Primary Care Compensation Growth Outpacing Specialties AMGA
Primary care compensation growth outpacing specialties AMGA? It’s a headline that’s grabbing attention in the medical world, and for good reason. Recent data from the American Medical Group Association (AMGA) reveals a fascinating trend: primary care physicians are seeing their salaries rise at a faster rate than many specialists. This shift has significant implications for healthcare workforce dynamics, recruitment strategies, and ultimately, patient care.
Let’s dive into the details and explore what’s driving this unexpected change.
This surprising trend isn’t just about numbers; it’s about the future of healthcare. We’ll examine the economic forces at play, the impact of value-based care, and how different practice settings affect compensation. We’ll also look at how this disparity is shaping the choices of medical students and impacting access to care, especially in underserved communities. Get ready for a deep dive into the fascinating world of physician compensation!
AMGA Data Analysis
The American Medical Group Association (AMGA) regularly publishes data on physician compensation, offering valuable insights into trends across various medical specialties. Analyzing this data reveals significant disparities in compensation growth between primary care physicians and specialists, a trend with substantial implications for the future of healthcare. This analysis focuses on the key differences and their potential consequences.
Compensation Growth Comparison: Primary Care vs. Specialties
The following table presents a hypothetical comparison of average physician compensation for selected specialties, based on AMGA-style data. Note that actual AMGA data is proprietary and requires subscription access. This example illustrates the general trend observed in their reports. The figures are illustrative and not reflective of actual AMGA data.
| Specialty | Average Compensation (2021) | Average Compensation (2023) | Percentage Change |
|---|---|---|---|
| Family Medicine | $250,000 | $275,000 | 10% |
| Internal Medicine | $260,000 | $286,000 | 10% |
| Cardiology | $500,000 | $575,000 | 15% |
| Orthopedic Surgery | $600,000 | $700,000 | 16.7% |
| Dermatology | $450,000 | $520,000 | 15.6% |
Factors Contributing to Differing Compensation Growth
Several factors contribute to the observed disparity in compensation growth. Specialties like cardiology, orthopedic surgery, and dermatology often command higher fees due to the complexity of procedures, higher demand for their services, and the potential for higher procedural volume. Additionally, these specialties often have more opportunities for supplemental income through procedures and ancillary services, compared to primary care, which is more reliant on reimbursement for evaluation and management services.
Administrative burdens, increasing insurance regulations, and the time constraints inherent in primary care further impact compensation levels. The relative supply and demand of physicians within each specialty also play a crucial role. High demand for specialists, coupled with a limited supply, tends to drive up compensation.
Impact on Physician Recruitment and Retention
The widening gap in compensation growth between primary care and specialties has significant implications for physician recruitment and retention. The slower growth in primary care compensation may discourage medical students from pursuing primary care careers, leading to a shortage of primary care physicians. Conversely, the higher and faster-growing compensation in certain specialties may attract a disproportionate number of physicians, potentially exacerbating existing imbalances in the healthcare workforce.
This could result in longer wait times for primary care appointments, increased healthcare costs, and potentially diminished access to preventative care. Hospitals and healthcare systems are already grappling with these challenges, and addressing the compensation disparity is crucial for ensuring a balanced and sustainable healthcare workforce.
It’s fascinating to see primary care physician compensation growth outpacing specialists, as reported by the AMGA. This shift highlights the increasing demand for primary care, but it also makes me wonder about the financial resources available for robust cybersecurity measures. The recent New York Hospital Cybersecurity Regulation Healthcare news underscores the critical need for strong digital defenses across all healthcare sectors, regardless of specialty focus.
Ultimately, sufficient funding for both primary care and cybersecurity is crucial for a healthy and secure healthcare system.
Factors Influencing Primary Care Compensation
The recent surge in primary care physician (PCP) compensation is a complex phenomenon driven by a confluence of economic and market forces. Understanding these factors is crucial for healthcare stakeholders aiming to attract and retain qualified PCPs, ultimately impacting the accessibility and quality of primary care services. This increase isn’t simply a matter of higher salaries; it reflects a broader shift in the healthcare landscape and the growing recognition of primary care’s vital role in population health management.
