The Trap of Extended Prescriptions: Unraveling the Polypharmacy Crisis in the Elderly
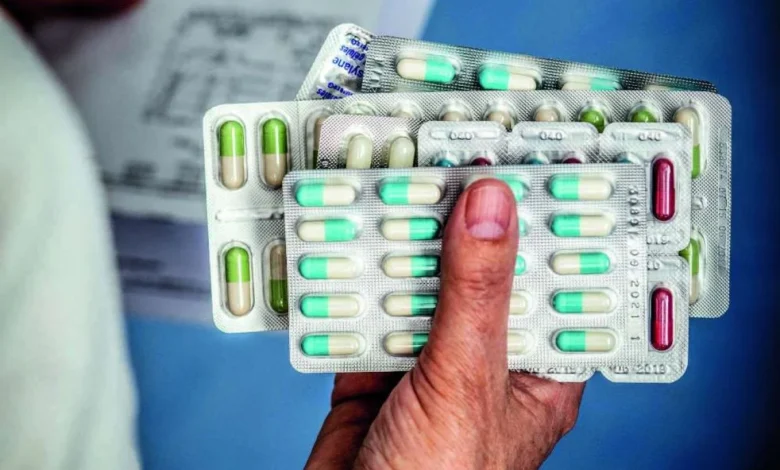
The widespread accumulation of medical treatments among older individuals has become a pervasive norm, transforming into a significant and often underestimated public health challenge. While each medication is individually intended to improve patient health, the simultaneous administration of multiple molecules, frequently prescribed by various practitioners, exposes seniors to a complex web of unforeseen adverse effects, dangerous drug-drug interactions, and a troubling rise in preventable hospitalizations. This critical issue, often termed polypharmacy, remains inadequately controlled, demanding urgent and comprehensive strategies to better manage the intricate medication regimens of our aging population. A recent investigation by Sciences et Avenir in its May 2026 issue (N°951), featuring an article by Marie-Cécilia Duvernoy, delves into the depths of this escalating crisis, highlighting the imperative for re-evaluating prescribing practices and patient care models.
Understanding the "Long Prescription" Trap: A Growing Public Health Crisis
Polypharmacy, broadly defined as the regular use of multiple medications, often five or more, is particularly prevalent among the elderly due to their increased likelihood of suffering from multiple chronic conditions, or multimorbidity. Conditions such as cardiovascular disease, diabetes, arthritis, osteoporosis, and various neurological disorders frequently coexist, leading to specialists prescribing drugs to manage individual ailments without always a holistic view of the patient’s entire medication list. This fragmented approach can inadvertently lead to a "prescribing cascade," where side effects of one drug are mistakenly treated with another, further expanding the prescription list.
The physiological changes associated with aging significantly alter how the body processes medications. Reduced kidney and liver function, changes in body composition (less muscle, more fat), and altered drug receptor sensitivity mean that older adults metabolize and excrete drugs differently than younger individuals. This makes them inherently more susceptible to adverse drug reactions (ADRs) and drug-drug interactions (DDIs), which can manifest in a myriad of ways, from mild discomfort to life-threatening events. For instance, a seemingly innocuous combination of an antidepressant and a diuretic, along with a medication for blood pressure, can lead to dangerous electrolyte imbalances or orthostatic hypotension, increasing the risk of falls—a leading cause of injury and mortality in seniors.
The Silent Threat: Mechanisms and Risks in the Elderly
The risks associated with polypharmacy extend far beyond simple side effects. They encompass a spectrum of clinical challenges that profoundly impact the health and quality of life of older adults.
-
Adverse Drug Reactions (ADRs): These are unintended and harmful reactions to a medication. In the elderly, ADRs are a major cause of hospital admissions. Common ADRs linked to polypharmacy include:
- Falls: Sedatives, antipsychotics, antidepressants, and blood pressure medications can cause dizziness, impaired balance, and hypotension, significantly increasing fall risk.
- Cognitive Impairment: Anticholinergic drugs (found in many medications for allergies, sleep, and bladder control), benzodiazepines, and some pain relievers can exacerbate or induce confusion, delirium, and memory problems, mimicking or worsening dementia symptoms.
- Gastrointestinal Issues: Non-steroidal anti-inflammatory drugs (NSAIDs) combined with anticoagulants can heighten the risk of gastrointestinal bleeding.
- Renal Dysfunction: Multiple drugs processed by the kidneys can accumulate to toxic levels if renal function is compromised, a common occurrence in older age.
- Cardiovascular Events: Certain drug combinations can affect heart rhythm or blood pressure regulation, leading to arrhythmias or hypertensive crises.
