Ulcerative Colitis Bloating Causes & Management
Why does ulcerative colitis cause bloating and how to manage it? That’s the burning question many of us with UC grapple with. The constant discomfort, the unpredictable swelling – it’s a real struggle. This post dives deep into understanding the link between ulcerative colitis and bloating, exploring the underlying inflammation, dietary triggers, and effective management strategies. We’ll look at everything from tweaking your diet to exploring medication options and making crucial lifestyle changes to ease the discomfort.
We’ll cover the science behind the bloating, looking at how inflammation in the colon affects your digestive system and how this leads to that uncomfortable feeling of fullness. We’ll also delve into practical solutions – from identifying food culprits to learning stress-management techniques – all designed to help you take control of your symptoms and improve your quality of life.
Understanding Ulcerative Colitis and its Relation to Bloating
Ulcerative colitis (UC) is a chronic inflammatory bowel disease (IBD) that primarily affects the large intestine (colon) and rectum. It’s characterized by inflammation and ulceration of the innermost lining of the bowel, leading to a range of symptoms, with bloating being a prominent one. Understanding the inflammatory process and its effects on the digestive system is key to managing this debilitating condition.
The Inflammatory Process in Ulcerative Colitis and its Impact on Digestion
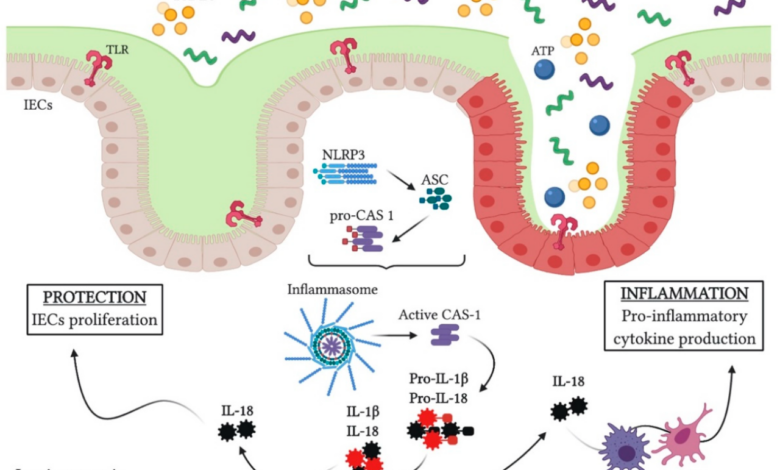
Ulcerative colitis involves a complex interplay of genetic predisposition, environmental factors, and an abnormal immune response. The immune system mistakenly attacks the lining of the colon, causing inflammation. This inflammation leads to swelling, irritation, and damage to the bowel wall. The affected area becomes inflamed, leading to increased permeability of the intestinal lining. This allows bacteria, gases, and other substances to pass more easily into the surrounding tissues, contributing to discomfort and bloating.
The inflammation also disrupts normal bowel movements, leading to changes in stool frequency and consistency. The colon’s ability to absorb water effectively is impaired, resulting in looser stools and increased frequency of bowel movements.
Mechanisms Linking Colon Inflammation to Bloating
Several mechanisms contribute to bloating in individuals with UC. Firstly, the inflammation itself causes swelling in the colon, reducing its capacity and leading to a feeling of fullness and distension. Secondly, impaired motility – the movement of food through the digestive tract – can lead to gas accumulation and bloating. The inflammation can slow down the movement of food and waste through the colon, allowing more time for gas to build up.
Thirdly, the increased permeability of the intestinal lining, as mentioned earlier, allows for increased bacterial fermentation, producing more gas which contributes to the sensation of bloating. Finally, changes in the gut microbiome composition, often observed in UC, can further exacerbate gas production and bloating.