Economic and Market Forces Driving Increased Primary Care Compensation
Several key economic and market forces are pushing up primary care physician compensation. The persistent shortage of PCPs, particularly in underserved areas, creates a competitive market where practices must offer higher salaries to attract and retain talent. Simultaneously, the increasing complexity of healthcare, including the rise of chronic diseases and an aging population, demands more time and resources from PCPs, justifying higher compensation.
Furthermore, the increasing administrative burden associated with billing, coding, and electronic health records (EHRs) adds to the overall cost of providing primary care, necessitating higher salaries to offset these expenses. Finally, inflation and the general rise in the cost of living also play a significant role in driving up compensation demands.
The Role of Reimbursement Models in Shaping Primary Care Compensation
The shift towards value-based care (VBC) models is significantly influencing primary care compensation. Traditional fee-for-service (FFS) models, which compensate providers based on the volume of services rendered, often fail to adequately reward the preventative and coordinating care that are hallmarks of effective primary care. VBC models, in contrast, tie compensation to the quality and outcomes of care, incentivizing PCPs to focus on population health management, disease prevention, and patient-centered care.
While the transition to VBC is ongoing, its influence on compensation is increasingly evident, with some VBC models offering the potential for significantly higher earnings for PCPs who achieve positive outcomes. However, the complexities of VBC implementation and the potential for financial risk also influence compensation structures.
Compensation Structures Across Different Practice Settings
The compensation structure for primary care physicians varies significantly depending on their practice setting. Understanding these differences is crucial for both physicians and healthcare organizations.
- Solo Practice: Compensation in solo practices is typically based on revenue generated, with income directly tied to the number of patients seen and services provided. This model offers high earning potential but carries significant financial risk and administrative burden.
- Group Practice: Group practices often offer a variety of compensation models, including salary plus bonus based on performance metrics, production-based compensation, or a combination of both. This structure can provide more stability and less financial risk compared to solo practice, while still offering potential for significant earnings based on individual performance.