-
Drug-Drug Interactions (DDIs): When two or more drugs interact, their effects can be altered. DDIs can lead to:
- Synergistic Toxicity: Where the combined effect of drugs is greater than the sum of their individual effects, leading to overdose-like symptoms.
- Antagonism: Where one drug reduces or cancels the effect of another, rendering treatments ineffective.
- Altered Pharmacokinetics/Pharmacodynamics: Drugs can influence how other drugs are absorbed, distributed, metabolized, or excreted, or how they interact with cellular targets, leading to unpredictable concentrations and responses.
-
Reduced Treatment Adherence: Complex medication regimens, often involving multiple pills taken at different times of the day, can be overwhelming for older patients, especially those with cognitive impairments or dexterity issues. This can lead to missed doses, incorrect dosing, or even abandonment of essential medications, undermining therapeutic goals.
-
Increased Healthcare Utilization and Costs: Polypharmacy is directly linked to higher rates of emergency department visits, hospitalizations, and readmissions, often due to preventable ADRs. This not only burdens the patient but also places immense strain on healthcare systems, driving up overall medical expenditures.
Unpacking the Causes: Why Polypharmacy Persists
The persistence of polypharmacy is not a simple oversight but rather a multifaceted problem rooted in several systemic and individual factors:

- Multimorbidity: As life expectancy increases, so does the prevalence of multiple chronic diseases in individuals. Each condition typically warrants specific pharmacological interventions, leading to a growing list of prescriptions.
- Multiple Prescribers and Fragmented Care: Patients often see several specialists (cardiologists, endocrinologists, neurologists, etc.) who may not have full visibility into all other medications the patient is taking. A lack of integrated electronic health records or poor communication channels between providers can exacerbate this issue.
- Lack of Regular Medication Reviews: Prescriptions, once initiated, are often continued indefinitely without periodic re-evaluation to assess their ongoing necessity, efficacy, and potential for harm, especially as a patient’s health status changes.
- "Prescribing Cascade": This occurs when a new drug is prescribed to "treat" an adverse effect of an existing drug, rather than recognizing and addressing the initial drug as the cause. For example, a patient might be given a drug for insomnia, when their sleep disturbance is a side effect of another medication they are already taking.
- Patient Expectations and Self-Medication: Patients may expect a pill for every ailment, and some may also use over-the-counter medications, supplements, or herbal remedies without informing their doctors, adding to the complexity of their regimen.
- Lack of Time and Training: Healthcare providers, particularly general practitioners, often face time constraints during consultations, making comprehensive medication reviews challenging. Furthermore, specific training in geriatric pharmacology and deprescribing techniques may not be universally standardized.
Charting the Course: A Chronology of Awareness and Intervention
While polypharmacy has likely existed for decades, its recognition as a significant public health issue requiring dedicated intervention is relatively more recent.
- Early 2000s: Growing awareness in academic and clinical circles regarding the specific vulnerabilities of the elderly to medication-related problems. Initial studies began to quantify the prevalence of polypharmacy and its association with adverse outcomes.
- Mid-2000s: Professional organizations, particularly in geriatrics and pharmacy, started to advocate for medication review processes and the concept of "deprescribing"—the planned and supervised process of dose reduction or stopping of medications that may be causing harm or are no longer beneficial.
- 2010s: Development of explicit criteria for potentially inappropriate medications in the elderly (e.g., Beers Criteria in the US, STOPP/START criteria in Europe) became widely adopted clinical tools to guide prescribers. Research intensified into the effectiveness of pharmacist-led medication reviews and interprofessional team approaches.
- Early 2020s: Integration of electronic health records (EHRs) and clinical decision support systems (CDSS) began to offer technological solutions to flag potential drug interactions and inappropriate prescriptions in real-time. Public health campaigns in several countries aimed at educating both patients and healthcare providers about the risks of polypharmacy.
- Mid-2020s (as of May 2026): Ongoing efforts focus on refining deprescribing guidelines, integrating polypharmacy management into routine primary care, leveraging artificial intelligence for personalized medication risk assessment, and fostering greater collaboration across the healthcare spectrum. The Sciences et Avenir report itself signifies a continued and heightened focus on this issue in mainstream scientific journalism.
Data Speaks: The Alarming Statistics
Statistics underscore the gravity of the polypharmacy crisis. While precise figures vary by region and definition, several trends are consistent:
- Prevalence: Studies consistently show that between 30% and 50% of older adults (aged 65 and above) take five or more medications concurrently. A significant subset, often 10-15%, may be on ten or more. For instance, in France, estimates suggest that a substantial proportion of seniors are on regimens classified as polypharmacy, aligning with broader European trends.