Comparison of UC-Related Bloating with Bloating from Other Causes
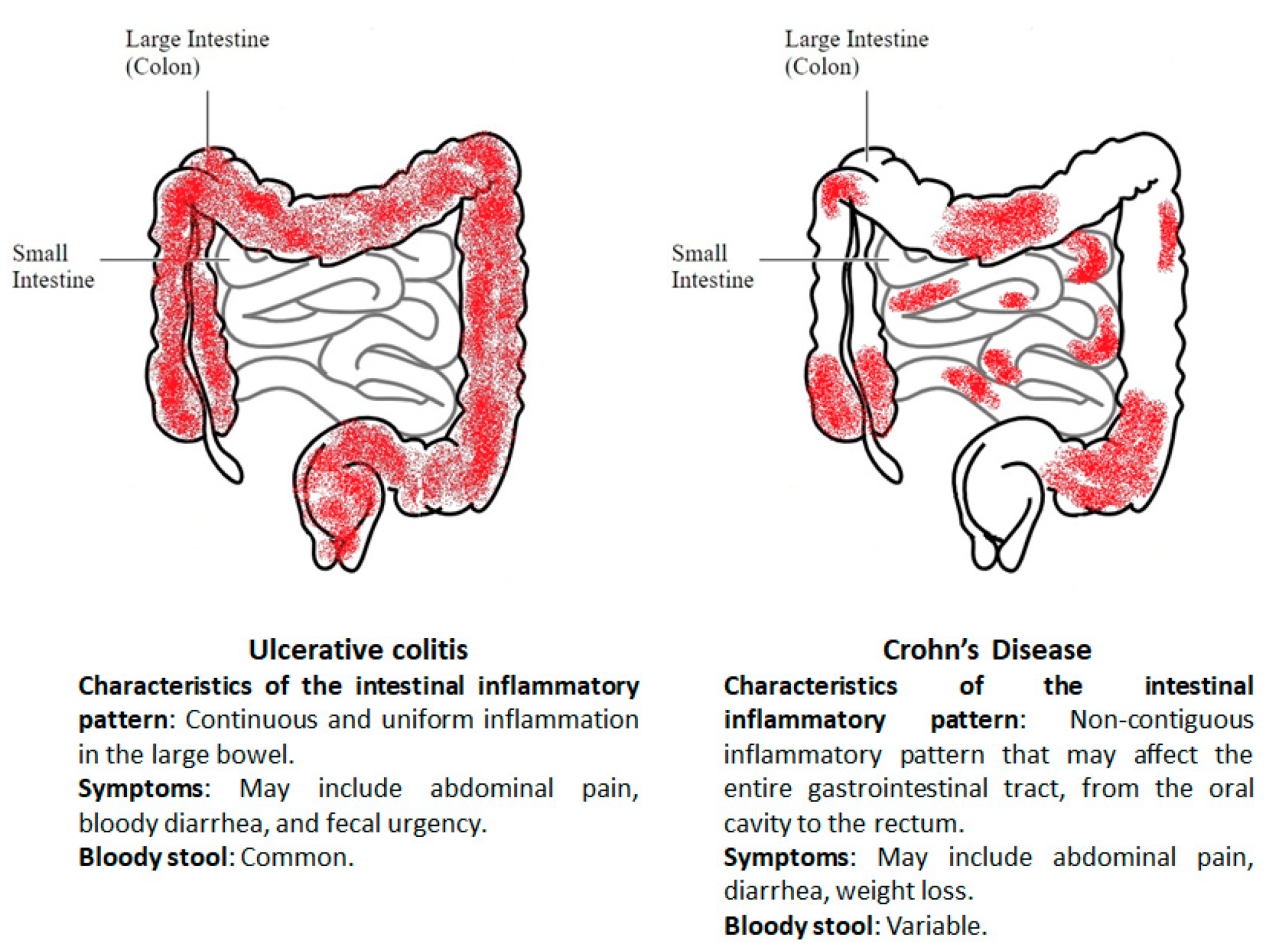
Bloating is a common symptom across many gastrointestinal conditions, making it crucial to differentiate UC-related bloating from other causes. While bloating from UC is often accompanied by other symptoms like bloody diarrhea, abdominal pain, and urgency, bloating from conditions like irritable bowel syndrome (IBS) or lactose intolerance might not necessarily involve these additional symptoms. UC-related bloating tends to be more persistent and severe, often worsening during flares of the disease.
Bloating from food intolerances or constipation is usually more episodic and often resolves with dietary adjustments or increased fiber intake. A proper diagnosis from a healthcare professional is crucial to determine the underlying cause of bloating and initiate appropriate treatment.