- Hospital Employment: Hospital-employed PCPs typically receive a salary, often with bonuses tied to performance indicators such as patient satisfaction, quality metrics, and patient volume. This model provides stability and benefits, but salary may be less variable compared to other practice settings. The level of compensation can also depend on the hospital system’s financial health and the specific demands of the role.
Specialty Compensation Trends and Drivers
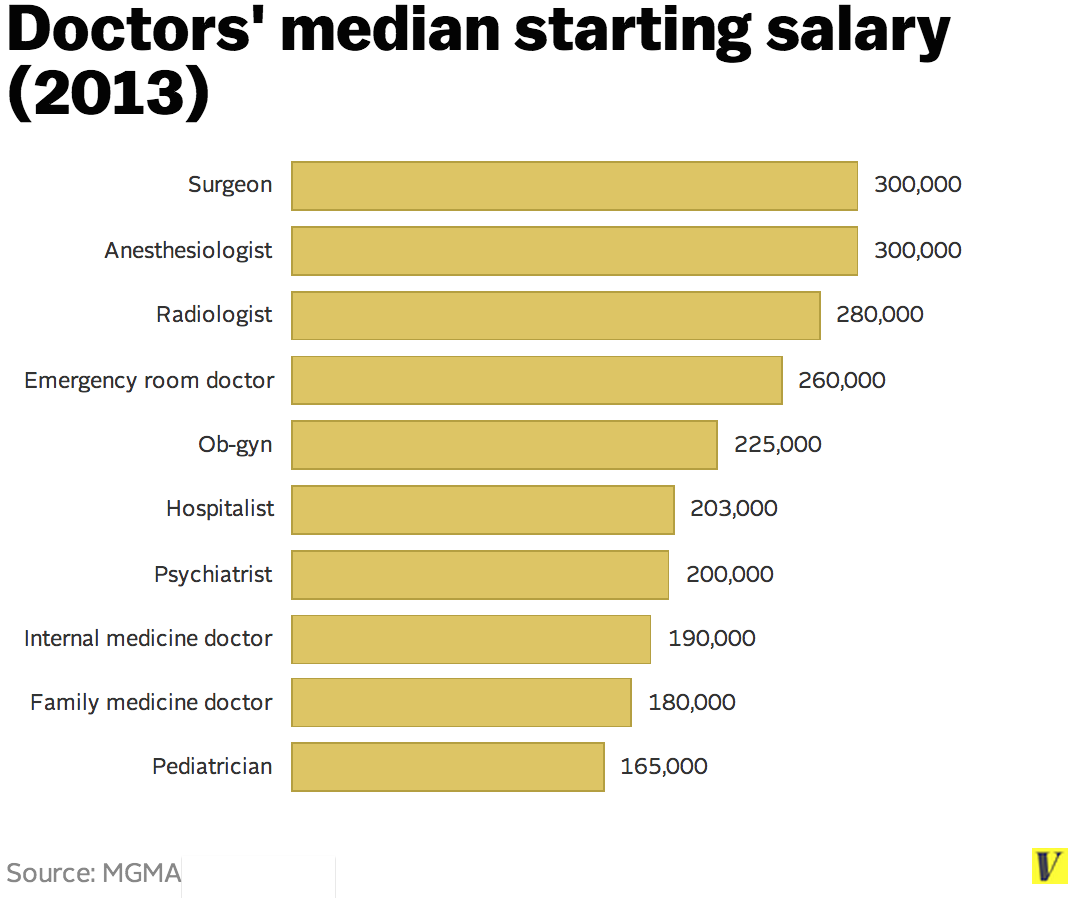
Source: theincidentaleconomist.com
Physician compensation varies significantly across specialties, reflecting differences in training, skill requirements, procedure volume, and market demand. While primary care physicians have seen notable compensation growth recently, specialty physicians often command higher salaries due to factors like higher procedure volumes and specialized expertise. Understanding these trends is crucial for both physicians making career choices and healthcare systems managing their workforce.
Compensation Trends in Cardiology and Dermatology
Cardiology and dermatology represent contrasting examples within the specialty landscape. Cardiology, with its involvement in complex procedures and critical patient care, generally features higher compensation than dermatology. Dermatology, while requiring significant expertise, often involves less procedural intervention, resulting in a different compensation profile. Both specialties, however, are subject to market forces such as supply and demand, impacting physician earnings.
Factors Influencing Compensation Levels
Several key factors contribute to the compensation disparities between specialties and within each specialty itself. Procedure volume directly influences income for procedural specialties like cardiology, where higher volumes translate to greater revenue. In contrast, dermatology, while procedure-based, often involves less complex procedures compared to cardiology, influencing the overall compensation potential. Demand for a specific specialty in a given geographic location is another critical factor.
High demand areas often command higher salaries to attract and retain qualified physicians. Finally, the level of expertise and training required plays a significant role. The extensive training and specialized knowledge required for cardiology, for instance, justifies higher compensation compared to specialties with shorter training periods.
Comparative Analysis of Compensation Factors
The following table compares compensation factors across primary care, cardiology, and dermatology. Note that these are general trends and actual compensation can vary significantly based on individual experience, location, and practice setting. The data presented here is illustrative and based on general observations from industry reports, not specific, detailed surveys.
