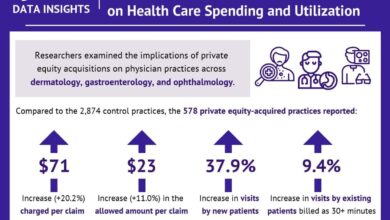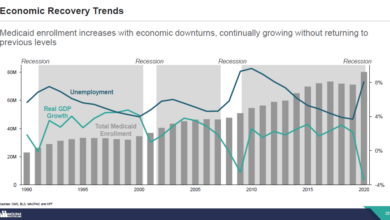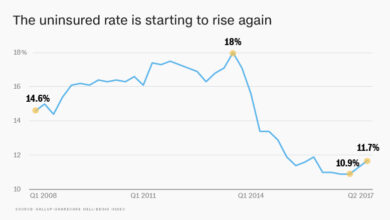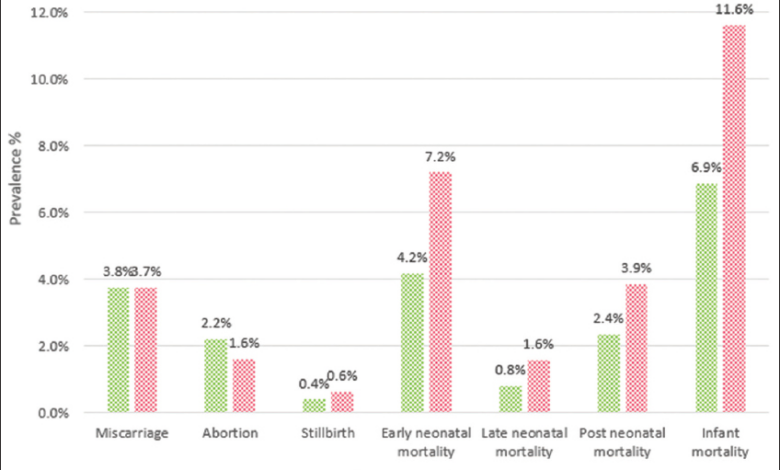
Why Are Indian Women Facing More High-Risk Pregnancies?
Why are indian women facing more high risk pregnancies – Why are Indian women facing more high-risk pregnancies? It’s a question that demands a multifaceted answer, going beyond simple statistics. This isn’t just about numbers; it’s about the interwoven threads of socioeconomic disparities, healthcare access, cultural practices, and underlying health conditions that paint a complex picture of maternal health in India. We’ll delve into the realities faced by countless women, exploring the challenges and potential solutions.
From the stark realities of poverty limiting access to prenatal care to the subtle yet significant impact of cultural beliefs on pregnancy outcomes, we’ll examine the key factors contributing to this alarming trend. We’ll also explore the role of government policies and the potential for improved healthcare models to make a real difference in the lives of pregnant women across India.
Socioeconomic Factors Contributing to High-Risk Pregnancies
High-risk pregnancies in India are significantly influenced by a complex interplay of socioeconomic factors. These factors often act in concert, creating a cycle of disadvantage that disproportionately affects women from lower socioeconomic strata. Addressing these underlying issues is crucial for improving maternal and child health outcomes.
Poverty and Access to Prenatal Care
Poverty acts as a major barrier to accessing adequate prenatal care. Limited financial resources prevent women from affording essential services like regular check-ups, antenatal testing (including for conditions like gestational diabetes and hypertension), and skilled birth attendance. The cost of transportation to healthcare facilities, especially in rural areas, also poses a significant hurdle. This lack of access leads to delayed or missed diagnoses of potential complications, increasing the likelihood of high-risk pregnancies and adverse outcomes.
For example, a woman living in a remote village might need to travel for several hours to reach the nearest health center, a journey that is both costly and time-consuming, potentially hindering timely interventions.
