New York Extends Medicaid & CHIP Postpartum
New york extend medicaid and chip postpartum – New York extends Medicaid and CHIP postpartum coverage! This is huge news for new parents in the state, offering a much-needed lifeline of support during a crucial, often challenging time. For months, advocates have pushed for this expansion, arguing that extending coverage beyond the current timeframe dramatically improves maternal and child health outcomes. This post dives into the details, exploring the impact, the challenges, and what this means for families across New York.
We’ll unpack the specifics of the extended coverage, looking at eligibility requirements, the duration of benefits, and how it compares to other states. We’ll also examine the potential economic benefits, both for families and the healthcare system as a whole. Plus, we’ll discuss the hurdles overcome to make this expansion a reality and what the future holds for postpartum care in New York.
Postpartum Medicaid and CHIP Expansion in New York: New York Extend Medicaid And Chip Postpartum
Source: thepublive.com
New York has significantly expanded its postpartum Medicaid and CHIP (Children’s Health Insurance Program) coverage, aiming to improve maternal health outcomes and reduce disparities in access to care. This expansion builds upon existing programs and reflects a growing national movement to extend postpartum coverage beyond the traditional timeframe. Understanding the current status, eligibility criteria, and duration of coverage is crucial for both healthcare providers and expectant mothers in the state.
Current Status of Postpartum Medicaid and CHIP Coverage in New York
New York currently offers extended postpartum Medicaid and CHIP coverage for a full year following childbirth. This represents a substantial improvement over previous coverage limits and aligns with the federal option to extend postpartum Medicaid coverage to one year. The expansion has been implemented to address the significant health risks women face in the postpartum period, including postpartum depression, hypertension, and other complications.
New York’s extension of Medicaid and CHIP postpartum coverage is fantastic news for new moms, ensuring access to vital healthcare. This is especially crucial considering the challenges faced by many rural areas, as highlighted in this insightful article on Rural Hospitals Labor Delivery & the struggles they face in providing adequate maternity care. Hopefully, this expanded coverage will help alleviate some of the pressure on these already strained facilities and improve maternal health outcomes across the state.
The state’s commitment to this extended coverage demonstrates a recognition of the importance of continuous access to healthcare for new mothers.
Eligibility Criteria for Postpartum Medicaid and CHIP Benefits
Eligibility for postpartum Medicaid and CHIP in New York generally follows the same guidelines as standard Medicaid and CHIP eligibility, with the crucial addition of a one-year postpartum extension. This means individuals who meet the income and residency requirements for Medicaid or CHIP during pregnancy will automatically qualify for continued coverage for twelve months after delivery. Specific income limits and residency requirements can be found on the New York State Department of Health website.
Individuals who were not eligible for Medicaid or CHIP during pregnancy may still be eligible for postpartum coverage if their circumstances have changed, resulting in a lower income or other qualifying factors. It’s important to apply for coverage even if unsure of eligibility, as determination is made on a case-by-case basis.
New York’s extension of Medicaid and CHIP postpartum coverage is fantastic news for new mothers, ensuring access to vital healthcare. This improved access highlights the need for efficient documentation, which is where advancements like those described in this article on nuance integrates generative ai scribe epic ehrs become incredibly important. Streamlining medical record-keeping will ultimately free up time for doctors to focus on patient care, a key benefit for the expanded postpartum coverage program.
Duration of Postpartum Coverage, New york extend medicaid and chip postpartum
As mentioned previously, New York provides a full year (12 months) of postpartum Medicaid and CHIP coverage following delivery. This continuous coverage ensures access to necessary medical services, including postpartum checkups, mental health support, and treatment for any complications arising after childbirth. This extended timeframe is designed to address the significant health needs of new mothers during a critical period of recovery and adjustment.
The consistent coverage aims to reduce the risk of delayed or forgone care due to financial constraints or administrative barriers.
Comparison of New York’s Postpartum Coverage to Other States
The following table compares New York’s postpartum Medicaid and CHIP coverage to that of other states. Note that state policies are constantly evolving, so it is advisable to check the individual state’s health department for the most up-to-date information.
| State | Coverage Duration | Eligibility Requirements | Funding Source |
|---|---|---|---|
| New York | 12 months | Income and residency requirements (similar to standard Medicaid/CHIP) | State and federal funds |
| California | 12 months | Income and residency requirements (similar to standard Medicaid/CHIP) | State and federal funds |
| Oregon | 12 months | Income and residency requirements (similar to standard Medicaid/CHIP) | State and federal funds |
| Texas | 60 days (currently, expansion efforts underway) | Income and residency requirements (similar to standard Medicaid/CHIP) | State and federal funds |
Impact of Extended Postpartum Coverage
Extending postpartum Medicaid and CHIP coverage in New York has the potential to significantly improve maternal and child health outcomes, reduce healthcare costs in the long run, and enhance access to vital care for vulnerable families. The benefits extend beyond individual families, impacting the overall health and economic well-being of the state.Postpartum care is crucial for both the mother’s physical and mental recovery and the child’s healthy development.
