safety net during COVID-19 undeniably improved health access for many, but it also highlighted existing disparities. A crucial area needing attention is maternal healthcare, especially in rural areas, as evidenced by the challenges faced by rural hospitals offering labor and delivery services, a topic explored in detail at this insightful article: Rural Hospitals Labor Delivery &.
Addressing these challenges is vital to ensuring that the improved access brought about by the expanded safety net reaches all communities, including those in rural areas.
Impact on Mortality Rates and Preventative Care
Improved access to healthcare, facilitated by the expanded safety net, contributed to a reduction in mortality rates for some populations. This was particularly evident in areas with high rates of uninsured individuals prior to the pandemic. The increased availability of testing, treatment, and hospitalization resources led to earlier interventions and better management of COVID-19 cases. Furthermore, the enhanced access to preventative care resulted in better management of pre-existing conditions, leading to improved overall health and a reduction in mortality from other causes.
However, it’s crucial to acknowledge that mortality data requires careful analysis to account for factors beyond healthcare access, such as socioeconomic determinants of health and variations in infection rates across different communities. For example, a comparison of mortality rates between states with varying levels of Medicaid expansion before and during the pandemic could offer valuable insights into the impact of the expanded safety net.
Challenges in Providing Healthcare Access to Underserved Populations, Expanded federal safety net covid 19 improved health access
Despite the expansion, significant challenges remained in providing healthcare access to underserved populations during the pandemic. These included geographical barriers, particularly in rural areas with limited healthcare infrastructure and provider shortages. Language barriers and cultural differences also presented obstacles to effective communication and care delivery. Furthermore, many underserved populations faced systemic issues such as lack of transportation, unreliable internet access, and mistrust of the healthcare system, which hindered their ability to access and utilize expanded services.
For instance, communities of color disproportionately experienced higher rates of COVID-19 infection and mortality, partly due to these pre-existing inequalities in healthcare access. Addressing these complex challenges requires a multi-faceted approach involving targeted outreach programs, community-based initiatives, and culturally sensitive healthcare delivery models.
The Role of Telehealth in Expanding Access
Telehealth played a pivotal role in expanding healthcare access during the pandemic, particularly for individuals in remote areas or those with mobility limitations. Virtual consultations, remote monitoring, and online health education significantly reduced geographical barriers and improved access to specialist care. The ability to consult with doctors remotely through video conferencing and receive remote monitoring of vital signs allowed for more convenient and timely care.
However, the effectiveness of telehealth relies on reliable internet access and technological literacy, which are not universally available. Digital literacy programs and subsidized internet access are crucial to ensuring equitable access to telehealth services.
Telehealth Access Flowchart
The following flowchart illustrates a simplified process of accessing telehealth services:[Imagine a flowchart here. It would begin with “Patient needs medical attention,” branching to “Does patient have internet access and a device?” A “yes” branch would lead to “Patient schedules telehealth appointment,” then to “Patient participates in virtual consultation,” and finally to “Follow-up care as needed.” A “no” branch from “Does patient have internet access and a device?” would lead to “Patient seeks alternative access options (e.g., in-person care, community resources).” ]
Financial Assistance and its Effects
The COVID-19 pandemic triggered an unprecedented economic crisis, leaving millions struggling financially. In response, the federal government implemented various financial assistance programs, aiming to mitigate economic hardship and ensure access to healthcare. Analyzing the effectiveness of these programs requires examining their impact on individuals’ financial stability and healthcare access, both in the short-term and long-term.The effectiveness of different financial assistance programs varied considerably, depending on factors such as program design, eligibility criteria, and the speed of disbursement.
Some programs, like the expanded unemployment benefits, provided immediate relief to millions of unemployed individuals, while others, such as the stimulus checks, offered broader, albeit less targeted, support. The efficacy of these programs was also influenced by factors outside of the programs themselves, such as the severity of the economic downturn in different regions and the pre-existing financial vulnerabilities of individuals and households.
Effectiveness of Different Financial Assistance Programs
The effectiveness of different financial assistance programs in mitigating economic hardship varied significantly. For instance, expanded unemployment insurance proved highly effective in preventing widespread destitution among those who lost their jobs. However, the rollout of some programs, like the Paycheck Protection Program (PPP), faced challenges, with some small businesses struggling to navigate the application process and access the funds they needed.
Stimulus checks, while providing broad-based relief, were criticized for not adequately addressing the needs of low-income households or those facing significant debt burdens. The effectiveness of these programs could also be seen through their impact on household income, consumer spending, and the overall economy. For example, the expanded Child Tax Credit significantly reduced child poverty and increased household income for many families.