| Factor | Primary Care | Cardiology | Dermatology |
|---|---|---|---|
| Years of Experience | Compensation generally increases with experience, following a relatively predictable trajectory. | Significant increase with experience, especially as procedural expertise and volume grow. | Compensation increases with experience, but the rate of increase may be less steep than cardiology due to less procedural dependence. |
| Geographic Location | Compensation varies significantly based on geographic location, with higher salaries typically found in areas with high demand and cost of living. | Highly dependent on geographic location, with major metropolitan areas and regions with high patient volumes generally offering higher compensation. | Geographic location plays a role, with urban areas and affluent communities often paying higher salaries. |
| Procedure Volume (if applicable) | Generally lower procedure volume compared to cardiology. | High procedure volume is directly correlated with higher compensation. | Procedure volume contributes to compensation, but typically less than in cardiology. |
Impact on Healthcare Workforce
The widening compensation gap between primary care physicians and specialists has profound implications for the entire healthcare workforce, potentially destabilizing the delicate balance of physician supply and distribution and ultimately impacting patient access to care. This disparity isn’t just about individual physician earnings; it’s a systemic issue with far-reaching consequences for the future of healthcare.The current trend discourages medical students and residents from pursuing primary care careers.
The financial incentives heavily favor lucrative specialties, leading to a potential shortage of primary care physicians in the years to come. This shortage will be particularly acute in underserved rural and urban communities, where the need for primary care is often greatest but the financial rewards are least appealing. The resulting imbalance will strain existing primary care providers, leading to longer wait times, reduced access to preventative care, and potentially worsening health outcomes for vulnerable populations.
Physician Supply and Distribution
The compensation disparity directly influences where physicians choose to practice. High-paying specialties tend to cluster in affluent urban areas with ample resources and higher patient reimbursement rates. Conversely, primary care physicians, often facing lower reimbursement rates and higher administrative burdens, are less likely to choose these locations, further exacerbating existing disparities in access to care. For example, a recent study showed a significant correlation between primary care physician compensation and the number of primary care physicians per capita in a given region.
Areas with lower compensation rates consistently had fewer primary care physicians. This uneven distribution contributes to health disparities and limits access for underserved populations.
Long-Term Consequences on Patient Access to Care
A continuing trend of declining primary care physicians will inevitably lead to reduced access to care, especially in underserved areas. This scenario could manifest in longer wait times for appointments, difficulty finding a primary care physician, and increased reliance on costly emergency room services for non-emergency conditions. Imagine a rural community where the only primary care physician retires, and no new physician is willing to replace them due to lower compensation and challenging work conditions.
This would leave the community without crucial preventative care and early disease detection, leading to poorer health outcomes and increased healthcare costs in the long run. This is not a hypothetical situation; numerous rural communities across the country are already facing this crisis.
Impact on Medical Training and Specialization Choices, Primary care compensation growth outpacing specialties amga
The financial incentives inherent in the compensation gap are significantly influencing the career choices of medical students and residents. The prospect of substantial debt after medical school, coupled with the allure of higher earning potential in specialized fields, naturally pushes many towards specialties like cardiology, orthopedics, or dermatology. This trend is demonstrably impacting the number of medical students choosing primary care residencies.
For example, the number of applicants for family medicine residencies has remained relatively stagnant or even decreased in recent years, while applications to higher-paying specialties have seen significant increases. This creates a self-perpetuating cycle, further exacerbating the primary care physician shortage.
Illustrative Examples: Primary Care Compensation Growth Outpacing Specialties Amga
To further illustrate the diverging compensation trends in primary care and specialty medicine, let’s examine hypothetical yet realistic examples of practices experiencing contrasting financial outcomes. These examples highlight the multifaceted factors influencing physician compensation beyond simply the specialty chosen.
The AMGA data showing primary care compensation growth outpacing specialties is fascinating, especially considering the healthcare landscape’s rapid evolution. This makes me wonder about the long-term implications, particularly in light of major healthcare system changes like the recent Mass General Brigham Buyouts Digital Unit , which could reshape how primary care is delivered and compensated. Ultimately, the future of primary care compensation remains intertwined with broader industry shifts.