The extended coverage period allows for more comprehensive care, addressing potential complications like postpartum depression, hypertension, and breastfeeding challenges. Early intervention during this critical period can prevent serious health issues and reduce long-term healthcare expenses.
Improved Maternal and Child Health Outcomes
Extended postpartum coverage ensures access to essential healthcare services, leading to improved maternal and child health outcomes. This includes routine check-ups, screenings for postpartum depression and other mental health conditions, and support for breastfeeding. Studies have shown a correlation between access to postpartum care and reduced rates of maternal mortality and morbidity, as well as improved infant health and development.
For example, a study published in the American Journal of Public Health demonstrated that states with extended postpartum Medicaid coverage saw a significant reduction in maternal mortality rates compared to states with shorter coverage periods. The improved access to care also facilitates early detection and treatment of potential health problems, preventing more serious and costly interventions later.
Economic Benefits for Families and the Healthcare System
While the initial cost of extending coverage might seem significant, the long-term economic benefits are substantial. By preventing complications and promoting early intervention, extended postpartum coverage can significantly reduce costly hospitalizations and emergency room visits later. Families benefit from reduced out-of-pocket expenses, enabling them to focus on their recovery and the care of their newborn. This improved financial stability can also positively impact other aspects of family well-being, including housing and nutrition.
For example, a reduction in premature births, a frequent cause of expensive neonatal intensive care, would contribute significantly to cost savings for both families and the healthcare system.
Impact on Healthcare Access and Utilization Rates
Extending postpartum coverage directly improves healthcare access for women, particularly those from low-income backgrounds. Without this coverage, many women would forgo necessary care due to financial constraints, leading to potentially serious health consequences. Increased access to care translates to higher utilization rates for preventive services and early intervention, ultimately resulting in better health outcomes and reduced long-term healthcare costs.
This is supported by evidence from states that have already implemented similar expansions; these states have reported increases in the utilization of postpartum check-ups and other preventive services, with a corresponding decrease in hospital readmissions for postpartum complications.
Successful Postpartum Medicaid Expansion Programs in Other States
Several states have successfully implemented postpartum Medicaid expansion programs, demonstrating the positive impact of extended coverage. For instance, Oregon’s experience with extended postpartum Medicaid coverage provides a strong case study, illustrating significant improvements in maternal and child health outcomes, coupled with a decrease in long-term healthcare spending. Similarly, states like Colorado and Illinois have also reported positive results following the expansion of their postpartum Medicaid programs, showcasing the effectiveness of this policy in improving healthcare access and reducing healthcare costs.
These successful examples offer valuable insights and provide a strong foundation for the anticipated positive effects of New York’s expanded postpartum coverage.
Funding and Implementation Challenges
Extending postpartum Medicaid and CHIP coverage in New York presents significant funding and implementation hurdles. Securing sufficient resources and ensuring smooth, equitable access for all eligible individuals requires careful planning and proactive problem-solving. The success of this expansion hinges on addressing these challenges effectively.
Potential Funding Sources for Extended Postpartum Coverage
Several funding avenues could support the extended postpartum coverage. The state could allocate funds from its general budget, potentially leveraging existing healthcare initiatives or reallocating resources from other programs. Federal matching funds under the Medicaid program are a crucial component, and securing these requires careful adherence to federal guidelines and reporting requirements. Additional funding might be sought through grants from private foundations or philanthropic organizations focused on maternal and child health.
Innovative financing mechanisms, such as public-private partnerships, could also be explored. For example, New York could explore models used in other states that successfully leveraged federal matching funds combined with state-level investments and private sector collaborations. One successful example could be a partnership with insurance companies incentivized to participate through reduced costs associated with later, more complicated care.
Logistical Challenges in Implementing the Expansion
Implementing the expansion requires overcoming significant logistical obstacles. The state’s Medicaid agency will need to update its IT systems to accommodate the extended coverage period and ensure seamless processing of claims. Training healthcare providers on the expanded eligibility criteria and new administrative procedures is essential. Public awareness campaigns are necessary to inform eligible individuals about the extended coverage and how to enroll.