The expanded federal safety net during COVID-19 undeniably improved health access for many, but the sheer volume of patient data created new challenges. Streamlining this process is crucial, and that’s where advancements like the integration of Nuance’s generative AI scribe with Epic EHRs, as detailed in this article nuance integrates generative ai scribe epic ehrs , become game-changers.
This technology could significantly reduce administrative burdens, freeing up healthcare providers to focus on patient care and further enhancing the positive impact of the expanded safety net.
Impact on Healthcare Access
Financial assistance programs demonstrably improved healthcare access for many individuals. The expanded Medicaid coverage in some states, coupled with the increased availability of subsidized health insurance through the Affordable Care Act marketplaces, ensured that many people could afford essential healthcare services. This was particularly crucial for those who lost their employer-sponsored health insurance due to job losses. The increased availability of telehealth services, often covered by these programs, further facilitated access to care, especially in remote areas or for individuals with mobility limitations.
Conversely, the lack of consistent, accessible mental health services was a common complaint, indicating that while the financial burden was alleviated, access to specific types of care still presented a challenge for many.
Long-Term Effects on Household Financial Stability and Health
The long-term effects of these financial assistance programs are still unfolding, but preliminary evidence suggests a mixed picture.
- Improved Financial Stability for Some: For many households, the financial assistance provided a crucial lifeline, preventing homelessness, eviction, and bankruptcy. This stability, in turn, positively impacted their mental and physical health.
- Persistent Financial Insecurity for Others: However, the assistance wasn’t sufficient for all, leaving many still struggling with debt and economic insecurity. The uneven distribution of assistance also exacerbated existing inequalities, disproportionately impacting low-income households and communities of color.
- Long-Term Health Impacts: The pandemic’s economic fallout had profound health consequences, including increased rates of stress, anxiety, and depression. While financial assistance mitigated some of these impacts, the long-term health effects of prolonged economic hardship are still being assessed. For example, studies are beginning to emerge about the long-term effects of stress and anxiety on cardiovascular health and overall well-being in populations affected by the pandemic and related financial hardship.
- Policy Implications: The experience with COVID-19 financial assistance programs highlights the need for more robust and targeted safety nets. Future policies should consider the diverse needs of different populations and ensure that assistance reaches those most in need in a timely and efficient manner. Furthermore, addressing systemic inequalities that disproportionately impact certain groups is crucial to building a more resilient and equitable economic and health system.
Long-Term Impacts and Sustainability

Source: pennlive.com
The unprecedented expansion of the federal safety net during the COVID-19 pandemic, while undeniably crucial in mitigating immediate crises, presents a complex legacy of long-term impacts on both the healthcare system and the broader economy. Understanding these implications, both positive and negative, is critical for building a more resilient and equitable healthcare infrastructure moving forward. The short-term gains, while significant, must be weighed against the potential for long-term systemic changes and the sustainability of these changes.The expanded safety net demonstrably improved access to healthcare for many previously underserved populations.
Increased Medicaid enrollment, expanded telehealth services, and the temporary suspension of certain healthcare regulations all contributed to this. However, the long-term effects depend heavily on whether these gains can be sustained beyond the immediate crisis. The potential exists for lasting improvements in health equity and outcomes, but this requires careful planning and sustained political will. A crucial aspect of this is ensuring that the lessons learned during the pandemic are not forgotten, and that the temporary measures implemented are not simply reversed once the immediate threat has passed.
This necessitates a shift from reactive crisis management to proactive long-term planning and investment.
The Economic and Healthcare System Impacts
The economic implications of the expanded safety net are multifaceted. While providing immediate relief to individuals and families, the increased government spending undoubtedly added to the national debt. However, the economic benefits of a healthier population – increased productivity, reduced healthcare costs in the long run due to preventative care and early intervention – should be considered. For example, studies have shown that increased access to preventative care can lead to significant reductions in hospitalizations and emergency room visits, offsetting some of the initial costs.
The long-term economic impact will depend on factors such as the sustainability of the expanded safety net programs and the effectiveness of these programs in promoting long-term health improvements. A failure to adequately address the long-term costs could lead to fiscal strain, while a successful strategy could result in a healthier, more productive workforce.
Potential for Sustainable Improvements in Health Access
The pandemic highlighted the critical need for improved digital infrastructure and telehealth capabilities. The rapid expansion of telehealth during the pandemic demonstrated its potential to overcome geographical barriers and improve access to care, particularly for rural and underserved communities. Sustaining and expanding these capabilities requires investment in broadband infrastructure and the development of robust telehealth policies that address issues such as reimbursement rates and data privacy.