Common Symptoms of Ulcerative Colitis
It is important to note that the severity and frequency of these symptoms can vary significantly between individuals and depend on the stage and activity of the disease.
| Symptom | Description | Severity | Frequency |
|---|---|---|---|
| Bloating | Feeling of fullness or distension in the abdomen | Mild to severe | Intermittent to constant |
| Abdominal Pain | Cramping, sharp, or persistent pain in the abdomen | Mild to severe | Intermittent to constant |
| Diarrhea | Frequent, loose, or watery stools | Mild to severe | Several times a day to many times a day |
| Rectal Bleeding | Presence of blood in the stool | Mild to severe | Intermittent to constant |
Dietary Factors Contributing to Bloating in Ulcerative Colitis
Managing bloating when you have ulcerative colitis can feel like navigating a minefield. What you eat plays a huge role in your comfort level, and understanding which foods are likely to trigger bloating is crucial for managing your symptoms. This section will explore the dietary aspects that contribute to bloating and provide practical strategies to minimize its impact.
Common Food Triggers for Bloating in Ulcerative Colitis
Many foods can trigger bloating in individuals with ulcerative colitis. These vary from person to person, but some common culprits include dairy products (due to lactose intolerance, which is common in UC patients), cruciferous vegetables (like broccoli, cauliflower, and cabbage) because of their high fiber content which can be difficult to digest during a flare, and certain high-FODMAP foods (explained below).
Processed foods, sugary drinks, and excessive caffeine can also contribute to increased gas and bloating. It’s important to keep a food diary to identify your personal triggers.
The Role of Fiber in Managing Bloating
Fiber is essential for digestive health, but its impact on bloating in ulcerative colitis is complex. The key lies in differentiating between soluble and insoluble fiber. Soluble fiber dissolves in water, forming a gel-like substance that can help regulate bowel movements and soften stools. This type of fiber is generally better tolerated by those with UC. Insoluble fiber, on the other hand, doesn’t dissolve and can add bulk to the stool, potentially exacerbating bloating and discomfort in individuals with already sensitive digestive systems.
Finding the right balance is crucial.
The Importance of a Low-FODMAP Diet for Reducing Bloating
A low-FODMAP diet focuses on eliminating foods high in fermentable oligosaccharides, disaccharides, monosaccharides, and polyols (FODMAPs). These short-chain carbohydrates are poorly absorbed in the small intestine, leading to fermentation by gut bacteria, which can result in gas, bloating, and abdominal pain. Many individuals with UC find that reducing FODMAPs significantly improves their bloating. This isn’t a long-term dietary solution for everyone, but it can be a very effective tool for managing symptoms during flare-ups.
It’s essential to work with a registered dietitian or gastroenterologist to ensure a balanced and nutritionally adequate low-FODMAP diet.
Sample Low-Bloating Meal Plan for Ulcerative Colitis
This is a sample meal plan and may need adjustments based on individual needs and tolerances. It emphasizes easily digestible foods low in FODMAPs and insoluble fiber. Remember to always consult with your doctor or a registered dietitian before making significant dietary changes, especially if you have a chronic condition like ulcerative colitis.
- Breakfast: Oatmeal made with water (not milk), topped with a small amount of berries (low FODMAP options like blueberries or raspberries).
- Lunch: Chicken salad sandwich on gluten-free bread (if gluten is a trigger) with lettuce and tomato. Avoid high-fat dressings.
- Dinner: Baked salmon with roasted sweet potatoes and a small portion of green beans (cooked until tender).
- Snacks: Rice cakes with avocado, a small portion of plain yogurt (if tolerated), or a handful of almonds (in moderation).
Medication and Treatment Strategies for Bloating Management: Why Does Ulcerative Colitis Cause Bloating And How To Manage It
Managing bloating associated with ulcerative colitis often requires a multi-pronged approach focusing on controlling inflammation and improving gut health. This involves medication, dietary changes, and sometimes, lifestyle adjustments. Let’s delve into the specifics of medication and treatment strategies.
Anti-inflammatory Medications
Anti-inflammatory drugs are cornerstones of ulcerative colitis treatment. By reducing inflammation in the digestive tract, these medications can significantly alleviate symptoms, including bloating. The most common types include aminosalicylates (like mesalamine), corticosteroids (like prednisone), and biologics (like infliximab or adalimumab). Aminosalicylates work locally in the gut to reduce inflammation, often with fewer systemic side effects than other options.
Corticosteroids are potent anti-inflammatories, but their use is usually short-term due to potential side effects. Biologics target specific parts of the immune system to dampen the inflammatory response, offering long-term disease management for many patients. It’s crucial to remember that these medications should only be taken under the strict supervision of a gastroenterologist.