This involves effective outreach to underserved communities and addressing potential language barriers. A key logistical challenge will be ensuring the efficient and timely processing of applications, avoiding delays that could leave vulnerable women without necessary care. The state could learn from past Medicaid expansions, analyzing what worked well and what could be improved to minimize bureaucratic delays.
Barriers to Accessing Extended Coverage
Even with expanded coverage, barriers to access remain. Navigating the enrollment process can be daunting for many individuals, particularly those facing socioeconomic disadvantages. Transportation limitations, lack of childcare, and inflexible work schedules can prevent timely enrollment and access to care. Language barriers and cultural sensitivities must be addressed to ensure equitable access for all. For example, some immigrant communities might be hesitant to engage with government programs due to fear of immigration status implications.
The state needs to actively address these concerns through culturally competent outreach and multilingual support. Furthermore, the availability of healthcare providers who accept Medicaid in certain regions could create geographical access barriers, particularly in rural areas.
Addressing Implementation Challenges and Ensuring Equitable Access
A comprehensive plan to address these challenges is vital. This includes robust funding allocation, thorough provider training, streamlined enrollment processes, and targeted outreach to underserved communities. The state should invest in technological infrastructure to facilitate efficient claims processing and online enrollment. Partnerships with community-based organizations can help overcome access barriers by providing enrollment assistance, transportation, and childcare support.
Regular monitoring and evaluation are crucial to identify and address emerging challenges and ensure that the program effectively reaches its intended population. The plan should include specific targets for enrollment rates among different demographic groups to ensure equitable access. For example, setting specific goals for enrollment among low-income women of color and rural residents could help track progress and identify areas needing additional support.
New York’s extension of Medicaid and CHIP postpartum coverage is fantastic news for new mothers, ensuring access to crucial healthcare. It makes me wonder about the broader healthcare landscape, and how initiatives like the one described in this article on Mass General Brigham Buyouts Digital Unit might impact access to care. Ultimately, expanding access, whether through state programs or technological innovation, benefits everyone.
The New York initiative is a step in the right direction.
Comparison of Different Extension Models
Extending postpartum Medicaid and CHIP coverage presents several model options, each with its own set of advantages and disadvantages. The optimal model depends on a state’s specific circumstances, including its existing healthcare infrastructure, budget constraints, and the demographics of its population. Choosing the right model is crucial for maximizing both cost-effectiveness and accessibility to vital healthcare services for new mothers.Choosing the right model for extending postpartum Medicaid and CHIP coverage requires careful consideration of various factors.
Different models offer varying degrees of coverage duration, eligibility criteria, and administrative complexities. This analysis will examine several potential models, weighing their respective strengths and weaknesses in terms of cost-effectiveness and accessibility.
Model Comparison: Duration of Coverage
The most significant difference between models lies in the duration of extended postpartum coverage. Some models extend coverage for the full 12 months postpartum recommended by the American College of Obstetricians and Gynecologists (ACOG), while others offer shorter durations. Shorter durations may be more cost-effective in the short term but could compromise the long-term health and well-being of mothers and newborns.
Longer durations, while potentially more expensive, can lead to better health outcomes and reduced long-term healthcare costs.
- Model A: 12-Month Extension: This model extends postpartum Medicaid and CHIP coverage for the full 12 months following childbirth. This aligns with ACOG recommendations and provides comprehensive coverage for the crucial postpartum period. Strengths include improved maternal and child health outcomes and potentially reduced long-term healthcare costs. Weaknesses include higher overall program costs compared to shorter extension models. This model would require significant funding increases.
For example, a state like California, with its large population, would need to allocate substantial additional funds to support a 12-month extension for all eligible mothers.
- Model B: 6-Month Extension: This model extends coverage for six months postpartum. It represents a compromise between cost-effectiveness and health benefits. Strengths include reduced costs compared to a 12-month extension. Weaknesses include potential gaps in coverage during a critical period for postpartum recovery and potential negative impacts on long-term health outcomes. A shorter extension might be suitable for states with limited budgets, but the potential for increased healthcare costs down the line due to untreated conditions should be carefully considered.
- Model C: Phased Extension (6 months initially, with possibility of extension to 12 months based on risk factors): This model starts with a 6-month extension, but allows for an extension to 12 months based on identified risk factors such as pre-existing conditions, complications during pregnancy or delivery, or socioeconomic factors. Strengths include a balance between cost and comprehensive coverage, targeting resources to those who need them most. Weaknesses include the administrative complexity of assessing risk factors and the potential for delays in extending coverage for high-risk individuals.