Furthermore, lessons learned about the effectiveness of various public health interventions, such as contact tracing and community-based testing, can inform future pandemic preparedness strategies and improve overall public health infrastructure. The success of these improvements depends on sustained investment and political commitment to ensure equitable access for all.
Short-Term Relief vs. Long-Term Systemic Change
The trade-offs between short-term relief and long-term systemic change are significant. While the expanded safety net provided immediate relief during the pandemic, it also raised concerns about fiscal sustainability and the potential for unintended consequences. A focus solely on short-term relief might lead to temporary improvements but fail to address underlying systemic issues that contribute to health inequities.
On the other hand, a solely long-term focus might not provide sufficient immediate relief, leading to worsening health outcomes and economic hardship. Finding the right balance requires careful consideration of the costs and benefits of various policy options.
| Short-Term Impacts | Long-Term Impacts |
|---|---|
| Increased access to healthcare for many | Potential for improved health equity and outcomes |
| Immediate economic relief for individuals and families | Increased national debt |
| Increased strain on healthcare systems | Potential for a healthier, more productive workforce |
| Temporary expansion of telehealth services | Potential for lasting improvements in telehealth infrastructure |
| Increased Medicaid enrollment | Need for sustainable funding mechanisms for expanded coverage |
Equity and Access for Vulnerable Populations: Expanded Federal Safety Net Covid 19 Improved Health Access
Source: dwcdn.net
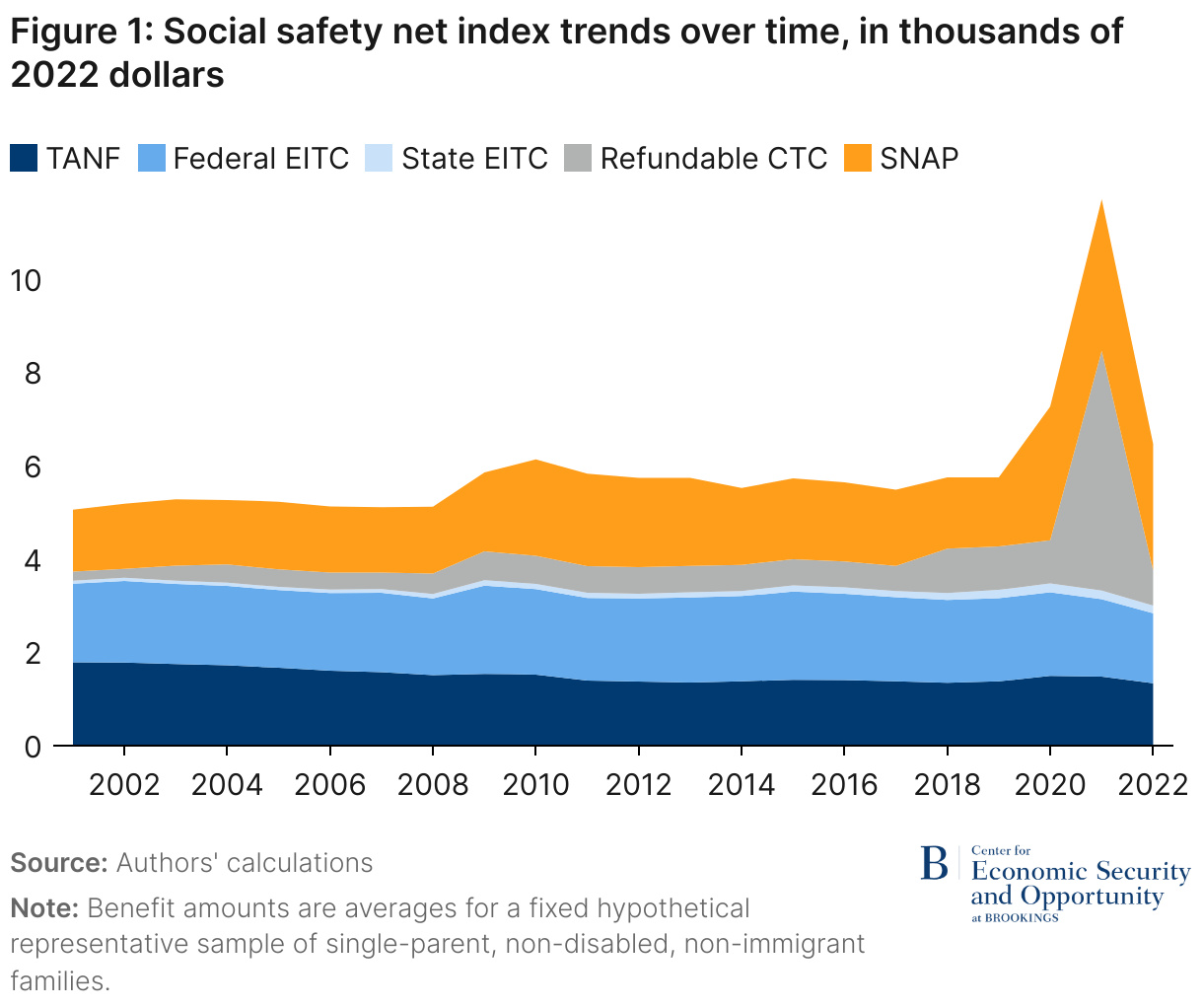
The expansion of the federal safety net during the COVID-19 pandemic aimed to improve healthcare access and financial assistance for all Americans. However, pre-existing inequalities meant that vulnerable populations—racial and ethnic minorities, low-income individuals, and those in rural areas—often faced significant barriers to accessing these crucial resources. Understanding these disparities and evaluating the effectiveness of the expanded safety net in addressing them is vital for building a more equitable and resilient healthcare system.The expanded safety net, while providing much-needed relief, didn’t uniformly benefit all groups.