Probiotics and Prebiotics
Maintaining a healthy gut microbiome is vital for managing ulcerative colitis and reducing bloating. Probiotics, which are live microorganisms, can help restore the balance of beneficial bacteria in the gut. Prebiotics, on the other hand, are non-digestible food ingredients that act as fuel for these beneficial bacteria. While research on the effectiveness of probiotics and prebiotics in UC is ongoing, many individuals find them helpful in managing symptoms like bloating.
Always discuss probiotic and prebiotic use with your doctor to ensure they are appropriate for your specific situation and don’t interfere with any other medications you are taking. For example, certain strains of
- Lactobacillus* and
- Bifidobacterium* are often recommended. However, it’s crucial to choose reputable brands with verified strains.
Medication Comparison Table
The effectiveness and side effects of medications vary greatly depending on the individual and the severity of their condition. It’s vital to work closely with your doctor to determine the best treatment plan for you.
| Medication Type | Mechanism of Action | Effectiveness in Reducing Bloating | Common Side Effects |
|---|---|---|---|
| Aminosalicylates (e.g., mesalamine) | Reduces inflammation in the gut | Moderate to high, depending on individual response and disease severity | Nausea, abdominal cramps, headache |
| Corticosteroids (e.g., prednisone) | Potent anti-inflammatory effect | High, but often short-term use due to side effects | Weight gain, increased blood sugar, mood changes, osteoporosis (with long-term use) |
| Biologics (e.g., infliximab, adalimumab) | Targets specific immune system components | High, particularly for moderate to severe UC | Infections, infusion reactions, increased risk of certain cancers (rare) |
| Probiotics/Prebiotics | Improves gut microbiome balance | Variable, often mild to moderate improvement | Generally well-tolerated, but potential for mild gastrointestinal discomfort in some individuals |
Lifestyle Changes for Reducing Bloating in Ulcerative Colitis
Living with ulcerative colitis (UC) often means navigating a complex interplay of factors that contribute to uncomfortable symptoms, including bloating. While medication and diet play crucial roles in management, incorporating specific lifestyle changes can significantly impact your overall well-being and reduce bloating episodes. These changes aren’t quick fixes, but rather sustainable practices that, when consistently implemented, can lead to noticeable improvements in your gut health and overall quality of life.
Stress Management Techniques for Bloating Reduction
Stress significantly impacts the gut-brain axis, a complex communication system between your brain and intestines. When you’re stressed, your body releases hormones that can exacerbate inflammation and digestive issues, leading to increased bloating. Effective stress management techniques are therefore crucial for managing UC symptoms. Practicing relaxation methods like deep breathing exercises, yoga, or meditation can help regulate your nervous system and reduce stress hormones, thereby potentially lessening bloating.
Mindfulness practices, focusing on the present moment without judgment, can also help manage stress responses. Consider incorporating these techniques into your daily routine for long-term benefits.
Regular Exercise Benefits for Gut Health and Symptom Management
Regular physical activity isn’t just good for your heart; it also positively influences your gut health. Exercise helps stimulate bowel movements, improving regularity and potentially reducing bloating caused by constipation, a common UC symptom. Moderate-intensity activities like brisk walking, swimming, or cycling are particularly beneficial. Aim for at least 30 minutes of moderate-intensity exercise most days of the week.
Remember to listen to your body and adjust your exercise routine based on your energy levels and symptoms. Consult your doctor before starting any new exercise program, especially if you are experiencing a flare-up.
Adequate Hydration for Preventing and Alleviating Bloating
Staying properly hydrated is essential for overall health and plays a significant role in managing UC symptoms. Water helps regulate bowel movements, preventing constipation, which is a major contributor to bloating. Adequate hydration also helps to soften stool, making it easier to pass. Aim for at least eight glasses of water per day, and consider incorporating other hydrating fluids like herbal teas (avoid caffeine, which can exacerbate symptoms) and clear broths.
Dehydration can worsen bloating, so pay close attention to your fluid intake, especially during warmer months or if you’re experiencing diarrhea.
Lifestyle Modifications for Improved UC Symptoms
Making several key lifestyle adjustments can contribute significantly to better UC symptom management and reduced bloating. These modifications often work synergistically, meaning their combined effect is greater than the sum of their individual impacts.
- Prioritize Regular Sleep: Aim for 7-9 hours of quality sleep per night. Lack of sleep can worsen inflammation and disrupt the gut microbiome, potentially leading to increased bloating and other digestive issues. Establish a consistent sleep schedule and create a relaxing bedtime routine to promote better sleep quality.