This model requires a robust risk assessment system to be effective and fair. For instance, a system could utilize algorithms incorporating data from electronic health records to identify high-risk individuals automatically.
Model Comparison: Eligibility Criteria
Variations in eligibility criteria also influence the cost-effectiveness and accessibility of different models. Some models might maintain existing eligibility criteria, while others could expand eligibility to include more women.
- Model A: Maintaining Existing Eligibility: This model uses the existing eligibility criteria for Medicaid and CHIP, extending coverage for those already enrolled. This minimizes administrative complexity. However, it may exclude some women who could benefit from extended postpartum coverage.
- Model B: Expanding Eligibility to Include More Women: This model broadens eligibility criteria, potentially including women with incomes slightly above the current threshold. This increases accessibility but also increases program costs.
Model Comparison: Implementation Strategies
The implementation of different models requires distinct strategies. Some models might require significant changes to existing systems, while others may involve relatively minor adjustments. These differences impact the overall cost and effectiveness of the program.
- Model A: Integration with Existing Systems: This model focuses on integrating the extension into existing Medicaid and CHIP administrative systems, minimizing disruption and administrative costs. However, it might require system upgrades to accommodate the extended coverage period.
- Model B: Creation of a Separate Program: This model involves establishing a separate program specifically for postpartum coverage, which offers greater flexibility but also increases administrative complexity and costs.
Advocacy and Policy Recommendations

Source: earlysuccess.org
Securing and maintaining extended postpartum Medicaid and CHIP coverage in New York requires a multifaceted approach involving strategic advocacy and robust policy recommendations. Success hinges on the collaborative efforts of various stakeholders, a clear understanding of funding mechanisms, and a commitment to long-term program sustainability.
Strategies for Advocating for Extended Postpartum Coverage
Effective advocacy requires a multi-pronged strategy. This includes grassroots mobilization, engaging community organizations to reach vulnerable populations and amplify their voices. Direct lobbying of state legislators and policymakers is crucial, presenting data on the positive impacts of extended coverage on maternal and child health outcomes. Public awareness campaigns, utilizing social media and traditional media outlets, can shape public opinion and generate support for the policy.
Finally, building coalitions with healthcare providers, professional organizations, and other advocacy groups strengthens the collective voice and increases the policy’s chances of success. For example, successful campaigns in other states leveraged powerful narratives from mothers who benefited from extended coverage, showcasing the program’s real-world impact.
Policy Recommendations for Long-Term Sustainability
Ensuring the long-term viability of the expanded postpartum coverage program requires careful consideration of funding sources and program design. Dedicated, predictable funding streams, such as increased state taxes or dedicated federal funding, are vital. Regular program evaluations, measuring key outcomes like maternal mortality rates and infant health indicators, will help demonstrate the program’s effectiveness and justify continued funding.
Streamlining administrative processes and reducing bureaucratic hurdles will increase efficiency and minimize administrative costs. Exploring innovative funding models, such as public-private partnerships, could also diversify funding sources and ensure the program’s resilience. For instance, a successful model in Colorado involved leveraging existing healthcare infrastructure and integrating postpartum care into existing maternal health programs.
Roles of Stakeholders in Advocacy and Implementation
Multiple stakeholders play crucial roles in both advocating for and implementing extended postpartum coverage. State legislators are responsible for enacting and funding the program. Healthcare providers, including obstetricians, midwives, and pediatricians, are essential in delivering care and advocating for their patients’ needs. Community organizations serve as crucial links to vulnerable populations, providing outreach and support. Insurance companies have a role in ensuring smooth program implementation and timely payments.
Finally, advocacy groups play a critical role in raising public awareness, lobbying for policy changes, and monitoring program implementation. Effective collaboration among these stakeholders is paramount to the program’s success. For example, the successful implementation of similar programs in other states involved strong partnerships between state health departments, healthcare providers, and community-based organizations.
Visual Representation of the Policy Advocacy Process
Imagine a flowchart. The process begins with Identifying the Need, represented by a box at the top. Arrows lead to subsequent boxes representing key steps: Research & Data Collection, Stakeholder Engagement & Coalition Building, Policy Drafting & Lobbying, Legislative Action & Approval, Program Implementation & Monitoring, and finally Evaluation & Adjustment. Each box contains icons representing the key players involved at each stage (e.g., a doctor icon for healthcare providers, a gavel for legislators, a megaphone for advocacy groups).