Impact of Malnutrition on Maternal and Fetal Health
Malnutrition, both undernutrition and micronutrient deficiencies, significantly impacts maternal and fetal health. Undernourished mothers are more prone to anemia, which increases the risk of premature birth, low birth weight, and postpartum hemorrhage. Deficiencies in essential vitamins and minerals, such as iron, folic acid, and iodine, can lead to birth defects and developmental problems in the child. The long-term consequences of malnutrition can extend beyond pregnancy, affecting the child’s physical and cognitive development.
A mother suffering from severe anemia, for instance, may experience complications during labor and delivery, leading to a high-risk pregnancy.
Influence of Education Level on Pregnancy Outcomes
A woman’s education level is strongly correlated with pregnancy outcomes. Higher levels of education are associated with better health-seeking behaviors, improved understanding of prenatal care, and greater awareness of risk factors. Educated women are more likely to seek timely medical attention, adopt healthy lifestyle choices during pregnancy, and adhere to recommended healthcare practices. Conversely, women with limited education may lack the knowledge and resources to manage pregnancy-related complications effectively.
For instance, a woman with limited literacy might struggle to understand instructions on medication or follow-up appointments, potentially leading to poor pregnancy outcomes.
Pregnancy Risks in Rural vs. Urban Areas
Rural women in India face significantly higher risks during pregnancy compared to their urban counterparts. Access to quality healthcare is significantly limited in rural areas, leading to a higher incidence of complications and maternal mortality. Poor sanitation, limited access to clean water, and inadequate nutrition further exacerbate these challenges. Urban women, while having better access to healthcare facilities, still face challenges related to stress, pollution, and unhealthy lifestyles, which can contribute to high-risk pregnancies.
The disparity in healthcare infrastructure and access is a crucial factor determining pregnancy outcomes. For example, a rural woman might have to rely on traditional birth attendants with limited medical training, whereas an urban woman is more likely to have access to qualified obstetricians and modern healthcare facilities.
Socioeconomic Indicators and High-Risk Pregnancies
| Socioeconomic Indicator | Impact on High-Risk Pregnancies | Example | Consequences |
|---|---|---|---|
| Poverty | Reduced access to prenatal care, malnutrition | Inability to afford regular check-ups or nutritious food. | Premature birth, low birth weight, infections |
| Malnutrition | Anemia, weakened immune system, birth defects | Iron deficiency leading to anemia in the mother. | Postpartum hemorrhage, infant mortality |
| Low Education Level | Lack of awareness about prenatal care, poor health-seeking behavior | Inability to understand health instructions or recognize warning signs. | Delayed diagnosis of complications, adverse pregnancy outcomes |
| Rural Residence | Limited access to healthcare facilities, poor sanitation | Long distances to health centers, reliance on traditional birth attendants. | Higher maternal and infant mortality rates |
Healthcare Access and Quality
The disparity in healthcare access and quality across India significantly contributes to the high rate of high-risk pregnancies. While significant strides have been made in expanding healthcare infrastructure, persistent challenges remain, particularly in reaching rural and marginalized communities. These challenges often intersect with socioeconomic factors, creating a complex web of obstacles for pregnant women seeking adequate care.The availability of maternal healthcare services varies drastically across India’s diverse landscape.
Urban areas generally boast better access to hospitals, qualified doctors, and advanced medical technologies compared to rural regions. This disparity is exacerbated by geographical barriers, poor infrastructure (lack of roads, transportation), and the concentration of skilled healthcare professionals in urban centers. This uneven distribution creates a significant disadvantage for women in rural areas, who often face long distances to reach healthcare facilities, potentially delaying or preventing them from accessing crucial prenatal and postnatal care.
Challenges in Accessing Qualified Medical Professionals
Many women, especially in rural areas, face significant challenges in accessing qualified medical professionals. The shortage of trained obstetricians, gynecologists, and midwives is a critical issue. This shortage is particularly acute in remote and underserved regions, leading to a reliance on less qualified healthcare providers, potentially increasing the risk of complications during pregnancy and childbirth. Furthermore, language barriers, cultural sensitivities, and a lack of awareness about available services can also hinder access to qualified care.