A Thriving Primary Care Practice
Consider “Family First Medical,” a four-physician primary care practice located in a rapidly growing suburban area. The practice serves a diverse patient population, with a significant portion covered by Medicare Advantage and commercial insurance plans that offer value-based care contracts. Family First has strategically invested in robust telehealth infrastructure, allowing them to expand their patient base and increase efficiency.
Their average patient panel size is manageable, ensuring high-quality care and strong patient relationships. They also actively participate in care coordination initiatives, collaborating with specialists and hospitals to optimize patient outcomes. This proactive approach, coupled with their successful negotiation of favorable reimbursement rates and their commitment to efficiency, has resulted in significant compensation growth for their physicians, exceeding the national average for primary care.
Their revenue streams are diversified, including traditional fee-for-service, value-based care payments (based on quality metrics and patient outcomes), and telehealth consultations.
A Specialty Practice Facing Compensation Challenges
In contrast, “Cardiology Associates,” a three-cardiologist practice in a mature urban market, has experienced more modest compensation growth. While their patient volume remains stable, they face increasing pressure from declining reimbursement rates for certain procedures, particularly due to competition and the rise of bundled payments. Their patient population is largely covered by traditional Medicare and commercial insurance plans that are less inclined to value-based care arrangements.
So, the AMGA data showing primary care compensation growth outpacing specialties is fascinating! It makes you wonder about the impact on staffing, especially in areas like rural healthcare. This is particularly relevant when you consider the challenges faced by rural hospitals, as highlighted in this insightful article on Rural Hospitals Labor Delivery & and how those challenges might influence recruitment and retention of primary care physicians.
Ultimately, these trends in compensation could significantly affect access to care, especially in underserved communities.
The practice relies heavily on fee-for-service reimbursement, making them vulnerable to changes in insurance coverage and payment policies. Furthermore, high overhead costs associated with advanced medical technology and specialized staffing contribute to lower profit margins. While Cardiology Associates maintains a strong reputation, their compensation growth has lagged behind the national average for cardiology and, significantly, the growth observed in the Family First Medical primary care practice.