- Hospitalizations: Adverse drug reactions (ADRs) are estimated to account for 5% to 10% of all hospital admissions, with the elderly being disproportionately affected. In some studies, ADRs are cited as a top 5 cause of death.
- Emergency Visits: Polypharmacy is a leading cause of emergency department visits among seniors, often for preventable issues such as falls, confusion, or gastrointestinal bleeding directly attributable to medication side effects or interactions.
- Economic Burden: The financial cost associated with preventable medication-related problems is staggering. Estimates suggest billions of dollars annually are spent on managing ADRs, hospitalizations, and long-term care attributable to inappropriate medication use.
Multifaceted Solutions: Strategies for Better Medication Management
Addressing polypharmacy requires a concerted, multidisciplinary effort involving patients, caregivers, healthcare providers, and policymakers.
- Comprehensive Medication Reviews (CMRs): These are systematic assessments of a patient’s entire medication regimen (prescribed, over-the-counter, supplements) conducted by a pharmacist or physician. The goal is to identify and resolve medication-related problems, simplify regimens, and optimize therapy.
- Deprescribing Initiatives: A structured process of identifying and stopping medications where the potential for harm outweighs the potential benefit. This requires careful consideration of individual patient goals, prognosis, and potential withdrawal effects. Deprescribing is not about denying necessary treatment but about ensuring appropriate and safe medication use.
- Interprofessional Collaboration: Fostering better communication and collaboration among all healthcare providers involved in a patient’s care—general practitioners, specialists, pharmacists, nurses, and caregivers. Integrated care models and regular team meetings can ensure a holistic view of the patient’s health and medication needs.
- Clinical Decision Support Systems (CDSS): Integrating advanced software into electronic health records that can flag potential drug-drug interactions, identify inappropriate medications for specific patient populations (e.g., the elderly), and suggest alternative therapies.
- Patient and Caregiver Education: Empowering patients and their caregivers with knowledge about their medications, potential side effects, and the importance of discussing all medications (including OTC and supplements) with their healthcare team. Encouraging patients to maintain an up-to-date medication list is crucial.
- Geriatric Assessment Units: Specialized units that provide comprehensive geriatric assessments, including detailed medication reviews, to optimize care for complex older patients.
- Standardized Guidelines and Training: Developing and implementing clear guidelines for managing polypharmacy and providing ongoing education and training for healthcare professionals in geriatric pharmacology and deprescribing.
Voices from the Frontlines: Perspectives of Healthcare Professionals
Healthcare professionals are acutely aware of the polypharmacy challenge. General practitioners often express feeling overwhelmed by the complexity of managing multiple chronic conditions and the sheer volume of medications prescribed by specialists. Pharmacists, positioned at the interface of patient and prescription, frequently identify potential issues but sometimes lack the direct authority or systematic framework to intervene effectively without direct physician consultation. Geriatricians consistently advocate for a "less is more" approach, emphasizing individualized care and the careful consideration of a patient’s overall goals rather than treating each disease in isolation. There is a broad consensus among these groups that systemic changes are needed to facilitate better communication and support more integrated, patient-centered care.
The Patient’s Journey: Navigating Complex Regimens
For older patients and their caregivers, navigating a complex medication regimen can be a daily struggle. The "piluliers" (pill organizers) mentioned in the original article are a testament to the sheer number of pills many seniors manage. Remembering which pill to take, when, and for what purpose can be daunting, leading to anxiety, confusion, and a diminished sense of autonomy. The burden often falls on family caregivers, who must meticulously organize medications, monitor for side effects, and communicate with multiple healthcare providers. This adds significant stress and can impact their own well-being. Empowering patients with simple tools, clear instructions, and consistent support from their healthcare team is paramount to improving adherence and safety.
Broader Implications: Towards a Safer Future for Geriatric Care
The escalating issue of polypharmacy has profound implications for the future of geriatric care. It highlights the urgent need for a paradigm shift from a disease-centric model to a patient-centric, holistic approach. Policymakers must consider initiatives that support integrated care, incentivize medication reviews, and invest in robust electronic health record systems that can seamlessly share patient information across different care settings. Research into novel pharmacotherapies that address multiple conditions with fewer drugs, and better understanding of drug-drug-disease interactions, is also critical.
Ultimately, controlling polypharmacy is not merely about reducing the number of pills; it is about enhancing the safety, efficacy, and overall quality of life for older adults. As the global population continues to age, proactively addressing this challenge will be fundamental to ensuring that longevity is accompanied by vitality and well-being, rather than being overshadowed by the unintended consequences of medical interventions. The insights from Sciences et Avenir serve as a timely reminder that the quest for improved health must also prioritize thoughtful and judicious prescribing practices.