The financial burden of seeking care from qualified professionals, including consultation fees and travel costs, also presents a significant barrier for many women from lower socioeconomic backgrounds. For instance, a woman living in a remote village might have to travel for days to reach a qualified doctor, incurring significant expenses in the process, making access to quality care financially prohibitive.
Quality of Prenatal Care in Different Regions
The quality of prenatal care varies significantly across different regions of India. While urban areas often have access to advanced diagnostic tools and specialized care, the quality of care in rural areas is often compromised due to a lack of resources, skilled personnel, and infrastructure. This translates to inadequate monitoring of pregnancy-related complications, delayed or missed diagnoses, and suboptimal management of high-risk pregnancies.
Furthermore, the quality of care can also be affected by factors such as poor hygiene standards, inadequate sanitation facilities, and a lack of essential medicines in healthcare facilities. A lack of awareness about the importance of regular prenatal check-ups further contributes to poor pregnancy outcomes. For example, a woman in a rural area might receive only basic antenatal care, missing crucial screenings and interventions that could prevent complications.
A Hypothetical Improved Healthcare Model
An improved healthcare model should prioritize a multi-pronged approach to address the challenges of healthcare access and quality. This would include:* Increased investment in rural healthcare infrastructure: This involves building more primary healthcare centers and community health clinics in underserved areas, ensuring they are equipped with essential diagnostic tools and medicines.
Strengthening the training and deployment of healthcare professionals This includes increasing the number of trained obstetricians, gynecologists, and midwives, particularly in rural areas, and providing them with ongoing professional development opportunities. Incentivizing healthcare professionals to work in rural areas through attractive salary packages and other benefits would also be crucial.
So many factors contribute to the high rates of high-risk pregnancies among Indian women, from malnutrition to inadequate healthcare access. It’s fascinating to consider how seemingly unrelated research, like the study on whether an eye test can detect dementia risk in older adults – check out this interesting article: can eye test detect dementia risk in older adults – highlights the importance of early detection and preventative measures.
Similarly, early prenatal care is crucial for reducing high-risk pregnancies in India, ensuring better maternal and child health outcomes.
Improved transportation and communication infrastructure Improving road networks and providing reliable transportation options would facilitate access to healthcare facilities. Telemedicine initiatives can also play a crucial role in connecting remote areas with specialists.
Public awareness campaigns Educating women about the importance of prenatal care, available services, and warning signs of complications is vital. This should be conducted in local languages and culturally sensitive ways.
Financial assistance programs Providing financial assistance to women from low-income backgrounds can reduce the financial burden of accessing healthcare services.
Healthcare Infrastructure Gaps
The following points highlight the significant gaps in healthcare infrastructure that contribute to high-risk pregnancies in India:
- A severe shortage of skilled healthcare professionals, especially in rural areas.
- Inadequate infrastructure in many healthcare facilities, including a lack of essential equipment and medicines.
- Poor transportation networks, hindering access to healthcare for women in remote areas.
- Limited access to diagnostic tools and technologies for early detection of complications.
- Inadequate sanitation and hygiene standards in some healthcare facilities.
- Lack of awareness and education about maternal health among women and communities.
- Financial barriers preventing many women from accessing quality healthcare.
Cultural and Traditional Practices: Why Are Indian Women Facing More High Risk Pregnancies
The tapestry of Indian culture is rich and diverse, with traditions and beliefs deeply interwoven into the fabric of daily life. These cultural norms, while often enriching and meaningful, can sometimes inadvertently impact pregnancy outcomes, sometimes negatively. Understanding the interplay between cultural practices and maternal health is crucial for developing effective interventions and improving the well-being of expectant mothers.Cultural beliefs and practices significantly influence pregnancy care-seeking behavior, dietary habits, and the overall management of pregnancy and childbirth.