- Quit Smoking: Smoking is a known risk factor for inflammatory bowel disease (IBD) and can worsen symptoms. Quitting smoking can significantly improve your overall health and potentially reduce bloating and other UC symptoms. Seek support from your doctor or utilize resources available to help you quit.
- Maintain a Healthy Weight: Obesity is associated with increased inflammation, and managing your weight can be beneficial for UC symptom management. Focus on a balanced diet and regular exercise to maintain a healthy weight.
When to Seek Medical Attention for Bloating
Source: mdpi.com
Bloating is a common symptom of ulcerative colitis (UC), but it’s crucial to understand when that bloating signals something more serious requiring immediate medical attention. While some bloating is manageable with lifestyle changes and medication, certain signs indicate a worsening of your UC or potential complications. Ignoring these warning signs can have serious consequences, so it’s vital to know when to contact your doctor.Severe or persistent bloating, especially when accompanied by other symptoms, necessitates a prompt visit to your gastroenterologist.
This proactive approach helps ensure timely diagnosis and treatment, potentially preventing more serious health issues. Regular check-ups are also essential for ongoing management and early detection of any complications.
Warning Signs Requiring Immediate Medical Attention
Several warning signs indicate a possible worsening of UC or the development of complications. These necessitate immediate medical attention. Delaying treatment can lead to severe consequences, including hospitalization.
- Severe abdominal pain that doesn’t respond to usual pain relief measures.
- Bloody or black, tarry stools, indicating significant bleeding.
- High fever (above 101°F or 38.3°C) accompanied by chills.
- Rapid or irregular heartbeat.
- Signs of dehydration, such as decreased urination, dizziness, or lightheadedness.
- Severe persistent vomiting that prevents you from keeping down fluids or medication.
- Significant weight loss without trying.
Scenarios Requiring a Doctor’s Visit, Why does ulcerative colitis cause bloating and how to manage it
Even without the above severe symptoms, there are scenarios where bloating warrants a doctor’s visit. Don’t hesitate to seek medical advice if your bloating is significantly impacting your quality of life.
- Bloating that is significantly worse than usual, even with medication and lifestyle adjustments.
- Bloating accompanied by persistent diarrhea, even if it’s not bloody.
- Bloating that is accompanied by significant fatigue or weakness.
- Bloating that interferes with your daily activities or sleep.
- New onset of severe bloating after a period of remission.
The Importance of Regular Check-ups
Regular check-ups with your gastroenterologist are crucial for managing UC and preventing complications. These appointments allow your doctor to monitor your condition, adjust medication as needed, and address any emerging concerns, including persistent bloating. This proactive approach helps to maintain your overall health and well-being. For example, regular blood tests can help monitor inflammation levels and identify potential problems early.
Communicating Effectively with Your Healthcare Provider
Effective communication is key to successful UC management. When discussing bloating with your doctor, be prepared to provide detailed information. This includes:
- The duration and severity of your bloating.
- Any other symptoms you’re experiencing.
- Recent dietary changes.
- Your current medication regimen.
- Any lifestyle changes you’ve made.
Keeping a symptom diary can be incredibly helpful in tracking your symptoms and communicating effectively with your doctor. This detailed record allows your doctor to identify patterns and trends that might otherwise be missed. For instance, noting the timing of bloating in relation to meals or medication can be particularly valuable.
Last Word
Source: mdpi.com
Living with ulcerative colitis and the associated bloating can be challenging, but it’s definitely manageable. By understanding the root causes – the inflammation, the dietary triggers, and the impact of stress – we can arm ourselves with the knowledge and tools to navigate this condition more effectively. Remember, this isn’t just about managing symptoms; it’s about improving your overall well-being.
Don’t hesitate to reach out to your doctor for personalized advice and support – you deserve to feel your best.
FAQ Resource
Can stress worsen ulcerative colitis bloating?
Yes, stress can significantly exacerbate UC symptoms, including bloating. Stress hormones can increase inflammation in the gut.
Are there specific probiotics that help with UC bloating?
Some studies suggest certain probiotics may be beneficial, but it’s crucial to discuss this with your doctor before starting any probiotic regimen as individual responses vary greatly.
How long does it take to see improvement after dietary changes for UC bloating?
This varies greatly depending on the individual and the severity of their condition. Some people see improvements within weeks, while others may take longer. Patience and consistency are key.
What are the potential side effects of medication for UC bloating?
Side effects vary depending on the medication. Common side effects can include nausea, diarrhea, and headaches. It’s crucial to discuss potential side effects with your doctor.