Existing systemic inequities, including historical underinvestment in healthcare infrastructure in underserved communities and persistent biases in healthcare delivery, hindered equitable access. For instance, language barriers, lack of transportation, and limited digital literacy prevented some individuals from even applying for assistance programs. Furthermore, mistrust of government institutions, stemming from historical injustices, created additional obstacles for certain communities.
Disparities in Access to Healthcare and Safety Net Programs
Several factors contributed to the unequal distribution of resources. Racial and ethnic minorities experienced higher rates of COVID-19 infection and mortality, yet faced disproportionately higher rates of unemployment and lacked sufficient access to testing, treatment, and vaccination. Low-income individuals struggled with food insecurity and housing instability, making it difficult to prioritize healthcare needs. Rural communities, often characterized by limited healthcare infrastructure and provider shortages, faced considerable challenges in accessing timely and quality care.
These disparities highlight the need for targeted interventions to address the root causes of inequitable access.
The Expanded Safety Net’s Impact on Disparities
The expanded safety net, including increased unemployment benefits, stimulus checks, and enhanced Medicaid coverage, undoubtedly offered crucial relief to many vulnerable populations. However, the effectiveness varied considerably across different groups. While stimulus checks provided immediate financial assistance, they did little to address the underlying systemic issues contributing to health disparities. The expansion of Medicaid coverage improved access for some, but significant gaps remained due to enrollment barriers and limited provider networks in underserved areas.
Furthermore, the design of some programs inadvertently excluded certain vulnerable populations, such as undocumented immigrants, who were often ineligible for crucial support.
Visual Representation of Safety Net Resource Distribution
Imagine a map of the United States. Each state is shaded according to the proportion of its population receiving benefits from the expanded safety net programs. Darker shades represent higher rates of access. Overlayed on this map are demographic data points, indicating the concentration of racial and ethnic minorities, low-income individuals, and rural populations. A clear visual correlation would likely show that darker shades (higher access) are less concentrated in areas with higher proportions of vulnerable populations.
For instance, rural counties, often predominantly white, might show higher access to certain programs compared to urban counties with larger minority populations, even if the per capita income is similar. This visual representation would highlight the uneven distribution of safety net resources, despite the expansion.
End of Discussion
The expanded federal safety net during COVID-19 undeniably improved health access for many, but it also highlighted existing systemic inequities. While temporary relief measures provided a crucial lifeline, the long-term sustainability of these changes and the need for equitable access remain pressing concerns. The pandemic served as a harsh but necessary spotlight, revealing both the resilience of the human spirit and the fragility of our systems.
The lessons learned, both positive and negative, should guide us toward a more robust and just approach to public health and social welfare in the future. The journey to truly equitable healthcare access is far from over, but the path forward is clearer thanks to the hard-won insights of this unprecedented period.
Key Questions Answered
What were some unintended consequences of the expanded safety net?
Increased bureaucratic hurdles, program inefficiencies, and potential for fraud are among the unintended consequences.
How did the expanded safety net impact mental health services?
Increased access to telehealth and some expansion of mental health services occurred, though disparities remained.
What long-term funding models are being considered for sustaining improvements?
Discussions involve a mix of increased taxes, reallocation of existing funds, and potential public-private partnerships.
How did the pandemic affect the uninsured rate?
While some temporary coverage expansions occurred, the long-term impact on the uninsured rate is still being assessed.