Some practices, rooted in generations of tradition, may pose unforeseen risks to both the mother and the child. Conversely, strong family support systems, a hallmark of many Indian communities, can provide invaluable emotional and practical assistance during this crucial period. The adoption of modern healthcare practices varies considerably across different socio-economic groups and geographic locations, leading to disparities in maternal health outcomes.
Harmful Traditional Practices and Their Impact
Certain traditional practices prevalent in some Indian communities can significantly increase the risk of complications during pregnancy and childbirth. For instance, the practice of restricting dietary intake during pregnancy, often based on traditional beliefs about maintaining a “balanced” constitution, can lead to nutritional deficiencies affecting both the mother and the developing fetus. Similarly, the delay in seeking professional medical care, often due to reliance on traditional healers or home remedies, can result in delayed diagnosis and treatment of pregnancy-related complications.
The continued practice of female genital mutilation (FGM) in some communities poses severe health risks, including infection, bleeding, and childbirth complications. These practices highlight the urgent need for culturally sensitive educational initiatives that promote evidence-based practices.
Variations in Adoption of Modern Healthcare Practices
The adoption of modern healthcare practices varies widely across different communities in India. Urban, educated women are more likely to seek antenatal care, opt for institutional deliveries, and utilize modern medical interventions compared to their rural counterparts. This disparity is often linked to factors such as accessibility to healthcare facilities, financial constraints, and levels of awareness about the benefits of modern medical care.
For example, in remote villages with limited access to hospitals and qualified healthcare professionals, women may rely on traditional birth attendants, increasing the risk of complications. Bridging this gap requires focused efforts to improve healthcare infrastructure in rural areas, coupled with community-based education programs that emphasize the importance of seeking timely and appropriate medical care.
The Role of Family Support in Pregnancy
Family support plays a crucial role in navigating the challenges of pregnancy, especially in Indian society. The extended family system often provides practical assistance with household chores, childcare, and emotional support. However, the influence of family members on healthcare decisions can be a double-edged sword. While supportive families can encourage timely medical care, overly traditional or interfering family members might discourage the adoption of modern medical interventions, leading to suboptimal outcomes.
Therefore, empowering women to make informed decisions about their healthcare, while respecting the role of family support, is crucial.
Comparative Impact of Cultural Practices on Maternal Health
| Cultural Practice | Impact on Maternal Health | Impact on Fetal Health | Community Prevalence |
|---|---|---|---|
| Restricted Diet during Pregnancy | Nutritional deficiencies, anemia | Low birth weight, preterm birth | High in some rural communities |
| Delay in seeking professional medical care | Untreated infections, delayed diagnosis of complications | Increased risk of mortality and morbidity | High in rural and low-literacy communities |
| Home deliveries without skilled assistance | Increased risk of postpartum hemorrhage, infection | Increased risk of neonatal mortality | High in remote areas with limited healthcare access |
| Female Genital Mutilation (FGM) | Infection, bleeding, obstetric fistula | Increased risk of complications during childbirth | Varying prevalence across different regions |
Medical Factors and Underlying Health Conditions
High-risk pregnancies in India are significantly influenced by a complex interplay of medical factors and underlying health conditions prevalent among the female population. These conditions often pre-date pregnancy and can exacerbate existing vulnerabilities, leading to complications during gestation and delivery. Understanding these factors is crucial for developing effective preventative and interventional strategies.
Prevalence of Anemia and Infections, Why are indian women facing more high risk pregnancies
Anemia, characterized by a deficiency of red blood cells or hemoglobin, is alarmingly common among pregnant women in India. This is often due to iron deficiency, folic acid deficiency, or both. The consequences can be severe, including low birth weight, premature delivery, and even maternal mortality. Infections, such as malaria, tuberculosis, and sexually transmitted infections (STIs), also pose significant threats.