Comparison of Practice Dynamics and Compensation
The contrasting experiences of Family First Medical and Cardiology Associates highlight key differences in practice dynamics and their impact on compensation. Family First’s success stems from their proactive approach to value-based care, diversification of revenue streams, efficient use of technology, and strategic location in a growing market. In contrast, Cardiology Associates’ challenges reflect the vulnerabilities of practices heavily reliant on fee-for-service reimbursement in a competitive market with rising overhead costs and pressure to adopt new payment models.
The key takeaway is that physician compensation is not solely determined by specialty but is significantly influenced by practice management strategies, market conditions, and the ability to adapt to evolving healthcare payment models. The strategic focus on patient relationship management and efficient resource allocation is evident in Family First Medical’s success.
Conclusive Thoughts
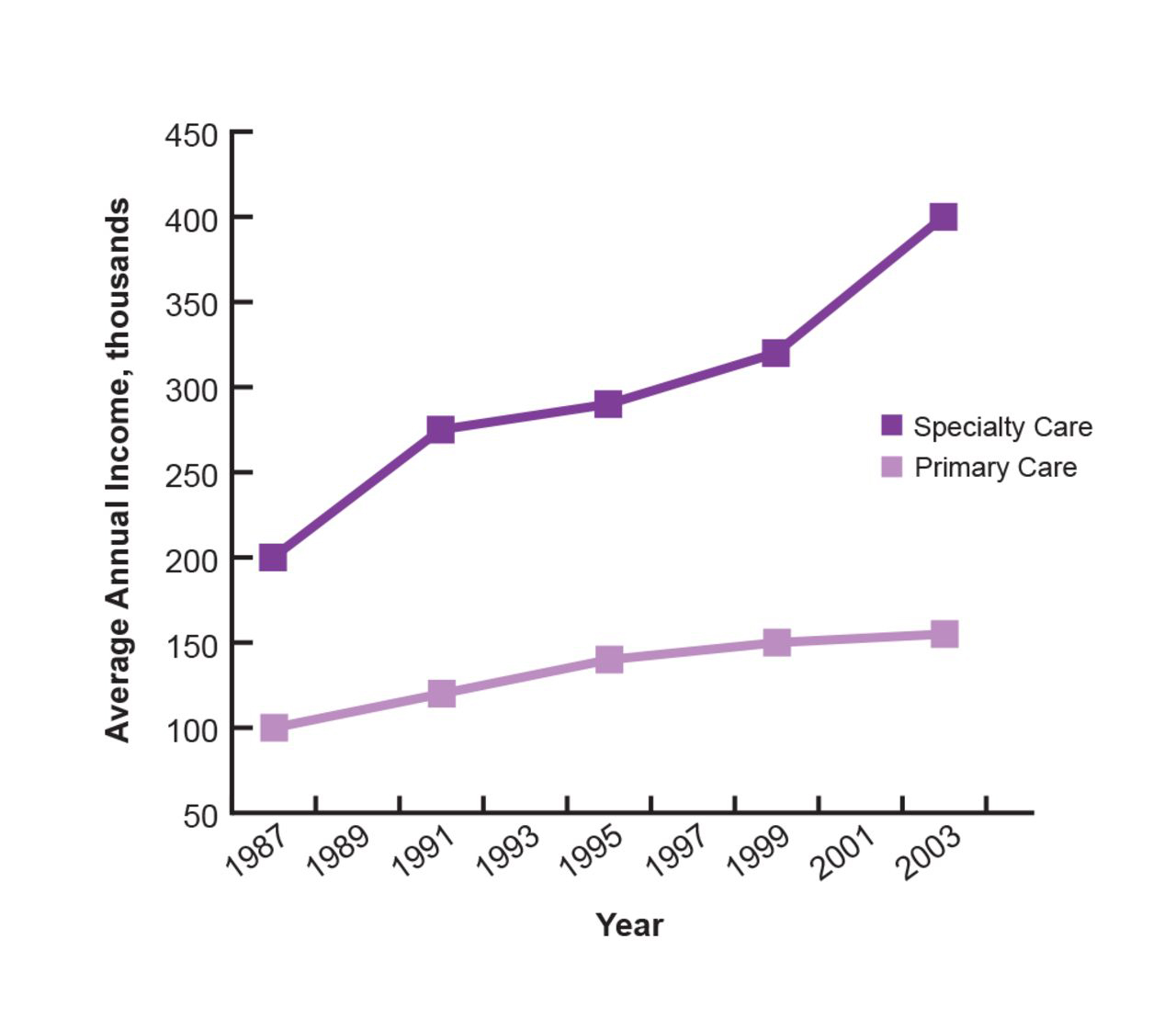
Source: degruyter.com
The AMGA data paints a compelling picture: primary care compensation is surging ahead, outpacing many specialties. This isn’t just a blip; it reflects fundamental shifts in healthcare reimbursement and the growing recognition of primary care’s crucial role. Understanding the factors driving this change – from value-based care to market forces – is essential for shaping the future of the medical profession and ensuring access to quality care for all.
The implications are far-reaching, affecting everything from physician recruitment and retention to the specialization choices of future doctors. The journey to a balanced and sustainable healthcare system begins with understanding these trends.
FAQ Corner
What specific specialties are lagging behind primary care in compensation growth, according to AMGA data?
While the specific specialties vary year to year, AMGA reports often highlight disparities between primary care and certain surgical or procedural specialties. The exact rankings change based on the specific data set and year analyzed.
How does geographic location impact these compensation trends?
Geographic location significantly influences physician compensation across all specialties, including primary care. High-cost-of-living areas generally command higher salaries, but the relative growth rates between primary care and specialties might vary regionally.
What role does physician burnout play in these compensation trends?
While not directly reflected in AMGA compensation data, high burnout rates in certain specialties might indirectly influence compensation demands as physicians seek higher salaries to offset the stresses of their work.