Timelines could be indicated by arrows connecting the boxes, with estimated durations for each stage. Key milestones, such as legislative hearings or program launch dates, could be marked on the timeline. The final box, Evaluation & Adjustment, shows a cyclical loop, emphasizing the ongoing nature of program monitoring and refinement. This visual representation provides a clear, concise overview of the entire advocacy process, highlighting the collaborative nature of the effort and the importance of continuous evaluation.
Final Review
The extension of postpartum Medicaid and CHIP coverage in New York marks a significant victory for maternal and child health. By providing longer-term support, this initiative promises to improve health outcomes, reduce financial strain on families, and create a more equitable healthcare system. While challenges remain in implementation and funding, the commitment to extending this vital coverage is a step towards ensuring healthier futures for New York’s families.
This is a story worth celebrating and one that hopefully inspires similar changes nationwide.
Q&A
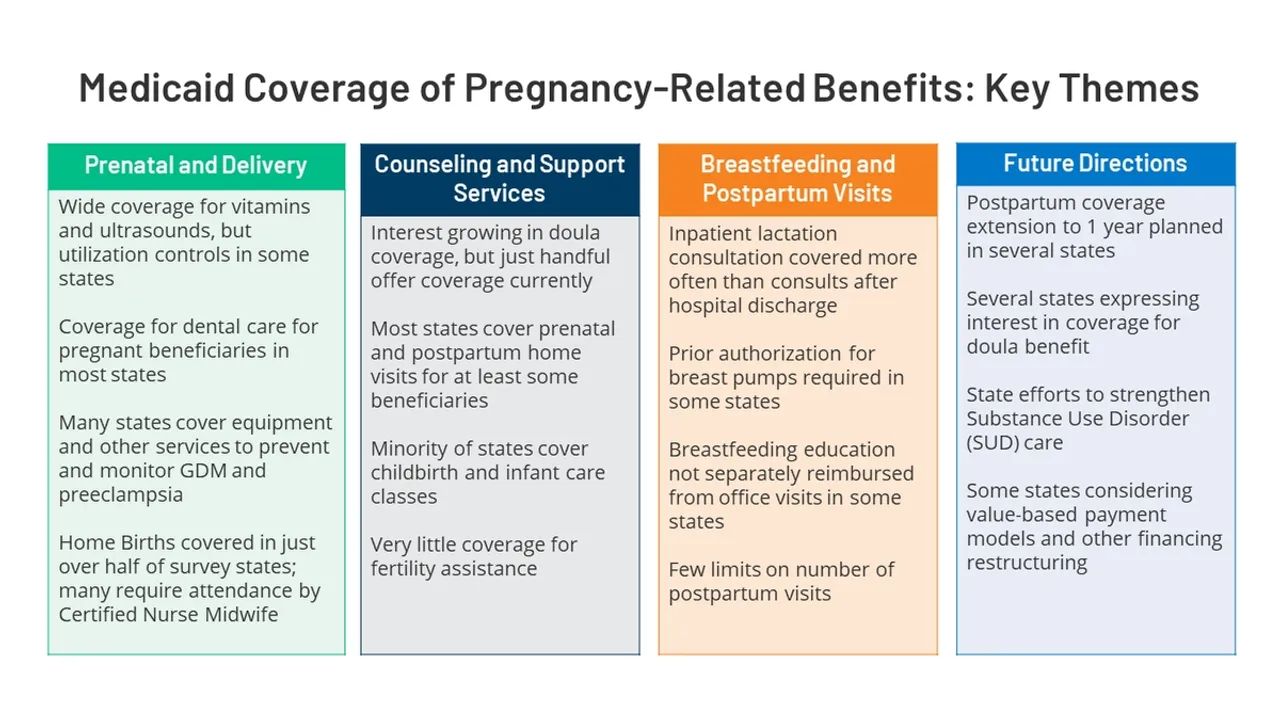
What specific services are covered under the extended postpartum Medicaid and CHIP?
The extended coverage typically includes a wide range of services, including prenatal and postnatal checkups, vaccinations, well-baby visits, and treatment for postpartum depression. Specific services can vary depending on individual needs and provider availability.
How do I apply for the extended postpartum Medicaid and CHIP benefits?
You can usually apply through the New York State Department of Health website or by contacting your local social services office. They will guide you through the application process and provide assistance with eligibility requirements.
What happens if my coverage ends before my postpartum period is complete?
This shouldn’t happen under the extended coverage, but if you experience issues, contact your healthcare provider and the relevant state agency immediately to ensure continued care. They will work to rectify any coverage gaps.