These infections can lead to preterm labor, intrauterine growth restriction, and congenital anomalies in the newborn. Studies have shown that a substantial percentage of pregnant Indian women suffer from one or more of these conditions, highlighting the urgent need for widespread screening and preventative measures. For instance, a study published in theIndian Journal of Medical Research* reported that nearly half of pregnant women in a specific region were anemic.
Similarly, reports from the World Health Organization highlight the significant burden of infectious diseases on maternal and child health in India.
Impact of Pre-existing Health Conditions on Pregnancy Complications
Pre-existing health conditions, such as diabetes, hypertension, heart disease, and kidney disease, dramatically increase the risk of complications during pregnancy. These conditions can worsen during pregnancy, placing both the mother and the fetus at considerable risk. For example, gestational diabetes, a type of diabetes that develops during pregnancy, can lead to macrosomia (large babies), birth injuries, and future health problems for the child.
Similarly, pre-existing hypertension can lead to pre-eclampsia, a dangerous condition characterized by high blood pressure and protein in the urine, which can cause seizures and even death. The management of these pre-existing conditions requires specialized care and monitoring throughout the pregnancy. Furthermore, chronic conditions often necessitate modifications to medication regimens during pregnancy to ensure both maternal and fetal well-being.
Maternal Age and Pregnancy Risk
Maternal age is another crucial factor influencing pregnancy risk. Pregnancies in women under 18 (adolescent pregnancies) and over 35 (advanced maternal age) are associated with increased risks of complications. Adolescent mothers are more likely to experience premature delivery, low birth weight babies, and pregnancy-induced hypertension. Women over 35 face a higher risk of gestational diabetes, pre-eclampsia, and chromosomal abnormalities in the fetus.
These risks are amplified by the presence of other underlying medical conditions. Public health initiatives focusing on family planning and reproductive health education are crucial to address the challenges posed by both adolescent and advanced maternal age pregnancies.
Statistics on Medical Conditions Affecting Pregnant Women
Precise statistics vary across regions and studies, but several key indicators highlight the scale of the problem. The prevalence of anemia during pregnancy in India is estimated to be between 40% and 60%, according to various surveys. Similarly, the prevalence of infections like tuberculosis and malaria, which can severely impact pregnancy outcomes, remains significant in many parts of the country.
So many factors contribute to the alarmingly high rate of high-risk pregnancies among Indian women, from malnutrition and lack of access to healthcare to underlying health conditions. It makes me think about medical advancements, like the incredible news that the fda approves clinical trials for pig kidney transplants in humans , which shows how far we’ve come. But while organ transplantation is a huge leap, addressing the root causes of these high-risk pregnancies in India remains a critical and urgent need.
Data on the prevalence of pre-existing chronic conditions in pregnant women is less readily available on a national scale but is undoubtedly a substantial contributor to high-risk pregnancies. The lack of comprehensive, nationally representative data underscores the need for improved surveillance and data collection systems to better understand and address the challenges faced by pregnant women in India.
Government Policies and Interventions
India’s commitment to improving maternal health is evident in its numerous government policies and programs. However, the effectiveness of these initiatives varies significantly across states and communities, highlighting the need for a more nuanced and targeted approach to address the persistent problem of high-risk pregnancies among Indian women. A comprehensive analysis of existing policies, their implementation, and their impact is crucial for identifying areas requiring improvement.
Effectiveness of Current Maternal Health Policies
The effectiveness of current government policies in improving maternal health is a complex issue. While programs like the National Rural Health Mission (NRHM) and the Janani Suraksha Yojana (JSY) have expanded access to antenatal care, institutional deliveries, and postnatal care, significant challenges remain. These include inconsistent implementation across regions, inadequate infrastructure in rural areas, and a shortage of skilled healthcare providers.
The success of these programs is often dependent on factors like local governance, community engagement, and the availability of resources. For example, JSY, while successful in increasing institutional deliveries, has faced challenges in ensuring the quality of care provided in these institutions. Effective monitoring and evaluation mechanisms are essential to track progress and identify areas needing improvement.
Areas Requiring Policy Improvement
Several areas require significant policy improvements to effectively reduce high-risk pregnancies. Strengthening primary healthcare infrastructure in rural and underserved areas is paramount. This includes investing in more skilled healthcare professionals, improving access to essential medicines and equipment, and ensuring regular training and updates for existing staff. Furthermore, policies should address the underlying social determinants of health, including poverty, malnutrition, and lack of education.
Targeted interventions focusing on adolescent health, nutrition during pregnancy, and access to family planning services are crucial. Improved data collection and analysis are also needed to accurately track progress and inform policy adjustments. A more integrated approach, coordinating efforts across various government departments and involving community stakeholders, is essential for successful implementation.
Impact of Government Programs on Healthcare and Education
Government programs have demonstrably improved access to healthcare and education, albeit unevenly. The NRHM, for instance, has expanded the reach of primary healthcare services to remote areas, leading to increased antenatal check-ups and institutional deliveries. Similarly, initiatives promoting girls’ education have indirectly contributed to better maternal health outcomes by empowering women to make informed decisions about their reproductive health.
However, the impact is not uniform. Disparities persist between urban and rural areas, and among different socioeconomic groups. Furthermore, the quality of care provided often varies, and access to specialized services remains a challenge in many areas. Addressing these disparities requires targeted interventions and a commitment to equitable resource allocation.
Comparison of Government Initiatives Across States
Government initiatives aimed at reducing high-risk pregnancies vary considerably across Indian states. Some states have implemented innovative programs focused on community health workers, while others have prioritized strengthening existing healthcare infrastructure. For example, Kerala has consistently demonstrated strong maternal health indicators, partly due to its robust public health system and high literacy rates. In contrast, states with lower socioeconomic indicators and weaker healthcare infrastructure often grapple with higher rates of high-risk pregnancies and maternal mortality.
This variation highlights the need for a flexible approach that tailors interventions to the specific needs and context of each state. Sharing best practices and lessons learned across states is crucial for improving nationwide maternal health outcomes.
Summary of Government Policies and Their Impact
| Policy | Objective | Impact | Challenges |
|---|---|---|---|
| Janani Suraksha Yojana (JSY) | Reduce maternal mortality by promoting institutional deliveries | Increased institutional deliveries, but quality of care remains inconsistent | Implementation challenges, inadequate infrastructure in rural areas |
| National Rural Health Mission (NRHM) | Improve access to primary healthcare in rural areas | Expanded access to antenatal and postnatal care, but disparities persist | Shortage of skilled healthcare providers, uneven implementation |
| National Health Mission (NHM) | Improve overall health indicators, including maternal health | Improved access to healthcare services, but challenges in quality and equity remain | Funding constraints, capacity building challenges |
| Pradhan Mantri Jan Arogya Yojana (PM-JAY) | Provide health insurance coverage to vulnerable populations | Increased access to healthcare services for eligible beneficiaries | Coverage gaps, challenges in claim processing |
Illustrative Case Studies
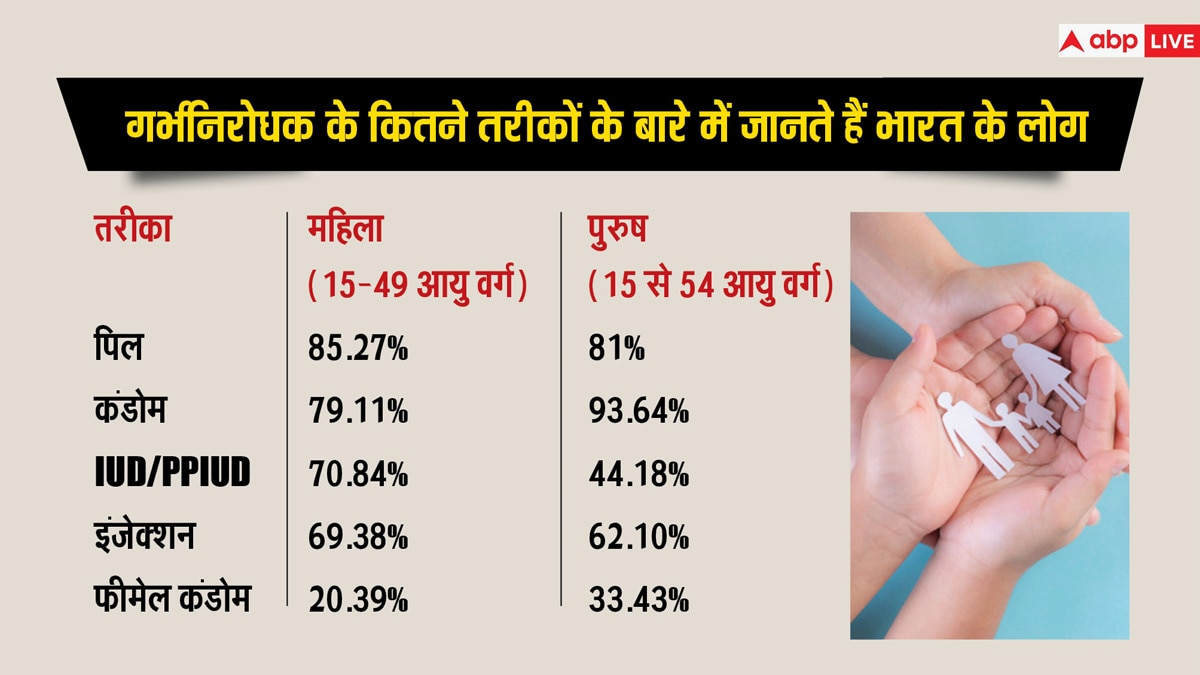
Source: abplive.com
Understanding the complexities of high-risk pregnancies in India requires looking beyond statistics. Real-life examples illuminate the challenges faced by women and the impact of various factors on pregnancy outcomes. The following case studies offer a glimpse into these realities.
Case Study 1: Challenges Faced During a High-Risk Pregnancy
Lakshmi, a 28-year-old woman from a rural village in Uttar Pradesh, faced a high-risk pregnancy due to gestational diabetes and pre-eclampsia. She and her husband are subsistence farmers, living below the poverty line. Access to healthcare was severely limited; the nearest functioning health center was a two-hour journey away by bus, a significant barrier given her condition. Her limited education and understanding of her pregnancy complications hindered effective self-management.
So many factors contribute to the high rates of high-risk pregnancies among Indian women, from nutritional deficiencies to limited access to healthcare. It’s a complex issue, and sometimes I find myself thinking about how managing chronic conditions in children impacts families – for example, learning about effective strategies to manage Tourette syndrome in children highlights the importance of early intervention and support systems.
This need for proactive care is mirrored in the fight to improve maternal health outcomes in India, requiring similar focused efforts on prevention and access to quality care.
Initial symptoms were dismissed as normal pregnancy discomfort. The delay in seeking proper medical attention led to complications during labor, resulting in a premature birth. The baby, though surviving, required extensive neonatal care, incurring further financial strain on the family. Lakshmi’s experience highlights the intertwined issues of poverty, geographical isolation, and limited health literacy contributing to adverse pregnancy outcomes.
The financial burden of medical expenses further exacerbated her already precarious situation, emphasizing the socio-economic vulnerabilities faced by many Indian women.
Case Study 2: Successful Intervention and Improved Outcome
Priya, a 32-year-old teacher from Mumbai, experienced a high-risk pregnancy due to a previous cesarean section and a history of hypertension. However, her outcome differed significantly from Lakshmi’s. Priya had access to quality healthcare through a private health insurance plan provided by her employer. She received regular prenatal checkups, including ultrasounds and specialized monitoring for hypertension. Her doctor proactively addressed her concerns and educated her about managing her condition.
She also benefited from a supportive network of family and friends, enabling her to prioritize her health and reduce stress. The consistent monitoring and proactive management prevented complications, resulting in a healthy full-term delivery through a planned cesarean section. Priya’s case demonstrates the positive impact of access to quality healthcare, comprehensive prenatal care, and a strong support system in achieving a favorable outcome in high-risk pregnancies.
Her story underscores the crucial role of socioeconomic stability and access to resources in mitigating risks associated with high-risk pregnancies.
Final Wrap-Up
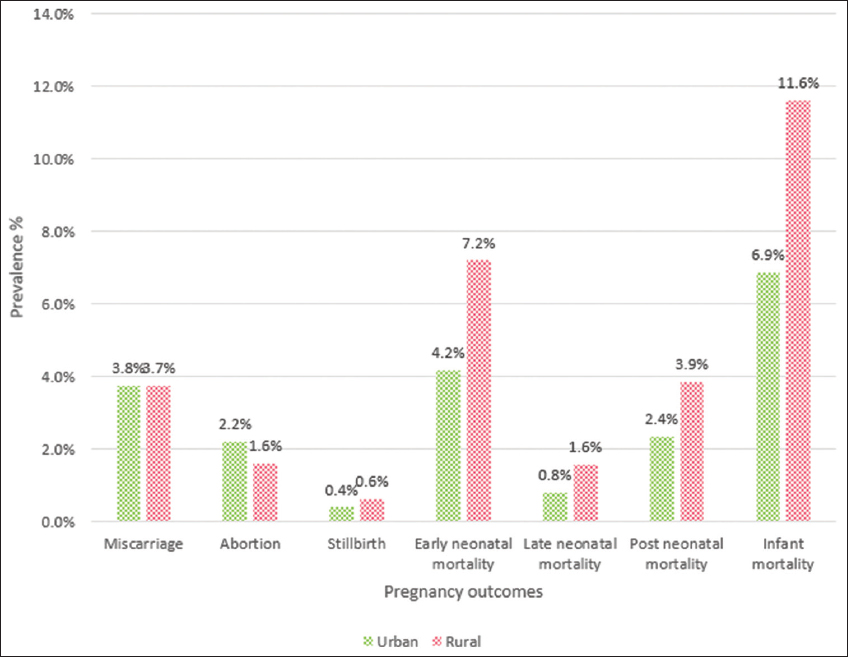
Source: mchandaids.org
The issue of high-risk pregnancies among Indian women is a deeply concerning one, demanding immediate and comprehensive action. While the challenges are significant, ranging from socioeconomic inequalities to healthcare deficiencies and cultural practices, there is hope. By addressing these factors head-on through improved healthcare access, targeted interventions, and empowering women with knowledge and resources, we can work towards a future where every pregnancy is a safe and healthy journey for both mother and child.
The fight for maternal health in India is a fight for the future.
FAQ Overview
What are some common medical conditions contributing to high-risk pregnancies in India?
Anemia, infections (like HIV and tuberculosis), gestational diabetes, and hypertension are prevalent and significantly increase pregnancy risks.
How does malnutrition affect pregnancy outcomes?
Malnutrition weakens the mother’s body, leading to complications like premature birth, low birth weight, and increased risk of infections for both mother and baby.
Are there specific government initiatives aimed at reducing high-risk pregnancies?
Yes, India has several national programs focusing on maternal and child health, but their effectiveness varies across regions due to implementation challenges.
What role does family support play in managing high-risk pregnancies?
Strong family support provides crucial emotional, physical, and financial assistance, improving the chances of a positive outcome.